

|

|

Volume 4: No.
4, October 2007
SPECIAL TOPIC
Development of a Culturally Appropriate, Home-Based Nutrition and Physical Activity Curriculum for Wisconsin American Indian Families
Tara L. LaRowe, PhD, Deborah P. Wubben, MD, MPH, Kate A. Cronin, MPH, SuAnne M. Vannatter, RN, BSN, Alexandra K. Adams, MD, PhD
Suggested citation for this article:
LaRowe TL, Wubben DP, Cronin KA, Vannatter
SM, Adams K. Development of a culturally appropriate, home-based nutrition and physical activity curriculum for Wisconsin American Indian families. Prev Chronic
Dis 2007;4(4). http://www.cdc.gov/pcd/issues/2007/
oct/07_0018.htm.
Accessed [date].
PEER REVIEWED
Abstract
We designed an obesity prevention intervention for American Indian families
called Healthy Children, Strong Families using a participatory approach involving three Wisconsin tribes.
Healthy Children, Strong Families promotes healthy eating and physical
activity for preschool children and their caregivers while respecting each
community’s cultural and structural framework. Academic researchers, tribal
wellness staff, and American Indian community mentors participated in development of the
Healthy Children, Strong Families educational curriculum. The curriculum is based on social cognitive and family systems theories as well as
on community eating and activity patterns with adaptation to
American Indian cultural values. The curricular materials, which were delivered
through a
home-based mentoring model, have been successfully received and are being modified so that they can be tailored to individual family needs. The
curriculum can serve as a nutrition and physical activity model for health
educators that can be adapted for other American Indian preschool children and their families or as a model for development of a culturally specific curriculum.
Back to top
Introduction
Childhood overweight and obesity rates in the United States are increasing (1), with American Indian (AI) children having the highest rates (2,3). Nearly 37% of AI children aged 2
to 5 years are overweight or obese compared with 30%
of the same-aged children in all ethnic groups combined (1). The Wisconsin Nutrition and Growth Study (WINGS), our previous research
on this topic, showed that the prevalence of overweight
for
Wisconsin AI children aged 5 to 8 years was 27% and that an additional 19% are at risk for being overweight (4). Compared with a national sample of children aged 6
to 11 years (5), the prevalence of overweight for WINGS children was almost 8% greater.
We observed several health-related behaviors among WINGS children that are hypothesized as
being associated with overweight in children, including low fruit and vegetable intake, high soda and candy consumption, low levels of physical activity, and watching television more than 2 hours
per day (6). These observations highlight the need for risk factor modification early in life to prevent the development of overweight
in children. Additional qualitative research conducted in WINGS showed that most caregivers of AI children did not recognize the link between excess weight and chronic disease later in life (4), underscoring the need for education and awareness building in families.
Our current study, Healthy Children, Strong Families (HCSF), focuses on obesity prevention in early childhood in three Wisconsin AI tribal communities. Early childhood is a critical period, both physiologically and psychologically, as children are growing rapidly and developing their own food consumption and physical activity patterns. A child’s diet is determined by the food
environment that the parent provides, which in turn shapes the child’s preferences and food acceptance patterns (7). For children, parents are the primary mediators of change in adopting healthy eating
habits (8-12) and reducing sedentary behaviors (13,14). Research has also found that parental involvement is important to both prevention and treatment of childhood obesity (8,15,16). This
finding is also
true in AI communities where the sphere of influence includes the extended family (12,17).
HCSF is a family-based intervention guided by trained AI community mentors through home visits. It will test the effectiveness of an early childhood obesity prevention program that directly involves primary caregivers of preschool-age children in three Wisconsin AI communities. This paper presents the process of the development of a nutrition and physical activity curriculum and delivery of
the curriculum in a home-based setting with the participation of academic and tribal researchers, tribal community members, and tribal wellness staff.
Back to top
Description of HCSF Intervention
Background
The Great Lakes Inter-Tribal Council, three Wisconsin AI tribes, and researchers at the University of Wisconsin–Madison have formed an ongoing academic and community partnership that is
in its seventh year of research (18). WINGS was the first research project conducted
by this research partnership. Its primary goal was to document the prevalence of obesity and
cardiovascular risk factors and familial and environmental factors contributing to obesity in children aged 3
to 8 years at three Wisconsin tribal sites (4,6). Another goal of WINGS was to design and implement an obesity prevention intervention (18). Thus, WINGS served as the formative research for the HCSF project, which was jointly designed by the academic and community partners:
Great Lakes Inter-Tribal Council, University of Wisconsin–Madison researchers, and tribal wellness staff. The Great Lakes Inter-Tribal Council obtained
initial funding for HCSF, with University of Wisconsin–Madison researchers and the three tribal communities as subcontracted partners.
Intervention design
HCSF is a 12-month randomized trial for AI children aged 2 to 5 years and
their primary caregivers. The goal of the project is to evaluate the
effectiveness of a series of targeted home visits and group sessions on obesity
reduction and healthy lifestyle behaviors for caregivers and their children. Families
from each community that enroll in HCSF are
randomly assigned according to the child’s body mass index (BMI)
percentile (i.e., 85th percentile and <85th percentile) into
either an intervention or a control group. Tribal wellness staff and tribal health directors
decided to randomly select by family rather than by community because all tribal communities wanted to be part of the intervention.
Over the course of 12 months, intervention families will receive 12 lessons on nutrition and physical activity delivered by a home-visiting mentor,
and control families will receive the same 12 lessons by mail. In addition, the intervention families will receive three group-activity lessons designed to help intervention families support one another in making
and sustaining healthy lifestyle choices. Group activity lesson topics reinforce the curriculum topics from the lessons.
Target population and recruitment strategy
The intervention was approved by tribal councils, Head Start site directors, and tribal health directors at each
of the three reservation sites. The University of Wisconsin–Madison Human Subjects Review Board approved HCSF prior to recruitment. Recruitment began in
April 2006 and focused on Head Start programs in all communities. Academic and
tribal research staff attended school meetings and functions to generate interest among Head Start teachers, staff, and families. Each family that enrolled in HCSF included at least one child aged 2
to 5 years and one primary caregiver.
Back to top
Curriculum Development
Theoretical framework
HCSF educational materials are based on psychological theories that support
lifestyle behaviors for obesity prevention, including social cognitive theory
(19) and family systems theory (20). Cognitive-behavioral approaches, such as
goal setting, incentives, interactive delivery of educational material, and
reinforcement, have been shown to be effective in family-based obesity
interventions (21,22). Several studies using combinations of this theoretical
framework within family-based intervention models showed improvement in physical
risk factors in children (23) as well as behavioral changes in both children
(24) and their parents or caregivers (25). By using this theoretical framework, HCSF curriculum
designers created a learning model to involve both
caregiver and child and to improve self-efficacy of parents to model healthy eating and physical activity behaviors for their children. During the WINGS project, many parents were anxious for an assessment of their own health risks. In addition, during WINGS focus groups, parents described an interest in more education and information on healthy eating and activity for their families
(26). Thus, we combined our community-based knowledge with theoretical frameworks to assist in intervention design and curriculum development.
Curriculum development process
A curriculum for AI children aged 2 to 5 years and their primary caregivers was designed by academic researchers, tribal researchers, child development specialists, dietitians who had experience working with AI children, and a home-visiting expert experienced in working with underserved communities. The curriculum consists of 12 lessons that are distributed to families
during the 12-month intervention. The lessons are delivered in front-loaded frequency during the first 3 months;
that is, we distribute the first six lessons approximately every 2 to 3 weeks
and the last six lessons every four to six weeks thereafter. The process for curriculum
development included 1) creating a framework for each lesson, 2) brainstorming ideas and activities, 3) drafting each lesson, 4) evaluating and modifying the lessons, and 5) finalizing each lesson. The process is illustrated in the Figure. This participatory process was used to maximize early community input before intervention delivery and to allow for modifications by community members in an ongoing process as the intervention is delivered to families and feedback
is received.
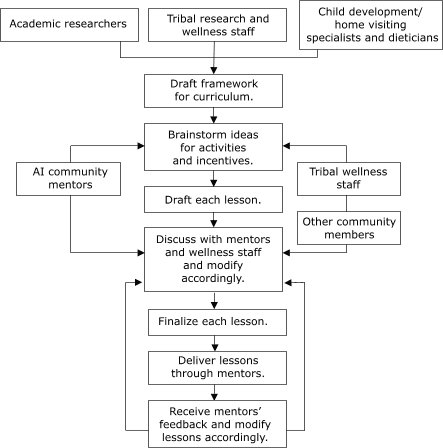
AI indicates American Indian.
Figure. Participatory process for curriculum development in the
Healthy Children, Strong Families intervention, Wisconsin, 2005. [A text description of this flow chart is also available.]
Curriculum objectives and framework
Our previous research in these tribal communities showed that children had low fruit and vegetable intake, consumed high levels of soda and candy, and watched television
excessively (6). Meal patterns were similar to those found in the general U.S. population, and diets included few traditional AI foods and a high proportion of processed foods. Therefore, we chose to use the following nutrition
and physical activity behaviors as objectives for the curriculum: 1) increasing fruit and vegetable intake; 2) increasing physical activity; 3) decreasing consumption of candy, soda, and other sweetened beverages; and 4) decreasing television viewing time. The primary aim of the curriculum is to educate and enable caregivers to make healthier food and activity choices for themselves and
for their
children. The curriculum involves and teaches caregivers and children simultaneously in a series of fun, experiential home lessons delivered by a knowledgeable community member.
In developing the framework for each lesson, the HCSF team emphasized traditional AI learning through storytelling, family activities, reflecting on lessons learned, and goal setting. The lesson format has five components: 1) a topic introduction with lesson objectives, 2) a review of the last lesson to reinforce previously learned skills, 3) new material
and a learning
activity, 4) a brainstorming session to identify ways to change behavior and to discuss barriers and strategies for overcoming those barriers, and 5) reflection on the lesson and goal setting for behavior change between lessons Table 1.
We decided that introducing each lesson topic in the form of storytelling would
be most effective as this is a culturally acceptable method of learning from
elders. Therefore, we developed a segment within each lesson that focused on
traditional AI physical activity and eating patterns compared
with today’s patterns. This segment focuses on bringing a balance of traditional AI eating and activity into family life today.
Activity ideas for the four healthy-behavior objectives were developed as each lesson was drafted. After an initial draft, lessons were discussed with and peer reviewed by tribal wellness staff and AI community mentors. We modified lessons to accommodate cultural acceptability, ease of use in the home, and seasonal activities and foods (e.g., snow activities for the winter, berry picking in
the summer). AI community mentors also contributed to the curriculum by adding activities that their communities participate in,
such as basket making, beading, and snow games in the winter, and suggesting ways to incorporate those activities into the lessons. AI mentors further modified the curriculum by including their own stories of hunting, fishing, berry picking, and gathering wild rice and
by adding favorite recipes for traditional foods. A sample lesson with objectives and activities is shown in Table 2.
Each lesson developed became part of a tool kit, which includes additional games, books, or recipes specific to that lesson for both child and caregiver. A tip sheet for each lesson is also included in the tool kit to give families ideas for achieving the corresponding objective (e.g., a tip for increasing fruit consumption is to add fresh fruit to cereals or muffins). Lastly, each
family is given a 12-month calendar filled with pictures of local families engaging in healthy behaviors, such as playing lacrosse, dancing at a powwow, growing squash, sledding, and harvesting wild rice. The purpose of the calendar is to track family goals throughout the year.
Back to top
Description of Intervention Delivery by Community Mentors
The intervention arm of the HCSF includes home visits by an AI community
mentor to review the curriculum with the families, assist families in setting
healthy behavior goals, and track the families’ progress throughout the intervention. A fundamental goal for the HCSF intervention is to use the traditional AI model of elders teaching life skills to the next generation by instilling
values of healthy nutrition and exercise while reinforcing cultural values such as consumption of traditional foods. We hypothesize that AI families participating in HCSF will be
most successful in behavior change using this learning model.
We chose home-mentored visits as the delivery method for the intervention group because previous research has shown
that this approach has an overall positive impact on families and preschool children (27,28) and improves participation and retention (22). Home-based visiting was also successful in behavior change in one small study
focusing on AI families (17). Furthermore, home visits in AI communities are appropriate because of the cultural preference for face-to-face contact, the tradition of elders teaching life skills to the next generation, and the familiarity of home visits for young families in these communities.
We hired eight mentors from the three tribal communities for the HCSF intervention. These mentors are experienced older parents, grandparents, and respected community members and are capable of delivering the intervention according to study protocol. Mentors were trained extensively by the University of Wisconsin Extension staff, tribal wellness staff (including
nurses, diabetes educators, and dietitians), knowledgeable tribal elders, and HCSF research staff
before beginning home visits. This training modified a well-developed home visiting program, Healthy Families America, to encompass the needs of the HCSF intervention and its objectives (29). Additional training was provided on child development, nutrition, and physical activity so that mentors have basic knowledge of the
lesson topics they are presenting to the families.
Back to top
HCSF Evaluation
Before randomization of families, baseline assessments are being collected from
each primary caregiver and child to measure primary and secondary outcomes of the intervention. Primary outcomes of HCSF include measurements of child waist circumference and caregiver BMI. Secondary outcomes for children and caregivers include servings of fruit and vegetables and servings of sweetened beverages
and candy consumed per day, hours per day of watching television, and percentage of day spent in sedentary activities. Additional adult secondary outcomes include measures of cultural identity, health-related quality of life, self-efficacy for healthy behaviors, and biochemical markers of cardiovascular and diabetes disease risk. All primary and secondary measurements will be assessed again after
completion of the 12-month intervention.
HCSF is currently recruiting families and collecting baseline data. Of the
enrolled families, 92 have been
randomly assigned to the control or the intervention group. Seventy-four percent of the families in the intervention group have completed two or more mentored home visits to date. Structured interviews with the HCSF mentors at the 6-month mark have revealed that the first few meetings are
more focused on rapport and relationship building than on the lessons. The mentors report that families have been enthusiastic about the curriculum and particularly enjoy the active portions of the lesson. Mentors also report to HCSF staff
about specific activities within the lessons that work well or do not work well during family visits. Modifications to lessons are being made
throughout the intervention period so that the lessons are more acceptable and appropriate for the participating families.
Back to top
Discussion
To our knowledge, few studies have developed a curriculum for preschool-aged children as part of an obesity intervention. The Hip Hop to Health Jr. program, which is similar to HCSF, developed a culturally specific nutrition and physical activity curriculum for preschool-aged children participating in Head Start programs
that included a primary caregiver component (30). However, that program
was delivered in Head Start classrooms with a separate adult component and did not involve adult–child interaction or mentoring. The Healthy Start study also developed a culturally sensitive curriculum for preschool-aged children that focused on healthy behaviors (31). However, the topics that Healthy Start focused on were different from those of HCSF
(Healthy Start topics included dental hygiene
and violence prevention); the program was conducted entirely within the school; and it involved parents only through take-home activities (31).
The HCSF intervention has several limitations. We did not conduct a pilot study because of the communities’ desire to begin the intervention immediately as well as time constraints related to study funding.
In addition, the time frame for curriculum development did not allow for the full participation of all community members, specifically the community AI mentors,
because they had to be
hired after initial curriculum development.
Although we were limited by not involving all community members in the
beginning phases of curriculum development, AI mentors and other community
members were involved in revising and modifying lessons to ensure that they were culturally appropriate and acceptable for the families. A main strength of HCSF is that we
are using a community-based participatory research approach that is both data
driven and community driven. Tribal communities expressed their need for an obesity prevention project after academic researchers returned the results of WINGS to the participating communities.
We found that to successfully develop and deliver the HCSF curriculum in AI communities, strong participation from community members was needed. It was also important to foster and maintain relationships and develop trust with tribal wellness staff, AI community mentors, and other community members, including Head Start teachers and staff.
The HCSF curriculum provides a nutrition and physical activity model for health and nutrition educators that may be adapted for other AI preschool children and their families or may serve as a model for development of a culturally specific curriculum.
Back to top
Acknowledgments
The HCSF research study is supported by grants from the Wisconsin Partnership Fund for a Healthy Future and NIH Grants
Nos. T32-HP-10010-10 and 1-U01-HL087381-01.
We thank Tassy Parker, PhD, RN, Judy Arneson, BS, Amy Meinen, MS, RD, and Mary Lamon-Smith, MS, RD, for their contributions and expert advice in developing the curriculum. We extend special thanks to tribal wellness
staff members Mark Casky and Scott Krueger, the wellness staff and community mentors in the three Wisconsin AI communities, and Pence Revington of the University of Wisconsin Extension for their participation in, and contributions to, this project.
Back to top
Author Information
Corresponding Author: Tara L. LaRowe, PhD, Department of Family Medicine, University of Wisconsin–Madison, 777 South Mills Street, Madison, WI 53714. Telephone: 608-262-6535. E-mail: tara.larowe@fammed.wisc.edu.
Author Affiliations: Deborah P. Wubben, Kate A. Cronin, Alexandra K. Adams, Department of Family Medicine, University of Wisconsin–Madison, Madison,
Wisconsin, SuAnne M. Vannatter, Great Lakes Inter-Tribal Council, Inc., Lac du Flambeau,
Wisconsin.
Back to top
References
- National Center for Health Statistics. Prevalence of overweight among children and adolescents: United States, 1999. Hyattsville
(MD): National Center for Health Statistics; 2001.
- Broussard BA, Johnson A, Himes JH, Story M, Fichtner R, Hauck F, et al.
Prevalence of obesity in American Indians and Alaska Natives. Am J Clin Nutr 1991;53(6
Suppl):1535S-42S.
- Troiano RP, Flegal KM, Kuczmarski RJ, Campbell SM, Johnson CL.
Overweight prevalence and trends for children and adolescents. The National Health and Nutrition Examination Surveys, 1963 to 1991. Arch Pediatr Adolesc Med 1995;149(10):1085-91.
- Adams AK, Quinn RA, Prince RJ.
Low recognition of childhood overweight and disease risk among Native-American caregivers. Obes Res 2005;13(1):146-52.
- Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM.
Prevalence of
overweight and obesity in the United States, 1999-2004. JAMA 2006;295(13):1549-55.
- Adams A, Prince R, Webert H. The Wisconsin Nutrition and Growth Study (WINGS), a participatory research project with three Wisconsin tribes. The Great Lakes EpiCenter News 2004;5:1-3.
http://www.glitc.org/epicenter/publications*
- Birch LL, Fisher JO.
Development of eating behaviors among children and adolescents. Pediatrics 1998;101(3
Pt 2):539-49.
- Golan M, Crow S.
Parents are key players in the prevention and treatment of weight-related problems. Nutr Rev 2004;62(1):39-50.
- Birch LL, Davison KK.
Family environmental factors influencing the developing behavioral controls of food intake and childhood overweight. Pediatr Clin North Am 2001;48(4):893-907.
- Benton D.
Role of parents in the determination of the food preferences of children and the development of obesity. Int J Obes Relat Metab Disord 2004;28(7):858-69.
- Teufel NI, Perry CL, Story M, Flint-Wagner HG, Levin S, Clay TE, et al.
Pathways family intervention for third-grade American Indian children. Am J Clin Nutr 1999;69(4
Suppl):803S-9S.
- Davis SM, Going SB, Helitzer DL, Teufel NI, Snyder P, Gittelsohn J, et al.
Pathways: a culturally appropriate obesity-prevention program for American Indian schoolchildren. Am J Clin Nutr 1999;69(4
Suppl):796S-802S.
- Crespo CJ, Smit E, Troiano RP, Bartlett SJ, Macera CA, Andersen RE.
Television watching, energy intake, and obesity in US children:
results from the Third National Health and Nutrition Examination Survey, 1988-1994. Arch Pediatr Adolesc Med 2001;155(3):360-5.
- Polley DC, Spicer MT, Knight AP, Hartley BL.
Intrafamilial correlates of overweight and obesity in African-American and Native-American grandparents, parents, and children in rural Oklahoma. J Am Diet Assoc 2005;105(2):262-5.
- Wrotniak BH, Epstein LH, Paluch RA, Roemmich JN.
Parent weight change as a predictor of child weight change in family-based behavioral obesity treatment. Arch Pediatr Adolesc Med 2004;158(4):342-7.
- St Jeor ST, Perumean-Chaney S, Sigman-Grant M, Williams C, Foreyt J.
Family-based interventions for the treatment of childhood obesity. J Am Diet Assoc 2002;102(5):640-4.
- Harvey-Berino J, Rourke J.
Obesity prevention in preschool Native-American children:
a pilot study using home visiting. Obes Res 2003;11(5):606-11.
- Adams AK, Miller-Korth N, Brown D.
Learning to work together:
developing academic and community research partnerships. WMJ 2004;103(2):15-9.
- Bandura A.
Health
promotion by social cognitive means. Health Educ Behav 2004;31(2):143-64.
- Golan M, Weizman A.
Familial approach to the treatment of childhood obesity: conceptual mode. J Nutr Educ 2001;33(2):102-7.
- Kirk S, Scott BJ, Daniels SR.
Pediatric obesity epidemic:
treatment options. J Am Diet Assoc 2005;105(5 Suppl 1):S44-51.
- Williams K, Prevost AT, Griffin S, Hardeman W, Hollingworth W,
Spiegelhalter D, et al.
The ProActive trial protocol — a randomised controlled trial of the efficacy of a family-based, domiciliary intervention programme to increase physical activity among individuals at high risk of diabetes
[ISRCTN61323766]. BMC Public Health 2004;4:48.
- Epstein LH, Myers MD, Raynor HA, Saelens BE.
Treatment of pediatric obesity. Pediatrics 1998;101(3
Pt 2):554-70.
- Golan M, Fainaru M, Weizman A.
Role of behaviour modification in the treatment of childhood obesity with the parents as the exclusive agents of change. Int J Obes Relat Metab Disord 1998;22(12):1217-24.
- Golan M, Weizman A, Apter A, Fainaru M.
Parents as the exclusive agents of change in the treatment of childhood obesity. Am J Clin Nutr 1998;67(6):1130-5.
- Adams A, Harvey H, Brown D. Listening to parents:
child health concerns inform obesity prevention in American Indian communities. Obesity.
Forthcoming.
- Worobey J, Pisuk J, Decker K.
Diet and behavior in at-risk children: evaluation of an early intervention program. Public Health Nurs 2004;21(2):122-7.
- McNaughton DB.
Nurse home visits to maternal-child clients: a review of intervention research. Public Health Nurs 2004;21(3):207-19.
- Ericson N. Healthy families America. Fact sheet No. 23. Washington (DC):
U.S. Department of Justice; 2001.
http://www.ncjrs.gov/pdffiles1/ojjdp/fs200123.pdf. Accessed June 8, 2007.
- Fitzgibbon ML, Stolley MR, Dyer AR, VanHorn L, KauferChristoffel K.
A community-based obesity prevention program for minority children:
rationale and study design for Hip-Hop to Health Jr. Prev Med 2002;34(2):289-97.
- Williams CL, Squillace MM, Bollella MC, Brotanek J, Campanaro L,
D'Agostino C, et al.
Healthy Start: a comprehensive health education program for preschool
children. Prev Med 1998;27(2):216-23.
Back to top
|
|
