

|

|

Volume 4: No. 2, April 2007
REVIEW
Filipino Child Health in the United States: Do Health and Health Care Disparities Exist?
Joyce R. Javier, MD, MPH, Lynne C. Huffman, MD, Fernando S. Mendoza, MD, MPH
Suggested citation for this article: Javier JR, Huffman LC, Mendoza FS. Filipino child health in the
United States: do health and health care disparities exist? Prev Chronic Dis [serial online] 2007 Apr [date cited]. Available from:
http://www.cdc.gov/pcd/issues/2007/
apr/06_0069.htm.
PEER REVIEWED
Abstract
Introduction
Filipinos are the second largest Asian subgroup in the United States, but few studies have examined health and health care disparities in Filipino children. The objectives of this review are 1) to appraise current knowledge of Filipino children’s health and health care and 2) to present the implications of these findings for research, clinical care, and policy.
Methods
We identified articles for review primarily via a Medline search emphasizing the terms Filipino and
United States crossed with specific topics in child and adolescent health that fall under one of Healthy
People 2010’s 28 focus areas.
Results
Filipino children are underrepresented in medical research. Studies that compare
Filipino children and adolescents with white children or children of other Asian Pacific Islander subgroups suggest disparities with regard to gestational diabetes,
rates of neonatal mortality and low birth weight, malnutrition in young children, overweight, physical
inactivity and fitness, tuberculosis, dental caries, and substance abuse. Studies
that compare Filipino adults with white adults describe adult Filipino health
problems similar to those of Filipino children, including higher rates of diabetes, hypertension, and metabolic syndrome. Health care disparities remain to be determined.
Conclusion
Health and health care disparities appear to exist for Filipino children, but more research is needed to confirm these findings. Practitioners serving this population need to consider social and cultural factors that can increase or diminish risk for health problems. There are priorities in research and policy that, if pursued, may improve the health care and health
outcomes of Filipino children.
Back to top
Introduction
The population of Asian Pacific Islander (API) children in the United
States is expected to more than double by 2025 (1). Yet, we have only a limited understanding of the health and health care issues that characterize these children. Many studies that include API children report aggregated results, which mask key variations in health status among API subgroups. Moreover, many recent national surveys of
children and adolescents do not collect data on API subgroups (2,3).
Filipinos are the second largest API subpopulation in the United States
(4). On average, one in five Asians in the United States is Filipino (5).
Most Filipinos live in California or Hawaii; however, Filipino populations
in other states have more than doubled in the past decade (e.g., Texas,
Florida). California is home to the largest Filipino population with more
than 1 million, and Hawaii ranks second. Between 1990 and 2000 the U.S.
Filipino population grew by 68.1% (6). Figures 1 and 2 display the distributions of the U.S. child population by ethnicity and by Asian
population subgroup (7), respectively.
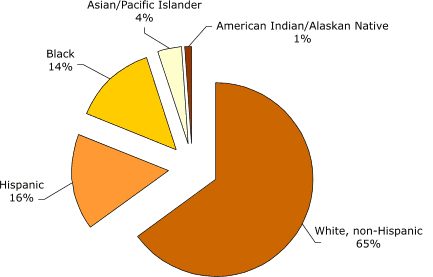
Figure 1. Percentage of U.S. children (Aged 0–18) by
racial or ethnic group, 2000. All categories include those of mixed race or mixed ethnicity (7).
Calculated by Joyce R. Javier from U.S. Census Bureau, Census 2000
Summary File 2 (SF 2) 100-Percent Data files. [A tabular version of this chart is also available.]
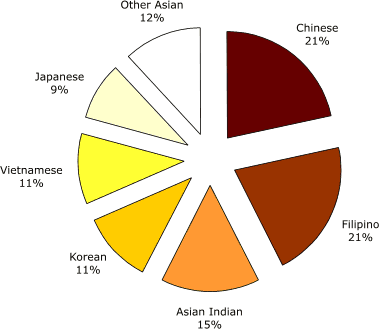
Figure 2. U.S. Asian children (Aged 0–18) by subgroup, 2000. All categories include those of mixed race
or mixed ethnicity (7). Calculated by Joyce R. Javier from U.S. Census Bureau, Census 2000
Summary File 2 (SF 2) 100-Percent Data files. [A tabular version of this chart is also available.]
Studies that compare Filipino adults with other API or white
adults have found disparities in areas such as cancer, cardiovascular health, and mental health (8,9). Little has been published about the health of Filipino children and adolescents. In this descriptive review of the literature, we compare the health of Filipino and white children to determine whether Filipino children are
among those children in the United States that experience health and health care disparities. When data are available, we highlight differences between Filipino and other Asian subgroups. We also present important health and health care issues
for which data are available on Asians but not on Filipinos specifically.
Back to top
Methods
We identified articles for review primarily via a Medline search of the terms Filipino and United States crossed with specific topics in child and adolescent health that fall under one of Healthy People
2010’s 28 focus areas. Studies selected for review were for the most part
limited to those that were published between 1985 and 2005, were written in
English, had subjects in the United States, compared Filipinos or Asians with
other racial or ethnic groups, and addressed specific topics in child and
adolescent health. Topics addressed were access to quality health
services, maternal and infant health, nutrition, oral health, overweight,
physical activity and fitness, respiratory diseases, infectious diseases and
immunizations, sexually transmitted diseases, substance abuse, tobacco use,
injury and violence prevention, mental health, and conditions highly prevalent
among adults on which there are no studies with Filipino children as subjects (e.g., diabetes, heart disease). These topics were
selected because they fall under one of Healthy People 2010’s 28 focus areas (10).
We further examined the references listed in the identified articles and, where
available, followed electronic links to related articles through the PubMed
search engine.
In this article the term Filipino denotes any U.S. resident originating from any of the original peoples of the Philippine Islands. We do not use the terms API and Asian interchangeably. API refers to Asians and Pacific Islanders together as one group. When we refer to these two groups separately, the term Asian does not
include Pacific Islanders. An Asian is a person whose origins are
in any of the original people of the Far East, Southeast Asia, or the Indian subcontinent, including the Philippine Islands. A Pacific Islander is a person whose origins are in any of the original peoples of Hawaii, Guam, Samoa, or other Pacific Islands. Pacific Islanders are
a separate category from Asians, although they are sometimes included with
Asians or relegated to an other category.
Back to top
Results
Health disparities can manifest in two major areas: health and health care. In this review, we first address health care, specifically examining access to quality health care. We then focus on the health of Filipino youth
in three categories: infant and young child health, school-age youth and
adolescent health, and relevant adult health problems. We present the identified health studies with specific data on Filipino infants and
young children
(Table 1), school-age youth and adolescents
(Table 2), and relevant adult diseases
(Table 3).
Access to quality health services
Research is lacking on the quality of medical care among Filipino children. With respect to health care access, national data show that Filipino children
in the United States are more likely than white children to have health insurance. Filipino youths also have more favorable health status than white youths as indicated by less frequent school absence, less learning disability, less use of prescription
medications, and fewer chronic conditions. However, Filipino children are more likely than white children to be without a usual place for receiving health care and not to have had contact with a health professional within the
previous 12 months (11). Also, compared with Filipino adolescents living in the
United States for short periods, Filipino adolescents living in the United
States for long
periods tended to report more physical health problems (12). These studies suggest that Filipino children face barriers to health care access and
use that extend beyond health insurance issues, highlighting the need to consider generational status
(i.e., whether the child is a first, second, or third generation
immigrant) and time spent in the United States when considering risk for health problems.
Infants’ and young children’s health (aged 0–5 years)
Maternal and infant health
Studies have documented mixed perinatal
outcomes for Filipinos, and when these outcomes are worse compared to whites,
familiar risk factors (e.g., lack of prenatal care, smoking status) do not
completely explain this variation. Compared
with white mothers, Filipino mothers have similar infant, neonatal, and postneonatal mortality rates (13).
However, Filipino women are at increased risk for delivering infants who are of moderately low
(defined as 1,500–2,499g) and very low birth weight (defined as 500–1,499g) (14), preterm (15),
or stillborn (16).
For Filipino women, the association between maternal place of
birth and child health has been mixed. National data demonstrate a pattern consistent with the epidemiological paradox in that, compared
with the offspring of U.S.-born mothers, the offspring of Philippine-born mothers have more favorable birth weights as well as lower infant mortality rates (13,17,18).
Philippine-born mothers are also less
likely to use alcohol and tobacco and have inadequate prenatal care during their pregnancies but are more likely to have inadequate weight gain (less than 22 pounds) (18). A study in Hawaii found that, compared
with U.S.-born Filipinos, foreign-born Filipinos had a higher risk of preterm delivery and low birth weight (19).
According to the National Vital Statistics Report (17), in 2002 Filipino mothers (data not available by
place of birth) had the highest rate of gestational diabetes among all measured subgroups at 59.8 per 1,000. Another study using national data reported that Philippine-born Filipino mothers are significantly more likely to have diabetes during pregnancy than U.S.-born Filipino mothers (20). The
impact of the mother’s place of birth on diabetes prevalence may be partially explained by the older childbearing age of Filipino immigrant mothers, but differences in diabetes prevalence remain even after adjusting for differences in maternal age and other sociodemographic characteristics.
Weitz et al examined teen pregnancy among API subgroups and reported that when data on APIs are disaggregated, Filipinos have the highest percentage of births to teens (6%) among California’s six largest API groups (Chinese, Filipino, Vietnamese, Korean, Indian, and Japanese) (21). Compared
with white teens, Filipino teens are more likely to request a pregnancy test and no other services from a provider, suggesting that they are sexually active but not looking for birth control. According to national data, U.S.-born Filipino mothers are more likely to be under age 20 than foreign-born Filipino mothers (11.0% vs 2.7%) (17). These studies reveal the importance of considering moderating variables
(e.g., maternal place of birth, regional variations, maternal age, and genetic predisposition) when examining maternal and infant health outcomes in Filipinos.
Nutrition
There have been a limited number of nutrition studies on Filipino children because they are not sampled
as a group in national or large regional studies. A longitudinal study of immigrant school-aged children in San Francisco revealed that all immigrant children, including those from the Philippines, showed catch-up growth in weight and height. This
finding suggests that they arrived in this country with a
deficiency in either height or weight and that they were malnourished before
arriving in the United States (22). Another study of children participating in Hawaii’s Women, Infants, and Children program found that, among 1-year-olds, Filipinos had the highest percentage of underweight (30.2%); among
children aged 2 to 4 years, Filipinos had the highest percentage of short stature (19.0%) (23). These two studies suggest
that Filipino immigrant children may be affected by a statistically significant degree of relative malnutrition.
Oral health
There are no national data on the prevalence of dental caries
among Filipino children. In Hawaii, Filipino children stand out as having one of the highest rates of dental caries (defined as decayed
and filled teeth), a rate nearly three times the national average. The proportion of
Filipino children with baby bottle tooth decay and unmet dental treatment needs
is higher than the proportion of white
children (24). A study using community focus groups in the Northern Mariana Islands, a commonwealth of the United States, found that the low value of baby teeth and the negative treatment experiences parents had with painful dental care were major determinants of health beliefs surrounding oral health care for their children (25). Qualitative research allows for cultural tailoring of
interventions, which may make dental treatment more acceptable to the targeted group. For example, our literature review revealed that advertising
claiming that preventive visits are pain- and fear-free, in contrast to the experiences of parents when they were young, could be an important strategy to promote dental visits earlier in childhood.
School-age youth and adolescent health (aged 6–18 years)
Overweight, physical activity, and fitness
A study of fifth, seventh, and ninth graders in California demonstrated that Filipino males were more likely to be obese (defined as Body Mass Index [BMI] >85th percentile) than white males, and Filipino females were more likely to be obese than white females (26). In a study that did not separate males from females, Filipino adolescents had a lower prevalence of obesity than
white adolescents. However, Filipino adolescents born in the United States were more than twice as likely to be obese
as were those born outside the United States (27).
Research on perceptions of obesity and body- or self-dissatisfaction reported varied results based on age and sex. A study of college students found that Filipino males had the highest BMI and were the most body-
or self-dissatisfied of all male comparison groups (28). A study of third grade children in
13 Northern California public elementary schools revealed that Filipino girls were as
likely to have overweight concerns and body-dissatisfaction as white girls (29).
Filipino adolescents were significantly less likely to be physically active than white
adolescents (30). Filipino females (aged 10–15 years) and Filipino males
(aged 10–11 years) also exhibited slower mile run or walk times than white boys and girls (26). The foregoing studies suggest that estimates of the prevalence of obesity, physical activity, and body dissatisfaction
among Filipino children vary according to age and immigration
status.
Respiratory diseases
There are no national prevalence data available on Filipino children for asthma, a highly prevalent chronic condition. According to a California survey of 7th, 9th, and 11th grade students
conducted from 2001 to 2003, Filipinos have the highest lifetime asthma prevalence rates (23.3%) among API subgroups (31). This prevalence rate is lower than
the rate for African Americans, higher than the rate for whites and Asians overall,
and comparable with the rate for Puerto Ricans, an already recognized high-risk population.
Infectious diseases and immunizations
Immigrant children from the Philippines are the second largest immigrant group in the United States
with tuberculosis (32). A study of targeted school-based tuberculosis screening among high-risk adolescent populations in San Diego revealed that Filipinos are more likely to have positive tuberculin skin test (TST) results than whites. Although
the Bacille Calmett-Guerin (BCG)
vaccine was mentioned as a potential source of false-positive TST results,
researchers were unable to correlate BCG vaccination with size of skin test induration because of lack of reliable data on past BCG vaccinations (33).
We were unable to find any studies reporting national or state immunization rates for Filipino children. Perinatal transmission is the most common mode of hepatitis B transmission, and the
remainder of hepatitis B carriers are usually infected during early childhood. Among pregnant Asian American women, the prevalence of hepatitis B surface antigen positivity is higher
among women
born in the Philippines (5.1%) than among Asian American women born in the United States (2.0%) (34). A study in Los Angeles County found that about one third of Filipino fourth-grade students had their full series of hepatitis B vaccine (35). Both studies reveal the need to raise awareness
that hepatitis B virus plays a role in the etiology of liver carcinoma and that
infection is largely preventable through hepatitis B vaccination.
Sexually transmitted diseases
Filipino adolescents appear to be at high risk for contracting sexually transmitted diseases. In San Francisco, they have sexual activity rates similar to those of white students and higher than those of Chinese students (36,37). Filipino adolescents are less likely to have knowledge of HIV prevention,
to talk with their parents about sexual issues, or to use contraception once sexually
active (21,37,38). Furthermore, a study of Filipino adolescents in Los Angeles revealed that
knowledge of HIV prevention was not associated with condom use at last
intercourse. Rather, high self-efficacy
with respect to condom use (i.e., confidence in one’s ability to put a condom
correctly on oneself or partner) and carrying condoms was associated with high condom use at last intercourse (39). These findings suggest that traditional variables related to AIDS risk behavior
among non-Asian populations may not explain condom use among Filipinos. Future studies should identify determinants of AIDS risk behavior among Filipinos as a first step toward developing culturally relevant AIDS prevention programs for these groups. For example, research examining communication about sex in Filipino families revealed that respect for parental authority directly conflicts with
open discussions with children that are promoted in U.S. culture. Recognizing generational differences in acculturation that may lead to impaired transmission
of values may be important in developing interventions addressing adolescent sexual health (38).
Tobacco use and substance abuse
Filipino adolescents have prevalence rates similar to those of whites for inhalant, tobacco, and alcohol use (40). Multiple studies that include API subgroup analyses show that Filipinos use alcohol, tobacco, and drugs at rates that are much higher than previously reported from surveys that aggregate APIs and thus
probably have an unrecognized need for treatment (41,42).
Substance abuse in Filipino youth also appears to be related to mental health
problems. A study in San Francisco found that Filipinos attribute taking drugs
to feeling isolated and depressed shortly after immigrating to the United States
and indicate that gang members initiate other youths into drug use (42).
Among Filipino adolescent females in California, cigarette smoking is associated with
depression and low self-esteem. In contrast, alcohol use is associated with high self-esteem
in Filipino males (43).
Injury and violence prevention
A study in Hawaii revealed that Filipino parents have had to alter their child management style in the United States. Although they are less likely to exhibit verbally and physically aggressive behavior toward their children than Polynesian
American parents, Filipino parents are faced with the need for more direct parental involvement than was customary in the Philippines, where
the extended family
shared in the training and discipline of children (44).
Mental health
Several studies conducted with small samples of Filipinos show differences in
self-esteem and depression scale scores based on sex and immigration status. In
Hawaii, Filipino females have higher mean depression scores than Filipino males,
as measured by the Center for Epidemiologic Studies Depression Scale (45). Research from the Children of Immigrants Longitudinal Study reveal that
low self-esteem was associated with being Filipino (46). Similar findings were supported in a separate qualitative study in two California cities
(47). This study found that when asked what it means to be Filipino, the most prevalent response consisted of statements about family as the center. The family can offer a positive base of Filipino identity for
Filipino youth; however, it
also is a source of stress and alienation that has been associated with depression and suicidal thoughts. Interviews in high schools revealed that counselors were “concerned about the mental health of Filipino students as a group” because they are averse to seeking counseling for fear that their parents will find out (47).
Relevant diseases in Filipino adults
It is imperative to consider adult diseases among Filipinos so that preventive measures can be started in childhood. Given the relatively limited data on Filipino children’s
health, examining diseases of Filipino adults provides some insight regarding the prevalence of certain conditions that may be higher
among Filipino children than children of other races. For example, Filipino adults have a higher prevalence of
diabetes and hypertension than whites and other API subgroups (48-51).
The use of BMI to define overweight and obesity across populations has been questioned in numerous studies because the relationship between BMI and risk for diabetes, hypertension, and metabolic syndrome in the Filipino adult populations differs from that in white populations (52,53). For example, compared with white women, Filipino women have a higher prevalence of diabetes and metabolic
syndrome despite the fact that 90% of Filipino women were not defined as obese (54). This study suggests that the high prevalence of diabetes in Filipinos may be missed
by health care providers because they are not obese by Western standards.
Discussion
Our literature review yielded two important findings. First, it identified disparities in Filipino child health and health care, a critical first step because considering social and cultural factors that influence health and health care can help us to begin to understand these disparities.
Some factors may be protective in terms of health outcomes or they may increase risk. Second, we
identified areas of Filipino child health in need of more research.
Filipino children and adolescents: health disparities do exist and health care
disparities remain to be determined
Our literature review suggests that disparities in Filipino child and adolescent health do exist and are notable with regard to gestational diabetes, neonatal mortality and low birth weight, malnutrition, overweight, physical inactivity, tuberculosis, dental caries, and substance abuse. In addition, there is a high prevalence of diabetes, hypertension, and
metabolic syndrome among Filipino adults, which is significant because of growing evidence that these diseases are affected by events during gestation and early childhood (55,56) and by health-related behavior that is established in childhood and adolescence, such as eating preferences, exercise patterns, and tobacco use (56).
Factors that may contribute to health disparities for Filipino children
Social and cultural factors appear to play an important role
in the health of Filipino children. Fundamental values in Filipino culture
include respect for authority figures, pakikisama, and hiya (57). In general, Filipino adolescents are less willing
than white adolescents to openly disagree with their parents, and they place less emphasis on
autonomy (58). Pakikisama (family unity and closeness) emphasizes smooth interpersonal relationships and reflects a high value on family, harmony, and conflict
avoidance (57). Filipinos often focus on child-rearing practices that develop group-oriented behaviors
in their children, whereas mainstream U.S. culture often emphasizes independent,
individualistic, and self-reliant behaviors. Hiya is shame and is a motivating factor behind behavior. Filipino culture, like other Asian cultures, holds that a child’s behavior is a reflection of family upbringing. This
cultural perception may explain a delay in seeking services for stigmatized problems, such as teen pregnancy and mental illness (59-62).
Lack of communication and cultural understanding between Filipino youths and
their parents may be a source of intergenerational conflict, especially during adolescence when Filipino youths may become more assertive
because of their Western acculturation towards individuality (63). Intergenerational conflict may affect where a child or an adolescent receives help and support. In an unpublished survey of
254 Filipino youths aged 15 to 17 years in Vallejo, California, 65%–85% felt their parents would not be supportive if
they were aware of an alcohol or drug problem or unwanted pregnancy. Also, 76% knew of no place in the Filipino community where they would feel safe seeking help with personal problems (47). This
finding is of special concern given the empirical
evidence that depression
affects Filipino youths and that adolescent health risk behaviors increase with each generation
of Filipino youth. These behaviors include early sexual activity, nonuse of birth control, delinquency, use of violence, and substance abuse (12).
The cultural and social factors presented are meant to increase awareness. However, given the heterogeneity of this group
(i.e., variability in immigration history and demographics), it is important never
to assume that every Filipino family adheres to particular values.
Needed research
There are inadequate data to allow for any firm conclusions regarding disparities
experienced by Filipino children and adolescents in the areas of health care access,
use, and quality; injury and violence prevention; chronic conditions such as asthma; and mental illness. Filipinos and other API subgroups need to be included in research in these areas so that we can determine where disparities exist and monitor
progress in addressing these disparities over time (2,64). In addition, the quality of data must be examined by developing valid and reliable research instruments for use
with this population. Measures used with other immigrant groups can be modified. For example, a Short Acculturation Scale for Hispanics has been cross-culturally validated for use with Filipino adults, and the Center for Epidemiologic Studies Depression
Scale and State-Trait Anxiety Inventory has been evaluated for use in Filipino adolescents (65-67). When collecting data, researchers need to know immigration status variables such as
whether subjects are first or second generation immigrants and the time subjects
have been in the United States (68).
Finally, interventions need to be designed to achieve equity in health and health care
for Filipino youths. Whenever possible, the strengths of Filipino communities (i.e., emphasis on family and interpersonal relationships)
should be used. Some interventions have been implemented. For example, the
National Institutes of Health (NIH) National Heart, Lung, and Blood Institute funded a community-based
partnership to investigate health practices related to cardiovascular disease in the Filipino community (69). Currently, the NIH National Center on Minority Health and Health Disparities is funding a project that is using community-based participatory research
(i.e., research that encourages investigators and community members to
collaboratively answer questions posed by the community, collect data locally,
and communicate results directly to the community for its use [70]) to improve health
care access and health status for cardiovascular disease for Filipino Americans with hypertension living in New York City (70).
Similar community-based participatory research has been described in the area of teen pregnancy prevention in Filipino families (38,59).
Clinical care implications
The social and clinical factors discussed here have significant implications for Filipino children who depend primarily on their parents to access and receive appropriate medical services. For example, health screening and education for stigmatized problems (e.g., tuberculosis) need to take cultural beliefs such as hiya into consideration (62).
For those who care for Filipino adolescents, discussing and assuring confidentiality may assist in getting these young people to open up about their problems.
Both physical and mental health care practitioners can help parents develop communication skills for interacting with their often more acculturated children. Cross-cultural awareness can bridge the intergenerational and intercultural gaps between parents and
children and facilitate the development of a bicultural identity (71). Increased ethnic identity and a greater appreciation of the struggles
of immigrant families could improve intergenerational communication and lead to increased self-esteem and fewer risk behaviors among youths, a perspective with some empirical support (59,73,74).
Policy implications
To address the Healthy People 2010 goals for APIs, health services research needs to include API subgroups. On the national level, APIs can be oversampled in national surveys such as
the National Health and Nutrition Examination Survey. On the state and local level, increased funding should be made available for regions where there are substantial numbers of APIs (67). For example, the California Health Interview Survey
conducted by the Center for Health Care Policy at the University of California, Los Angeles, is the first large-scale state survey to include API subgroups (75).
The need for cultural sensitivity and culturally effective care will only increase as
health providers attempt to meet the needs of an increasingly racially diverse population (76,77). Proposed bills requiring cultural competency should be supported and such training should include information on Filipinos as well as other API subgroups.
Conclusion
The year 2006 marked the centennial anniversary of the start of Filipino
immigration to the United States. Despite their long history in the United States, Filipinos are understudied in medical
research. This review reveals that Filipino children and adolescents are an important, yet hidden, minority group with multiple health needs. Since APIs are the fastest growing minority group within
the United States, it is imperative that we address gaps in knowledge for all API subgroups. After understanding their health needs and recognizing their social and cultural strengths, we can then develop culturally appropriate interventions that work toward the goal of a healthier
Filipino population with an improved quality of life.
Back to top
Acknowledgments
We thank Paul Wise and Thomas Robinson for reviewing earlier versions of this manuscript.
The first author received fellowship funding from the Children’s Health Initiative Pediatric Research Grant (Lucile Packard Foundation for Children’s Health) and The William Randolph Hearst Foundation.
Back to top
Author Information
Corresponding Author: Joyce R. Javier, Division of General Pediatrics, Stanford University School of Medicine, 750 Welch Road, Suite 325, Palo Alto, CA 94304. Telephone: 650-736-2958. Fax: 650-498-5684. E-mail: jjavier@stanford.edu.
Author affiliations: Lynne C. Huffman, Fernando S. Mendoza, Division of
General Pediatrics, Stanford University School of Medicine, Palo Alto, Ca.
Back to top
References
- Stoddard JJ, Back MR, Brotherton SE.
The respective racial and ethnic diversity of US pediatricians and
American children. Pediatrics 2000;105(1 Pt 1):27-31.
- Brahan D, Bauchner H.
Changes in reporting of race/ethnicity, socioeconomic status, gender,
and age over 10 years. Pediatrics 2005;115(2):e163-6.
- Surveys and data collection systems. Hyattsville (MD): National
Center for Health Statistics;[cited 2005 Oct 1]. Available from: http://www.cdc.gov/nchs/express.htm
- U.S. Census Bureau. The Asian population: 2000. Washington (DC): U.S. Department of Commerce; 2002.
- U.S. Census Bureau. We the people: Asians in the United States. Washington (DC): U.S. Department of Commerce; 2004.
- Dela Cruz M, Agbayani-Siewert P. Filipinos. In: Lai
E, Arguelles D, eds. The new face of Asian Pacific America: numbers,
diversity, and change in the 21st century. San Francisco (CA): Asian
American Studies Center Press;
2003. p. 45-50.
- U.S. Census Bureau. Census 2000
summary file 2
(SF2): 100-percent data files. Washington (DC): U.S. Department of Commerce; 2001.
- Dela Cruz FA, McBride MR, Compas LB, Calixto PR, Van Derveer CP.
White paper on the health status of Filipino Americans and recommendations for research. Nurs Outlook 2002;50(1):7-15.
- Gomez SL, Kelsey JL, Glaser SL, Lee MM, Sidney S.
Immigration and acculturation in relation to health and health-related
risk factors among specific Asian subgroups in a health maintenance
organization. Am J Public Health 2004;94(11):1977-84.
- U.S. Department of Health and Human Services. Healthy People 2010: national health promotion and disease prevention objectives. Washington
(DC): U.S. Government Printing Office; 1999.
- Yu SM, Huang ZJ, Singh GK.
Health status and health services utilization among US Chinese, Asian Indian, Filipino, and other Asian/Pacific Islander
children. Pediatrics 2004;113(1 Pt 1):101-7.
- Harris K. The health status and risk behavior of adolescents in immigrant families. In: Hernandez DJ, ed. Children of
immigrants: health, adjustment, and public assistance. Washington (DC): National Academy Press; 1998. p. 286-347.
- Mathews TJ, Menacker F, MacDorman MF.
Infant mortality statistics from the 2002 period: linked birth/infant death data set. Natl Vital Stat Rep 2004;53(10):1-29.
- Fuentes-Afflick E, Hessol NA.
Impact of Asian ethnicity and national origin on infant birth weight. Am J Epidemiol 1997;145(2):148-55.
- Alexander GR, Baruffi G, Mor JM, Kieffer EC, Hulsey TC.
Multiethnic variations in the pregnancy outcomes of military dependents. Am J Public Health 1993;83(12):1721-5.
- Walton DL, Norem CT, Schoen EJ, Ray GT, Colby CJ.
Second-trimester serum chorionic gonadotropin concentrations and
complications and outcome of pregnancy. N Engl J Med 1999;341(27):2033-8.
- Martin JA, Hamilton BE, Sutton PD, Ventura SJ, Menacker F, Munson ML.
Births: final data for 2002. Natl Vital Stat Rep 2003;52(10):1-113.
- Landale NS, Oropesa RS, Gorman BK. Immigration and infant health: birth
outcomes of immigrant and native-born women.
Committee on the Health and Adjustment of Immigrant Children and Families. In: Hernandez DJ, ed. Children of
immigrants: health, adjustment, and public assistance. Washington (DC): National Academy Press; 1998. p. 244-85.
- Alexander GR, Baruffi G, Mor J, Kieffer E.
Maternal nativity status and pregnancy outcome among U.S.-born Filipinos. Soc Biol 1992;39(3-4):278-84.
- Kieffer EC, Martin JA, Herman WH.
Impact of maternal nativity on the prevalence of diabetes during pregnancy among U.S. ethnic groups. Diabetes Care 1999;22(5):729-35.
- Weitz T, Harper C, Mohllajee A. Teen pregnancy among Asians and Pacific Islanders in California:
final report. San Francisco: University of California, San Francisco Center for Reproductive Health Research and Policy; 2001.
- Schumacher LB, Pawson IG, Kretchmer N.
Growth of immigrant children in the newcomer schools of San Francisco. Pediatrics 1987;80(6):861-8.
- Baruffi G, Hardy CJ, Waslien CI, Uyehara SJ, Krupitsky D.
Ethnic differences in the prevalence of overweight among young children in Hawaii. J Am Diet Assoc 2004;104(11):1701-7.
- Greer M, Tengan S. Dental caries in early childhood among Native Hawaiians. Pacific Health Dialog 1998;5(2):332-6.
- Riedy CA, Weinstein P, Milgrom P, Bruss M.
An ethnographic study for understanding children's oral health in a multicultural community. Int Dent J 2001;51(4):305-12.
- Beets MW, Pitetti KH.
One-mile run/walk and body mass index of an ethnically diverse sample of youth. Med Sci Sports Exerc 2004;36(10):1796-803.
- Popkin BM, Udry JR.
Adolescent obesity increases significantly in second and third generation U.S. immigrants: the National Longitudinal Study of Adolescent Health. J Nutr 1998;128(4):701-6.
- Yates A, Edman J, Aruguete M.
Ethnic differences in BMI and body/self-dissatisfaction among Whites, Asian subgroups, Pacific Islanders, and African-Americans. J Adolesc Health 2004;34(4):300-7.
- Robinson TN, Chang JY, Haydel KF, Killen JD.
Overweight concerns and body dissatisfaction among third-grade children:
the impacts of ethnicity and socioeconomic status. J Pediatr 2001;138(2):181-7.
- Gordon-Larsen P, McMurray R, Popkin B.
Adolescent physical activity and inactivity vary by ethnicity: The National Longitudinal Study of Adolescent Health.
J Pediatr 1999;135(3):301-6.
- California Department of Health Services. Asthma in Schools: Results from the California Healthy Kids Survey, 2001-2003. California Asthma Facts 2004;2(3).
- Nelson LJ, Schneider E, Wells CD, Moore M.
Epidemiology of childhood tuberculosis in the United States, 1993-2001: the need for continued vigilance. Pediatrics 2004;114(2):333-41.
- Pong AL, Anders BJ, Moser KS, Starkey M, Gassmann A, Besser RE.
Tuberculosis screening at 2 San Diego high schools with high-risk populations. Arch Pediatr Adolesc Med 1998;152(7):646-50.
- Stevens CE, Toy PT, Tong MJ, Taylor PE, Vyas GN, Nair PV, et al.
Perinatal hepatitis B virus transmission in the United States. Prevention by passive-active immunization.
JAMA 1985;253(12):1740-5.
- Jenkins CN, Buu C, Berger W, Son DT.
Liver carcinoma prevention among Asian Pacific Islanders. Getting hepatitis B shots into arms. Cancer 2001;91(1 Suppl):252-6.
- Grunbaum JA, Lowry R, Kann L, Pateman B.
Prevalence of health risk behaviors among Asian American/Pacific Islander high school students. J Adolesc Health 2000;27(5):322-30.
- Horan PF, DiClemente RJ.
HIV knowledge, communication, and risk behaviors among white, Chinese-, and Filipino-American adolescents in a high-prevalence AIDS epicenter: a comparative analysis. Ethn Dis 1993;3(2):97-105.
- Chung PJ, Borneo H, Kilpatrick SD, Lopez DM, Travis R, Lui C Jr, et al.
Parent-adolescent communication about sex in Filipino American families: a demonstration of community-based participatory research. Ambul Pediatr 2005;5(1):50-5.
- Maxwell AE, Bastani R, Warda US.
Knowledge and attitudes toward condom use — do they predict behavior among Filipino Americans? Ethn Dis 2000;10(1):113-24.
- Wong MM, Klingle RS, Price RK.
Alcohol, tobacco, and other drug use among Asian American and Pacific Islander Adolescents in California and Hawaii. Addict Behav 2004;29(1):127-41.
- Chen X, Unger JB, Cruz TB, Johnson CA.
Smoking patterns of Asian-American youth in California and their relationship with acculturation. J Adolesc Health 1999;24(5):321-8.
- Nemoto T, Aoki B, Huang K, Morris A, Nguyen H, Wong W.
Drug use behaviors among Asian drug users in San Francisco. Addict Behav 1999;24(6):823-38.
- Otsuki TA.
Substance use, self-esteem, and depression among Asian American adolescents. J Drug Educ 2003;33(4):369-90.
- Hartz DT.
Comparative conflict resolution patterns among parent-teen dyads of four ethnic groups in Hawaii. Child Abuse Negl 1995;19(6):681-9.
- Edman JL, Andrade NN, Glipa J, Foster J, Danko GP, Yates A, et al.
Depressive symptoms among Filipino American adolescents. Cult Divers Ment Health 1998;4(1):45-54.
- Rumbaudt RG. The crucible within: ethnic identity, self-esteem, and
segmented assimilation among children of immigrants. In: Portes A, editor. The
new second generation. New York (NY): Russel Sage Foundation; 1996. p. 119-70.
- Wolf D. Family secrets: transnational struggles among children of Filipino
immigrants. Sociol Perspect 1997;40(3):457-82.
- Sloan NR.
Ethnic distribution of diabetes mellitus in Hawaii.
JAMA 1963;183:419-24.
- Ryan C, Shaw R, Pliam M, Zapolanski AJ, Murphy M, Valle HV, et al.
Coronary heart disease in Filipino and Filipino-American patients: prevalence of risk factors and outcomes of treatment. J Invasive Cardiol 2000;12(3):134-9.
- Klatsky AL, Armstrong MA.
Cardiovascular risk factors among Asian Americans living in northern California. Am J Public Health 1991;81(11):1423-8.
- Stavig GR, Igra A, Leonard AR.
Hypertension and related health issues among Asians and Pacific Islanders in California. Public Health Rep 1988;103(1):28-37.
- Grandinetti A, Chang HK, Theriault A, Mor J.
Metabolic syndrome in a multiethnic population in rural Hawaii. Ethn Dis 2005;15(2):233-7.
- Novotny R, Davis J, Ross P, Wasnich R.
Adiposity and blood pressure in a multiethnic population of women in Hawaii. Ethn Health 1998;3(3):167-73.
- Araneta MR, Wingard DL, Barrett-Connor E.
Type 2
diabetes and metabolic syndrome in Filipina-American women : A high-risk nonobese population. Diabetes Care 2002;25(3):494-9.
- Halfon N, Hochstein M.
Life course health development: an integrated framework for developing health, policy, and research. Milbank Q 2002;80(3):433-79.
- Wise P.
The
transformation of child health in the United States. Health Aff
(Millwood) 2004;23(5):9-25.
- Anderson JN.
Health and illness in Pilipino immigrants. West J Med 1983;139(6):811-9.
- Fuligni AJ.
Authority, autonomy, and parent-adolescent conflict and cohesion: a study of adolescents from Mexican, Chinese, Filipino, and European backgrounds. Dev Psychol 1998;34(4):782-92.
- Javier JR, Chamberlain L, Huffman L, Mendoza F.
Filipino American families and intergenerational communication about sex. Ambul Pediatr 2006;6(2):120.
- Richardson LP, DiGiuseppe D, Garrison M, Christakis DA.
Depression in Medicaid-covered
youth: differences by race and ethnicity. Arch Pediatr Adolesc Med 2003;157(10):984-9.
- Bui KV, Takeuchi DT.
Ethnic minority adolescents and the use of community mental health care services. Am J Community Psychol 1992;20(4):403-17.
- Yamada S, Caballero J, Matsunaga DS, Agustin G, Magana M.
Attitudes regarding tuberculosis in immigrants from the Philippines to the United States. Fam Med 1999;31(7):477-82.
- Tompar-Tiu A, Sustento-Seneriches J. Depression and other mental
health issues: the Filipino American experience. San Francisco (CA): Jossey-Bass Publishers; 1995.
- Ghosh C.
Healthy People 2010 and Asian Americans/Pacific Islanders: defining a baseline of information. Am J Public Health 2003;93(12):2093-8.
- Dela Cruz FA, Padilla GV, Agustin EO.
Adapting a measure of acculturation for cross-cultural research. J Transcult Nurs 2000;11(3):191-8.
- Hishinuma ES, Miyamoto RH, Nishimura ST, Nahulu LB, Andrade NN, Makini
GK Jr, et al.
Psychometric properties of the state-trait anxiety inventory for Asian/Pacific-islander adolescents. Assessment 2000;7(1):17-36.
- Edman JL, Danko GP, Andrade N, McArdle JJ, Foster J, Glipa J.
Factor structure of the CES-D (Center for Epidemiologic Studies Depression Scale) among Filipino-American adolescents. Soc Psychiatry Psychiatr Epidemiol 1999;34(4):211-5.
- Srinivasan S, Guillermo T.
Toward improved health: disaggregating Asian American and Native Hawaiian/Pacific Islander data. Am J Public Health 2000;90(11):1731-4.
- Cardiovascular risk in the Filipino community, formative research from
Daly City and San Francisco, California. Washington (DC): U.S.
Department of Health and Human Services, National Institutes of Health; 2003.
- Minkler M, Wallerstein N, editors. Community-based participatory
research for health. San Francisco (CA): Jossey-Bass; 2003.
- Computer Retrieval of Information on Scientific Projects (CRISP)
Database. Bethesda (MD): National Institutes of Health, Office of
Extramural Research;[cited 2006 May 31]. Available from: http://crisp.cit.nih.gov
- Huang L, Lee Y, Arganza G. Promising approaches in youth development and
risk prevention for Asian American/Pacific Islander youth: voices from the
field. Washington (DC): Georgetown University Center for Child and Human Development; 2004.
- Yancey AK, Siegel JM, McDaniel KL.
Role models, ethnic identity, and health-risk behaviors in urban adolescents. Arch Pediatr Adolesc Med 2002;156(1):55-61.
- Coll CG, Szalacha LA. The multiple contexts of middle childhood. The
Future of Children: Children of Immigrant Families 2004;14(2):81-97.
- Brown ER, Holtby S, Zahnd E, Abbott GB.
Community-based participatory research in the California Health Interview Survey. Prev Chronic Dis
[serial online] 2005 Oct.
- Tervalon M, Murray-Garcia J.
Cultural humility versus cultural competence: a critical distinction in
defining physician training outcomes in multicultural education. J Health Care Poor Underserved 1998;9(2):117-25.
-
Culturally effective pediatric care: education and training issues. American Academy of Pediatrics Committee on Pediatric Workforce. Pediatrics 1999;103(1):167-70.
Back to top
|
|
