

|

|

Volume
3:
No. 2, April 2006
LETTER TO THE EDITOR
Using Pedometers to Promote Physical Activity Among Working Urban Women
Suggested citation for this article: Garbers S, Nelson JA, Rosenberg T, Chiasson MA. Using pedometers to promote physical activity among working urban women [letter to the editor]. Prev Chronic Dis [serial online] 2006 Apr [date cited]. Available from: URL: http://www.cdc.gov/pcd/issues/2006/
apr/05_0157.htm.
PEER REVIEWED
To the Editor:
In light of recent research showing that the prevalence of overweight and obesity among American men and women has reached 65% (1), scientific and media attention has been increasingly focused on ways to address this epidemic. One approach has been to increase Americans’ physical activity levels, because even a moderate increase in physical activity may prevent weight gain (2). Evidence,
including the study by Wilson et al recently published in Preventing Chronic Disease (3), suggests that walking-based programs, particularly those incorporating pedometers, may be an effective way to increase individuals’ physical activity levels (4). As a first step toward implementing a similar program among urban working women — who face numerous barriers to structured
physical activity — a project was undertaken with two goals. The first goal was to compare the performance of two pedometer models:
a low-cost maternal and child health (low-cost MCH),
which costs $2.90 and is marketed to maternal child health programs, and a Consumer Reports
best buy (CR best buy),
which costs $20.00 and was rated by Consumer Reports
as a best buy for accuracy, ease of use, and value (5). The second goal was
to determine the real-life feasibility of pedometer use among working urban women.
Participants were recruited through workplace-based e-mail and flyer postings at public health project sites of a large public health organization in New York City in March and April 2005. Women of any age who worked full time or part time at participating projects and had no physical limitations that would require the use of special equipment, such as a wheelchair or cane, were eligible to
participate in the study. The protocol and data collection materials for the internally funded study were approved by the Medical and Health Research Association’s
institutional review board.
Of the 30 women who agreed to participate in the study and completed the baseline survey, two did not provide any information on their pedometer use and were excluded from this analysis (n = 28). Participants were asked to wear two pedometers — one on each hip — every day for 6 days, to record
on a preformatted daily log sheet the number of steps measured by each pedometer, and to track any problems with use, such
as forgetting, dropping, or losing the pedometers. Participants were told that they did not have to increase their physical activity for the study.
The Table summarizes the
participants’ characteristics.
Half of the participants (n = 14) did not wear the pedometers on at least 1 day; from a total of 168 user-days in the study, pedometers were worn on 133 user-days (79% of all days). The most common reasons for not wearing the pedometers were forgetting (28 user-days), losing the pedometers (4 user-days), and wearing a dress (3 user-days). The low-cost MCH pedometer functioned on only 80 user-days,
representing 60% of user-days worn, while the CR best-buy pedometer functioned on all days worn. Counts on both pedometers were accidentally reset on approximately 10% of user-days worn. The low-cost MCH pedometer fell off or was dropped more frequently than the
CR best-buy model (7% versus 2% of user-days worn). In all instances of
resetting or dropping, the pedometers continued to measure steps throughout the
day. Although the difference between the two models in mean daily step counts for the
6-day study period was only 75 steps, on 45% of the 78 days on which both models were worn and functioning, the daily step counts differed between
the two models by more than 2000 steps (Figure). Using measurements from the
CR best-buy model, we found that fewer than 12% of participants achieved
the popularly cited goal of 10,000 steps per day (6), and more than half had
fewer than 5000 steps per day. As shown in the Table, women who drive to work
took significantly fewer steps per day compared with women who ride the subway,
train, or bus, and women who mostly sit or stand at work took significantly
fewer steps per day compared with women who mostly walk at work. One-way
analysis of variance [ANOVA] was used to compare means.
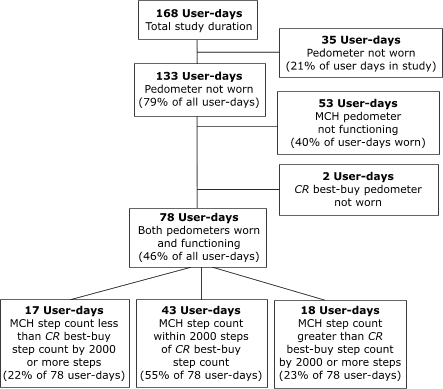
Figure. Summary of low-cost maternal and child
health (MCH) pedometer model performance compared with Consumer Reports
(CR) best-buy model performance. [A text description of this chart is also available.]
In this study, the low-cost MCH pedometer model was found to be largely ineffective. Although the CR best-buy model was more reliable in terms of user-days functioning,
developers of walking programs using pedometers need to
consider cost in addition to reliability. In this study, the benefit of keeping costs low was offset by the poor functioning of the low-cost MCH
pedometer model. Programs should carefully evaluate the reliability of any
pedometer before use in an intervention.
This study had the following limitations: all participants were employees of
a large public health organization and may have been more aware of physical
activity interventions; the data were collected through self-report; and
participants were not asked to change their physical activity, unlike
participants in an intervention program. This feasibility study revealed some
difficulties in the day-to-day use of pedometers, including the pedometers not
being worn and accidentally resetting counts. The high proportion of women who
forgot to wear the pedometer on at least 1 day during the short study duration
of 6 days (50%) suggests that programs using pedometers to promote physical
activity must also incorporate motivational techniques and reminders for
participants.
Samantha Garbers, MPA
Medical and Health Research Association of New York City, Inc
New York, NY
Jennifer A. Nelson, MPH
Medical and Health Research Association of New York City, Inc
New York, NY
Terry Rosenberg, PhD
Medical and Health Research Association of New York City, Inc
New York, NY
Mary Ann Chiasson, DrPH
Medical and Health Research Association of New York City, Inc
New York, NY
Back to top
References
- Hedley AA, Ogden CL, Johnson CL, Carroll MD, Curtin LR, Flegal KM. Prevalence of
overweight and obesity among US children, adolescents, and adults, 1999-2002. JAMA 2004;291(23):2847-50.
- Hill JO, Wyatt HR, Reed GW, Peters JC. Obesity and the
environment: where do we go from here? Science 2003;299:853-5.
- Wilson DB, Porter JS, Parker G, Kilpatrick J.
Anthropometric changes using a walking intervention in African American breast cancer survivors: a pilot study.
Prev Chronic Dis [serial
online] 2005 Apr.
- Croteau KA.
A preliminary study on the impact of a pedometer-based intervention on
daily steps. Am J Health Promot 2004;18(3):217-20.
- Consumer Reports pedometers:
walking by the numbers. Yonkers (NY): Consumers Union of U.S., Inc; 2004
Oct.
- Tudor-Locke C, Bassett DR.
How many steps/day are enough? Preliminary pedometer indices for public health. Sports Med 2004;34(1):1-8.
Back to top
Table
 Table. Characteristics and Pedometer Use of Participants in
a Study to Promote Physical Activity Among Working Urban Women (n = 28)a Table. Characteristics and Pedometer Use of Participants in
a Study to Promote Physical Activity Among Working Urban Women (n = 28)a
| Characteristics |
% of
Participants |
Mean Daily Steps (95% CI)b |
P Value |
| Age, y |
| ≤39 |
54 |
5762 (3989-7536) |
.47 |
| ≥40 |
46 |
4812 (2573-7052) |
| Race or ethnicity |
| Latina |
43 |
6548 (4087-9010) |
.14 |
| Black, non-Hispanic |
29 |
3451 (1915-4988) |
| White, non-Hispanic |
21 |
5080 (493-9666) |
| Asian, non-Hispanicc |
7 |
— |
|
Body mass index |
| Normal (18.5-24.9) |
43 |
5791 (3220-8362) |
.10 |
| Overweight (25.0-29.9) |
25 |
6909 (3589-10228) |
| Obese (≥30.0) |
32 |
3572 (2235-4909) |
| Children in household |
| At least one child (aged <18 y) in household |
57 |
4740 (3519-5961) |
.36 |
| No child in household |
43 |
6005 (3319-8692) |
| Work setting |
| Sedentary (mostly sitting or standing) |
82 |
4548 (3550-5547) |
.002 |
| Mostly walking |
18 |
9590 (1761-17419) |
| Usual mode of commuting to work |
| Drive
automobile |
36 |
3302 (2000-4605) |
.009 |
| Ride
train, subway, or bus |
64 |
6587 (4799-8376) |
| Study
compliance |
| Wore both pedometers all 6 daysd |
50 |
5039 (3167-6910) |
.64 |
| Forgot to wear pedometers at least 1 day |
50 |
5657 (3506-7808) |
|
aComparison of means excludes participants who did not wear pedometers on any day.
One-way analysis of variance (ANOVA) was used to compare means.
bCI indicates confidence interval.
cAsian participants were excluded from comparison of means
because of small sample size (n = 2).
dIncludes days when pedometers were worn but not functioning; excludes days when pedometer was forgotten, lost, or not worn because participant wore a dress.
Back to top
|
|
