

|

|

Volume 2: No.
4, October 2005
ORIGINAL RESEARCH
The Effect of Two Church-based Interventions on Breast Cancer
Screening Rates Among Medicaid-Insured Latinas
Adrienne L. Welsh, PhD, MSPH, Angela Sauaia, MD, PhD, Jillian Jacobellis,
PhD, MS, Sung-joon Min, PhD, Tim Byers, MD, MPH
Suggested citation for this article: Welsh AL, Sauaia A, Jacobellis
J, Min S, Byers T. The effect of two church-based interventions on
breast cancer screening rates among Medicaid-insured Latinas. Prev Chronic Dis
[serial online] 2005 Oct [date cited]. Available from: URL:
http://www.cdc.gov/pcd/issues/2005/
oct/04_0140.htm.
PEER REVIEWED
Abstract
Introduction
Latinas face disparities in cancer screening rates compared with non-Latina
whites. The Tepeyac Project aims to reduce these disparities by using a
church-based approach to increase breast
cancer screening among Latinas in Colorado. The objective of this study was
to compare the effect of two Tepeyac Project interventions on the mammogram
rates of Latinas and non-Latina whites enrolled in the Medicaid
fee-for-service program.
Methods
Two intervention groups were compared: 209 churches in Colorado that
received educational printed materials in Spanish and English (the printed statewide
intervention) and four churches in the Denver area that received
personalized education from promotoras,
or peer counselors (the promotora
intervention), in addition to the printed statewide intervention. Biennial Medicaid mammogram claim rates in Colorado before the
interventions (1998–1999) and after (2000–2001) were used to compare the
effect of the interventions on mammogram use among Latinas and non-Latina
whites aged 50 to 64 years who were enrolled in the Medicaid fee-for-service
program. Adjusted rates were computed using generalized estimating equations.
Results
Small, nonsignificant increases in screening were observed among Latinas
exposed to the promotora intervention (from 25% at baseline to 30% at
follow-up [P = .30]) as compared with 45% at baseline and 43% at
follow-up for the printed statewide intervention (P = .27). Screening
among non-Latina whites increased by 6% in the promotora intervention
area (from 32% at baseline to 38% at follow-up [P = .40]) and by 3% in
the printed statewide intervention (from 41% at baseline to 44% at follow-up [P
= .02]). No significant disparities in breast cancer screening were detected
between Latinas and non-Latina whites. After adjustment for the confounders by
generalized estimating equations, the promotora intervention had a
marginally greater impact than the printed statewide intervention in
increasing mammogram use among Latinas (generalized estimating equation, P
= .07).
Conclusion
A personalized community-based education was only modestly effective in
increasing breast cancer screening among Medicaid-insured Latinas. Education
alone may not be the answer for this population. The barriers for these
Medicaid enrollees must be investigated so that interventions can be tailored
to address their needs.
Back to top
Introduction
Disparities in mammogram screening rates have been identified among
Latinas, the poor, and those with lower levels of education (1-3). Personal
beliefs and practices, access to medical care, low income, and language issues
(4-6) are common barriers for people with low use of cancer screening
services. Studies conducted specifically with Latinas have identified cultural
barriers to obtaining these services, such as “fatalismo,” difficulties with
acculturation, fear, and embarrassment (7-9). Barriers found to be associated
with lack of breast cancer screening among low-income women include older age,
low level of education, lack of health insurance, work-related obligations,
transportation issues, and lack of recent physician visits (10). Interventions
used in the general population aimed at increasing the rates of mammogram
screening, such as media campaigns and chart reminders, have shown little
effectiveness among Latinas (11,12). Church-based interventions and the use of
peer counselors are two recent
promising approaches to reaching the Latina community (12-14).
This study describes a pilot project aimed at increasing breast cancer
screening among Latinas in Colorado through two church-based interventions.
The Colorado Foundation for Medical Care (CFMC) conducted the study with
funding from the Centers for Medicare & Medicaid Services (CMS), formerly
the Health Care Financing Administration. The study objective was to compare
the effect of the two interventions on the mammogram rates of Latinas and non-Latina
whites (NLWs) enrolled in the Medicaid fee-for-service program.
To ensure that the interventions in this pilot study were culturally
appropriate, the involvement of the community was sought in all phases of the
project. The project was named Tepeyac because of its importance to Latinos as
the site in Mexico where Our Lady of Guadalupe appeared to Saint Juan Diego.
The interventions incorporated themes identified by the community, such as the
importance of family, and were delivered through the
Catholic church,
an integral part of the Latino social network.
This report is the second in a series that examines the impact of the
Tepeyac interventions on the mammogram screening rates among Latinas and NLWs
enrolled in Medicare, Medicaid, and health maintenance organizations (HMOs).
The Tepeyac project has previously demonstrated success in decreasing the
disparity between older Latinas and NLWs enrolled in the Medicare
fee-for-service program (15). This analysis focuses on
the effect of these interventions on younger women covered by the Medicaid
fee-for-service program, an optimal vehicle for evaluating education
initiatives in this high-risk, low-income group.
Back to top
Methods
This study has a quasi-experimental design comprised of two groups: 1) 209
Catholic churches that received a printed statewide intervention (PSI), and 2)
four Catholic churches in the Denver area that received a promotora
(peer counselor) intervention (PI) in addition to the PSI. The PSI entailed
the display of bilingual printed materials about breast cancer screening in
the churches with possible delivery of bilingual short messages to
parishioners through the pulpit, church bulletin, or both. The 209 churches that received this
intervention were included in the PSI group in an intent-to-treat analysis.
The PI entailed education about breast cancer
screening delivered in person by promotoras.
Implementation of interventions
Printed statewide intervention (PSI)
Focus groups were held with organizations
serving Latinas to review published information about barriers Latinas face in
obtaining mammograms. The focus groups identified and confirmed the following
barriers faced by Latinas: lack of access to care, modesty, and lack of time
because of primary role
as family caretaker. Previously identified barriers in the literature, such
as strong sense of family (13,16), were also confirmed. Materials for the
intervention printed by the National Cancer Institute (NCI) reflected the
pre-identified theme of a sense of family with the chosen message, “Do it
for you. Do it for your family.” The materials were enhanced by adding
contact information for the local Colorado Women’s Cancer Control Initiative (CWCCI),
a program administered by the Colorado Department of Public Health and
Environment and funded by the Centers for Disease Control and Prevention
(CDC). The CWCCI provides referrals and free mammograms to eligible
women.
After an initial contact by the archdioceses, the churches were mailed an
intervention package containing a letter describing the Tepeyac Project;
the NCI educational materials about breast cancer screening; a display unit;
short camera-ready messages in English and Spanish to be delivered from the pulpit, published in the church bulletins,
or both; and a fax–back form asking at
which level they would agree to participate (display materials, publish
messages, deliver messages from pulpit). The first mailing to all churches
in the state occurred in March 2000, a second in
October 2000, and a third in February 2001. The second
and third mailings included issues of the Tepeyac Project newsletter
(available from www.cfmc.org) (15). Information about the level of church participation was obtained by phone
call, personal visit, or fax after the first mailing and was available for 154 (72%)
of the 213 participating churches (209 in the PSI and 4 in the PI). Of the 154
churches, 61 (40%) displayed the printed materials, 8 (5%) published
messages in the bulletin, and 85 (55%) did both. In addition to these
activities, 18 (12%) made pulpit announcements. The level of participation was
undetermined at 47 churches, and 12 churches declined to participate.
Promotora intervention (PI)
The four churches that received the PI are all in the Denver area. The promotoras
selected these churches because the parishioners and priests had expressed
interest in having them come and educate women. The churches, located in
largely Hispanic areas, are central reference points to Latinos in Colorado.
The PI was an expansion of a pre-existing community-based
intervention initiated by La Clinica Tepeyac that provides health care to the
local underserved Hispanic population. Each promotora was trained
using a standardized curriculum developed by La Clinica Tepeyac and assigned a
specific church to visit monthly. Promotoras approached their peers after Sunday masses and
during church fairs and other church-related activities. La Clinica Tepeyac
coordinated the promotoras’ work and paid their salaries. The promotoras also
facilitated health groups, or platicas, where a group of women met at
one another’s houses to discuss breast health. This intervention
started in 2000 and is ongoing.
Reach of interventions
According to parish register data from the Archdiocese of Denver, the size
of the congregations in the four parishes that received the PI varied from
1950 to 5000 total parishioners, of whom 32% to 84% were Latinos, for a
potential of 9427 Latino parishioners reached by the PI. Also based on these parish
register data, we estimate that the PSI reached a minimum of 349,340
parishioners, of whom 34,419 were Latinos (with an average church size of 3235
parishioners). Latinos are less likely to register than whites; therefore,
these numbers are likely to underestimate the number of Latinos potentially
reached by these church-based interventions (17).
Study population
The eligibility criteria for this study were: women aged 50 to 64 years,
enrolled in the Colorado Medicaid fee-for-service health insurance program
(not enrolled in an HMO), and enrolled for more than 18 months (continuously
or as a sum of individual enrollment periods) during the baseline period
January 1998 through December 1999 and similarly during the follow-up period January 2000
through December
2001. Subjects enrolled in a primary care case management (PCCM) program
reimbursed by fee-for-service were included in the database for
analysis.
Exposure to the PI or PSI among study subjects was determined by zip codes.
Women in the study living in the three zip codes of the four churches visited
by the promotoras were assumed to be exposed to the PI, whereas
women living in remaining zip codes were assumed to be exposed to the PSI.
While using zip codes to assess the intervention effects may be a
methodological limitation, many churches do not release individual-level
parish membership data, as it is potentially damaging to the trusting
relationship required to implement this intervention. According to the
Archdiocese of Denver’s Hispanic Ministry, a large proportion of Latinos
attend their neighborhood church (i.e., in the same zip code) because of a
recent increase in the number of churches offering masses in Spanish.
Mammogram screening rates
Mammogram claims obtained from Medicaid fee-for-service administrative data
were used for the analysis. We compared the rates obtained during the baseline
period before the intervention (January 1998–December 1999) with those
obtained during a follow-up period (January 2000–December 2001) for
Medicaid-enrolled women in each of the intervention groups.
Mammogram use was determined by having the claims with any of the following
codes: International Classification of Diseases, Ninth Revision, Clinical
Modification (ICD-9-CM) procedure codes 87.36, 87.37, or diagnostic
code V76.1X; Healthcare Common Procedure Coding System (HCPCS) codes GO202,
GO203, GO204, GO205, GO206, or GO207; Current Procedural Terminology (CPT)
codes 76085, 76090, 76091, or 76092; and revenue center codes 0401, 0403,
0320, or 0400 in conjunction with breast-related ICD-9-CM diagnostic
codes of 174.x, 198.81, 217, 233.0, 238.3, 239.3, 610.0, 610.1, 611.72, 793.8,
V10.3, V76.1x.
The outcome variable was mammography screening status as determined by the
above codes. The main predictors were ethnicity as determined by the
Passel-Word Spanish surname algorithm (18), time (baseline and follow-up), and
the interventions. The covariates collected from Medicaid administrative data
were date of birth (to determine age); total length of time on Medicaid
(determined by summing lengths of time spent within dates of enrollment);
length of time on Medicaid during the study periods (determined by summing
only the lengths of time spent within dates of enrollment corresponding to
study periods); number of spans of Medicaid enrollment (a span defined as a
period of time spent within one enrollment date to its corresponding disenrollment date); Medicare–Medicaid dual eligibility status; and reason
for enrollment in Medicaid. Reasons for enrollment in Medicaid were grouped by
categories of aid, which were: 1) old age pension, for persons aged 60 to 64;
2) disabled or blind, representing those with disabilities, along with a small
number of refugees combined into this group because of similar mammogram
screening rates; and 3) those receiving Aid to Families with Dependent
Children (AFDC).
Statistical analysis
The chi-square test or Fisher exact test (for cells with expected values
less than 5) was used for categorical variables, and ANOVA testing was used on
continuous variables with the Welch modification when the assumption of
similar variances did not hold. An analysis with generalized estimating
equations (GEE) was conducted to determine intervention effects on mammogram
screening before and after intervention while adjusting for differences in
demographic characteristics, dual Medicare–Medicaid eligibility, total
length of time on Medicaid, length of time on Medicaid during the study
periods, and number of Medicaid spans enrolled. GEE analysis accounted for
clustering by enrollees who were present in both baseline and follow-up time
periods. About 69% of the PI enrollees and about 67% of the PSI enrollees were
present in both time periods.
GEE models were used to directly compare PI and PSI areas on trends in
mammogram screening among each ethnic group. The hypothesis for this model was
that for each ethnic group, the PI was associated with a larger increase in
mammogram rates over time than the PSI. To test this hypothesis, the following
two statistical models were used (one for Latinas, one for NLWs):
Logit P = a + β1time (follow-up vs baseline) + β2intervention (PI vs PSI)
+ β3 (time*intervention) + β4…n (covariates),
where “P” is the probability of having a mammogram, “a” is the
intercept, “β1” is the parameter estimate for time, “β2” is
the parameter estimate for the intervention, and “β3” is the
parameter estimate for the interaction between time and intervention. A
positive significant interaction term suggests that the PI had a greater
impact on mammogram screening over time than the PSI among that ethnic
group.
An analysis was also conducted to measure the effect of each of the
interventions on reducing the disparity of mammogram screenings between ethnic
groups. This analysis involved creating two separate models for each of the
interventions (PI and PSI) to test two hypotheses: 1) Among women exposed to
the PI, screening disparity between Latinas and NLWs is smaller at follow-up
than at baseline; and 2) Among women exposed to the PSI, screening disparity
between Latinas and NLWs is smaller at follow-up than at baseline. The two
statistical models used (one for the PI, one for the PSI) were:
Logit P = a + β1time (follow-up vs baseline) + β2ethnicity (Latina vs NLW)
+ β3 (time*ethnicity) + β4…n (covariates),
where “P” is the probability of having a mammogram, “a”
is the intercept, “β1” is the parameter estimate for time, “β2” is the
parameter estimate for ethnicity, and “β3” is the parameter estimate for the
interaction between time and ethnicity. A significant, positive two-way
interaction would indicate that for each intervention, mammogram screening improvement (before and after) was significantly greater
in Latinas than in NLWs.
Back to top
Results
Study subjects
The baseline period included 16,277 women aged 50 to 64, of whom 5865 (36%)
were enrolled in Medicaid HMO and subsequently removed, leaving 10,412 with
fee-for-service reimbursements for analysis. Analyses were restricted to the
6696 (64%) women enrolled in Medicaid fee-for-service longer than 18 months
(Table 1). Latinas represented 22% of this Medicaid population, whereas NLWs
represented 57%. More than half of the enrollees in this database (59%) were
disabled, a small minority (2%) received AFDC, with the remaining receiving
old age pensions (39%). The disabled category consisted of enrollees with
disabilities and enrollees who are blind. The majority of enrollees receiving old age pensions and the
majority of disabled enrollees were dually eligible for Medicare and Medicaid,
in contrast to those receiving AFDC, where the majority were eligible for
Medicaid only. Sixty percent did not have any mammogram procedure during the
baseline study period. Similar characteristics were observed in the follow-up
study population (data not shown).
The baseline demographic characteristics of the study population by
intervention region and ethnicity are shown in Table 2. Latinas were significantly older than NLWs in both intervention areas
(P = .002 for the PI, P <.001 for the PSI) and significantly less likely
to be dually eligible for Medicare and Medicaid in the PSI (P <
.001). In the follow-up time period, similar observations were made (data not
shown).
Mammogram rates
The crude biennial mammogram rates for Latinas and NLWs enrolled in
Medicaid during the
baseline and follow-up periods by intervention are shown in Figure 1 and
Table
3. In the PI region, follow-up mammogram rates for both Latinas and NLWs
slightly increased over time, from 25% to 30% for Latinas (unadjusted GEE, P
= .30) and from 32% to 38% for NLWs (unadjusted GEE, P = .40); however,
this difference was not statistically significant compared with baseline rates.
No significant disparities in mammogram rates were observed in either time
period, regardless of intervention group, although Latinas had slightly lower
rates in the PI area. In the PSI area, follow-up mammogram rates for Latinas
remained unchanged when compared with baseline rates (45% in baseline compared
with 43% in follow-up [unadjusted GEE, P = .27]). NLWs in the PSI
demonstrated a significant increase in mammogram rates over time (41% in
baseline compared with 44% in follow-up [unadjusted GEE, P = .02]). Latinas in the PSI had significantly higher
mammogram rates than NLWs in the baseline period only (chi-square test, P = .02).
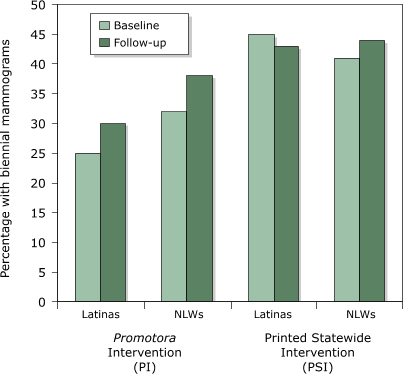
Figure 1. Unadjusted Medicaid biennial mammogram
rates in Colorado by intervention during baseline (January 1998–December 1999) and follow-up (January 2000–December 2001) periods
for Latinas and non-Latina whites (NLWs). [A
tabular version of this chart is also
available.]
The GEE analysis directly compared the effects of the interventions on
mammogram screening rates for each ethnic group. There was a marginally
significant positive interaction term between time and intervention (adjusted
GEE, P = .07), suggesting that the PI was more effective than the PSI in increasing
mammogram screening among Latinas (Figure 2). Among NLWs, the PI
was associated with increases in mammogram screening over time (adjusted GEE, P
= .10) (Figure 3). These results suggest that the PI was the only intervention
in which Latinas demonstrated modest increases in mammogram screening
rates.
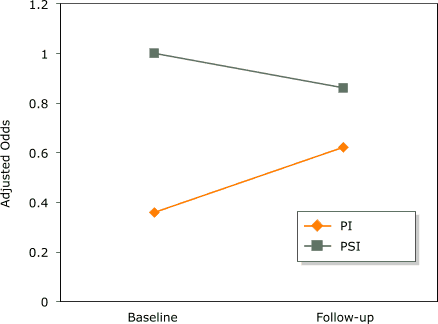
Figure 2. Adjusted odds of having a mammogram during
baseline (January 1998–December 1999) and follow-up (January 2000–December 2001) periods by intervention for Latinas
insured by Medicaid in Colorado. Odds calculated using generalized estimating
equations (GEE) (interaction time x intervention, P = .07). PI
indicates promotora intervention; PSI,
printed statewide intervention. [A tabular version of
this graph is also available.]
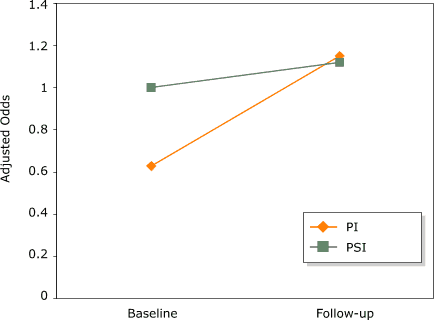
Figure 3. Adjusted odds of having a mammogram during
baseline (January 1998–December 1999) and follow-up (January 2000–December 2001) periods
by intervention for non-Latina whites (NLWs) insured
by Medicaid in Colorado. Odds calculated using generalized estimating equations
(GEE) (interaction time x intervention, P = .10). PI indicates
promotora intervention; PSI, printed
statewide intervention. [A tabular version of this
graph is also available.]
GEE was also used to determine the effect of each intervention on mammogram
disparity between Latinas and NLWs. No significant ethnic disparities in
screening were observed in the PI regions. Although Latinas residing in the PI
regions had less screening than NLWs, the difference was not statistically
detectable (adjusted GEE, P = .19). The improvement in the PI region
among Latinas did not entail a statistically significant difference (adjusted GEE, P = .90).
Interestingly, Latinas in the PSI initially had higher mammogram screening
rates than NLWs (adjusted GEE, P = .03). Only the PSI group had a
negative significant two-way interaction between time and ethnicity due to an
increase in mammogram rates for NLWs compared with Latinas over time (adjusted
GEE, P = .04 for baseline and adjusted GEE, P = .24 for
follow-up).
An additional analysis excluding the nonparticipating churches in the PSI
showed no significant differences in mammogram rates between nonparticipating
and participating PSI groups in either ethnic group.
Back to top
Discussion
Type of health insurance coverage is an important factor in determining the
use of preventive services (19,20). This report is the second in a series that
examines the effects of the Tepeyac Project, a community-participatory,
church-based educational initiative to increase mammogram screening among
Latinas who have different types of health insurance coverage. The focus of
this paper has been on the publicly funded Medicaid health insurance program.
It is our hope that initiatives that increase use of preventive screening
services among populations with relatively low screening rates may provide
public health benefits and decrease future costs of late-stage detection.
Results from the Tepeyac Project in a Medicare population (15) suggested that a personalized, church-based educational initiative
was more effective than a printed intervention in changing mammogram screening
over time among Latinas. In that population, the PI was associated with a
reduction in screening disparity between Latinas and NLWs, whereas PSI and
control region rates increased slightly but disparity remained unchanged. The
decrease in disparity observed in the PI region was associated with a
significant increase in mammogram rates among Latinas over time after
adjustment for confounders. However, large differences in baseline rates limit
the evaluation.
Screening rates for Medicaid beneficiaries in our study ranged from 25% to
38% in the PI and 41% to 45% in the PSI region. These results are similar to
those reported by the Behavioral Risk Factor Surveillance System (BRFSS)
for women with incomes less than $25,000 in 1998–1999 (3) and the Health Plan
Employer Data and Information Set (HEDIS) for Colorado Medicaid recipients in
2000 (21). Of women with incomes less than $25,000 residing in Colorado, 55%
reported receiving biennial mammogram screenings, whereas HEDIS rates for
Medicaid recipients in Colorado were 52% for PCCM and 36% for fee-for-service.
One report studying the effects of health insurance on cancer detection found
that people insured by Medicaid were more likely to be diagnosed with
late-stage cancer than people with other insurance plans, suggesting low use
of cancer screening (22).
Another potential reason for low mammogram screening rates among our study
population may be the high proportion of participants with disabilities. Results from
several studies report that individuals with disabilities are at increased
risk for not receiving preventive services (23,24). The Department of Health
Care Policy and Financing (HCPF) for the state of Colorado reported in Access
to Preventive Care for the Disabled that the mammogram rate among disabled
women aged 52 to 64 years enrolled in Medicaid was 20% (25).
Our datasets do not include information on whether a woman received a
mammogram outside of the fee-for-service Medicaid system; therefore, we may
have underestimated mammogram rates. Because mammograms may have been paid by
other insurers, we compared the rates of Medicaid enrollees with and without
dual Medicare–Medicaid eligibility status. A lower rate among these dually
eligible subjects would suggest claims were being paid by Medicare. This was
not the case, since dual eligibility status did not affect our screening
rates. Since HEDIS reports of Medicaid fee-for-service are also alarmingly
low, we believe that the screening rates are probably accurate, underscoring
the continuing need for concentrated efforts to increase screening practices
in this population.
A usual source of care has often been cited as a factor influencing
preventive screening practices (6,26). Interestingly, our results found that
one third of Medicaid enrollees obtained mammograms from hospitals, suggesting
a possible lack of a usual source of care. This is consistent with results
reported by McCall and colleagues, where an association was found between
decreased diabetes care and emergency department use in a population of dual
Medicare–Medicaid-eligible elderly (27). This may also have contributed to
low screening rates in our Medicaid population.
Latinas have typically been described in the literature as an ethnic group
at increased risk for not obtaining mammograms and receiving routine screening
when compared with NLWs (2,28). This has been consistent with evidence that
Latinas are diagnosed with later stages of breast cancer (4,29,30). However,
we observed this trend toward screening disparity only in the
lowest-income region of Colorado. Interestingly, our study did not demonstrate
significant disparities in mammogram screening rates between Latinas and NLWs
residing in the rest of Colorado. This observation has also been made in other
studies with low-income populations. Hedegaard and colleagues examined
factors associated with obtaining mammograms among low-income women attending
a community health center in Denver. After controlling for subsidized care and
other variables, little difference in screening rates between racial groups
was found (20). In a more recent study, researchers using data from the National
Health Interview Survey (NHIS) analyzed the contribution of sociodemographic
factors to differences in screening practices between Latinas and NLWs covered
by private health insurance. Latina mammogram screening rates were initially lower than NLW rates; however, after controlling for age, education, and family income,
disparities in mammogram screening between Latinas and NLWs were no longer
significant (31). Similarly, trends in breast cancer and breast cancer
survival observed in Latinas residing in Colorado were largely associated with
poverty (32).
Despite the slight increases in screening observed, the Tepeyac Project
interventions were not associated with large improvements in mammogram
screening rates among Medicaid recipients. Women residing in the PI regions
still remained at higher risk for not obtaining mammogram screening than women
residing in the rest of Colorado. Several study limitations may contribute to
the finding of a lack of significant improvement in screening including lack
of study power, potential underestimation of mammogram claims by Medicaid
fee-for-service, heterogeneity of church intervention, and differences in
baseline rates of mammogram screening between interventions. Some of
these limitations are inherent to community research studies using large
databases. For example, diagnostic codes may be subject to variation and
incompleteness and are originally intended for reimbursement purposes rather
than research (33).
The lack of study power is related to the pilot nature of this study, which
had financial constraints that limited the number of churches reached by the promotora
intervention to four. Another study limitation is that the interventions were
placed in the churches, but the outcomes were measured in the neighborhood
population with the assumption that a church intervention will diffuse into
the community. The qualitative evaluation done by Sauaia et al (15) as part of the Tepeyac Project using eight focus groups across the intervention
regions showed
that Latinas saw the churches as a trusted and convenient place to receive
health messages and voiced a strong preference for personally delivered
education. These findings will be tested by a survey being
conducted in the neighborhood surrounding the churches that will allow for a
measure of exposure to the intervention among Latinas as well as further
characterization of how this intervention addresses barriers to preventive
health care that they encounter.
In addition, the printed materials have been improved in Phase II of the Tepeyac
Project, with development of new, locally produced
printed materials reflecting local community barriers, language, and
misconceptions. Future research should also evaluate the effect of having paid
versus volunteer promotoras and the feasibility of a randomized
controlled trial to overcome some of the study design issues experienced in
this pilot study.
However, more important from a policy point of view, our study population
may simply represent a group that is particularly difficult to target for
outreach activities. Low-income women — especially low-income Latinas —
experience multiple barriers that may preclude their participation in
preventive care activities, of which education may be only a small component.
Low-income women have fewer health services available and are more likely to
lack access to available services; low-income women are also more likely to
have physical and comorbid conditions (10). More than half of our study
participants were categorized as either blind or disabled, potentially
limiting exposure to or understanding of the educational interventions. When
mammograms were categorized as either preventive or diagnostic, the majority
of our study population obtained diagnostic mammograms in the baseline period.
This is suggestive of a high prevalence of comorbid conditions, a potential
barrier, among these women.
This pilot study has demonstrated provocative results that should be
discussed and that should generate hypotheses and new research in public
health. To substantially increase preventive care screening, this type of
intervention may need to be combined with other strategies to overcome
significant barriers faced by these women. Successful cancer screening
initiatives targeting Latinas must address not only culturally specific
barriers but also access and broader institutional and societal factors.
Finally, while a randomized controlled trial may pose ethical and logistical
dilemmas quite difficult to overcome, it may be the necessary next step to
evaluate this type of intervention and to address some of the limitations
experienced in this pilot study.
Back to top
Acknowledgments
This study was made possible by the Colorado Department of Health Care
Policy and Financing who provided the Medicaid fee-for-service dataset. The research was supported in part by a grant from the National Cancer
Institute (1RO3CA110820-01).
Back to top
Author Information
Corresponding Author: Angela Sauaia, MD, PhD, Assistant Professor, Division
of Health Care Policy and Research, University of Colorado Health Sciences
Center, 13611 East Colfax Ave, Suite 100, Aurora, CO 80011. Telephone:
303-724-2498. E-mail: Angela.Sauaia@UCHSC.edu.
Author Affiliations: Adrienne L. Welsh, PhD, MSPH, Tim Byers, MD, MPH,
Sung-joon Min, PhD, University of
Colorado Health Sciences Center, Denver, Colo; Jillian Jacobellis, PhD, MS,
Colorado Department of Public Health
and Environment, Denver, Colo.
Back to top
References
- Centers for Disease Control and Prevention. National Health
Interview Survey, 2002. Atlanta (GA): Centers for Disease Control and
Prevention; 2002 [cited 2004 Jan]. Available from: URL: www.cdc.gov/nchs/nhis.htm.
- Wells BL, Horm JW.
Targeting the underserved for breast and
cervical cancer screening: the utility of ecological analysis using the
National Health Interview Survey. Am J Public Health 1998;88(10):1484-9.
- Colorado Department of Public Health and Environment.
Behavioral Risk Factor Surveillance System. Denver (CO):
Colorado Department of Public Health and Environment; 2004 [cited 2004 Jul]. Available from: URL:
http://www.cdphe.state.co.us/hs/brfss/*.
- American Cancer Society. Cancer prevention and early detection:
facts and figures, 2001. Atlanta (GA): American Cancer Society; 2002.
- Pearlman DN, Clark MA, Rakowski W, Ehrich B.
Screening for
breast and cervical cancers: the importance of knowledge and perceived
cancer survivability. Women Health 1999;28(4):93-112.
- George SA.
Barriers to breast cancer screening: an integrative
review. Health Care Women Int 2000;21(1):53-65.
- Suarez L, Roche RA, Nichols D, Simpson DM.
Knowledge, behavior
and fears concerning breast and cervical cancer among older low-income
Mexican-American women. Am J Prev Med 1997;13(2):137-42.
- Lobell M, Bay RC, Kelton VL, Rhoads MA, Keske B.
Barriers to
cancer screening in Mexican-American women. Mayo Clin Proc 1998;73(4):301-8.
- Solis JM, Marks G, Garcia M, Sheldon D.
Acculturation, access
to care, and use of preventive services: findings from HHANES 1982-84. Am
J Public Health 1990;80(Suppl):11-9.
- Hardy RE, Ahmed NU, Hargreaves MK, Semenya KA, Wu L, Belay Y, et al.
Difficulty in reaching low-income women for screening mammography. J
Health Care Poor Underserved 2000;11(1):45-57.
- Suarez L, Roche RA, Pulley LV, Weiss NS, Goldman D, Simpson
DM.
Why a peer intervention program for Mexican-American women failed to
modify the secular trend in cancer screening. Am J Prev Med
1997;13(6):411-7.
- Navarro AM, Senn KL, McNicholas LJ, Kaplan RM, Roppe B, Campo
MC.
Por La Vida model intervention enhances use of cancer screening
tests among Latinas. Am J Prev Med 1998;15(1):32-41.
- Castro FG, Elder J, Coe K, Tafoya-Barraza HM, Moratto S, Campbell N, et al.
Mobilizing churches for
health promotion in Latino communities: Companeros en la Salud. J Natl
Cancer Inst Monogr 1995;(18):127-35.
- Davis DT, Bustamante A, Brown CP, Wolde-Tsadik G, Savage EW, Cheng X, et al.
The urban church and
cancer control: a source of social influence in minority communities.
Public Health Rep 1994;109(4):500-6.
- Sauaia A, Dauchot CP, Borrayo E, Min S, Leyba J, Gallo SM, et al. The Tepeyac
Project: a church-based approach to increase breast cancer screening
among Latinas in Colorado. Conference proceedings from the 9th Biennial Symposium on Minorities, the
Medically Underserved and Cancer, Intercultural Cancer Council. 2004 Mar
24-28; Washington, DC.
- Suarez L.
Pap smear and mammogram screening in
Mexican-American women: the effects of acculturation. Am J Public Health
1994;84(5):7426.
- D’Antonio WV. Latino Catholics: how different? National Catholic Reporter. 1999 Oct [cited 2005 Mar]. Available from:
URL:
http://www.findarticles.com/p/articles/mi_m1141/ is_2_36/ai_57589376*.
- Perkins R. Evaluating the Passel-Word Spanish surname list: 1990
decennial census post enumeration survey results. Washington (DC): U.S. Census
Bureau, Population Division; 1993.
- Agency for Healthcare Research and Quality. MEPS
Statistical Brief #22: Use of mammography as a cancer screening
tool, 2001. Rockville (MD): U.S. Department of Health
and Human Services [cited 2003 Sep]. Available from: URL: http//www.meps.ahrq.gov/papers/st22/stat22.htm.
- Hedegaard HB, Davidson AJ, Wright RA.
Factors associated with
screening mammography in low-income women. Am J Prev Med 1996;12(1):51-6.
- Colorado Department of Health Care Policy and Financing. Health
Plan Employer Data and Information Set (HEDIS) 2000. Denver (CO): Colorado Department of Health Care Policy
and Financing, Division of Managed Care Contracting [cited 2004 Jul]. Available from: URL:
http://www.chcpf.state.co.us/HCPF/QIBEHLTH/ 2000%20HEDIS%20Final%20Report.pdf*.
- Roetzheim RG, Pal N, Tennant C, Voti L, Ayanian JZ, Schwabe A, et al.
Effects of health insurance and race on early detection
of cancer. J Natl Cancer Inst 1999;91(16):1409-15.
- Iezzoni LI, McCarthy EP, Davis RB, Siebens H.
Mobility
impairments and use of screening and preventive services. Am J
Public Health 2000;90(6):955-61.
- Roetzheim RG, Chirikos TN.
Breast cancer detection and
outcomes in a disability beneficiary population. J Health Care Poor
Underserved 2002;13(4):461-76.
- Colorado Department of Health Care Policy and Financing. Colorado
Medicaid physician news (FY2003-04/2nd
Quarter). Denver (CO): Colorado Department of
Health Care Policy and Financing [cited 2004 Jul]. Available from: URL: http://www.chcpf.state.co.us/default.asp*.
- Corbie-Smith G, Flagg EW, Doyle JP, O’Brien MA.
Influence of
usual source of care on differences by race/ethnicity in receipt of
preventive services. J Gen Intern Med 2002;17:458-64.
- McCall DT, Sauaia A, Hamman RF, Reusch JE, Barton P.
Are
low-income elderly patients at risk for poor diabetes care? Diabetes Care
2004;27(5):1060-5.
- National Cancer Institute. Cancer progress report, 2001. Bethesda (MD): National Cancer Institute
[cited 2004 Jan]. Available from: URL: http://progressreport.cancer.gov.
- Boyer-Chammard A, Taylor TH, Anton-Culver H.
Survival
differences in breast cancer among racial/ethnic groups: a
population-based study. Cancer Detect Prev 1999;23:463-73.
- Zaloznik AJ.
Breast cancer stage at diagnosis: Caucasians
versus Hispanics. Breast Cancer Res Treat 1997;42:121-4.
- Abraido-Lanza AF, Chao MT, Gammon MD.
Breast and cervical cancer screening among Latinas and non-Latina
whites. Am J Public Health 2004;94(8):1393-8.
- Colorado Department of Public Health and Environment. Cancer and poverty in Colorado, 2004. Denver (CO): Colorado
Department of Public Health and Environment; 2004.
- Iezzoni, LI.
Assessing quality using administrative data. Ann
Intern Med 1997;127(8):666-74.
Back to top
*URLs for nonfederal organizations are provided solely as a
service to our users. URLs do not constitute an endorsement of any organization
by CDC or the federal government, and none should be inferred. CDC is
not responsible for the content of Web pages found at these URLs.
|
|
