

|

|

Volume
2:
No. 1, January 2005
COMMUNITY CASE STUDY
Developing and Adapting a Family-based Diabetes Program at the
U.S.-Mexico Border
Nicolette I. Teufel-Shone, PhD, Rebecca Drummond, MA, Ulrike
Rawiel, MS
Suggested citation for this article: Teufel-Shone NI,
Drummond R, Rawiel U. Developing and adapting a family-based diabetes program at
the U.S.-Mexico border. Prev Chronic Dis [serial online] 2005 Jan [date cited].
Available from: URL:
http://www.cdc.gov/pcd/issues/2005/
jan/04_0083.htm.
PEER REVIEWED
Abstract
Context
The prevalence of diabetes among Hispanics is more than twice
that of non-Hispanic whites in communities along the U.S.-Mexico
border. The University of Arizona and two community health
agencies on the Arizona border, Campesinos Sin Fronteras
and Mariposa Community Health Center, collaborated to design,
pilot and assess the feasibility of a lay health-outreach worker-
(promotora-) delivered diabetes education program for
families. La Diabetes y La Unión Familiar was
developed to build family support for patients with diabetes and
to teach primary prevention behaviors to family members.
Method
Community and university partners designed a culturally
appropriate program addressing family food choices and physical
activity, behavior change, communication, and support behaviors.
The program offers educational content and activities that can be
presented in home visits or multifamily group sessions.
Community partners led the implementation, and university
partners guided the evaluation.
Consequences
Seventy-two families (249 total participants) including children
and grandchildren participated. Preintervention and postintervention questionnaires completed by
adults (n = 116) indicate a significant increase in knowledge of eight diabetes risk factors (P
values for eight factors range from <.001 to .006) and a significant
increase in family efficacy to change food (P < .001) and activity
behaviors (P < .001). Interviews with participants highlight the
program’s positive psychosocial impact.
Interpretation
Community and university collaboration involved building upon the promotoras' expertise in engaging the community and
the university’s expertise in program design and
evaluation. A promotora-delivered family-based diabetes
prevention program that emphasizes family support, communication,
and health behaviors is feasible and can yield change in family
knowledge, attitude, and behavior relative to diabetes risk
factors.
Back to top
Background
Among Hispanic populations in the United States, rates of type
2 diabetes and secondary complications (e.g., retinopathy,
neuropathy, renal failure) are more than twice those reported for
non-Hispanic whites (1-3). The high prevalence of associated
conditions corresponds to the poor rates of adherence to American
Diabetes Association recommendations for diabetes self-management
documented for this population (4,5). Hispanic adults in the
United States with diabetes and cardiovascular disease cite
attitudes, perceptions, and preferences of family members as
significant barriers to making recommended changes in their diet
and exercise patterns (4,6,7). Yet family members of Hispanic
patients with diabetes are at a particularly high risk for
developing the disease themselves because of their family history
of diabetes and because of high rates of risk factors (e.g.,
gestational diabetes, obesity, physical inactivity) in this
population (1,8). Providing diabetes education to the entire
family would address both prevention and treatment.
Because of a strong cultural emphasis on family connectedness
among Hispanics, family members may be particularly influential
in the development of health behaviors in this population
(7,9-11). Family behaviors and attitudes can support or challenge
a patient’s psychosocial adaptation to illness and
subsequently a patient’s confidence, intent, and
willingness to implement disease-management strategies (12-15).
In a study of 76 Hispanic patients with diabetes, Chesla et al
(16) reported that 23% of the patients noted troubling changes in family
relations since their diagnosis, and 32% feared that more changes created by the
social and financial stress of the patient’s increasing dependency on other
family members were imminent.
In several studies from Mexico, family support has been shown
to have significant positive association with glucose control in
patients with diabetes (17,18). Family diabetes education studies
in Cuba (19) and Costa Rica (20) have demonstrated improved glycemic control and treatment compliance in patients whose
families had information about diabetes and were supportive of
recommended health behaviors. In the United States, family
education and health-behavior change among Hispanic populations
has been related to weight loss. Foreyt et al (21) and Cousins et
al (22) demonstrated that interactive family-oriented
weight-loss interventions yield greater success than approaches
that target the individual. Both studies highlight the importance
of family support within Hispanic culture and call for additional
efforts to evaluate the effectiveness of family-oriented health
interventions.
Despite the documentation of family influence on health
behaviors, particularly within Hispanic populations, the
literature offers no U.S. examples of diabetes interventions that
target the family and address the family’s collective
behaviors. Brown et al (23,24) encourage the involvement of a
family member in support groups in a diabetes self-management
intervention but do not specifically target the family or family
behaviors.
La Diabetes y La Unión Familiar (Diabetes and
the Family) is the family component of the Border Health
Strategic Initiative (Border Health ¡SI!). Border Health ¡SI! is a comprehensive community-based diabetes
prevention and control project developed by the Mel and Enid
Zuckerman College of Public Health at the University of Arizona
(MEZACOPH) and various community partners serving Arizona
residents at the U.S.-Mexico Border. The various components and
multiple community-university partnerships of Border Health ¡SI! are described in this issue (25).
The objectives of this family-based diabetes education
intervention are the following: 1) to enhance family
members’ social support of patients with diabetes and 2) to
increase the range of primary prevention behaviors associated
with diabetes in family members of patients with diabetes. This
community case study describes the collaborative development,
delivery, and outcome of the initial implementation of La
Diabetes y La Unión Familiar.
Back to top
Context
Geographically and demographically, the context of Border Health ¡SI! and the family component are the
underserved Hispanic communities of Yuma and Santa Cruz counties,
located along Arizona’s southern border with Mexico. Both
counties report an annual median household income of less than
$33,000 with greater than 19% of residents living below the
poverty level (26). In addition, 43.5% of households in Yuma
County and 79.2% in Santa Cruz County report that Spanish is the
predominant language spoken at home (26). Many residents in these
counties do not seek regular health care because they lack access to Spanish-speaking health care providers
and do not have access to health insurance (20%
of Arizona residents do not have health insurance); some are fearful
about their immigration status
(26,27).
To adapt to the needs of Hispanic families in these counties
and to the skills of local promotoras, MEZACOPH,
Campesinos Sin Fronteras (CSF) in Yuma County, and
Mariposa Community Health Center (MCHC) in Santa Cruz County
collaborated to develop, implement, and evaluate La Diabetes y
La Unión. The promotoras from MCHC had
extensive experience in providing education and support to
Hispanic patients with diabetes. The promotoras from
CSF had received national attention for their health
education efforts extended to Hispanic families and migrant farm
workers, but they had limited experience with diabetes education.
In both communities, the promotoras reported the
need for a diabetes intervention that addressed family support and education.
Program development used promotoras’
knowledge of local context and experience in providing outreach
services to this population.
Back to top
Methods
Development
MEZACOPH investigators, CSF and MCHC directors and
promotoras, and the MCHC-certified diabetes educator met
in a day-long work session to discuss local strengths,
challenges, and educational needs. The group reached consensus on
module subject areas, order, format, appropriate instructional
styles, and community differences that might influence
recruitment, retention, and program delivery. After this initial
meeting, MEZACOPH investigators met separately with
promotoras from each site in monthly meetings over an
eight-month period to review draft instructional materials and to
gain feedback on the approach, format, and translation of the
developing curriculum. In these meetings, promotoras from
both sites also provided examples of health education materials
that had been well received in their communities.
Training
Once the curriculum was developed, a bilingual MEZACOPH
investigator conducted a day-long training session in Spanish
with CSF and MCHC promotoras. Since the
promotoras had contributed to the development of many of
the materials incorporated into the curriculum, the training
offered an introduction to the overall flow and format of the
curriculum and instruction in the use of educational materials.
Promotoras gained familiarity and comfort with the
curriculum during and after the training through playing roles,
practicing delivery, and having coworkers critique their
style.
Intervention
La Diabetes y La Unión Familiar is a 12-week
program with 10 points of contact: three home visits, five
educational sessions, and two celebratory events. Drawing on key
concepts of Social Learning Theory, a theoretical model was developed to guide
the program design process (Figure). Key concepts include the influence of
the social environment in behavior change, the need for knowledge
and skills to change behavior (behavioral capability), and
the importance of building confidence in the ability to take action
(self-efficacy). Intervention
activities include teaching team-building and communication skills to build and
reinforce intrafamily communication, collective esteem (so all family members accept and value the family as a group), and collective efficacy (which
promotes confidence in the family's ability to make changes). Intervention
activities also include providing information on food choices and physical
activity so families can make informed choices. Key concepts related to diet,
exercise, and family support are introduced and discussed through the use of
pictorial flipcharts, educational games, food sampling and preparation, and
low-level physical activities.
Family social behaviors such as cohesion, adaptation (exhibited by resiliency
and problem solving), and support within the family influence family food choice
and physical activity behaviors. The proposed outcome of targeting family social
behaviors to change health behaviors is improved nutrient intake, activity
level, and diabetes management or prevention for all family members. The program
encourages family members to collectively set health-behavior goals, to overcome
obstacles hindering healthy behaviors, and to develop a plan to sustain behavior
changes.
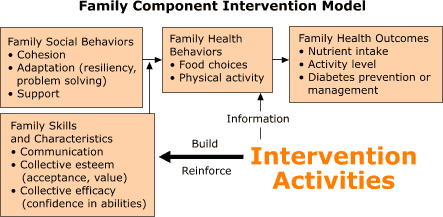
Figure.
A family-based diabetes control and prevention program at the U.S.-Mexico
border.
The promotora instructional manual provides an overview
of the goals and format of the program, a description of the
objectives, and an outline of the activities and supplies needed
for each point of contact. Each family is given a notebook that
includes copies of the flipchart materials and pockets for
handouts, recipes, and other memorabilia such as photographs and
a graduation certificate.
To accommodate differences in promotora skills and
community characteristics, curriculum delivery is flexible.
Educational flipcharts and games are prescribed for specific
modules, but foods/snacks, exercises, and supplemental activities
(e.g., additional games and stories) are selected by the
promotoras from appendices in the instructional
manual.
The program sequence and content are described below:
- Conocer a la Familia (Meet the Family) is the first
home visit to explain the length and format of the program to the
family, register interested family members (name, age and
relationship to the family member with diabetes), gain informed
consent for participation in evaluation activities, and
administer a preintervention questionnaire to all participating
family members aged 18 years and older. All consent and
evaluation procedures were approved by the University of Arizona
Institutional Review Board.
- Bienvenidos! (Welcome!) is a kick-off event for all
families.
- Five weekly interactive educational modules are described
below:
- Familias y Diabetes (Families and Diabetes) is a
general introduction addressing diabetes risk factors, symptoms,
and complications.
- Ser Saludable (Being Healthy) addresses the
relationship between physical activity, food choices, and
diabetes control and prevention.
- Crear Metas (Creating Goals) asks families to evaluate
their own current health behaviors and provides steps for
creating, reaching, and maintaining health-behavior goals.
- La Unión Familiar (Working Together) encourages
families to discuss their progress and goals and suggests ways
they can enhance their success through family support and unity.
This module expands the discussion of support by teaching all
family members to recognize, avoid, and remedy low and
high blood sugar.
- Seguir Saludable (Staying Healthy) encourages families
to continue to support one another in reaching goals and to create
new goals as previous goals are obtained. In this module, family
communication and support skills useful in recognizing and coping
with the stress and depression that often accompany diabetes are
discussed.
- Felicidades! (Congratulations!) is a celebratory event
for all families to acknowledge completion of educational
modules.
- Cómo Están? (How Are You?) is the second
home visit and provides an opportunity for promotoras to
meet with each family to discuss progress and challenges to
family health goals.
- Evaluación (Evaluation) is the third and final
home visit and provides an opportunity for an outside evaluator
to administer the postintervention questionnaire to all
participating family members aged 18 years and older.
All training, intervention, and evaluation materials and
activities were produced and delivered in Spanish.
Recruitment
Two CSF and two MCHC promotoras implemented the
program at their respective sites. Promotoras contacted
patients who had completed the Border Health ¡SI!
patient education classes and extended an invitation to
participate in a family diabetes education program. If a patient
expressed interest, one or two promotoras made a
home visit, scheduling a time when interested family members might be present.
See previous description of this first meeting under Conocer a la Familia (Meet the Family).
The term family was defined by the patient and included spouses,
children, parents, siblings, and friends. Even family members and
friends not living in the same household with the patient could
be identified as family if they had weekly contact with the
patient. To avoid barriers created by child-care needs, no age
limit was imposed, and even infants were permitted to attend. In
the group-delivery format, child care was provided. Children aged
less than 18 years participated in the intervention but were not
included in assessment activities. Once registered, all family
members were invited to the kick-off event (Bienvenidos!)
to meet other families participating in the intervention to play
games and to enjoy a healthy meal.
Delivery
Each agency chose a different delivery style for the five
educational modules based on their experience with family
education efforts in their communities. In Yuma County, two
promotoras delivered the five sessions through a series of
weekly home visits. In Santa Cruz County, two promotoras
delivered the modules in weekly evening classes to five to 10
families in a group format at a central location; if requested
during the initial home visit, promotoras provided
transportation and child care. Home visits and celebratory events
were implemented comparably at the two sites.
Retention
In the group format, families who missed an education session
were called or visited by a promotora to determine if
transportation, illness, lack of interest, or other barriers had
prevented their attendance. The promotora would offer to
help solve any problem, such as providing transportation or
reassuring participants who felt uncomfortable with the format or
information. In the home delivery, retention was not an issue.
Families were consistently home at the prearranged time.
Assessment
Impact of the intervention was assessed using the following:
1) a written preintervention and postintervention Knowledge, Attitudes, Beliefs, and
Behaviors (KABB) questionnaire with 15 close-ended
items that documented adult participants’
self-reported knowledge of risk factors, dietary and exercise
habits, perception of need to eat healthy foods and be active,
collective (family) exercise habits, and collective efficacy to
make behavior changes; and 2) postgraduation interviews.
Questions were designed to track changes in the stated learning
objectives of each of the educational sessions. Promotoras
reviewed the questionnaires for readability and comprehension. A
team of university Border Health ¡SI! investigators
reviewed the individual questions and entire questionnaire for
content and face validity. The design of the questionnaire was
driven by community and university collaborators’ intent to
develop a user- and administrator-friendly instrument that the
promotoras would continue to use to document program
impact.
The McNemar test for paired categorical data and the Wilcoxon signed rank
test for paired continuous data were used to compare preintervention and postintervention
responses of 116 adult participants (48 Santa Cruz County and 68 Yuma County).
In the initial visit, promotoras administered the
preintervention questionnaire. In the final home visit, an
evaluator not identified with the intervention administered the postintervention questionnaire. To accommodate variations in
literacy levels and to avoid bias, all administrators were
instructed to use a straightforward objective style when reading
questionnaires aloud in Spanish. Participants were instructed to
make their selection independently.
In the second home visit (Cómo Están?)
two weeks after graduation, promotoras were impressed by
participants’ comments emphasizing the psychosocial
importance of the program. To further explore an outcome not
assessed by the preintervention and postintervention questionnaire, MEZACOPH
investigators decided to conduct follow-up interviews with a
sample of participants. One year after graduation, a sample of 18
participants consented to an open-ended interview with a MEZACOPH
investigator not identified with the intervention. Given the
small sample and an interest in documenting all experiences
within this case study, participants’ statements, as
recorded in writing by the interviewer, were grouped by common
themes.
Back to top
Consequences
The following outcomes of the initial implementation of La
Diabetes y La Unión Familiar are offered in support of
the feasibility and potential impact of a promotora-delivered family-based diabetes education intervention.
Participation
Four rounds of La Diabetes y La Unión Familiar
were implemented in each intervention county, yielding 72
patients with diabetes and 177 support people, including children
and grandchildren. Table 1 illustrates the distribution of
participants by sex and age group; figures include all
patients with diabetes, family members, and supporters.
Twenty-five percent of participants were children (younger than
18 years). Depending on their age and interest, children
participated in the games, listened to stories, and participated
in discussions generated by the flipcharts. Younger children and
infants played or were cared for in a separate child-care area in
the multifamily group sessions.
Adult daughters and wives were the predominant participating
supporters. Percentage of supporters by relationship to the
family member with diabetes was: 22% daughters, 20% spouses (with
54% wives and 46% husbands), 15% sons, and 9% friends. Of the
total adult participants, 87% attended three or more of the five
educational modules, and 43% of the youth and adults attended
eight or more of the 10 points of contact.
Preintervention and Postintervention Knowledge, Attitudes, Beliefs, and Behaviors (KABB) Outcomes
Sixty-one (53% of total participants) of the preintervention and postintervention response pairs were from the family member with diabetes.
Table 2 provides the percent of yes responses to a list of
possible diabetes risk factors listed in the questionnaire. A
family history of diabetes (heredity) and being Hispanic,
overweight, inactive, and older than 45 years were introduced
in the first educational session (Familias y Diabetes) as
known risk factors for diabetes. Based on their outreach
experience, promotoras reported that some clients believed
that stress, fear, and contact with an individual with diabetes
were also risk factors. This first session provided an
opportunity to discuss these perceptions. Preintervention and postintervention
test comparisons indicate a significant increase in participants who identified
the five known risk factors and a significant
decrease in those who indicated yes to stress, fear, and contact
after the intervention.
Table 3 provides a comparison of participants’ preintervention and
postintervention responses to family efficacy questions.
Participants responded to the following questions on a five-point scale with 1 = not very confident and 5 = very confident:
How confident are you that your family can become more physically
active? How confident are you that your family can eat healthier?
After the intervention, participants report a significant
increase in their perception of their family’s efficacy to
make specific behavior changes.
Questions of food intake and activity were changed during the course of the
program in response to questionnaire administrators’ report that participants
may be misinterpreting questions. The initial questions asked about general
intake of specific foods and participation in specific activities. Questionnaire
administrators indicated that respondents did not believe that they had regular
food and activity behaviors and answered based on their behavior over the
previous week. To create a questionnaire responsive to the
administrators’ observations and to provide an evaluation
instrument that allowed participants to report behavior change in
their own terms, these questions were changed after two rounds of
administration from "in general" to "in the last week." Given the
change, responses to these two different sets of questions were
analyzed separately (separate data table not provided). Despite
the difference in question wording, these separate data sets do
reflect similar patterns of change, which are described
below:
- The frequency of sweetened drink consumption decreased
significantly (P < .001 for both response to question on general
intake as well as question on previous week). These drinks included fruit
drinks distinctive within Hispanic culture (e.g. horchata,
tamarindo, jamaica, Tampico™ as well as
Gatorade™ and Sunny Delight™, but not
carbonated soft drinks.
- No consistent change was noted in reported fruits, vegetables,
soft drinks, or low- and nonfat milk consumption.
- A nonsignificant trend in respondents reportedly exercising
five or more times per week for 30 minutes or more.
- A significant increase in family members participating
together in a physical activity (P = .002).
- A significant increase in participants reporting that family
members help and support each other (P = .01).
- A nonsignificant trend toward greater communication and
cohesive behaviors, such as talking about food choices, going to
the doctor with the family member with diabetes, and agreeing to
eat out or buy food from places with healthy choices.
Changes in knowledge, attitudes, behaviors, and beliefs were
not different in a comparison of family members with diabetes and
family members without diabetes.
Interviews
Eighteen individuals (both patients and family members) from both sites were
interviewed individually for approximately one hour. All statements could be
grouped into one of three themes:
- Program participation had a positive psychosocial impact on
participants. Those with diabetes and family members reported
feeling better and being less depressed and isolated.
- Family communication, particularly about food choices and
understanding of depression, improved; communication was more
frequent and/or less emotional.
- The social interaction provided by the promotoras was
the best part of the program.
No other follow-up data were collected to assess long-term
behavior change or retention of knowledge.
Back to top
Interpretation
La Diabetes y La Unión Familiar, a Spanish
language family diabetes education intervention that targets
family support, communication, and family health behaviors, implemented by promotoras in two Arizona border
communities, yielded changes in family members’ knowledge,
attitudes, behaviors, and beliefs relative to diabetes prevention
and control.
The development of the program content, delivery format, and
even evaluation methods was a collaborative process among a
university, MEZACOPH, and two community health agencies,
CSF and MCHC. The description of the collaborative process
illustrates how standard research practices and community
experience, observation, and interests contributed to the final
intervention. Program outcomes demonstrate that teaching the
family as a group can influence health behaviors, yielding an
increase in family-based physical activity and ameliorating
family member feelings of depression and isolation. This
community case study supports the use of a family-based approach
to diabetes prevention and control. This study indicates that
family involvement should go beyond diabetes
support groups that tend to focus only on the behaviors of the
person with diabetes. Addressing the family’s collective
behaviors as well as patterns of cohesion and communication can
yield change in the family environment, an important influence in
chronic disease management and prevention.
Certain preexisting factors and limiting conditions of this
case study should be acknowledged. The promotoras had
previous experience and training in community outreach services.
They were uniquely familiar with the curriculum as they
collaborated in its development and adapted its delivery for
their communities’ needs. The small sample size in this
case study limits the authors’ ability to project the
applicability and impact of La Diabetes y La Unión
Familiar in other communities. Yet these results are promising and
warrant continued implementation of the program in these counties and piloting
in similar communities. The program is available to other agencies by accessing
its Web site (available from: http://www.borderhealthsi.org/*). Furthermore, the preintervention and
postintervention evaluation instrument did not capture the psychosocial
impact of the program as revealed by promotoras’
observations and a small number of interviews. Future
implementation should consider revising the evaluation instrument
or supplementing evaluation activities with a formal guided
interview conducted by an evaluator not identified with the
intervention.
Back to top
Author Information
Corresponding author: Nicolette I. Teufel-Shone, PhD, Mel and
Enid Zuckerman Arizona College of Public Health, PO Box 245158,
University of Arizona, Tucson, AZ 85724. Telephone:
520-321-7777, ext 16. E-mail: Teufel@u.arizona.edu.
Author affiliations: Rebecca Drummond, MA, Ulrike Rawiel, MS,
Mel and Enid Zuckerman Arizona College of Public Health,
University of Arizona, Tucson, Ariz.
Back to top
References
- National Institute of Diabetes and Digestive and Kidney
Disease. Diabetes in Hispanic Americans [Internet]. Bethesda (MD): The
Institute, National Diabetes Information Clearinghouse [Accessed 2004 Oct 18].
- Harris MI, Klein R, Cowie CC, Rowland M, Byrd-Holt DD.
Is
the risk of diabetic retinopathy greater in non-Hispanic blacks and Mexican
Americans than in non-Hispanic whites with type 2 diabetes. A U.S. population
study. Diabetes Care
1998;21(8):1230-5.
- Harris MI, Cowie CC, Eastman RC. Symptoms sensory neuropathy
in adults with NIDDM in the US population. Diabetes Care 1993;16
(11):1446-52.
- von Goeler DS, Rosal MC, Ockene JK, Scavron J, De Torrijos
F.
Self-management of type 2 diabetes; a survey of low-income
urban Puerto Ricans. Diabetes Educator 2003;29(4):663-72.
- Stern MP, Mitchell BD. Diabetes in Hispanic Americans. In:
National Diabetes Data Group, editors. Diabetes in America,
2nd ed.
Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases,
National Institutes of Health; 1995. NIH Publication No. 95-1468, p. 631-59.
- Juarbe T.
Cardiovascular disease-related diet and exercise
experiences of immigrant Mexican women. West J Nurs Res
1998;20(6):765-82.
- Lipton RB, Losey LM, Giachello A, Mendez
J, Girotti MH.
Attitudes and issues in treating Latino patients with type 2
diabetes: views of healthcare providers. Diabetes Educ
1998;24(1):67-71.
- Khan A, Lasker SS, Chowdhury TA.
Are spouses of patients with
type 2 diabetes at increased risk of developing diabetes?
Diabetes Care 2003;26(3):710-2.
- Brown SA, Garcia AA, Winchell M.
Reaching underserved
populations and cultural competence in diabetes education. Curr
Diab Rep 2002;2(2):166-76.
- Anderson RM, Goddard CE, Garcia R, Guzman JR, Vazquez F.
Using focus groups to identify diabetes care and education issues
for Latinos with diabetes. Diabetes Educ 1998;24(5):618-25.
- Hunt LM, Valenzuela MA, Pugh JA.
Porque me toco a mi? Mexican
American diabetes patients' casual stories and their relationship to
treatment behaviors. Soc Sci Med 1998;46(7):959-69.
- Schafer JC, McCaul KD, Glasgow RE.
Supportive and
non-supportive family behavior: relationships to adherence and
metabolic control in persons with type 1 diabetes. Diabetes Care
1986;9(2):179-85.
- Trief PM, Himes CL, Orendorff R, Weinstock RS.
The marital
relationship and psychosocial adaptation and glycemic control of
individual with diabetes. Diabetes Care
2001;24(8):1384-9.
- Trief PM, Grant W, Elbert K, Weinstock RS.
Family
environment, glycemic control, and the psychosocial adaptation of
adults with diabetes. Diabetes Care 1998;21(2):241-5
- Fisher L, Chesla CA, Skaff MM, Gilliss C, Mullan JT, Bartz RJ, et al.
The family and disease management in
Hispanic and European-American patients with type 2 diabetes.
Diabetes Care 2000;23(2):267-72.
- Chesla CA, Skaff MM, Bartz RJ, Mullan JT, Fisher L.
Differences in personal models among Latinos and European
Americans. Diabetes Care 2000;23(12):1780-5.
- Rodríguez-Morán M, Guerrero-Romero JF.
Importancia del apoyo familiar en el control de la glucemia. [Importance of family support in the control of glycemia]. Salud
Publica Mex 1997;39(1):44-7.
- Valadez-Figueroa I, Aldrete-Rodríguez MG,
Alfaro-Alfaro N.
Influencia de la familia en el control
metabolico del paciente diabético tipo II. [Family
influence on metabolic control of patients with type II Diabetes]. Salud Publica Mex
1993;35(5):464-70.
- Valenciaga Rodríguez J.L.G.d.l.V. F, Pons
Bravet P, Sanchez Valdes O. Repercusion en el control
de la diabetes mellitus de una técnica educativa dirigida
a la familia. [Repercussion of an educational technique aimed to
the family for the control of diabetes mellitus.] Rev Cuba Med Gen Integr 1995;11(2):144-149.
- Aráuz AS, Padilla G, Fernandez G, Rosello M,
Guzman S.
Intervención educativa comunitaria sobre la
diabetes en el ambito de la atencion primaria. [Community diabetes educational
intervention at the primary care level]. Rev Panam Salud Publica 2001
Mar;9(3):145-53.
- Foreyt JP, Ramirez, AG, Cousins JH.
Cuidando El Corazon: a weight-reduction intervention for Mexican
Americans. Am J Clin Nutr 1991 Jun;53(6 Suppl):1639S-1641S.
- Cousins JH, Rubovits DS, Dunn JK, Reeves RS, Ramirez AG, Foreyt JP.
Family versus individually oriented intervention for weight loss in Mexican
American women. Public Health Rep 1992 Sep-Oct;107(5):549-55.
- Brown SA, Hanis CL.
Culturally competent diabetes
education for Mexican Americans: the Star County Study. Diabetes Educ 1999
Mar-Apr;25(2):226-36.
- Brown SA, Hanis CL.
A community-based, culturally
sensitive education and group-support intervention for Mexican
Americans with NIDDM: a pilot study of efficacy. Diabetes Educ
1995;21(3):203-10.
- Cohen SJ, Ingram M. Border
health strategic initiative:
overview and introduction to a community-based model for diabetes
prevention and control. Prev Chronic Dis [serial online] 2005 Jan.
- U.S. Census Bureau.
State and
county quick facts. 2000 census of population and housing, small area income and
poverty estimates. Washington (DC): U.S. Census Bureau [Accessed
2004 Oct 18].
- Centers for Disease Control and Prevention. Behavioral Risk Factor
Surveillance System, 2000. Atlanta (GA): National Center for Chronic Disease
Prevention and Health Promotion.
Back to top
|
|
