 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Tuberculosis Transmission in a Homeless Shelter Population --- New York, 2000--2003In 2003, the incidence of tuberculosis (TB) cases in the United States declined for the eleventh consecutive year to a record low of 5.1 cases per 100,000 population (1). In 2003, 6.3% of reported TB cases in the United States were among homeless persons (2). Compared with the general population, this group has a greater risk for latent TB infection (LTBI) and progression to active disease (3). This report summarizes a recent outbreak of TB and highlights the challenges of preventing TB among homeless persons, particularly when multiple chains of transmission are occurring and multiple jurisdictions are involved. The findings underscore the complementary role of rapid DNA genotyping in the detection of possible TB transmission in homeless populations. To ensure early detection of unsuspected TB transmission in homeless populations, health department TB-control programs are encouraged to use CDC's universal Mycobacterium tuberculosis rapid genotyping system. During January--July 2003, four TB cases were reported by the Orange County Health Department (OCHD), New York, among residents of a homeless shelter for men. The New York City (NYC) Department of Homeless Services (DHS) operates the shelter, located 65 miles north of NYC. The New York State Department of Health (NYSDOH) communicated with the NYC Department of Health and Mental Hygiene (NYCDOHMH), which had identified four additional TB cases among residents of the same shelter during the same period. A joint investigation of this cluster was undertaken by OCHD, NYSDOH, and NYCDOHMH. Before recognition of this cluster in July 2003, two patients associated with this shelter had been reported to NYSDOH and NYCDOHMH in 2001, and another two patients in 2002. TB contact investigations in the shelter focused on residents who shared a dormitory with persons who had TB. Few of these contacts successfully completed tuberculin skin tests (TSTs) and chest clinic referrals because of difficulties with transportation, transience of the population, and follow-ups not being mandatory. The shelter is a 1,001-bed, 28-dormitory, 3--housing-unit facility. Six dormitories have air-handling systems that provide outdoor air (i.e., nonrecirculating systems) on a continuous basis; the remainder of the facility has mechanical heating that does not provide continuous outdoor air ventilation. Although clients requesting NYC shelter services are immediately offered screening for medical conditions including TB, they may decline both the physical examination and the TST. To determine the extent of the outbreak and to implement control measures, M. tuberculosis--genotyping databases at NYSDOH were searched for strains matching the genotype of the isolates of the initial cases reported in 2003. These databases include approximately 20,000 isolates identified during a 12-year period, mainly from the northeastern United States, and include all isolates from New York state since 2001. In addition, a list of shelter residents since January 2001 was matched to the statewide TB registry from 2000--2003. Five additional TB cases among former residents of this shelter were identified from genotyping databases from patients with disease onset during 2002--2003, and six other cases were identified from the registry match from patients with disease onset during 2000--2003. The decision to conduct intensive, active case finding was based on 1) identification of two long-term residents with acid-fast-bacillus (AFB) sputum-smear--positive pulmonary TB in August 2003, one of whom had bilateral cavitary lesions on chest radiograph (CXR); 2) newly identified human immunodeficiency virus (HIV) coinfections in four of the TB patients; and 3) suspicion of recent TB transmission in the shelter. During September 13--15, 2003, the health departments, with logistical support from DHS and shelter staff, screened residents by using results from TB symptom surveys, CXRs, and TSTs. Of 1,038 residents, 958 (92%) were registered for the screening and interviewed for TB symptoms and HIV risk factors. Among residents screened, 927 (97%) had a portable CXR, and 593 (62%) had TSTs administered, with 583 (98%) having TSTs read. Of the 583 TSTs that were read, 223 (38%) were positive (defined as induration >5 mm). An additional 213 residents had positive TST results before screening, for an overall minimum TST-reactivity prevalence of 46%. Residents with no TST performed during the screening might have been tested during the contact investigation or had a previous TST-positive result. Few residents refused TST. A total of 537 residents underwent further medical evaluation on the basis of these initial screening results; of these, 51 (10%) had a sputum smear taken and culture performed. Four additional culture-positive pulmonary TB cases were identified as a result of the screening. Treatment with isoniazid through twice-weekly, directly observed therapy (DOT) provided at the shelter was started by 161 (72%) of the 225 residents for whom LTBI treatment (3) was recommended. Fast-food coupons were provided to promote adherence. Of 297 shelter workers, 228 (77%) were assessed for TB; of these, 25 had a documented previous positive TST, and 16 (7%) were newly TST positive. TB disease was not identified among shelter workers. During 2000--2003, a total of 29 TB cases were identified among residents in this facility. Three local health jurisdictions received the initial reports: NYC (17), Orange County (11), and Dutchess County (one). The median age of patients was 49 years (range: 39--81 years); 16 (55%) were born in the United States, all of whom were black, and 13 (45%) were foreign-born. Twelve (41%) patients had positive AFB sputum smears and thus were potentially more contagious; seven (24%) had cavitary lesions on CXRs, and 12 (57%) of 21 tested had HIV coinfection. All M. tuberculosis isolates were susceptible to first-line medications. TB patients and those with known HIV were offered and referred to appropriate treatment. Of 26 TB cases with genotype data available, 11 (42%) shared the M. tuberculosis genotype associated with this facility* (Figure 1). One additional TB case was identified in an outside contact to a source patient with the same genotype. The earliest case identified with this strain occurred in a patient who had culture-confirmed pulmonary TB diagnosed on three occasions: in 1996 and 2000, when the patient had incomplete treatment for TB before being lost to follow-up, and in April 2001, approximately 6 months after the patient had entered the shelter with his TB status unknown to shelter staff. At that time, the patient completed a full course of DOT. His M. tuberculosis isolates from 1996 and 2001 had the same genotype and were susceptible to anti-TB drugs. The only patient outside the shelter with this strain had TB diagnosed in October 2000. This patient and the probable source patient had worked together in 2000. All subsequent shelter residents who had M. tuberculosis isolates with this strain were documented to have stayed in the shelter with at least one AFB sputum-smear--positive TB patient with the same genotype (Figure 2). Patients resided at the shelter for a median of 2.5 years (range: 4 months--6 years), and all patients shared the same dining and recreational areas. Analysis of dormitory contacts revealed that three patients had shared a dormitory during the infectious period of a person with TB who had a positive sputum-smear result. The isolates from eight other shelter residents shared a different genotype†, known as C-strain (Figure 1). Of 79 patients with this pattern identified in NYC during 2001--2003, a total of 33 (42%) were homeless persons from shelters throughout NYC. Seven (24%) TB patients had genotypes not matching those of other shelter patients, and specimens were not available for three patients. Reported by: J Hudson, MD, S Van Zetta, MPH, B Brissette, Orange County Health Dept, Goshen; C Driver, M Macaraig, MPH, A Winters, MD, S Poonja, MPH, S Munsiff, MD, M Beatty, MD, New York City Dept of Health and Mental Hygiene; D Marder, MD, A Gutkovich, New York City Dept of Homeless Svcs; M Oxtoby, MD, J Grabau, PhD, J Driscoll, PhD, P Smith, MD, New York State Dept of Health. Div of Tuberculosis Elimination, National Center for Infectious Diseases; F Coronado, MD, EIS Officer, CDC. Editorial Note:This investigation and recent reports from Maine and Washington (4,5) indicate ongoing transmission of M. tuberculosis among homeless persons. In addition, rapid disease progression in persons coinfected with HIV was noted in this and other shelter-associated outbreaks (6,7). Notification of cases to three different local health departments and incomplete sharing of information across jurisdictions initially masked the extent of TB disease and transmission in this population. Some cases were not linked initially to the shelter because of homelessness and varying methods of recording addresses but were later linked through matches in the homeless shelter registry. Genotyping helped elucidate transmission among TB patients and suggested that multiple chains of M. tuberculosis transmission were occurring simultaneously. Other TB clusters at homeless shelters have been documented through genotyping (4--6,8). To improve nationwide access to this useful technology, in 2004, CDC began offering universal M. tuberculosis rapid genotyping to all health department TB-control programs in the United States. This system is expected to help with early detection of unsuspected transmission (9). In this outbreak, 11 TB cases could have been prevented if the index patient with the shelter-associated strain had completed treatment when his TB was diagnosed in 1996 or when his disease reactivated in 2000. The extensive occurrence of TB in this homeless population underscores the need for strengthening and maintaining interjurisdictional reporting procedures. As a result of this investigation, the shared responsibilities of NYSDOH and NYCDOHMH were evaluated with regard to case management, infection control, and TB contact investigation, and the intake procedures at shelters for TB screening and for LTBI treatment were strengthened. The impact of the control measures will be monitored through analysis of future cases and through surveys of screening results. References
* 13-band IS6110-RFLP and spoligotype octal code designation 777777600060771. † 3-band IS6110-RFLP and spoligotype octal code designation 700036777760731. Figure 1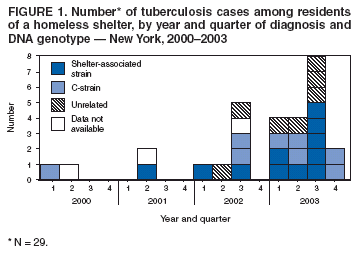 Return to top. Figure 2 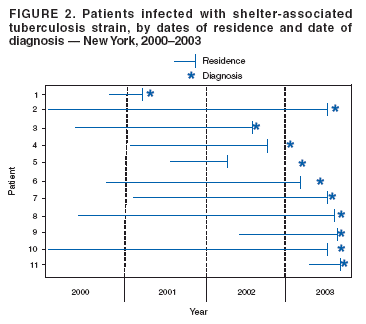 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 2/17/2005 |
|||||||||
This page last reviewed 2/17/2005
|