 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Measuring Exposure to an Elemental Mercury Spill --- Dakota County, Minnesota, 2004Elemental mercury spills can cause contamination of neighborhoods and homes and result in neurologic and kidney disorders in exposed persons who inhale mercury vapors. Often, however, difficulties exist in determining the magnitude of exposure and effectiveness of decontamination or in recognizing that reexposure has occurred. This report summarizes the response to an elemental mercury exposure that resulted in the decontamination of 48 persons and the subsequent analysis of blood and urine samples from 14 exposed youths aged 6--16 years. Data from these analyses suggest that 1) blood samples are more sufficiently acquired and can be used to evaluate recent acute exposure and 2) use of a real-time mercury vapor analyzer can help public health officials determine the magnitude of exposures and help prevent reexposures. In addition, demolition and waste-disposal firms and government agencies must take actions to ensure that elemental mercury is adequately secured before disposal. Case ReportIn preparation for demolition of a factory in Dakota County, Minnesota, hazardous waste from the factory was temporarily stored in a shed, which was not effectively secured. During a late afternoon in September 2004, two teenagers entered the shed and found two canning jars containing approximately 21 pounds of elemental mercury. The teenagers brought the mercury back to their neighborhood, where they and approximately 12 other youths played with it, throwing handfuls of mercury at each other and splashing in a large puddle of mercury on an outdoor basketball court. This initial exposure was limited to <2 hours because of rapid response by a parent who saw what the youths were doing, told them to go home and shower, and contacted the police. Subsequently, 48 persons, including 18 youths, were decontaminated with water and detergent by the Dakota County Special Operations Team between 10 p.m. and 2 a.m. Beginning at 9 p.m., homes were scanned for contamination by using a real-time mercury vapor analyzer (RA-915+; Ohio Lumex Company; Twinsburg, Ohio). On the recommendation of Minnesota Department of Health (MDH) staff, residents of 12 contaminated homes* were sheltered in a motel by the American Red Cross. As part of its epidemiologic investigation, MDH staff interviewed some of the youths the morning after the event and learned that the teenagers had attempted to ignite the mercury and might have been exposed to fumes. Subsequent sampling with the mercury vapor analyzer in motel rooms of displaced families revealed mercury contamination, and high concentrations of mercury vapor found near the hair of three youths 24 hours after exposure (Table 1) suggested that exposures might have been more severe than initially indicated, that decontamination was incomplete, and that exposures were continuing. Consequently, 14 youths aged 6--16 years with known exposures were examined by physicians; 11 were evaluated at Regions Hospital in St. Paul, Minnesota. Blood and/or urine samples were obtained from all 14 youths. However, although the youths were provided bottles for urine samples when their blood was drawn, the first samples were not provided until 3 days later, during the weekend. In addition, at Regions Hospital and at one extended-stay motel, mercury vapor concentrations were measured with a mercury vapor analyzer near the skin of the youths, and exhaled air mercury vapor concentrations were measured by analyzing air in plastic bags inflated by some of the youths. Contaminated hair and scalps of the youths were washed at the hospital with shampoo containing selenium sulfide and dried with terry-cloth towels, which were then discarded. Decontamination was verified with a mercury vapor analyzer. Follow-up samples were obtained for youths with elevated mercury levels. Epidemiologic and Sampling FindingsAll 14 patients had routine physical examinations. Two had new onset cough, and one complained of a poor appetite; these symptoms had resolved by a follow-up visit. Samples from four youths were taken at different times because not every patient agreed to provide a blood sample on day 2. In addition, blood samples drawn from two youths on day 2 coagulated; one of these persons was retested on day 10. Elevated mercury (>8 µg/L) was found in five of eight analyzed blood samples taken on day 2 (Table 2). Additionally, measurable amounts (5 µg/L and 6 µg/L, respectively) of mercury were found in samples collected from one child on day 4 and another child on day 10. Second blood samples collected during days 9--15 from the five youths with the initial elevated readings determined their blood mercury levels had declined below the laboratory reporting limit (5 µg/L). Second blood samples could not be obtained from two youths. Measurable mercury was found in the urine samples of five youths (Table 2). However, these urine sample results might be unreliable because of small sample volumes. From hour 44 to hour 98, exhaled mercury decreased for three youths (patients 5, 6, and 7), whereas readings for two youths (patients 3 and 9) indicated increases (Table 1). The increases, along with high concentrations in a motel room, suggested reexposure; investigation identified the source as a contaminated motor vehicle. Patient 7, who had a longer half-life of exposure than patients 5 or 6, was determined to have been reexposed by the same contaminated motor vehicle (Table 1). Comparison of mercury vapor concentrations near the skin and hair at hours 42--44 and 98 confirmed the reexposures observed in exhaled mercury (Table 1) and the motel room. Mercury vapor concentrations in motel rooms decreased after isolation of the contaminated motor vehicle and disposal of contaminated personal items. The last blood mercury analyses for all youths, except patients 12 and 13, indicated concentrations below laboratory reporting limits (4--5 µg/L), suggesting cessation of the exposure. No further treatment was indicated for any patient. The correlation between blood mercury and exhaled mercury for individual youths was low (R2 = 0.27). Testing in eight of the youths' residences indicated maximum mercury vapor concentrations ranging from <60 ng/m3 to >50,000 ng/m3 (Table 3). Three additional homes were found to be contaminated by adults tracking mercury. Cleanup in accordance with MDH criteria and reoccupancy of all contaminated homes was completed 22 days after the initial incident. The Minnesota Pollution Control Agency used a mercury-sniffing dog (1) to find the source of contamination in the last house cleared. Tracked mercury was located by using a mercury vapor analyzer. Three of four contaminated cars could not be cleaned to the MDH criterion for clearance and were scrapped. All visible traces of mercury were cleaned from the basketball court and other affected outdoor areas. Dakota County Public Health nurses tracked all of the youths, facilitating medical examinations and testing and providing support for families. Reported by: BA Baker, MD, Regions Hospital Occupational Medicine Clinic, St. Paul; C Herbrandson, PhD, T Eshenaur, MPH, RB Messing, PhD, Minnesota Dept of Health. Editorial Note:Exposure to elemental mercury occurs largely from inhaling mercury vapors; very little mercury is absorbed through the skin or by ingestion. Mercury spills pose a serious health hazard and are difficult to clean because most common methods (e.g., sweeping or vacuuming) disperse mercury, increasing the surface area of the mercury, increasing evaporation, and exacerbating the contamination. This report illustrates that use of real-time portable instruments such as mercury vapor analyzers can enable investigators to rapidly measure mercury vapor concentrations and determine the extent of an exposure incident. Geometric mean and 95% total blood mercury concentrations in the 1999--2002 National Health and Nutrition Examination Surveys (NHANES) for women of childbearing age were 0.92 µg/L and 6.04 µg/L, respectively, and for young children were 0.33 µg/L and 2.21 µg/L, respectively (2). Almost all inorganic mercury blood concentrations in the NHANES study were below the detection level of 0.4 µg/L (2). Geometric mean and 95% concentrations of urine mercury for women aged 16--49 years in the 1999--2000 NHANES data were 0.72 µg/L and 5.00 µg/L, respectively (3). Normal exhaled air mercury concentrations are typically <50 ng/m3 for persons without dental amalgams (Minnesota Department of Health and Minnesota Pollution Control Agency, unpublished data, 2004). The half-life of total mercury in blood for persons exposed to mercury vapor is 2--5 days, reflecting distribution to tissues and elimination through exhalation (4,5), which corresponds to the results in this report; blood mercury levels were below the detection limit 7--13 days after initial positive measurement. Exhaled mercury concentrations have been found to decrease, with half-lives of 13--25 hours (6) and 1.6--2.3 days (7). These half-lives also are consistent with the results in this report. However, exhalation half-lives longer than 30 hours might indicate continuing exposure or reexposure to mercury. The patient with the calculated half-life of 44 hours had been reexposed on day 4. Exhaled vapor concentrations can also depend on proper exhalation by patients. To compare data between patients, investigators should instruct all patients to exhale in the same manner; however, mercury vapor half-lives are repeated measures and will not be as sensitive to individual differences. The lack of correlation between exhaled mercury and blood mercury is likely caused by measurement of different forms of mercury (i.e., total mercury for blood and mercury vapor for exhaled) and the small range of exposures. Approximately 70%--80% of inhaled mercury enters the blood before distribution to tissues; the rest is immediately exhaled. An estimated 7% of retained mercury is exhaled in the first 3 days after exposure (8,9). Approximately 9.2% and 2.4% is excreted in feces and urine, respectively, within 7 days (4). Conversely, mercury concentrations in blood can increase rapidly after an acute exposure to mercury, providing timely indication of exposure. In addition, the short half-life of mercury in blood can enable confirmation of the cessation of exposure. However, investigators should be aware of potential confounders to measurements of mercury concentrations (e.g., fish consumption, dental amalgams, medicinal use, and ritualistic use of mercury such as sprinkling on a floor for good luck) (10). In this report, the experiences of responders and investigators also underscore several recommendations for demolition and waste-disposal companies and government agencies. These include 1) securing elemental mercury at demolition sites, 2) confirming mercury decontamination by sampling, 3) providing sensitive field instruments and appropriate training for tracking mercury contamination and exposure, and 4) incorporating quality-assurance controls into all data collection activities. Acknowledgments This report is based on information contributed by Regions Hospital/Health Partners, St. Paul; G Kalstabakken, D Kuhns, Rosemount Police Dept; P Adams, K Dickinson, B Schroeder, J Springsted, K Wick, Dakota County Public Health Dept; D Fier-Tucker, C Hubbard, S Lee, H Neve, Minnesota Pollution Control Agency; DBW Jones, Minnesota Dept of Health. Agency for Toxic Substances and Disease Registry. References
* In this incident, MDH recommended evacuation of homes with a maximum mercury vapor concentration >1,000 ng/m3 and recommended cleanup of all homes with a maximum concentration (unventilated) >500 ng/m3, as measured by a mercury vapor analyzer. Cleanup or disposal of vehicles was recommended at concentrations >1,000 ng/m3. These cleanup/clearance criteria were intended to limit exposures to no more than the Environmental Protection Agency chronic reference concentration of 300 ng/m3 or the acute California reference effects level of 1,800 ng/m3.
Table 1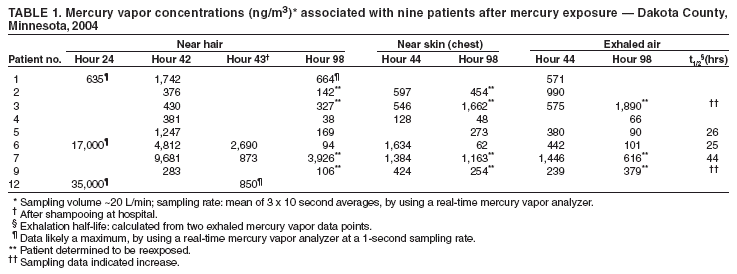 Return to top. Table 2  Return to top. Table 3 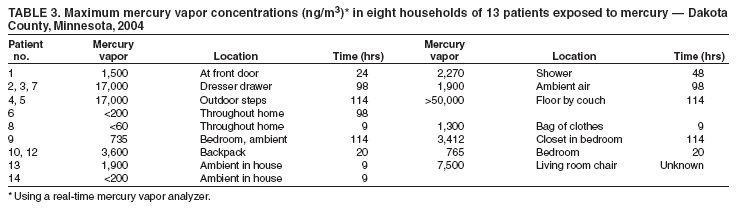 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 2/17/2005 |
|||||||||
This page last reviewed 2/17/2005
|