 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Racial/Ethnic and Socioeconomic Disparities in Multiple Risk Factors for Heart Disease and Stroke --- United States, 2003Heart disease and stroke are the first and third leading causes of death, respectively, in the United States (1). Certain modifiable risk factors, including high blood pressure, high cholesterol, diabetes, tobacco use, obesity, and lack of exercise, are the main targets for primary and secondary prevention of heart disease and stroke. A substantial proportion of the population has multiple risk factors, increasing their likelihood of cardiovascular disease (2,3). To assess the prevalence of multiple risk factors for heart disease and stroke and to identify disparities in risk status among population subgroups, CDC analyzed data from the 2003 Behavioral Risk Factor Surveillance System (BRFSS) survey. This report summarizes the results of that analysis, which indicated that approximately 37% of the survey population had two or more risk factors for heart disease and stroke and that considerable disparities in risk factors existed among socioeconomic groups and racial/ethnic populations. To decrease morbidity and mortality from heart disease and stroke, public health programs should improve identification of persons with multiple risk factors and focus interventions on those populations disproportionately affected. BRFSS is a state-based, random-digit--dialed telephone survey of the noninstitutionalized, U.S. civilian population aged >18 years. CDC analyzed self-reported data from the 2003 BRFSS survey, which included 256,155 participants from 50 states, the District of Columbia, Puerto Rico, Guam, and the U.S. Virgin Islands. In 2003, the median CASRO response rate among states/territories was 53.2% (range: 34.4% [New Jersey] to 80.5% [Puerto Rico]). These rates reflect both telephone sampling efficiency and the degree of participation among eligible respondents who were contacted. This analysis examined six risk factors for heart disease and stroke: high blood pressure, high cholesterol, diabetes, current smoking, physical inactivity, and obesity. Persons reported whether they were ever told by a doctor or other health professional that they had high blood pressure, high cholesterol, or diabetes. Current smoking was defined as having smoked at least 100 cigarettes during one's lifetime and still smoking by the date of the survey. Physical inactivity was assessed by a "no" response to the question, "During the past month, other than your regular job, did you participate in any physical activities or exercises, such as running, calisthenics, golf, gardening, or walking for exercise?" Obesity was defined as having a body mass index >30.0 kg/m2 on the basis of self-reported height and weight (4). Multiple-risk--factor status was defined as having two or more of the six risk factors. Differences in the prevalence of multiple risk factors were examined by age, sex, race/ethnicity, education, income, and employment status; pregnant women were excluded from analysis. Data were weighted to reflect the noninstitutionalized, civilian population of each state/territory. Statistical software was used to account for the complex sampling design. Data were age-standardized to the 2000 U.S. standard population. Age-specific and age-adjusted prevalences are reported. For this report, references to white and black populations mean non-Hispanic whites and non-Hispanic blacks, respectively. In 2003, 25.6% (95% confidence interval [CI] = +0.3) of respondents reported having high blood pressure, 25.3% (CI = +0.3) reported having high blood cholesterol, 25.0% (CI = +0.3) were obese, 24.1% (CI = +0.3) were physically inactive, 22.6% (CI = +0.3) were current smokers, and 7.4% (CI = +0.2) reported having diabetes. Overall, 29.8% (CI = +0.4) reported having no risk factors, 33.1% (CI = +0.4) reported one risk factor, and 37.2% (CI = +0.3) reported two or more risk factors. The percentage of respondents reporting two or more risk factors increased among successive age groups (Table 1). The prevalence of having two or more risk factors was highest among blacks (48.7%) and American Indians/Alaska Natives (46.7%) and lowest among Asians (25.9%); prevalences were similar in women (36.4%) and men (37.8%). The prevalence of multiple risk factors ranged from 25.9% among those who graduated from college to 52.5% among those with less than a high school diploma (or equivalent). Household income followed a similar pattern, with persons reporting >$50,000 annual income having the lowest prevalence (28.8%) and those reporting <$10,000 having the highest prevalence (52.5%) of two or more risk factors. Household income was not provided by 12.3% of respondents; these persons reported a 36.9% prevalence of multiple risk factors. The occurrence of two or more risk factors also varied by employment status. Adults who reported being unable to work had the highest prevalence (69.3%) of two or more risk factors, followed by retired persons (45.1%), adults who reported being unemployed (43.4%), homemakers (34.3%), and employed persons (34.0%) (Table 1). The prevalence of two or more heart disease and stroke risk factors also varied by state/territory and ranged from 27.0% (Hawaii) to 46.2% (Kentucky) (Table 2; Figure). Twelve states and two territories had a multiple-risk--factor prevalence of >40% (Alabama, Arkansas, Georgia, Indiana, Kentucky, Louisiana, Mississippi, North Carolina, Ohio, Oklahoma, Tennessee, West Virginia, Guam, and Puerto Rico). Reported by: DK Hayes, MD, KJ Greenlund, PhD, CH Denny, PhD, JB Croft, PhD, NL Keenan, PhD, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:This report indicates that, in 2003, a high proportion of the U.S. population had multiple risk factors for heart disease and stroke, particularly certain population subgroups defined by race/ethnicity and socioeconomic status (i.e., education, family income, and employment). Prevalence of multiple risk factors also varied considerably by state/territory. A better understanding of the reasons for these differences could guide public health prevention programs. Furthermore, the small proportion of the population that reports no risk factors demonstrates the substantial public health burden of heart disease and stroke. In this study, 37.2% of respondents reported having two or more of the six heart disease and stroke risk factors examined. A previous study that used BRFSS examined five risk factors and observed an 18% increase in the prevalence of multiple risk factors from 1991 to 1999, with 27.9% of the population reporting two or more risk factors in 1999 (5). If physical inactivity is excluded from the 2003 BRFSS survey analysis, the prevalence of multiple risk factors is 28.8%; thus, the greater prevalence determined by the current study is probably attributable to the inclusion of physical inactivity as an additional risk factor. Changes in self-reported risk-factor status might also be attributable either to an increasing prevalence of risk factors overall or to better detection and awareness of certain risk factors. For example, in a study using data from the National Health and Nutrition Examination Survey, hypertension based on actual blood pressure measurements increased from 24.5% during 1988--1994 to 28.4% during 1999--2000 (6), suggesting an increase in prevalence. High blood pressure based on self-reports (i.e., BRFSS survey) also increased, from 23.8% in 1991 to 25.4% in 1999 (5), suggesting a greater awareness of the risk factor. However, for the same period, self-reports of high blood cholesterol increased (5), whereas the prevalence based on actual measurement of blood cholesterol changed minimally (7). Regardless of the differences between actual measurements and self-reports, the results indicate that a substantial proportion of the adult population has multiple risk factors for heart disease and stroke. The findings in this report are subject to at least five limitations. First, BRFSS data are based on self-reported information and are subject to recall and social desirability bias (e.g., underreporting of actual weight) (8). Second, this study did not examine the degree of individual cardiovascular risk factors nor their control through lifestyle, behavioral, or pharmacologic means. Third, those respondents who had not been screened for high cholesterol, diabetes, or high blood pressure might not have been aware they had these risk factors, an obstacle possibly attributable to unequal access to health-care services. Fourth, the low response rate might have influenced the results; however, when compared with other surveys, data from BRFSS have been demonstrated to be reliable and valid (9). Finally, this study only examined modifiable risk factors and did not include other established risk factors (e.g., family history of premature coronary heart disease) (5). Many modifiable risk factors for heart disease and stroke can be addressed through prevention, early recognition, and treatment. Policy and environmental changes (e.g., workplace smoking cessation programs and health-care provider adherence to primary care guidelines) also are essential in influencing persons to live heart-healthy and stroke-free lives. CDC has formed multiple local, national, and global partnerships to address the burden of heart disease and stroke. One example is the Public Health Action Plan to Prevent Heart Disease and Stroke, which is being implemented by the National Forum for Heart Disease and Stroke Prevention (10). Through one of its eight task groups, this forum is assessing existing research agendas and gaps in policy development for preventing heart disease, stroke, and associated risk factors. Another task group is examining current data systems and identifying gaps in surveillance, including incidence of risk factors for heart disease and stroke, incidence and case fatality of acute events, and disability among survivors. CDC funds health departments in 32 states and the District of Columbia to promote heart-healthy and stroke-free communities. These programs emphasize the use of education, environmental strategies, and system changes to address heart disease and stroke among diverse populations. For example, Oregon's program uses population-based public health approaches to raise public awareness of the urgency of addressing cardiovascular disease, the symptoms of heart disease and stroke, and the need to call 911. To decrease the disproportionate burden of multiple risk factors on minority populations, public health programs should focus on improving identification and treatment of affected persons and promoting policy and lifestyle changes conducive to cardiovascular health. References
Table 1 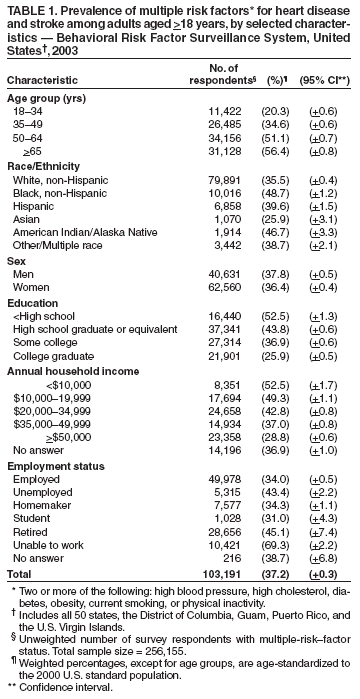 Return to top. Table 2 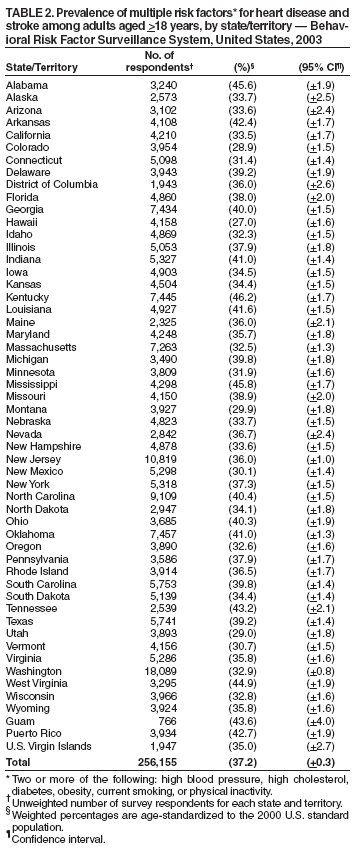 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 2/10/2005 |
|||||||||
This page last reviewed 2/10/2005
|