 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Rapid Health Response, Assessment, and Surveillance After a Tsunami --- Thailand, 2004--2005On December 26, 2004, an earthquake triggered a devastating tsunami that caused an estimated 225,000 deaths in eight countries (India, Indonesia, Malaysia, Maldives, Seychelles, Somalia, Sri Lanka, and Thailand) on two continents. In Thailand, six provinces (Krabi, Phang-Nga, Phuket, Ranong, Satun, and Trang) were impacted (Figure 1), including prominent international tourist destinations. The Thai Ministry of Public Health (MOPH) responded with rapid mobilization of local and nonlocal clinicians, public health practitioners, and medical supplies; assessment of health-care needs; identification of the dead, injured, and missing; and active surveillance of syndromic illness. The MOPH response was augmented by technical assistance from the Thai MOPH--U.S. CDC Collaboration (TUC) and the Armed Forces Research Institute of Medical Sciences (AFRIMS), with support from the office of the World Health Organization (WHO) representative to Thailand. This report summarizes these activities. The experiences in Thailand underscore the value of written and rehearsed disaster plans, capacity for rapid mobilization, local coordination of relief activities, and active public health surveillance. Rapid ResponseMOPH rapidly activated mass casualty plans and deployed personnel and resources to meet local health-care needs. On December 26, a central command center in Bangkok and command centers in each of the six impacted provinces were established to coordinate activities. Deployments included approximately 100 teams providing emergency clinical care, 12 teams providing technical support and health education, five teams conducting active surveillance and investigating potential outbreaks, six teams providing mental health support, and three teams of MOPH-accredited massage therapists providing traditional Thai massage therapy for relief workers and displaced persons. The first team from Bangkok arrived on December 26, approximately 6 hours after the tsunami struck. As of January 9, an estimated 90,000 persons in affected communities, relief centers, and displaced-person camps had received medical and mental health care; 9,798 received outpatient services, 2,233 received inpatient services (398 were in intensive care, and 1,254 underwent major surgical procedures), and approximately 80,000 persons received other types of care from mobile teams. Outbreak risks and sanitation, environmental, and community mental health needs were rapidly assessed and addressed. Health education programs on personal hygiene, water and food safety, garbage disposal, toilet construction, injury prevention, and mental health were initiated. Laboratories used for disease surveillance were supplemented with additional staff and equipment; food, drinking water, and sea water were assessed for safety. Health and Needs AssessmentDuring December 30, 2004--January 6, 2005, three teams of Thai and U.S. health professionals from TUC and AFRIMS conducted a rapid health and needs assessment in the impacted provinces. Logistic and strategic support was provided by the Joint U.S.-Thai Military Advisory Group, Thailand. Using a WHO rapid assessment tool (1), investigators collected data on hospital characteristics; damage to buildings and communication, electricity, water, and sewage systems; adequacy and condition of health-care personnel, medical supplies, and morgue facilities; and anticipated medical needs. Questions were initially directed to provincial health office staff members. However, on the provincial staffs' recommendation, staff from 10 mainland hospitals (four in Phuket, two in Phang-Nga, and one each in Krabi, Ranong, Satun, and Trang) and leaders from approximately 12 coastal and island communities in the six impacted provinces also were interviewed. The 10 hospitals, with approximately 2,000 inpatient beds and 24 operating rooms, served as the primary referral centers for tsunami-related medical care. None of the 10 hospitals had been damaged by the tsunami; all had activated previously rehearsed, written mass casualty plans. Shortages of blood, blood products, and certain medical supplies (e.g., surgical devices and antibiotics) were noted during the first 2 days after the tsunami. Hospital morgue facilities were inadequate for the number of dead, and corpses were moved from hospitals to temporary morgues at nearby wats (temples). Rapid mobilization of health professionals from multiple areas in Thailand resulted in adequate numbers of staff. By December 30, hospital patient loads were returning to usual levels, and the supplementary medical staff were released. By January 4, provincial health officials reported that needs for staff and supplies were being met. However, coordination of relief efforts was a challenge. One province was required to coordinate the concurrent activities and service areas of 14 health teams from volunteer organizations. A small hospital on the island of Koh Phi Phi in Krabi Province was destroyed by the tsunami, and four health clinics in coastal villages and islands were severely damaged or destroyed. Temporary clinics were established by provincial medical staff and volunteer organizations in some coastal villages and in displaced-person shelters. In the hospitals and communities assessed, food and bottled water were plentiful, and written guidance on water decontamination was posted. Public Health SurveillanceAs of January 25, in the six impacted provinces, 5,388 deaths had been confirmed; 8,457 persons were reported injured, and 3,120 persons remained missing (2). Phang-Nga Province was most severely affected, with 4,217 (78%) deaths, 5,597 (66%) persons injured, and 1,813 (58%) persons missing. Among the 3,762 confirmed dead whose nationality was established, 1,814 (48%) were reported to be Thai nationals (2). Since 1970, MOPH has operated a national passive surveillance system for infectious diseases by using a standard reporting form; as of 2000, the system had 68 diseases under surveillance. After the tsunami, MOPH implemented active surveillance for 20 of these diseases plus wound infections and electric shock; five of these disease syndromes (i.e., clinically diagnosed acute diarrhea, wound infections, respiratory illness, meningitis, and febrile illness) are summarized in this report. Active surveillance was initiated in all 20 districts in the six provinces impacted by the tsunami. Surveillance was established during December 26--January 2. Data for the 20 districts were collected from all medical facilities (77 health centers, 22 public hospitals, and four private hospitals), the two shelters for displaced persons, and the two forensic identification centers. Surveillance team members visited each site daily and collected individual case-report forms that included information on disease syndrome, age, sex, and nationality. Each day, these teams analyzed data and identified events requiring further investigation and preventive measures. Population data for 2004 from the Thai Ministry of the Interior were used to calculate incidences. During December 26--January 11, the six provinces reported the following cases: 1,237 cases of acute diarrhea, 356 wound infections, 177 febrile illnesses, and 156 respiratory illnesses (including six cases of aspiration pneumonia). No cases of meningitis were reported; two deaths were attributed to pneumonia. The incidences of febrile illness and pneumonia were comparable with those during the same period a year ago. Cases of acute diarrheal disease increased steadily until January 3; since then, the number has stabilized at approximately 100 case reports per day (Figure 2). During December 26--January 11, seven disease clusters were detected; all were diarrheal disease. Implementation of active surveillance enhanced detection of diarrheal disease. The annualized rate from active surveillance was 1.7 times greater than that recorded from passive surveillance during the same period a year ago (2,950 cases per 100,000 population versus 1,758). Incidence of wound infections was substantially higher than that recorded in previous years. Preliminary results from an ongoing investigation of 33 patients at two government hospitals in Phuket Province indicated that approximately two thirds of the infections were polymicrobial. The most common organisms recovered included Proteus spp., Klebsiella spp., Pseudomonas spp., Staphylococcus aureus, Enterobacter spp., and Escherichia coli. Aeromonas hydrophila was recovered from two infections. Active disease surveillance continues in the six impacted provinces. Reported by: Ministry of Public Health; World Health Organization representative to Thailand; Thai Ministry of Health--US CDC Collaboration, Nonthaburi; Armed Forces Research Institute of Medical Sciences, Bangkok, Thailand. Editorial Note:Thailand has a well-developed public health infrastructure that provides residents with more than 90% of their health care. The MOPH response to the December 26 tsunami was rapid and effective at mitigating the health consequences of the tsunami among survivors. Mass casualty plans were immediately activated, and medical personnel, technical experts, and supplies arrived soon after the tsunami struck (3). Health assessments conducted 1 week after the tsunami indicated that, despite a huge influx in the number of patients, the medical system was intact and functioning effectively. As seen in other disasters, rapid health assessments can identify immediate health needs and help prioritize public health interventions (4). Active disease surveillance was useful in identifying disease events and clusters requiring intensive investigation. Although active surveillance demonstrated an increase in the number of acute diarrhea cases, much of this increase can likely be attributed to active searching for rather than passive reporting of cases. Concerns by WHO and other authorities about post-tsunami infectious disease mortality have centered on massive outbreaks of cholera and other epidemic forms of diarrhea (5). In comparison with the post-tsunami rates of diarrheal disease observed in Thailand (2,950 cases per 100,000 population), the rate of diarrhea during previously studied outbreaks in disaster settings in other countries has been much higher (i.e., 87,000--120,000 cases per 100,000 population) (6). The increased number of wound infections suggests that many who survived the initial impact of the tsunami were injured by debris (7). A large tsunami in 1998 in Aitape, Papua New Guinea, had high numbers of persons with traumatic wounds; an Australian team of three surgeons and one nurse reported performing 182 surgical procedures in 15 days (8). The large number of enteric pathogens cultured from wounds in Thailand suggests surface contamination with enteric pathogens or true polymicrobial infections. Treatment should include empiric antibiotic coverage for a range of organisms until results from wound tissue cultures are available to guide therapy. Infection with organisms commonly associated with wounds exposed to sea water, including A. hydrophila and Vibrio vulnificus, should be considered in the differential diagnoses of these patients (9,10). Substantial challenges remain for Thailand, including identification of approximately 5,000 bodies and reconciliation of remains with the bereaved in Thailand and other countries. Forensic experts from Thailand and approximately 30 other countries are working together to complete the identification and processing of human remains. Other challenges include maintaining active surveillance to detect infectious disease outbreaks, treating wound infections, preventing posttraumatic injuries, maintaining safe drinking water and sanitation, and meeting mental health needs. As of January 19, a total of 7,423 survivors had sought psychiatric help (MOPH, unpublished data, 2005). Further mental health interventions will likely be needed to mitigate the postdisaster effects on residents of coastal communities. References
Figure 1 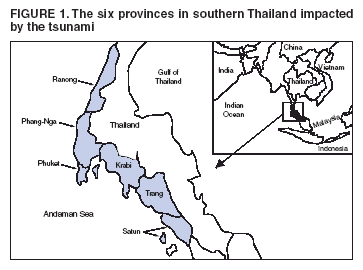 Return to top. Figure 2 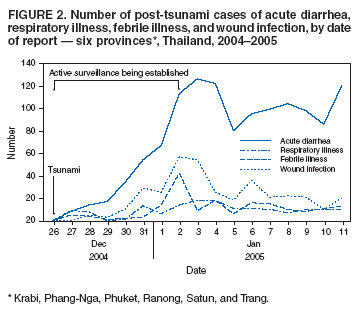 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 1/27/2005 |
|||||||||
This page last reviewed 1/27/2005
|