 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Indoor Air Quality in Hospitality Venues Before and After Implementation of a Clean Indoor Air Law --- Western New York, 2003Secondhand smoke (SHS) contains more than 50 carcinogens (1). SHS exposure is responsible for an estimated 3,000 lung cancer deaths and more than 35,000 coronary heart disease deaths among never smokers in the United States each year (2), and for lower respiratory infections, asthma, sudden infant death syndrome, and chronic ear infections among children (3). Even short-term exposures to SHS, such as those that might be experienced by a patron in a restaurant or bar that allows smoking, can increase the risk of experiencing an acute cardiovascular event (4). Although population-based data indicate declining SHS exposure in the United States over time (5), SHS exposure remains a common but preventable public health hazard. Policies requiring smoke-free environments are the most effective method of reducing SHS exposure (6). Effective July 24, 2003, New York implemented a comprehensive state law requiring almost all indoor workplaces and public places (e.g., restaurants, bars, and other hospitality venues) to be smoke-free. This report describes an assessment of changes in indoor air quality that occurred in 20 hospitality venues in western New York where smoking or indirect SHS exposure from an adjoining room was observed at baseline. The findings indicate that, on average, levels of respirable suspended particles (RSPs), an accepted marker for SHS levels, decreased 84% in these venues after the law took effect. Comprehensive clean indoor air policies can rapidly and effectively reduce SHS exposure in hospitality venues. The specific class of RSP monitored was PM2.5 (i.e., particulate matter that is <2.5 microns in diameter). Particles of this size are released in substantial amounts from burning cigarettes and are easily inhaled deep into the lungs. Baseline measurements were made during July 11--23 in a purposeful sample of 22 hospitality venues in three counties in western New York. Sites were selected to provide a range of venue types, sizes, and locations. The sample consisted of seven bars, six bar/restaurants, five restaurants, two bowling alleys, a pool hall, and a bingo hall. The venues were located in popular downtown entertainment districts and suburban areas and ranged from small neighborhood bars to large bar/restaurant chains. At baseline, smoking was occurring in 14 bars and restaurants and four large recreation venues. Two bar/restaurant combinations allowed smoking in the bar section but not in the adjoining restaurant section. In these two venues, air quality was monitored separately in the restaurant and bar areas. In two restaurants, no smoking was occurring at baseline because restaurants were already required to be smoke-free by local clean indoor air ordinances. Follow-up measurements of air quality were made in all 22 venues during September 9--November 1. The follow-up measurements were taken on the same day of the week and at approximately the same time of day as the measurements taken before the smoke-free law was implemented. The median time spent in each venue for all 44 baseline and follow-up observations combined was 38 minutes (range: 22--140 minutes). Measurements were taken at 1-second intervals. The number of persons and the number of burning cigarettes in each venue were recorded every 10 minutes during sampling, and the average number of persons and the average number of burning cigarettes in each venue were calculated. The volume of each venue also was measured*, and the cigarette density was calculated by dividing the average number of burning cigarettes by the room volume. An air monitor† was used to sample and record RSP levels. The monitor was placed in a central location on a table or bar near the height at which a person breathes air. The monitor recorded continuous measurements, which were averaged over time. The first and last minute of logged data were removed, and the remaining data points were averaged to provide an average concentration of PM2.5 within the venue. The percentage change in PM2.5 levels was then determined by comparing average PM2.5 levels in each venue before the law went into effect with levels after the law was implemented. The Wilcoxon signed-rank test was used to assess changes between pre-law and post-law PM2.5 levels, stratified by type of venue. The average PM2.5 concentration was substantially lower after the law went into effect in every venue where smoking or indirect SHS exposure had been observed at baseline, with a grand mean reduction in PM2.5 concentration of 84% (324 µg/m3 to 25 µg/m3; p<0.001) (Table). When stratified by the type of venue sampled, the average PM2.5 concentration decreased 90% (412 µg/m3 to 27 µg/m3; p<0.001) in the 14 bars and restaurants in which smoking was occurring at baseline (including bar/restaurant J, which was the only venue where smoking was observed during the post-law sampling). The restaurant portions of the two bar/restaurants that allowed smoking in the bar section but not in the restaurant section experienced an average 58% decrease in PM2.5 concentrations (156 µg/m3 to 31 µg/m3; p<0.001) after the law was implemented, even though they had only indirect SHS exposure at baseline. In the four other large recreation venues, which had larger volumes and lower smoker densities, the average PM2.5 concentration decreased 76% (101 µg/m3 to 18 µg/m3). In contrast, the PM2.5 concentration remained low and virtually constant in the two restaurants that were already smoke-free at baseline; these venues were not included in the grand mean calculation. Reported by: MJ Travers, KM Cummings, PhD, A Hyland, PhD, Dept of Health Behavior, Roswell Park Cancer Institute, Buffalo, New York. J Repace, MSc, Repace Associates, Bowie, Maryland. S Babb, MPH, T Pechacek, PhD, R Caraballo, PhD, Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The findings in this report indicate that a statewide law to eliminate smoking in enclosed workplaces and public places substantially reduced RSP levels in western New York hospitality venues. RSP levels were reduced in every venue that permitted smoking before the law was implemented, including venues in which only SHS from an adjacent room was observed at baseline. These findings are consistent with those of previous studies. In Delaware, a similar decline in RSP levels was observed in eight hospitality venues after smoking was prohibited there by state law (7). Previous studies also have assessed the health effects of smoke-free laws. One study indicated that respiratory health improved rapidly among a sample of bartenders after a state smoke-free workplace law was implemented in California (8), and another study reported a 40% reduction in acute myocardial infarction admissions to a regional hospital during the 6 months that a local smoke-free ordinance was in effect in Helena, Montana (9). The results of these studies (both those assessing changes in indoor air quality and those assessing changes in health) suggest that improvements can occur within months of policy implementation. The findings in this report are subject to at least two limitations. First, the venues sampled were not necessarily representative of venues in western New York. However, they did provide a range of venue types, sizes, and locations. Second, SHS is not the only source of indoor particulate matter. However, although ambient particle concentrations and cooking are additional sources of indoor particle levels, secondhand smoke is the largest contributor to indoor RSP pollution (3). Eliminating nonsmoker exposure to SHS is one of the four goals of comprehensive state tobacco-control programs, as set forth in CDC's Best Practices for Comprehensive Tobacco Control Programs (10). The results of the study described in this report indicate that a comprehensive statewide ban on smoking in indoor workplaces and public places can substantially reduce SHS exposure in these settings. Six states (California, Connecticut, Delaware, Maine, Massachusetts, and New York) currently meet the national health objective for 2010 calling for implementation of such laws. These six states account for approximately 23% of the U.S. population. Rhode Island also has adopted such a law, but the law does not take full effect until 2006. To further reduce the nearly 40,000 deaths among never smokers caused by SHS exposure each year, similar comprehensive laws are needed in the other 43 states and the District of Columbia. References
* The Zircon DM S50 Sonic Measure® (Zircon Corporation, Campbell, California) was used to perform this measurement. † The air monitor used was a TSI SidePak AM510 Personal Aerosol Monitor® (TSI, Inc., St. Paul, Minnesota). The SidePak uses a built-in sampling pump to draw air through the device, which then measures the real-time concentration in milligrams per cubic meter of PM2.5. The SidePak was calibrated against a SHS-calibrated nephelometer, which had been previously calibrated and used in similar studies. The SidePak was zero-calibrated before each use according to the manufacturer's specifications.
Table 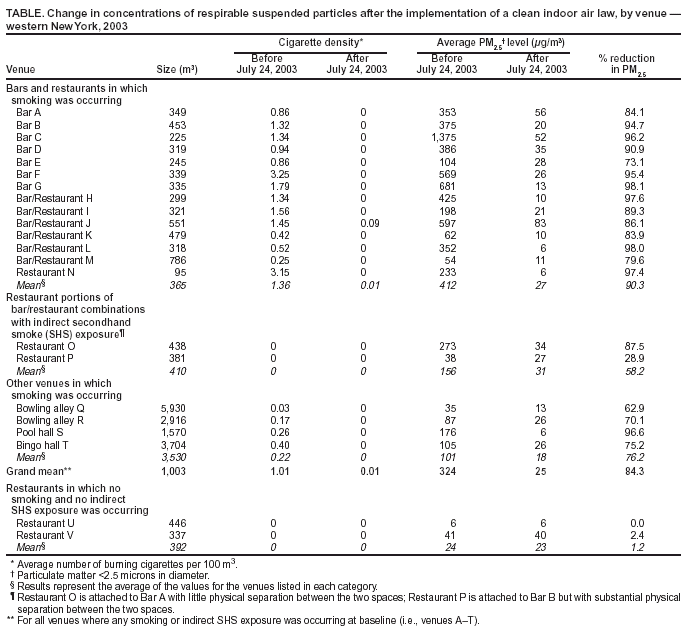 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/10/2004 |
|||||||||
This page last reviewed 11/10/2004
|