 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Use of Carbon Monoxide Alarms to Prevent Poisonings During a Power Outage --- North Carolina, December 2002Each year in the United States, approximately 500 persons die from unintentional carbon monoxide (CO) poisoning (1), often during electric power outages caused by severe storms (2--4). Use of residential CO alarms has been recommended to reduce the incidence of CO poisoning (5,6). In September 2000, Mecklenburg County, North Carolina (2002 population: 722,367), adopted a public health ordinance requiring a CO alarm in the majority of residences; all-electric residences without attached garages (35.4% of all homes) were exempt. The ordinance also permitted use of alarms without battery back-up. On December 4, 2002, an ice storm caused 78.9% of county households to lose power. During the next 9 days, 124 cases of symptomatic CO poisoning were reported. To characterize these poisonings and the effectiveness of the CO alarm ordinance, local emergency physicians, fire department authorities, and CDC conducted an investigation. This report summarizes the results of that investigation, which determined that 96.2% of the severe poisonings occurred in homes with no reported functioning CO alarm. As a result of these findings, on October 8, 2003, Mecklenburg County officials amended the ordinance to require alarms with battery back-ups in all residences (7). Officials in other communities should consider enacting such alarm ordinances to prevent CO poisonings. Data were extracted from 1) medical records of patients with CO poisoning at all hospitals serving Mecklenburg County, 2) emergency medical service (EMS) and fire department reports, and 3) readings from handheld CO meters operated by members of the Charlotte Fire Department (Figure 1). Cases were included if they occurred from the time electric power was lost on December 4 until full restoration on December 13. Confirmed CO exposure was defined as an elevated CO level in the ambient air of a person's home (>50 ppm) or in a person's blood (carboxyhemoglobin level >10% in smokers and >2% in nonsmokers) or in the blood of another person who shared the same breathing space. CO poisoning was defined as exposure plus any symptom (e.g., headache, nausea, dyspnea, or chest pain) not explained by a different diagnosis. Severe CO poisoning was defined as exposure and one or more of the following signs or symptoms: 1) loss of consciousness; 2) hypotension; or 3) physician-documented altered mental status, ataxia, or cardiac ischemia. Patients poisoned outside Mecklenburg County but transported into the county for medical care were excluded from the study; one burn victim and a group of warehouse workers who were mildly poisoned in an occupational exposure also were excluded. Characteristics of the study population (e.g., age, sex, and language spoken) were compared with those of the general population of Mecklenburg County (8). For persons aged >5 years, language was coded as "English" if all interviews by medical, rescue, and fire personnel were completed in English without documented difficulty or the use of an interpreter. If an interpreter was required, language was coded as "Spanish," "Asian/Pacific language," or "other language" to parallel classifications used by the U.S. Census Bureau. Data about homes (e.g., type, value, age, and CO alarm ordinance exemption status) were obtained from county records (9). A home was considered to have a functioning alarm if CO alarm activation was mentioned in a fire department dispatch record, fire department narrative report, EMS report, or hospital record for any household member. Among 161 persons with confirmed CO exposures, 124 (77.0%) had symptomatic poisoning (rate: 17.2 per 100,000 population), including 25 (15.5%) with severe poisoning and one death. Age data were known for 142 exposed persons; median age was 24 years (range: 6 days--90 years), and 59 (41.5%) were aged <18 years (relative risk [RR] = 2.0; 95% confidence interval [CI] = 1.4--2.8). Sex was known for 149 persons; 86 (57.7%) were female (RR = 1.3; 95% CI = 0.9--1.8). Language status was known for 128 persons aged >5 years; 72 (56.3%) did not speak English (RR = 15.1; 95% CI = 10.6--21.4), and both the Spanish-speaking (52 [40.6%]) and Asian/Pacific language--speaking (17 [13.3%]) populations were overrepresented (RR = 12.0; 95% CI = 8.4--17.1 and RR = 13.2; 95% CI = 7.9--22.0, respectively). The number of cases of asymptomatic CO exposure occurred almost equally among homes with a functioning CO alarm (n = 16) and homes with no reported functioning alarm (n = 18). However, 109 (87.9%) of the 124 cases of symptomatic CO poisoning occurred in homes in which no functioning CO alarm was reported (Figure 2); 25 (19.7%) of 127 persons with CO exposure in these homes had severe poisoning, including one who died. Of the 26 severe poisonings, 25 (96.2%) occurred in homes with no reported functioning alarm. Of the 56 CO exposure incidents reported, 30 (53.6%) occurred in rental homes (RR = 1.7; 95% CI = 1.0--3.0). Among the CO exposures, 46 (83.6%) were attributed to portable devices, including 41 (74.5%) grills (i.e., charcoal or gas) and electric generators (Table). CO exposures occurred more often in older residences (median age: 34 years; range: 1--62 years, compared with a county median of 18 years) and in homes of lower value (median value: $89,200; range: $19,000--$247,200, compared with a county median of $165,376 [rental homes excluded]). Exposure incidents occurred almost proportionally in homes subject to and homes exempt from the CO alarm ordinance; 35.4% of homes in Mecklenburg County were exempt from the ordinance, and 27.9% of the CO incidents were in exempt homes (RR = 0.7; 95% CI = 0.4--1.4). Reported by: EJ Lavonas, MD, WP Kerns II, MD, CA Tomaszewski, MD, TH Blackwell, MD, PN Galaska, MD, Carolinas HealthCare System; TL Hay, DO, Presbyterian Healthcare; GE McCormick, Charlotte Fire Dept, Charlotte, North Carolina. AS Brown, PhD, JA Mott, PhD, Div of Environmental Hazards and Health Effects, National Center for Environmental Health, CDC. Editorial Note:Gas furnaces and other fuel-burning appliances are common sources of CO poisonings (1). However, during power outages, all-electric homes can be just as likely as gas-fueled homes to harbor sources of CO poisoning (i.e., portable cooking and heating devices such as grills and generators) (2--4). The findings in this report indicate that a functioning CO alarm can protect against severe CO poisoning during a power outage, supporting the recommendation of the U.S. Consumer Product Safety Commission (6). A dual strategy of CO alarm deployment and public education might reduce CO exposures and poisonings; safety messages should emphasize that grills and generators must never be used inside a home or garage. However, because of language barriers, multilingual educational campaigns are necessary to reach non-English--speaking populations. After the North Carolina ice storm, recent immigrants and other non-English--speaking residents were at particular risk for CO poisoning, with the majority prevented from receiving multilingual emergency messages via television because of loss of electric power. In 2002, a total of 14,714 (4.6%) Mecklenburg County households had no adult who spoke English fluently, and 18,198 (2.5%) county residents had resided in the United States <2 years (8). The findings in this report are subject to at least two limitations. First, no distinctions could be made between homes with no alarms and homes with alarms that did not function because they had no battery power source or their batteries failed or were absent. Second, the number of survivors suffering permanent injury as a result of CO poisoning was not determined; approximately 10%--30% of CO poisoning survivors have persistent or delayed neurologic injury (10). After receiving these findings, the Mecklenburg Board of County Commissioners amended the county's CO alarm ordinance to require an alarm in every residence, regardless of heating source and appliance type, and a battery back-up in each CO alarm (7). County officials continue to provide free alarms to low-income homeowners and to target recent immigrants and other non-English--speaking residents with a multilingual program to prevent CO poisonings. Officials in other communities should consider these strategies in adopting CO poisoning--prevention programs. References
Figure 1  Return to top. Figure 2 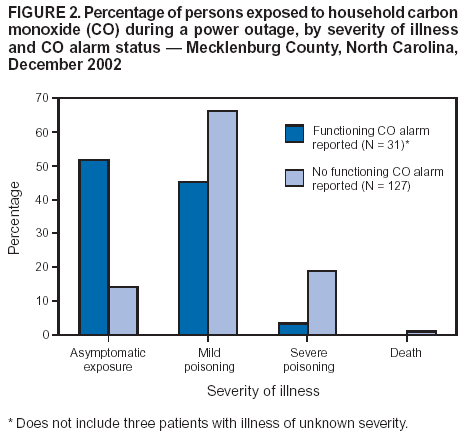 Return to top. Table  Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 3/11/2004 |
|||||||||
This page last reviewed 3/11/2004
|