 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
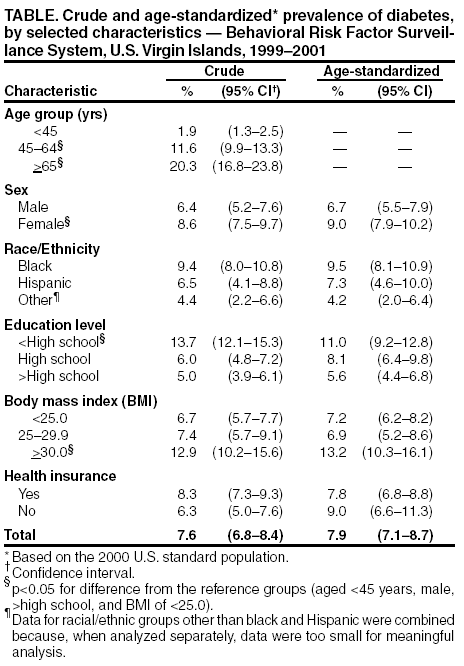
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Prevalence of Diabetes --- U.S. Virgin Islands, 1999--2001The U.S. Virgin Islands (USVI) comprises four islands (St. Croix, St. John, St. Thomas, and Water Island) (2000 population: 108,612) located 70 miles east of Puerto Rico. The median age of persons residing in USVI is 33.4 years (range: 0--110 years), and 87% are aged <60 years; the majority of the residents are either black (76.2%) or Hispanic (14.0%) (1). In 1997, diabetes was the fifth leading cause of death in USVI (2). Historically, the prevalence of diabetes has been lower among blacks in USVI than among blacks in the 50 states (3). To characterize the prevalence of diabetes in USVI, CDC analyzed data from the Behavioral Risk Factor Surveillance System (BRFSS) for 1999--2001 (4). This report summarizes the findings from the analysis, which indicate that approximately 8.0% of USVI residents aged >18 years have diagnosed diabetes, and the prevalence of diabetes among blacks and Hispanics in USVI is comparable to that among blacks and Hispanics in the 50 states. To prevent the burden of diabetes and diabetes-related complications in residents and to improve the quality of life for persons with diabetes, initiatives in USVI should target all persons with diabetes. BRFSS is a state-based, random-digit--dialed telephone survey of the U.S. civilian, noninstitutionalized population aged >18 years in the 50 states, the District of Columbia, Guam, Puerto Rico, and USVI. Response rates ranged from 75.5% in 1999 to 57.5% in 2001. BRFSS data for 1999--2001 were combined to estimate diabetes prevalence. Persons were classified as having diabetes if they responded "yes" to the question, "Has a doctor ever told you that you have diabetes?" Women reporting gestational diabetes only (i.e., <1.5%) were excluded. Persons with missing, refused, or unknown responses were coded as "missing." Logistic regression analyses were used to assess the association of diabetes prevalence with USVI residents after controlling for age, sex, race/ethnicity, education level, and body mass index (BMI). Values for BMI, which is the ratio of weight in kilograms to height in meters squared (kg/m2), were grouped in three categories (i.e., <25.0, 25--29.9, and >30.0). Race/ethnicity was categorized as black, Hispanic, or other (non-Hispanic white, Asian/Pacific Islander, American Indian/Alaska Native, and other). All analyses were conducted by using SAS (version 8) with SUDAAN to account for the complex survey design. The data were weighted to reflect the age, sex, and racial/ethnic distribution of noninstitutionalized adults in USVI. In addition to calculating crude estimates, age-standardized estimates were calculated by using direct standardization to the 2000 U.S. population. Multivariate-adjusted prevalence was computed as predicted marginal values from a logistic model that controlled for sex, race/ethnicity, education, age group, and BMI, and the significance of differences was determined from t-tests. During 1999--2001, the prevalence of diabetes in USVI was 7.6% (95% confidence interval [CI] = 6.8%--8.4%) (Table). The prevalence increased with age from 1.9% among persons aged <45 years to 11.6% among persons aged 45--64 years to 20.3% among persons aged >65 years (p<0.05). After standardizing for age, the prevalence of diabetes was higher among women (9.0%) than among men (6.7%) (p<0.05). Age-standardized prevalence did not differ statistically between blacks (9.5%) and Hispanics (7.3%). Among adults with less than a high school education, prevalence was approximately twice that of those with more than a high school education (11.0% versus 5.6%; p<0.05). Persons with BMI of >30.0 were approximately twice as likely to have diabetes as those with BMI of <25.0 (13.2% versus 7.2%; p<0.05). Health insurance was not significantly associated with diabetes (p>0.05), with rates of 9.0% for the uninsured and 7.0% for insured. A multivariate analysis indicated that the excess risk for diabetes persisted for persons aged >65 years, compared with those aged <45 years (predicted marginal difference [PMD] = 18.0 percentage points; p<0.05). Persons with less than a high school education had an excess risk (PMD = 4.1 percentage points; p<0.05), compared with those with more than a high school education. Adults with a BMI of >30.0 also had excess risk, compared with those with a BMI of <25.0 (PMD = 6.0 percentage points [p<0.05]). Reported by: A Thurland, MPH, U.S. Virgin Islands Dept of Health. Q Mukhtar, PhD, RB Gerzoff, MS, E Tierney, MPH, G Beckles, MD, Div of Diabetes Translation, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:During 1999--2001, approximately 8.0% of USVI residents aged >18 years had diagnosed diabetes. Prevalence was highest among persons aged >65 years, persons with less than a high school education, and those with a BMI of >30. The estimated prevalence among USVI blacks (9.5%) and Hispanics (7.3%) is comparable to that of blacks (9.7%) and Hispanics (8.0%) in the 50 states (4,5). The estimated prevalence of diabetes for USVI obtained in this analysis is approximately 4 percentage points lower than that obtained in a study conducted during 1995--1998 among adults aged >20 years residing on St. Croix (6). This difference might be explained by differences in the study design and study population (e.g., economic distribution). To prevent the burden of diabetes and to improve the quality of life for persons with diabetes, initiatives in USVI should target all persons with diabetes, particularly the elderly and those with a low-level education. The USVI Diabetes Prevention and Control Program (USVIDPCP) is working with its local and national partners to increase diabetes awareness and to improve quality of diabetes care for all, with special focus on underserved and elderly population. The findings in this report are subject to at least two limitations. First, BRFSS surveys reach only noninstitutionalized populations with telephones; therefore, these findings might not be generalizable to nursing home residents, other institutionalized populations, or persons without telephones. Second, BRFSS diabetes data are self-reported and are subject to recall bias; however, several validity studies indicate that persons with diabetes report their diabetes status accurately (7). Further efforts are needed to educate USVI residents regarding the seriousness and management of diabetes. CDC provides resources and technical assistance to the USVIDPCP to define the burden of diabetes and its complications and to help improve access to quality diabetes care. USVIDPCP plans to incorporate primary prevention in their strategies. Continued surveillance through BRFSS will be an important tool in monitoring changes in diabetes prevalence in USVI. References
 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 7/10/2003 |
|||||||||
This page last reviewed 7/10/2003
|