 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
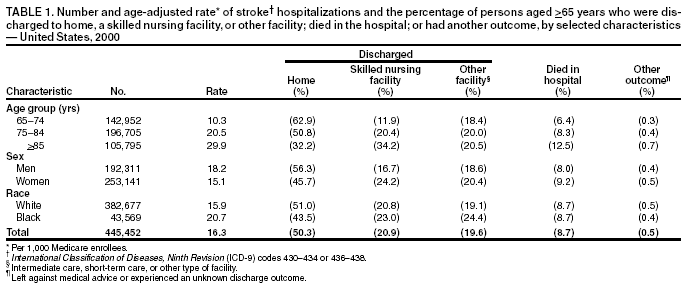
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Public Health and Aging: Hospitalizations for Stroke Among Adults Aged >65 Years --- United States, 2000Stroke is the third leading cause of death in the United States and a major cause of serious, long-term disability among adults; the projected cost of stroke during 2003 is $51 billion, including $12 billion in nursing home costs (1). During 1988--1997, the rate of hospital admissions for stroke increased 18.6%, from approximately 560 per 100,000 population in 1988 to 664 in 1997 (2). To assess the burden of stroke hospitalizations and discharge status after hospitalization among U.S. residents aged >65 years, CDC analyzed Medicare hospital claims for persons with stroke during 2000 for the 50 states and the District of Columbia (DC). This report summarizes the results of that analysis, which indicate that geographic variation exists in both rates of hospitalization for stroke and patient discharge status. Reducing the burden of stroke in the United States will require primary prevention and control of risk factors, public education, early evaluation and treatment of persons with acute stroke, and effective secondary prevention among persons living with stroke. Medicare hospital claims and enrollment record data for 2000 were obtained from the Centers for Medicare and Medicaid Services. A hospitalization for stroke was defined as one for which the principal diagnosis on the hospital claims record during 2000 was classified according to the International Classification of Diseases, Ninth Revision (ICD-9) codes 430--434 or 436--438. The number of persons at risk (i.e., U.S. residents in the 50 states and DC aged >65 years who were entitled to Medicare Part A benefits on July 1, 2000, excluding members of health maintenance organizations) was obtained from Medicare enrollment records. Age-adjusted hospitalization rates per 1,000 Medicare enrollees were calculated by using the 2000 U.S. standard population. Outcomes included discharge to home, a skilled nursing facility, or another care facility (i.e., intermediate care, short-term care, or other type of facility); death during the hospital stay; or other outcome (i.e., left against medical advice or experienced an unknown discharge outcome). During 2000, a total of 445,452 hospitalizations among Medicare enrollees were attributed to stroke, resulting in an age-adjusted rate of 16.3 per 1,000 enrollees. Stroke hospitalization rates increased with age and were higher among men than women and among blacks than whites (Table 1). The majority of hospitalizations for stroke resulted in discharge to home (50.3%), followed by discharge to a skilled nursing facility (21.0%), discharge to another facility (19.6%), and death (8.7%). A total of 0.5% either left against medical advice or experienced an unknown discharge outcome. Discharge status varied by age. Approximately half (54.7%) of persons aged >85 years were discharged to either a skilled nursing facility or other facility, compared with 30.3% of persons aged 65--74 years. Higher proportions of women and blacks were discharged to either a skilled nursing facility or other facility than men or whites, respectively. Age-adjusted stroke hospitalization rates per 1,000 Medicare enrollees varied by state (range: 11.8 [New Mexico]--21.9 [Mississippi]) (Table 2). Discharge status also varied by state; the proportion of persons hospitalized for stroke who were discharged to home ranged from 41.0% (Massachusetts) to 58.0% (West Virginia), and the proportion discharged to a skilled nursing facility ranged from 10.8% (Louisiana) to 34.4% (Connecticut). Reported by: HF Davis, PhD, JB Croft, PhD, AM Malarcher, PhD, C Ayala, PhD, TL Antoine, MPH, A Hyduk, MPH, GA Mensah, MD, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:As the U.S. population continues to age, stroke hospitalization rates and the proportion of persons discharged to skilled nursing facilities might increase (3). Older stroke patients, those with specific neurologic deficits (i.e., language deficits, facial weakness, and leg weakness), and those hospitalized longer are more likely to be discharged to a skilled nursing facility (3--5). Approximately 20% of stroke patients die within 1 year after discharge (6), and the types of post-acute care change over time, with an increasing proportion of patients using a combination of services (4). Use of Medicare services and Medicare spending rates vary across the United States (4). State-specific variations in discharge location probably reflect differences in patient demographics, medical practice styles, local regulatory practices, and availability and accessibility of post-acute care facilities (4). Payment for post-acute care is one of the fastest growing categories in Medicare spending, and stroke has been identified as one of the diagnostic-related groups with the highest number of beneficiaries using post-acute care (4). After adjustment for stroke severity, home health care for Medicare stroke patients results in better functional outcomes and is more cost-effective than skilled nursing home care, rehabilitation care, and recuperation at home with no formal care at both 6 weeks and 6 months after discharge (3). The findings in this report are subject to at least four limitations. First, the data cannot be generalized to other age and racial/ethnic groups because the population included only Medicare enrollees, and small numbers precluded the use of other racial/ethnic groups in this analysis. Second, the accuracy of physician and administrative reporting of ICD codes and the severity and timing of stroke could not be determined by using Medicare hospital claims. Third, these records could not be used to determine whether a person was discharged for a new or a recurrent stroke. Finally, because Medicare hospital claims data do not provide follow-up information, only discharge status was examined. Stroke hospitalization rates can be reduced by educating the public about the control and treatment of the major risk factors for stroke (i.e., high blood pressure, high cholesterol, smoking, and diabetes). Prompt treatment after a stroke decreases long-term disability, which reduces the need for admission to a skilled nursing facility; for example, thrombolytic therapy is time-dependent and beneficial to ischemic stroke patients only if administered within 3 hours of symptom onset (7). Educating health-care providers and officials who determine Medicare payment policies about optimal post-acute stroke care might help decrease the need to use skilled nursing facilities (4). Reducing the burden of stroke in the United States will require 1) primary prevention and control of risk factors; 2) public education about signs and symptoms of stroke, the need for emergency response (i.e., calling 911), and the importance of immediate transport to a primary stroke center (i.e., a specialized emergency facility for treatment of stroke); 3) early appropriate evaluation and treatment of persons with acute stroke; and 4) effective secondary prevention among persons living with stroke (8). References
 Return to top. Table 2 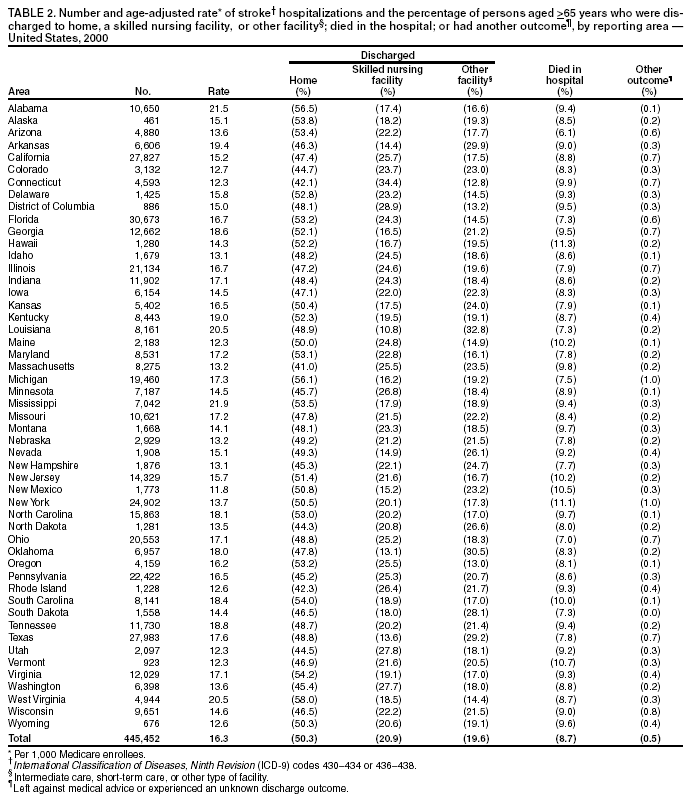 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 6/26/2003 |
|||||||||
This page last reviewed 6/26/2003
|