 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
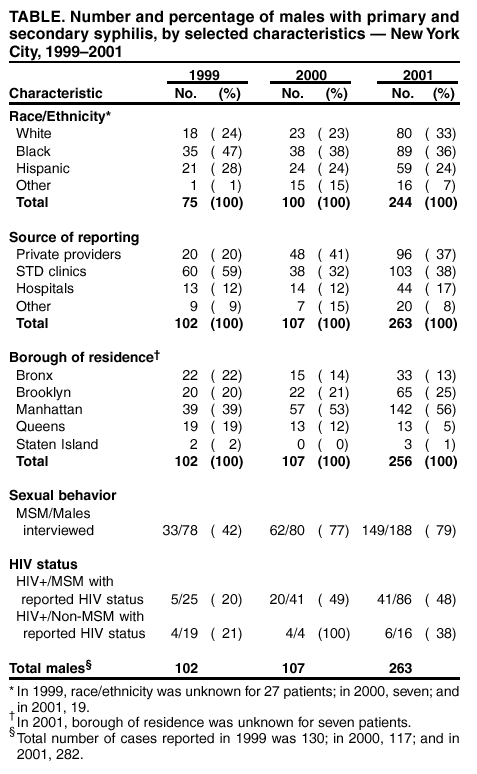
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Primary and Secondary Syphilis Among Men Who Have Sex with Men --- New York City, 2001After declining steadily for 10 years, the number of reported cases of primary and secondary (P&S) syphilis more than doubled in New York City (NYC) from 117 in 2000 to 282 in 2001 (1). The increases have occurred primarily among men who have sex with men (MSM). Of particular concern is the high proportion of syphilis cases among MSM who also have human immunodeficiency virus (HIV). This report summarizes 2001 P&S syphilis data for NYC and compares it with surveillance data for 1999 and 2000; findings indicate a substantial increase in the number of syphilis cases among MSM. These data suggest increases in high-risk sexual behavior among some MSM and underscore the importance of coordinating efforts between the MSM community public health officials, and health-care providers to strengthen HIV-prevention efforts. Syphilis cases are reported to the NYC Department of Health and Mental Hygiene (NYCDOHMH) by private health-care providers, health-care institutions, and laboratories in accordance with New York state and NYC laws. NYCDOHMH reports confirmed syphilis cases to CDC. NYCDOHMH interviews persons with syphilis of <1 year duration to obtain demographic and risk-behavior data and to provide disease-intervention counseling, which facilitates locating and treating sex partners in addition to treating patients. A case of P&S syphilis was defined as darkfield-positive lesions or reactive serologic tests for syphilis and accompanying symptoms in a person residing in NYC. For this analysis, patients were classified as MSM if they reported having sex with another man during the time when syphilis might have been acquired or transmitted to a sex partner. This time is based on stage of disease at the time of treatment. For primary syphilis, this period is defined as 3 months before the date of onset of a syphilitic lesion through the date of treatment, and for secondary syphilis, from 6½ months before onset of associated symptoms (e.g., rash, mucocutaneous lesions, lymphadenopathy, and fever) through the date of treatment. Behavioral data collected from male patients included sexual behavior, HIV status, number and sex of sex partners, frequency of condom use, alcohol and recreational drug use, and venues for meeting sex partners. HIV status was determined by self-reports or by laboratory-confirmed tests from specimens collected at the time of the interview or treatment. During 2001, a total of 282 cases of P&S syphilis were reported to NYCDOHMH; 263 (93%) were in males. The overall P&S syphilis rate in 2001 (3.5 per 100,000 population) was the highest since 1995, and the rate among males (6.9) was the highest since 1994 (Figure). The male:female case ratio for P&S syphilis increased from 3.6:1 in 1999 to 13.8:1 in 2001. The median age of male patients in 2001 was 35 years (range: 16--64 years); mean age was similar to that during previous years (Table). The number of cases among males increased in all racial/ethnic groups in 2001. Among males whose race/ethnicity was known, the proportion of cases that occurred among whites increased in 2001 (33%), compared with the proportion in 2000 (23%) and in 1999 (24%). In comparison, the proportion of cases among black males was less in 2001 (36%) and 2000 (38%) than in 1999 (47%). A greater proportion of cases was reported from private health-care providers and private hospitals in 2000 and 2001 than in 1999. The proportion of male patients residing in Manhattan was greater in 2000 and 2001 than in 1999. Information about sex partners was obtained for 188 males in 2001; of these, 79% were classified as MSM compared with 77% in 2000 and 42% in 1999 (Table). HIV status was known for 86 MSM in 2001; of these, 48% were HIV-infected compared with 49% in 2000 and 20% in 1999 (Table). Behavioral data from interviews of 103 MSM patients in 2001 indicated that during the interval when syphilis could have been transmitted or acquired, 77 (75%) reported having more than one sex partner, and 37 (36%) reported using alcohol or other recreational drugs. The venues cited most frequently for meeting sex partners were nightclubs and bars (31%), public cruising sites (22%), Internet chat rooms (14%), and bathhouses (11%). A total of 5% of MSM patients reported exchanging sex for money. Reported by: C de Luise, MPH, S Blank, MD, J Brown, S Rubin, A Meyers, MPH, L Neylans, MPA, STD Control Program, New York City Dept of Health and Mental Hygiene, New York, New York. G Paz-Bailey, MD, L Markowitz, MD, Div of STD Prevention, National Center for HIV, STD, and TB Prevention, CDC. Editorial Note:The findings in this report indicate an increasing rate of P&S syphilis among males in NYC, particularly among MSM, a pattern seen in several urban areas of the United States (2--4). Data obtained from case interviews indicated high-risk behavior among male patients, including having multiple sex partners, substance use, and frequenting venues in which they were likely to meet sex partners. A high proportion of patients with syphilis were infected with HIV. Transmission of HIV is enhanced by syphilis and other sexually transmitted diseases (STDs). Syphilis outbreaks often have affected economically disadvantaged minority groups with poor access to health care and have been commonly associated with heterosexual transmission, drug use, and exchange of sex for money or drugs. In comparison, urban outbreaks, including that in NYC, involve whites and minority groups, MSM, and persons who use private health-care services. The increasing rate of MSM cases is not unique to NYC; since 1997, syphilis outbreaks among MSM have occurred in other U.S. cities, including Seattle, Chicago, San Francisco, Los Angeles, and Miami (2--4). In each of these outbreaks, high rates of HIV co-infection were documented, ranging from 20% to 73%. Increases in gonorrhea among MSM also have been observed in the United States (5) and internationally (6). Several factors might be associated with increased high-risk sexual behavior among MSM, including the availability of highly active antiretroviral therapy (HAART) (7). HAART has had a substantial impact on the decline in AIDS-related mortality and is responsible for improved physical well-being, allowing higher rates of sexual activity than before treatment. Increased sexual risk taking might also be related to "AIDS burnout," which is associated with years of exposure to prevention messages and long-term efforts to maintain safer sex practices (8). Other factors described among young MSM include alcohol and drug use, unrecognized HIV infection, and misperception of risk (9). In response to the outbreak, NYCDOHMH has enhanced syphilis surveillance, intensified education about prevention and treatment of syphilis to affected communities, strengthened partnerships with community-based organizations, and encouraged health-care providers to increase screening of patients at high risk for other STDs and HIV. Despite these efforts, increases in syphilis rates, including among MSM, have continued in 2002 (1). A similar pattern has been observed in Los Angeles, where, despite extensive efforts to control a syphilis outbreak among MSM, syphilis transmission in this group has continued for several years (10). The findings in this report are subject to at least two limitations. First, information from public health records and from interviews was not collected systematically; variation occurred in data collection and recording. Second, behavioral data were not available for all patients. The increasing rate of syphilis among MSM reflects increased sexual risk-taking behavior among subpopulations of MSM, many of whom have HIV. Such behavior increases the risk for STDs and HIV and threatens the health of MSM. Public health officials, the MSM community, and others should continue to develop and implement new, effective prevention approaches to reduce the risk for STDs and HIV among MSM. References
 Return to top. Figure 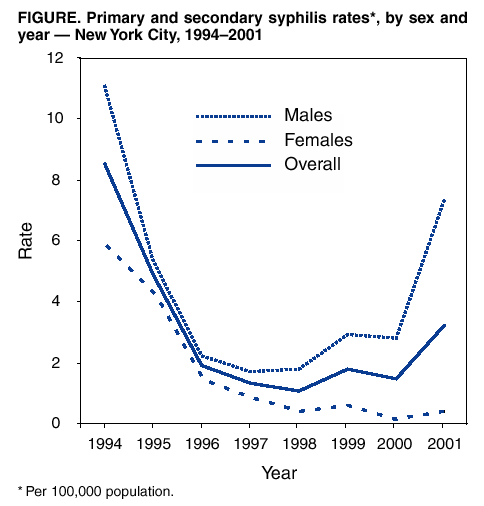 Return to top. |
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services. |
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 9/26/2002
|
|
|||||
|
HOME |
ABOUT MMWR |
MMWR SEARCH |
DOWNLOADS |
RSS
|
CONTACT
|
|||||
|
|
|||||
|
This page last reviewed 9/26/2002