 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. State-Specific Mortality from Sudden Cardiac Death --- United States, 1999Each year in the United States, 400,000--460,000 persons die of unexpected sudden cardiac death (SCD) in an emergency department (ED) or before reaching a hospital (1). Based on the latest U.S. mortality data, this report summarizes and analyzes 1999 national and state-specific SCD data. Reducing the proportion of out-of-hospital* SCDs would decrease the overall incidence of premature death in the United States. Heart attacks are the major cause of SCD; approximately 70% of SCDs are caused by coronary heart disease. National efforts are needed to increase public awareness of heart attack symptoms and signs and to reduce delay time to treatment. National and state mortality statistics for this report were based on data from death certificates filed in state vital statistics offices and were compiled by CDC (2). Demographic data (e.g., age and race/ethnicity) listed on death certificates were reported by funeral directors usually from information provided by the family of the decedent. Causes of death on death certificates were reported by a physician, medical examiner, or coroner. Cardiac disease death was defined as one for which the underlying cause of death was classified and coded using the International Classification of Diseases (ICD-10), Tenth Revision, for diseases of the heart (codes I00-I09, I11, I13, and I20-I51) or congenital malformations of the heart (Q20-Q24†). SCD was defined for this report as a death from cardiac disease that occurred out-of-hospital or in an ED or one in which the decedent was reported to be "dead on arrival" at a hospital. Populations at risk were defined on the basis of U.S. census bureau estimates of resident populations; age-adjusted death rates were standardized by the direct method to the 2000 projected U.S. population (3). Among 728,743 cardiac disease deaths that occurred during 1999, a total of 462,340 (63.4%) were SCDs; 120,244 (16.5%) occurred in an ED or were dead on arrival, and 341,780 (46.9%) occurred out-of-hospital. Women had a higher total number of cardiac deaths and higher proportion of out-of-hospital cardiac deaths than men (51.9% of 375,243 and 41.7% of 353,500, respectively), and men had a higher proportion of cardiac deaths that occurred in an ED or were dead on arrival (21.2% of 353,500 and 12.0% of 375,243, respectively) (Table 1). SCDs accounted for 10,460 (75.4%) of all 13,873 cardiac disease deaths in persons aged 35--44 years, and the proportion of cardiac deaths that occurred out-of-hospital increased with age, from 5.8% in persons aged 0--4 years to 61.0% in persons aged >85 years. SCDs accounted for 63.7% of all cardiac deaths among whites, 62.3% among blacks, 59.8% among American Indians/Alaska Natives, 55.8% among Asians/Pacific Islanders, and 54.2% among Hispanics. Whites had the highest proportion of cardiac deaths out-of-hospital, and blacks had the highest proportion of cardiac deaths in an ED or dead on arrival (Table 1). The age-adjusted SCD rate was 47.0% higher among men than women (206.5 and 140.7 per 100,000 population, respectively). Blacks had the highest age-adjusted rates (253.6 in men and 175.3 in women) followed by whites (204.5 in men and 138.4 in women), American Indians/Alaska Natives (132.7 in men and 76.6 in women), and Asians/Pacific Islanders (111.5 in men and 66.5 in women). Non-Hispanics (217.8 in men and 147.3 in women) had higher age-adjusted SCD rates than Hispanics (118.5 in men and 147.3 in women). In 1999, the state-specific proportion of all cardiac deaths that was SCD ranged from 57.2% (Hawaii) to 72.9% (Wisconsin) (Table 2). Other states with a high proportion of SCDs were Idaho (72.2%), Utah (72.1%), Colorado (71.3%), Oregon (71.0%), Connecticut (70.5%), Rhode Island (70.0%), South Dakota (69.8%), Montana (69.6%), and Vermont (69.5%). Age-adjusted SCD rates (per 100,000 population) in 1999 ranged from 114.6 (Hawaii) to 212.2 (Mississippi). Reported by: ZJ Zheng, MD, JB Croft, PhD, WH Giles, MD, CI Ayala, PhD, KJ Greenlund, PhD, NL Keenan, PhD, L Neff, PhD, WA Wattigney, M.Stat, GA Mensah, MD, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:Despite advances in the prevention and treatment of heart disease and improvements in emergency transport, the proportion of cardiac deaths classified as "sudden" remains high, probably because of the unexpected nature of SCD and the failure to recognize early warning symptoms and signs of heart disease. The age-adjusted SCD rates and the state-specific variation in the proportion of SCDs suggest a need for increased public awareness of heart attack symptoms and signs. The finding that cardiac deaths out-of-hospital were more likely to occur among women than men is consistent with findings that women more often delay seeking help for heart attack symptoms (4). Early recognition of heart symptoms and signs leads to earlier artery opening treatment or defibrillation that results in less heart damage and deaths. Education and media efforts should inform the public about heart disease symptoms and signs, particularly women and young adults who might dismiss heart disease as a problem of men and the elderly (5). Health-care providers should be alert for atypical symptoms of heart disease among female and young adult patients (6). The findings in this report are subject to at least three limitations. First, the cause of death information reported on the death certificate by the certifier is not always validated by a medical record or autopsy verification. The reliability and accuracy of the underlying cause of death also depend on the information reported by the certifier and on the state and national nosologists who determine the codes and the underlying causes. Second, because time of onset of disease symptoms and time of death are not available for analysis, the suddenness of death is determined arbitrarily and needs to be validated on the basis of clinical criteria on time frames. Third, data are subject to misclassification of race/ethnicity on death certificates, which might result in underestimating the number of deaths among American Indians/Alaska Natives, Asians/Pacific Islanders, and Hispanics and overestimating the number of deaths among blacks and whites (7). The proportion of SCDs that occur out-of-hospital has increased since 1989 (1). Death and disability from a heart attack can be reduced if persons having a heart attack can immediately recognize its symptoms (8) and call 9-1-1 for emergency care. These symptoms are chest discomfort or pain; pain or discomfort in one or both arms or in the back, neck, jaw, or stomach; and shortness of breath. Other symptoms are breaking out in a cold sweat, nausea, and light headedness (9). Prevention of the first cardiac event through risk factor reduction (e.g., tobacco control, weight management, physical activity, and control of high blood pressure and cholesterol intake) should continue to be the focus of public health efforts to reduce the number of deaths from heart disease. Education and systems support to promote physician adherence to clinical practice guidelines and more timely access to emergency cardiac care also are important to the prevention and early treatment of a heart attack. Prehospital emergency medical service systems can assist in reducing SCD rates by dispatching appropriately trained and properly equipped response personnel as rapidly as possible in the event of cardiac emergencies. However, national efforts are needed to increase the proportion of the public that can recognize and respond to symptoms and can intervene when someone is having a heart attack, including calling 9-1-1, attempting cardiac resuscitation, and using automated external defibrillators until emergency personnel arrive. References
* A death that occurs in a nursing home, residence, and other unspecified place outside of a hospital. † Diseases of the heart (ICD-10 codes I00-I09, I11, I13, and I20-I51) represent certain disease types (e.g., coronary heart disease, cardiomyopathy, dysrhythmias, and conduction system disorders, hypertensive heart disease, carditis and valvular heart disease, pulmonary heart disease, and heart failure). Congenital malformations of the heart (Q20-Q24) represent other disease types (e.g., congenital malformations of cardiac chambers and connections, cardiac septa, and pulmonary, tricuspid, and aortic and mitral valves). These codes are comparable to the ICD-9 codes of 390-398, 402, 404-429, and 745-746. Table 1 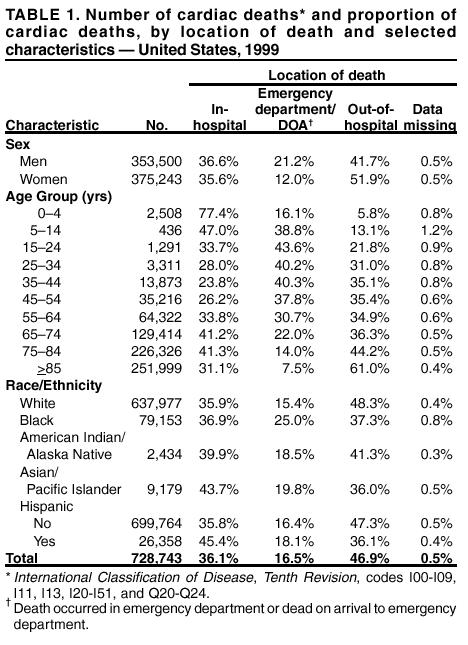 Return to top. Table 2 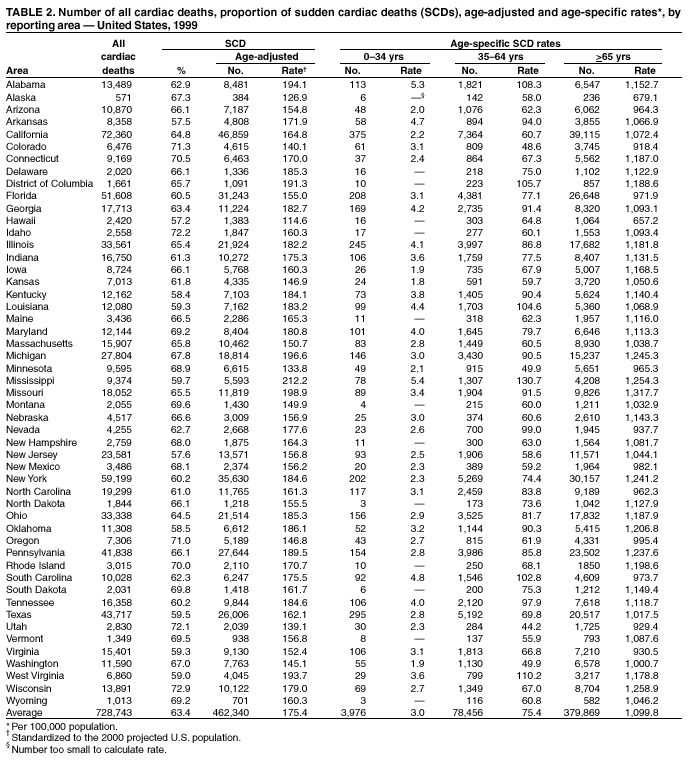 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 2/14/2002 |
|||||||||
This page last reviewed 2/14/2002
|