 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Impact of Targeted, School-Based Dental Sealant Programs in Reducing Racial and Economic Disparities in Sealant Prevalence Among Schoolchildren --- Ohio, 1998--1999Despite the availability of highly effective measures for primary prevention, dental caries (tooth decay) remains one of the most common childhood chronic diseases (1). When properly placed, dental sealants are almost 100% effective in preventing caries on the chewing surfaces of first and second permanent molar teeth (2). However, sealants remain underused, particularly among children from low-income families and from racial/ethnic minority groups (3). Schools traditionally have been a setting for both dental disease prevention programs and for oral health status assessment. To determine the prevalence of dental sealant use among third grade students from schools with and without sealant programs, during the 1998--99 school year, the Ohio Department of Health conducted an oral health survey among schoolchildren. This report summarizes the results of this survey, which indicate that targeted, school-based dental sealant programs can substantially increase prevalence of dental sealants. Providing sealant programs in all eligible, high-risk schools could reduce or eliminate racial and economic disparities in the prevalence of dental sealants. The study population was derived from a sample of elementary schools in Ohio. Eligible schools included those with complete data on enrollment and that participated in the free or reduced-cost lunch program. Of 1857 public schools with complete data, 335 (representing 87 of 88 Ohio counties) were selected randomly using the probability-proportional-to-size approach. The prevalence of dental sealant use was compared among students attending schools with a program (69 schools) to that of students attending schools without a program (266 schools). On the basis of a student census in randomly selected classrooms (grades 1--3), 34,668 students were eligible for the survey; 19,471 of these were from the third grade. Parental consent was obtained and oral screenings performed on 11,191 third graders (57.5% of those eligible). Using mouth mirrors, artificial lighting, and dental explorers, 12 dental professionals completed the clinical screening. Weighted data were analyzed using Stata software (4). The Design-Based Pearson Statistic was used to test for association. Weighting was based on the relation between the number of children screened and the number in the underlying eligible population. Among third grade students surveyed in Ohio, 34.2% (95% confidence interval [CI]=32.1%--36.4%) had at least one dental sealant on a permanent molar tooth. At schools with dental sealant programs, 56.7% of third grade students had a sealant, compared with 28.2% of students at schools without sealant programs (Table 1). By race, 61.6% of white third grade students in schools with sealant programs had sealants, compared with 30.0% of white third grade students in schools without programs. For black third grade students, 50.8% in schools with sealant programs had a sealant, compared with 17.7% of black third grade students in schools without programs. Using eligibility for free or reduced-cost lunch programs as a proxy for low income, 54.4% of eligible third grade students in schools with sealant programs had a sealant, compared with 64.8% of third grade students not eligible for the program in the same schools; 19.0% of eligible third grade students in schools without programs had a sealant. Among third grade students in schools with sealant programs, the prevalence of sealants was similar for students with and without health insurance. Among students who attended schools with sealant programs and had sealants on their teeth, 70.2% (95% CI=62.8--76.7) received them at school. Students who received sealants at school represented 22.6% of all Ohio students with sealants. Reported by: MD Siegal, DDS, DL Miller, MBA, D Moffat, MPA, Ohio Dept of Health; S Kim, PhD, P Goodman, MS, Center for Biostatistics, Ohio State Univ, Columbus. Surveillance, Investigations and Research Br, Div of Oral Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The findings in this report indicate that school-based dental sealant programs in Ohio that are targeted to groups at high risk for dental caries and least likely to receive regular dental care can substantially increase sealant prevalence. Third grade students in schools with dental sealants programs have two to three times greater prevalence of sealants compared with students in schools without sealant programs. One of the national health objectives for 2010 is to increase to 50% the proportion of children aged 8 years that have received dental sealants on their first permanent molar teeth (3). Periodic surveys in Ohio have documented steady increases in the overall prevalence of dental sealants among children aged 8 years, from 11% during 1987--1988 to 26% during 1992--1993 to 30% during 1998--1999 (5). Although the overall prevalence still falls short of the 2010 objective, among targeted schools, all racial and income groups have achieved or exceeded the objective. Providing programs in all eligible, high-risk schools would accelerate progress toward both achieving the 2010 objective and eliminating racial and income disparities. School-based sealant programs began in Ohio during the mid-1980s, expanding from a single demonstration program in one city in 1984 to 18 programs in 34 of 88 counties in 2000. During 1997--1998, approximately 12,000 second grade students received sealants through Ohio school-based programs. The findings in this report are subject to at least two limitations. First, it is not known to what extent the 42% of third grade students who did not return parental consent forms were similar to the students who did. In addition, it is unknown whether those without consent were equally distributed according to other factors that could influence the findings (e.g., receipt of regular dental care). Second, parental recall about whether children received sealants at school was subject to error. As a result, for this analysis, only children who attended a school with a sealant program, had a sealant on at least one tooth, and had a consent form indicating that they had received sealants at school were counted in that category. The findings of this survey indicate that, among students who participated, the use of appropriately targeted school-based programs increases the prevalence of dental sealants among children from low-income families and reduces the racial and income disparity in sealant prevalence among elementary school students. The extent to which sealant programs can eliminate the disparity in sealant prevalence in a population will be influenced by the manner in which the programs are targeted and by their penetration in the targeted population. Sealant programs provide additional benefits when they are linked to programs that ensure access to primary dental care for those in need of restorative services. References
Table 1 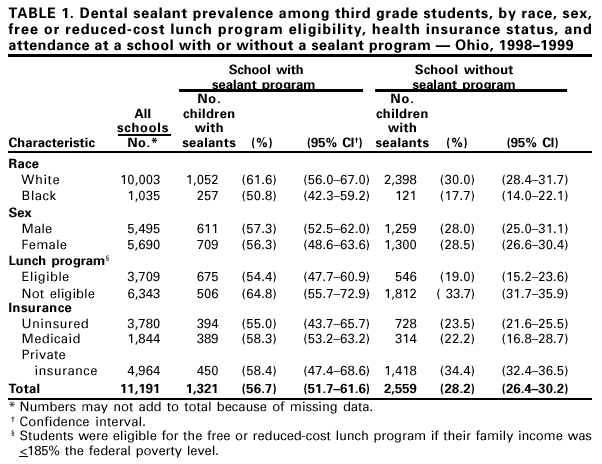 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 8/31/2001 |
|||||||||
This page last reviewed 8/31/2001
|