 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Measles Eradication: Recommendations from a Meeting Cosponsored by the World Health Organization, the Pan American Health Organization, and CDCSummary Recent successes in interrupting indigenous transmission of measles virus in the Americas and in the United Kingdom prompted the World Health Organization (WHO), Pan American Health Organization (PAHO), and CDC to convene a meeting in July, 1996 to consider the feasibility of global measles eradication. Presentations at the meeting included an overview of global measles control and elimination efforts; detailed reviews of successful measles elimination efforts in Latin America, the English-speaking Caribbean, Canada, and the United States; surveillance for clinical disease; laboratory tools for antibody detection and virus identification; and other factors that might influence the feasibility of disease eradication. With this background information, meeting organizers asked participants to address five questions:
Participants agreed that measles eradication is technically feasible with available vaccines and recommended adoption of the goal of global eradication with a target date during 2005-2010, with the proviso that measles eradication efforts should not interfere with poliomyelitis eradication but should build on the successes of the global Poliomyelitis Eradication Initiative. Although existing vaccines are adequate for eradication, vaccination strategies that rely on administration of a single dose of vaccine are not. In the Americas, sustained interruption of indigenous measles virus transmission has been achieved through a three-tiered vaccination strategy that includes a) "catch-up" vaccination of all persons aged 1-14 years, regardless of disease history or vaccination status; b) "keep-up" vaccination of greater than or equal to 90% of children in each successive birth cohort at age 12 months; and c) "follow-up" campaigns designed to vaccinate all persons within a specific age range whenever the number of susceptible persons in the preschool-aged population approximates the size of a typical birth cohort (in practice, every 3-5 years). In other regions, different strategies may be optimal. Surveillance, a critical component of any strategy to eliminate or eradicate measles, has two functions: to assess the effectiveness of the measles elimination strategy and to detect circulation of measles virus in a population. Systematic surveillance based on clinical diagnosis should be implemented early in any measles elimination program. In countries attempting to eliminate indigenous measles, all isolated cases of measles and at least one case in each chain of transmission should be confirmed by laboratory tests. Specimens for virus isolation (e.g., urine, nasopharyngeal swabs, or blood) should be collected in conjunction with field investigations. Vaccination campaigns generally have not proved to be effective responses to measles outbreaks. Outbreaks should be treated as opportunities to reinforce surveillance and to identify measures to prevent future outbreaks. The major obstacles to measles eradication are not technical but perceptual, political, and financial. Measles is often mistakenly perceived as a mild illness. This misperception, which is particularly prevalent in industrialized countries, can inhibit the development of public and political support for the allocation of resources required for an effective elimination effort. The disease burden imposed by measles should be documented, particularly in industrialized countries, so that this information can be used to educate parents, medical prac-titioners, public health workers, and political leaders about the benefits of measles eradication. INTRODUCTION During the early 1980s, in the aftermath of smallpox eradication, some scientists and public health officials urged consideration of a global effort to eradicate measles (1). During the mid-1980s, however, the high level of population immunity required to interrupt measles virus transmission became clear, and the prospect of measles eradication seemed to recede (2). As recently as 1993, a task force on disease eradication declared measles "not now eradicable"(3). The major obstacles to eradication cited by the task force were the contagiousness of measles, the lack of a vaccine that is effective among children aged less than 9 months (most of whom have maternal antibody to measles that protects them from disease but which also inhibits the immune response to the vaccine virus), and the incorrect perception that measles is a mild illness. Recent successes in implementing new approaches to control and eliminate measles virus transmission prompted the World Health Organization (WHO), the Pan American Health Organization (PAHO), and CDC to convene a meeting July 9-10, 1996, in Atlanta to reconsider the feasibility of global measles eradication. Among the participants were representatives of the sponsoring organizations, representatives of regions and countries that have implemented measles elimination activities, and persons affiliated with WHO Regional Offices, local and state health departments in the United States, and universities. During the meeting, presenters reviewed vaccination strategies and achievements in measles control in the Caribbean and Latin America, Canada, and the United States. In addition, representatives of Denmark, Kuwait, Mexico, South Africa, and the United Kingdom described their recent efforts to control or eliminate measles transmission. In each of these countries, intensification of efforts to control measles has been followed by sustained declines in the number of reported cases. Other presentations addressed surveillance for clinical disease and laboratory tools for virus identification and antibody detection. Information was presented concerning other factors that could potentially affect the feasibility of measles eradication (i.e., the possible existence of nonhuman reservoirs for the virus, the possibility of transmission of measles from persons with asymptomatic measles infection, and the possibility that vaccination-induced immunity to measles might wane with the passage of time). Based on this information and on subsequent discussion, meeting participants were asked to address five questions:
Discussion of these questions formed the basis for the conclusions and recommendations of the meeting. The rapporteur prepared a draft of the conclusions and recommendations that was distributed and discussed in the final session of the 2-day meeting. The discussion and subsequent modification of the draft ensured that the report would reflect both points of consensus and the sense of discussions among participants. Definitions of Measles Elimination and Eradication To facilitate communication among participants, working definitions of two important terms were developed during the meeting. Measles elimination refers to interruption of transmission in a sizable geographic area in which vaccination would nevertheless need to continue because of the continued threat of reintroduction of the virus. Eradication, defined as the global interruption of measles transmission, represents the sum of successful elimination efforts in all countries. Once eradication is achieved, vaccination could be stopped without risk for measles outbreaks. BACKGROUND This section a) describes the status of global measles control; b) summarizes efforts to eliminate measles in Latin America, the English-speaking Caribbean, and Canada; and c) describes progress toward measles elimination in the United States. The summaries are based upon material presented at the meeting and have been updated by the presenters. Status of Global Measles Control Since the inception of the World Health Organization's Expanded Programme on Immunization (EPI) in 1974, the numbers of cases and deaths attributed worldwide to measles have declined substantially, from an estimated 100 million cases and 5.8 million deaths in 1980 to an estimated 44 million cases and 1.1 million deaths in 1995. In 1974, only 5% of the world's children aged 12-23 months had been vaccinated against measles. By the mid-1980s, measles vaccination coverage among children aged 12-23 months in developing countries had reached only 42%, largely because of the lack of infrastructure for delivering vaccines and the perception that measles was not a serious public health problem (4). From 1985 through 1990, however, the number of measles cases reported worldwide declined by 56% as governments, international agencies and other organizations provided the human and financial resources needed to reach the global goal of 80% infant immunization coverage by the year 1990 (WHO, unpublished data). Despite these achievements, measles remains one of the leading causes of child mortality in developing countries, responsible for approximately 10% of all deaths among children aged less than 5 years (5). These deaths typically occur among young children in countries with low vaccination coverage levels. Even countries that have achieved high levels of measles vaccination coverage and have recorded several years of low incidence frequently have experienced large measles outbreaks (6-9). On the basis of vaccination coverage, case fatality rates, and vaccine effectiveness, WHO estimates that by 1995 measles-associated morbidity and mortality had decreased by 78% and 88%, respectively, in comparison with the pre-vaccine era (WHO, unpublished data). Although these estimates demonstrate a marked reduction in the health burden of measles, they also indicate that the mid-decade goals of reducing measles morbidity by 90% and measles mortality by 95% have not been met. Measles outbreaks have continued to occur because, even in countries with high vaccination coverage, the proportion of children susceptible to the disease increases over time and eventually reaches a level that sustains measles transmission. Ongoing measles outbreaks have been particularly problematic in developing countries. Low vaccination coverage has been primarily responsible for these outbreaks. However, the practice of vaccinating children aged less than 12 months has also contributed because the vaccine is less effective among children of this age. (Vaccinating of children aged less than 12 months has also substantially reduced measles incidence in this age group, in which mortality from the disease is highest.) Compared with vaccinating children aged greater than or equal to 12 months, vaccinating those younger than 12 months hastens the accumulation of susceptible persons in the preschool-aged population. In some developing countries, two-dose measles vaccination schedules were introduced to slow the increase of susceptible children by vaccinating those who had missed the first dose and providing protection to those who did not develop an immune response after a single dose of measles vaccine. This strategy has interrupted measles transmission in some industrialized countries that have achieved vaccination coverage levels exceeding 95% for both doses of vaccine. Attainment of such high coverage levels required active follow-up of children who missed a scheduled dose (10). In developing countries, outbreaks have continued to occur after two-dose schedules were implemented, because the second dose (scheduled at ages ranging from 18 months to primary- or secondary school entry) seldom reached previously unvaccinated children, and coverage attained with the second dose is always lower than with the first dose (11). Since 1994, a strategy of limited vaccination campaigns targeting all children aged 9 months to 5 years has been advocated to reduce measles morbidity and mortality by reaching unvaccinated children in areas in which risk for measles is high (e.g., large, densely populated urban and peri-urban centers)(12). This strategy is intended to improve vaccination coverage and not necessarily to interrupt measles virus transmission. Several countries in WHO's Southeast Asian Region (i.e., Bangladesh, India, Myanmar, and Nepal), and its Western Pacific Region (i.e., the Philippines) have used the strategy with only modest success. Many children who were unvaccinated before the campaigns remained unvaccinated afterward. In addition, poor case surveillance hindered efforts to evaluate the impact of the campaigns in reducing the disease burden. The experience in the Philippines provides an example of these difficulties. Immediately after a measles vaccination campaign that targeted urban areas in that country, a measles epidemic occurred. The epidemic prompted a vaccination coverage survey, which indicated that the campaign had succeeded in vaccinating only 44% of previously unvaccinated children (Philippine Ministry of Health, unpublished data). Although vaccination campaigns limited to high-risk areas can help reduce morbidity and mortality caused by measles, they do not result in the sustained interruption of measles virus transmission. Such campaigns must include provisions for vaccinating previously unvaccinated children and improving surveillance so that the impact of the campaign can be measured. The impact of measles vaccination has varied substantially among the six WHO Regions (Figure_1). These interregional differences reflect disparities in routine immunization coverage levels and, more importantly, in the effectiveness of different measles control strategies. Of the six WHO Regions, the most substantial progress in measles control has been achieved in the Americas, where most countries have implemented a strategy based on a one-time-only mass vaccination campaign across a wide age group. The goals of this strategy are to achieve a rapid reduction in the number of susceptible children in the population and to interrupt the transmission of measles virus. To keep the susceptible population from exceeding the epidemic threshold requires high routine coverage and periodic "follow-up" campaigns to vaccinate children born after the previous campaigns. A strategy similar to that used in the Americas has been implemented or is being considered in at least one country in each of the other WHO regions. For example, mass campaigns that included children aged less than or equal to 16 years have been conducted in the United Kingdom in the European Region, Bhutan and Mongolia in the Western Pacific Region, Kuwait and Oman in the Eastern Mediterranean Region, and South Africa in the African Region. Measles Elimination in Latin America, the English-Speaking Caribbean, and Canada After the eradication of wild poliovirus from the Americas was certified in 1994, the ministers of health of the countries of the region established the goal of eliminating measles virus circulation in the Western Hemisphere by the year 2000 (13). To achieve this goal, PAHO has developed a measles elimination strategy (14) that shares certain features with the successful poliomyelitis eradication strategy being implemented throughout the world (15). In addition to careful measles surveillance, the PAHO measles elimination strategy has three main components. First, a one-time-only "catch-up" measles vaccination campaign is conducted, targeting all children aged 9 months through 14 years without regard to previous history of measles disease or vaccination. The goal is to interrupt measles virus circulation rapidly by achieving high levels of measles immunity across a wide age cohort. Early in the implementation of the PAHO measles eradication strategy, some "catch-up" vaccination campaigns targeted only children who lacked documentation of measles vaccination. For several reasons, these campaigns were less successful than later "nonselective" campaigns that targeted all children without regard to disease history or vaccination status. Problems identified in the early "selective" campaigns included difficulties in determining the vaccination status of children and failure to vaccinate the small proportion of children who remained susceptible to the disease after receiving a previous dose of measles vaccine. After a "catch-up" campaign, efforts are directed at strengthening routine vaccination services for infants to slow the accumulation of susceptible preschool-aged children and to maintain the interruption of measles virus circulation. This component of the strategy is referred to as "keep-up" vaccination. Because interruption of measles virus transmission reduces an infant's risk for exposure to measles, the recommended age of routine measles vaccination can be safely increased from 9 months to 12 months. The concomitant increase in measles vaccine efficacy reduces the percentage of vaccinated children who remain susceptible to the disease (16). Efforts are made to achieve at least 90% coverage in each successive birth cohort in every district of every country. Because measles vaccine is less than 100% effective and universal vaccination coverage is rarely achieved, the number of susceptible infants and children inevitably increases over time, thus increasing the risk for a measles outbreak if the virus is reintroduced. To reduce the number of susceptible preschool-aged children, periodic "follow-up" vaccination campaigns are conducted that target all children aged 1-4 years, regardless of vaccination status or disease history. These campaigns are designed to protect susceptible children from measles, whether they are susceptible because they were not vaccinated or because they did not develop a protective immune response to previous vaccination. The vaccination coverage obtained through routine vaccination services dictates the interval between "follow-up" campaigns, which are conducted when the estimated number of susceptible preschool-aged children approaches the number of infants in an average birth cohort (in practice, every 3-5 years). The first "catch-up" campaign in the Americas was conducted during 1987 in Cuba; 98% coverage with measles-mumps-rubella (MMR) vaccine was achieved in the population aged 9 months to 14 years. In 1991, all countries of the English-speaking Caribbean conducted a "catch-up" campaign with either single-antigen measles vaccine or MMR vaccine. Vaccination coverage exceeded 90%. By the end of 1995, all countries of Latin America also had conducted "catch-up" campaigns. The estimated measles vaccination coverage for children aged 1-14 years in the countries of Latin America and the English-speaking Caribbean exceeded 93%. Since 1994, "follow-up" campaigns have been conducted in Belize, Brazil, Chile, Colombia, Costa Rica, Cuba, El Salvador, Guatemala, Jamaica, Nicaragua, Panama, and Peru (17). The remaining countries in Latin America and the Caribbean are planning to conduct similar campaigns by the end of 1998. To monitor progress toward measles elimination in the Americas, efforts have been made to strengthen measles surveillance in every country. The goal of the PAHO measles surveillance system is rapid detection of measles virus circulation. In Latin America and the Caribbean, greater than 20,000 health units report weekly on the presence or absence of suspected measles cases in their jurisdictions. At least one reporting unit operates in every district or municipio (municipality) in every country of Latin America and the Caribbean. For surveillance purposes, any patient in whom a clinician suspects measles virus infection is considered to have a suspected case of measles. Health-care workers are requested to report all suspected cases immediately to local health authorities. To determine whether suspected measles cases are actually caused by measles infection, field epidemiologists attempt to investigate every reported suspected case in a timely manner. Collecting a serum sample for laboratory analysis is an essential part of such investigations. Because other pathogens and conditions can produce clinical findings that resemble measles, only laboratory investigation can provide the information needed to confirm or discard suspected measles cases. Health-care workers are asked to collect a single serum specimen from every patient suspected to have measles at the time this presumptive diagnosis is made. In state or national laboratories, serum specimens are tested with an enzyme immunoassay (EIA) for the presence of measles IgM antibodies (14). Specimens are screened initially with a commercial indirect IgM measles assay that is sensitive but nonspecific. All specimens that are positive or indeterminate by the indirect assay, as well as a 10% random sample of negative sera, are sent to one of 11 regional reference laboratories in the PAHO measles laboratory network for confirmatory testing with the more specific IgM-capture EIA developed by CDC (18). A suspected measles case is classified as laboratory-confirmed if both the indirect and capture EIAs indicate the presence of measles IgM antibodies in a properly collected serum specimen or if there is an epidemiologic link to another laboratory-confirmed measles case. An epidemiologic link is defined as exposure to a person with a previous or subsequent laboratory-confirmed case of measles. A suspected measles case can be discarded only if a properly collected serum sample tests negative for the presence of measles IgM antibodies. The case is classified as clinically confirmed if a) no serum specimen is collected from a patient who has a suspected case, and b) the case investigation does not reveal an epidemiologic link to a laboratory-confirmed measles case. Such clinically confirmed cases are considered to represent failures of the measles surveillance system, because the epidemiologic investigation was not properly conducted. In addition, PAHO has developed surveillance indicators to measure the effectiveness and quality of national measles surveillance systems. These indicators include the proportions of:
As experience accumulates, these indicators may be modified if the process of assessing surveillance can be simplified without discarding information needed to improve national measles surveillance systems. After the 1977 initiation of the EPI in the Americas, measles vaccination coverage increased steadily, measles incidence declined, and the intervals between measles epidemics lengthened. However, a regionwide measles epidemic occurred in 1990, when 218,000 measles cases were reported in Latin America and the Caribbean. During this measles epidemic, the number of cases reported approached the number reported in 1977. The "catch-up" measles vaccination campaigns, conducted in Cuba in 1987 and in other Caribbean and Latin American countries during 1991-1994, immediately reduced the number of reported measles cases (Figure_2). During 1995, 13,340 suspected measles cases were reported from Latin American and Caribbean countries (Table_1). Of these, 9,517 (71.3%) were discarded because IgM serology results were negative, 441 cases (3.3%) were confirmed by positive measles IgM laboratory results, and 3,382 cases (25.3%) were classified as clinically confirmed because of an incomplete epidemiologic investigation. The total of 3,823 confirmed measles cases reported during 1995 from Latin America and Caribbean countries constitutes the lowest annual total ever reported for the region and represents a reduction of greater than 98% compared with the number reported in 1990. Measles is now rare in Latin America and the Caribbean. Surveillance evaluations conducted during 1995 and 1996 in El Salvador, Mexico, and Nicaragua found no evidence of measles virus circulation. During 1996, a provisional total of 864 confirmed measles cases was reported for Latin America and the Caribbean. Of the total, 70 (8.1%) were confirmed by positive serologic tests for measles IgM antibody. The remaining cases were classified as clinically confirmed because laboratory investigations were not conducted. The last laboratory-confirmed case of measles detected in the English-speaking Caribbean was reported in 1991, just before the mass vaccination campaign was conducted. Similarly, the last laboratory-confirmed cases of measles in Cuba and Chile were detected in 1993. In other Latin American and Caribbean countries, measles transmission is occurring at extremely low levels, if at all. Most laboratory-confirmed cases have been sporadic and isolated in time and place. Importations of measles cases from Latin America detected by the United States measles surveillance system provide an indirect measure of the impact of the PAHO measles elimination strategy (Figure_3). In 1990, greater than 200 cases, or greater than 80% of all cases of measles imported to the United States, came from Latin America (principally Mexico). Since then, the number and proportion of measles cases imported from Latin America have declined markedly. The last laboratory-confirmed case of measles imported from Latin America or the Caribbean to the United States was reported in 1994. Canada accounts for only 4% of the population of the Americas. In 1995, however, Canada reported 2,362 measles cases, or nearly 40% of all measles cases reported in the Western Hemisphere during that year. The routine measles vaccination schedule introduced in the mid-1960s (i.e., a single dose of measles-containing vaccine administered to children at age 12 months) had resulted in a 95% reduction in measles incidence, but did not interrupt measles virus transmission. Although Canada consistently reached coverage levels of greater than or equal to 97% with a single dose of measles-containing vaccine among children aged 2 years, measles outbreaks continued to occur, mostly among school-aged children. Outbreaks occurred even in populations with documented vaccination rates approaching 100%. Control measures such as exclusion from school and emergency mass revaccination proved disruptive, costly, and of limited effectiveness. Although in 1992 a National Conference on Measles Control had endorsed the goal of eliminating indigenous measles from Canada by 2005, little progress had been made by 1995. Competing developments in childhood vaccination programs preempted the formal introduction of a two-dose measles vaccination program in Canada. The numbers of cases in Canada in 1995 contrasted with numbers reported from other countries in the Americas and prompted the adoption of a national goal of measles elimination -- with the needed political support -- in late 1995. Several analyses clarified the benefits of efforts to achieve the elimination of measles in Canada. Mathematical modeling and a Delphi survey predicted that there were enough susceptible persons in the Canadian population to produce an annual average of 12,800 measles cases. An outbreak involving greater than or equal to 20,000 measles cases, 2,000 cases with complications, and several measles-related deaths was predicted to occur as early as April 1996 unless additional strategies to eliminate measles were implemented. Mathematical modeling also predicted that phasing in a two-dose vaccination schedule by administering a second dose only to young children would not eliminate measles for 10-15 years and that a national "catch-up" campaign was the only way to avoid the predicted epidemic and prevent an estimated 58,530 cases during the next several years. A cost-benefit analysis indicated that a measles vaccination campaign would save more than 2.5 dollars for every dollar expended (Laboratory Centre for Disease Control, Ottawa, unpublished data). In late 1995, the National Advisory Committee on Immunization recommended a mass measles vaccination campaign. By July 1996, six provinces (comprising 80% of Canada's population) had completed "catch-up" vaccination campaigns for all school-aged children: in some provinces this included children aged greater than or equal to 18 months, as well. Two additional provinces began implementation of a "catch-up" program in the fall of 1996. More than 4 million children received supplementary vaccinations and provincial coverage for the target populations averaged approximately 90%. Furthermore, all of Canada's provinces or territories have introduced a second MMR vaccination for children aged 18 months or 4-6 years, depending on the province. These successful vaccination campaigns produced immediate results: three measles outbreaks that had begun in early 1996 were quickly terminated as the campaigns began. Only 324 cases of measles were reported in Canada for 1996; most of these cases occurred before May, usually the month when incidence is highest. Transmission of measles virus appears to have been interrupted during fall, 1996. The same strategies should be implemented in the remaining provinces to ensure the sustained interruption of measles virus transmission because of the continuing problem of measles importations from countries where measles transmission continues. Measles Elimination in the United States The United States is in the midst of a third attempt to eliminate indigenous transmission of measles. Earlier efforts, initiated in 1966 and 1978, suppressed measles incidence to levels below any previously recorded; 1,497 cases were reported in 1983, the fewest in any year before the 1990s. Implementation of state requirements for vaccination with measles-containing vaccine as a condition for school entry was one of the major factors in increasing vaccination coverage and reducing the incidence of measles (19). Low levels of measles transmission persisted through the mid-1980s. An average of 2,900 cases was reported each year during 1983-1988. However, during 1989-1991, the United States experienced a resurgence of measles, during which 55,622 cases were reported. The largest increase in incidence occurred among preschool-aged children. Most cases occurred among children who had not been vaccinated. This increase in measles cases prompted a major effort to ensure vaccination against measles at the recommended age. In 1994, the Childhood Immunization Initiative established specific goals for vaccination coverage and disease reduction (20). For measles, the goal for first-dose coverage was 90% by 1996 and the elimination of indigenous measles by 1996. These goals have largely been achieved. Before the measles resurgence during 1989-1991, measles vaccination coverage levels among children aged 2 years had never reached 70% (21). Since 1991, coverage levels with measles-containing vaccine have increased to 91% (22). These improvements in coverage have been achieved through locally initiated efforts (e.g., linking immunization services with the Special Supplemental Nutrition Program for Woman, Infants, and Children (WIC) and a program that coupled assessment of coverage levels among providers with feedback) (23-24). In 1989, the Advisory Committee on Immunization Practices and the American Academy of Pediatrics recommended that children in the United States receive two doses of measles-containing vaccine. This recommendation was made to prevent outbreaks in schools; several well-documented outbreaks demonstrated that measles transmission could occur even with coverage levels greater than 95% for a single dose of measles vaccine (25-27). States have gradually implemented requirements that mandate a second dose of measles-containing vaccine as a condition for entering school. For the 1996-97 school year, 35% of school-age children in the United States were covered by such requirements (CDC, unpublished data). Records of doses of MMR vaccine purchased and administered suggest that as many as 65% of school-age children have received a second dose of measles-containing vaccine (CDC, unpublished data). As a result of these efforts, a sustained decline in measles incidence occurred in the United States beginning in 1993, when 312 confirmed measles cases were reported. The reported number of cases increased to 963 in 1994; outbreaks among members of groups that oppose vaccination were largely responsible for the increase. In 1995, a total of 309 cases was reported, the fewest since national surveillance began. In addition to the decline in reported cases, epidemiologic evidence suggests that indigenous measles transmission has been interrupted. From September 12 through December 31, 1993, 25 confirmed cases of measles were reported. Of these, seven cases were classified as imported and 14 as importation-associated cases (i.e., cases linked to a chain of transmission originating with an imported case). The four cases classified as indigenous were not clustered geographically or temporally. They occurred in widely separated geographic locations -- California, Florida, upstate New York, and Rhode Island. These cases were also widely separated in time -- periods of 4 weeks and 6 weeks occurred during which no indigenous cases were identified. These data suggest that the four indigenous cases (if they were, in fact, measles and not some other illness misclassified because of false-positive laboratory test results) more likely resulted from exposure to undetected imported cases than from ongoing indigenous transmission of measles virus. Molecular epidemiologic studies of wild-type measles virus also indicate that indigenous measles transmission was interrupted during 1993. Measles viruses isolated from throughout the United States during 1988-1993 were similar, suggesting a single predominant lineage (28). Since 1993, that lineage has not been detected in the United States, except in one case imported from the Philippines. Numerous wild-type measles viruses isolated since 1993 have been similar to strains circulating outside the United States. Strains similar to those found in Western Europe and East Asia were particularly common in 1996 (Figure_4). During October and November 1995, a 6-week period occurred during which all cases of measles reported in the United States were either imported or linked to an imported case. A similar 4-week period was observed during February 1996. During late 1996 and early 1997, a 16-week period occurred when a single indigenous case was identified. These data suggest that indigenous measles transmission in the United States has been interrupted numerous times and that, in each instance, transmission of the disease has been re-established by an importation of measles virus. Since 1992, imported cases have made up an increasing proportion of all measles cases reported in the United States. The number of imported cases detected has declined from an average of 120 per year during 1985-1992 to 53 per year since 1993. This reduction is almost entirely the result of decreases in imported cases from Latin America (Figure_3). Since 1994, only one case that could possibly have been imported from a Latin American country has been reported, and subsequent investigation revealed no evidence of measles transmission in that country. Since 1992, most measles cases imported to the United States have originated in Western Europe and East Asia, reflecting relatively poor control of measles in these regions and frequent travel to the United States. CONCLUSIONS AND RECOMMENDATIONS The five questions posed to meeting participants (see Introduction) were designed to structure discussion of the feasiblity of and strategies for measles eradication. The conclusions and recommendations developed by participants in response to these questions follow. Feasibility of Measles Eradication Conclusions: Based on the success of efforts to control measles in the Western Hemisphere and the United Kingdom, global measles eradication is technically feasible with available vaccines. National, subregional, and regional elimination of measles can and should be accomplished. Although nonhuman primates can be infected with measles virus, such nonhuman reservoirs are unlikely to sustain measles transmission. Although asymptomatic and nonclassical cases of measles can occur among vaccinated persons, these atypical cases would not impede elimination or eradication of the virus. Waning immunity does not appear to play a major role in vaccine failure. Recommendations: A goal of global measles eradication should be established, with a target date during 2005-2010. Factors that favor a global initiative to eradicate measles within this time frame include:
Although measles eradication is a logical addition to and extension of the poliomyelitis eradication initiative, the effort should build on the success of poliomyelitis eradication. Consequently, measles eradication should not be undertaken immediately and simultaneously in all parts of the world. Rather, measles eradication efforts should await maturation of the poliomyelitis eradication program in each region of the globe, and should be implemented as countries and regions become free of poliomyelitis. Because of the rapid accumulation of persons susceptible to measles, the implementation phase of an eradication effort should be compressed into as brief a time as possible. Research into the molecular pathogenesis of measles and the immune response to measles virus infection should continue. Vaccination Strategies Conclusions: Existing vaccines are sufficient to eradicate measles, but eradication requires more than a routine one-dose vaccination strategy. However, no single two-dose approach is optimal for all countries. Success has been attained in many countries, particularly in the Americas, with a strategy comprising a) "catch-up" mass campaigns during which all persons aged 1-14 years are vaccinated, regardless of prior vaccination status; b) high routine ("keep up") vaccination coverage following the "catch-up" campaign; and c) periodic "follow-up" campaigns during which all children aged 1-4 years are vaccinated. In some countries with highly developed vaccination programs capable of reaching greater than 95% coverage, an ongoing two-dose "plus" strategy appears capable of eventually eliminating measles. (The "plus" refers to special supplementary efforts to reach populations at high risk.) Regardless of the strategy selected, monitoring the accumulation of susceptible persons within the population is essential. Accumulation of susceptible persons occurs because a single dose of vaccine does not elicit a protective immune response in some children and because some children are not vaccinated. Such monitoring permits appropriate action, in the form of "follow-up" campaigns or special vaccination activities in areas at highest risk. Recommendations: Countries that adopt a strategy of measles elimination should implement some form of "catch-up" vaccination rather than simply adding a second dose to the routine vaccination schedule. All children must receive measles vaccine, and the "second dose" should also reach those who missed the first dose; such children should be vaccinated and should subsequently receive another dose. Exploration of alternative methods of vaccine delivery, particularly jet injectors, and of alternative preparations of the vaccine should continue. Surveillance Strategies Conclusions: Measles case surveillance is a critical component of any strategy to control measles, including strategies to eliminate or eradicate measles. The most important functions of surveillance are to assess the effectiveness of the strategy and to detect circulation of measles virus in a population, rather than to identify every case of measles infection (except during the final stages of eradication). Although a passive system of surveillance for measles may be adequate in countries or regions where health-care providers detect and report measles cases, active surveillance is required in many circumstances (e.g., areas where notification of suspected cases is low, where a confirmed case has been identified, where clusters of suspected cases have been reported, or where a dense population of unvaccinated children exists). As more countries interrupt measles transmission, importation of measles virus will become more prominent. Because determining the source of an imported case can be difficult, the following classification scheme for confirmed measles cases may be useful: indigenous; source unknown; imported (source known); and imported (source unknown). Surveillance indicators are a useful means of evaluating the performance of surveillance systems but must be limited in number to be optimally effective. No external standard for determining the completeness of measles surveillance exists that is equivalent to the rate of acute flaccid paralysis for poliomyelitis. Recommendations: Surveillance for individual measles cases should be implemented at an early stage of the elimination program. Measles notification should be based on clinical suspicion rather than rigid case definitions. Case definitions are important, however, during investigation and classification of suspected cases. To establish the source of imported measles cases, collaboration among countries can be facilitated by WHO offices. Experience in using measles surveillance indicators is limited, and proposed indicators may be modified based on accumulating experience. Laboratory Strategies Conclusions: Laboratory confirmation of suspected measles cases will become increasingly important as measles incidence declines and countries progress toward elimination. Establishment of a functioning global network of reference diagnostic laboratories will be a critical element in achieving global eradication. Development of a rapid field diagnostic test would facilitate surveillance and case investigations. In addition to confirmation of cases, the laboratory has a vital role in characterizing measles virus isolates to determine whether cases represent sustained indigenous transmission or importations. The laboratory can also serve an important function in surveillance for measles immunity because serologic measures may be useful in confirming the level of protection estimated by vaccination coverage of a population. Recommendations: In countries attempting to eliminate measles, all isolated cases of measles and at least one case from each chain of transmission should be confirmed by laboratory tests. In addition to serum or saliva specimens for laboratory confirmation, specimens for virus isolation should be collected within 7 days of rash onset in conjunction with case investigations. Specimens that can be cultured for virus isolation include urine, nasopharyngeal swabs, and blood. Reference laboratories with expertise in culturing measles virus should perform virus isolation. Development of a rapid field diagnostic test is the most urgent research need. Response to Measles Outbreaks Conclusions: Preventing measles outbreaks is more effective than trying to contain them. Mass vaccination campaigns undertaken in response to outbreaks are of limited usefulness in most countries because such efforts are costly, disruptive, and often ineffective by the time they are instituted. Careful investigation of all outbreaks, however, can generate data needed to obtain the political support required for an effective elimination effort. In addition, outbreak investigations can help determine why transmission of measles occurred; such investigations will be critical to refining measles elimination strategies as they are implemented. Recommendations: Measles outbreaks should be treated as opportunities to reinforce surveillance, assess the health burden of continuing measles transmission, and identify appropriate measures to prevent future outbreaks. Obstacles to Eradication Conclusions: The major obstacles to measles eradication are perceptual, political, and financial. The full health impact of measles is often underestimated. Measles is frequently perceived as a minor illness of little consequence, particularly in industrialized countries. This perception may make it difficult to develop the political support necessary to carry out a successful global eradication effort. Strong support for measles eradication can be expected in many developing countries, where measles is recognized as a major killer. Measles eradication will quickly pay for itself because of savings in vaccinations, hospitalizations, and deaths prevented. Recommendations: Parents, medical practitioners, and public health professionals -- particularly those in industrialized countries -- must be educated about the global disease burden imposed by measles. The disease burden of measles should be better documented in more countries, especially in the developed world, to gain support for global eradication. DISCUSSION This 2-day consultative meeting represents a landmark in the history of measles control. The data presented demonstrated the feasibility of interrupting measles transmission for prolonged periods over wide geographic areas. Recently developed molecular tools allow researchers to distinguish indigenous from imported virus strains. Data developed with these tools support the claim that transmission of indigenous strains of measles virus has been interrupted for substantial periods in the Americas and in the United Kingdom. In addition, global experience has now demonstrated that an important distinction must be made between the limited measles vaccination campaigns that have targeted urban or poorly served areas in many countries and the strategy that has interrupted measles transmission in the Americas and the United Kingdom. Limited campaigns targeted to underserved or high-risk populations may improve vaccination coverage, but they are not sufficient to interrupt transmission of the virus. Countries should undertake such geographically limited campaigns only as part of a larger measles control or elimination strategy. Presentations from representatives of individual countries and WHO regions documented the political and public interest in the eradication of measles, particularly among developing countries. However, global consensus and commitment are essential because measles eradication will require supplementary vaccination activities in industrialized countries as well as in developing countries. In countries and regions where endemic poliovirus transmission continues, poliomyelitis eradication efforts must be further strengthened to ensure that the introduction of measles elimination activities builds on the successes of the global poliomyelitis eradication initiative. A global plan of action for the eradication of measles is needed to facilitate coordination among countries, donors, technical agencies, and international organizations and to ensure that eradication activities are conducted efficiently. References:
Figure_1 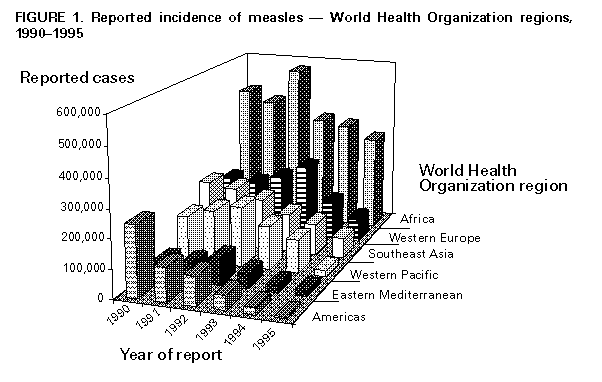 Return to top. Figure_2 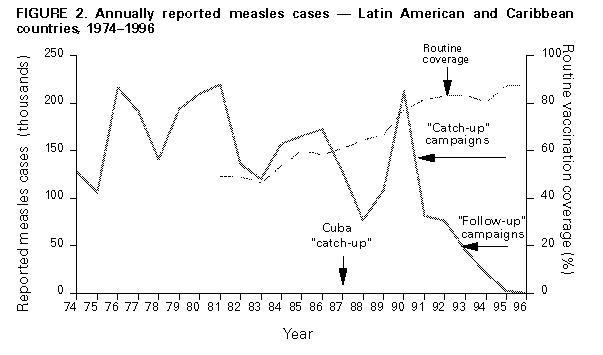 Return to top. Table_1 Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size.
TABLE 1. Final classification of reported suspected measles cases -- Latin American
and Caribbean countries, 1995
======================================================================================================================
Cases reported -- 1995
-------------------------------------------------------------------------
Total Confirmed cases Total
suspected Discarded --------------------------------------- confirmed
Country cases notified cases Clinically * Laboratory + Total cases, 1994
--------------------------------------------------------------------------------------------------------------------
South America
--------------------------------------------------------------------------------------------------------------------
Argentina 1,808 1,153 651 4 655 134
Bolivia 92 16 76 0 76 1,441
Brazil 3,533 2,740 780 13 793 35
Chile 300 300 0 0 0 0
Colombia 2,530 2,120 204 206 410 525
Ecuador 919 -- 919 -- 919 3,668
Peru 636 283 224 129 353 670
Paraguay 142 69 69 4 73 122
Uruguay 5 0 5 0 5 0
Venezuela 651 479 139 33 172 15,364
Mexico &
Central America
--------------------------------------------------------------------------------------------------------------------
Mexico 1,395 1,151 232 12 244 12
Belize 10 6 4 0 4 0
Costa Rica 251 216 32 3 35 0
El Salvador 260 260 0 0 0 0
Guatemala 56 33 0 23 23 204
Honduras 26 26 0 0 0 3
Nicaragua 195 190 5 0 5 3
Panama 92 73 16 3 19 3
Caribbean
--------------------------------------------------------------------------------------------------------------------
Anguilla 2 2 0 0 0 0
Antigua 1 1 0 0 0 0
Bahamas 11 11 0 0 0 0
Barbados 27 27 0 0 0 0
Cayman Isl. 0 0 0 0 0 0
Cuba 74 73 1 0 1 0
Dominica 37 37 0 0 0 0
Cuba 74 73 1 0 1 0
Dominican
Republic 32 32 0 0 0 3
Grenada 5 2 3 0 3 0
Fr. Guiana -- -- -- -- -- --
Guadeloupe 0 0 0 0 0 0
Guyana 16 16 0 0 0 0
Haiti -- -- -- -- -- --
Jamaica 133 118 15 0 15 0
Martinique -- -- -- -- -- 1
Montserrat 1 1 0 0 0 0
Netherlands
Antilles -- -- -- -- -- --
Puerto Rico 11 0 -- 11 11 13
St. Kitts & Nevis 2 1 1 0 1 0
St. Lucia 8 6 2 0 2 0
St. Vincent 0 0 0 0 0 0
Surinam 12 12 0 0 0 0
Trinidad & Tobago 57 57 0 0 0 0
Turks & Caicos 9 5 4 0 4 0
Br. Virgin Islands 1 1 0 0 0 0
U.S. Virgin Islands 0 0 0 0 0 0
TOTAL 13,340 9,517 3,382 441 3,823 22,317
--------------------------------------------------------------------------------------------------------------------
-- No information provided.
* Clinical suspicion of measles without laboratory investigation.
+ Includes epidemiologically linked cases.
======================================================================================================================
Return to top. Figure_3 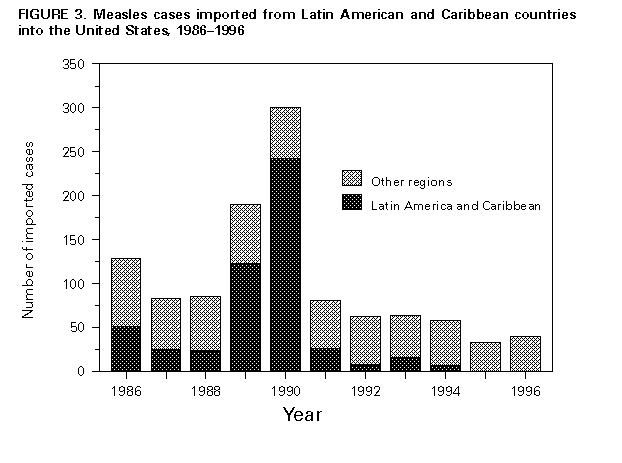 Return to top. Figure_4 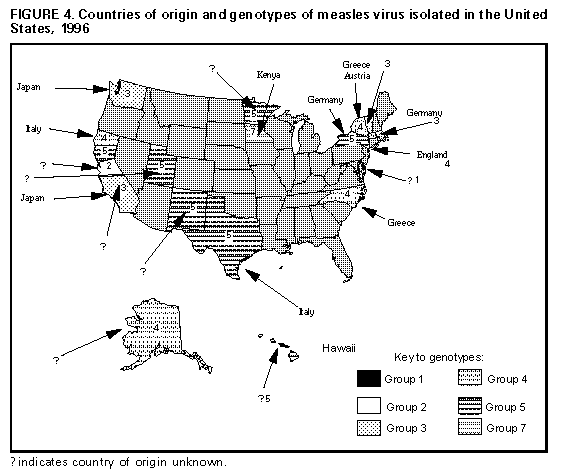 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|