 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Guidelines for School Health Programs to Promote Lifelong Healthy EatingSummary Healthy eating patterns in childhood and adolescence promote optimal childhood health, growth, and intellectual development; prevent immediate health problems, such as iron deficiency anemia, obesity, eating disorders, and dental caries; and may prevent long-term health problems, such as coronary heart disease, cancer, and stroke. School health programs can help children and adolescents attain full educational potential and good health by providing them with the skills, social support, and environmental reinforcement they need to adopt long-term, healthy eating behaviors. This report summarizes strategies most likely to be effective in promoting healthy eating among school-age youths and provides nutrition education guidelines for a comprehensive school health program. These guidelines are based on a review of research, theory, and current practice, and they were developed by CDC in collaboration with experts from universities and from national, federal, and voluntary agencies. The guidelines include recommendations on seven aspects of a school-based program to promote healthy eating: school policy on nutrition, a sequential, coordinated curriculum, appropriate instruction for students, integration of school food service and nutrition education, staff training, family and community involvement, and program evaluation. INTRODUCTION School-based programs can play an important role in promoting lifelong healthy eating. Because dietary factors "contribute substantially to the burden of preventable illness and premature death in the United States," the national health promotion and disease prevention objectives encourage schools to provide nutrition education from preschool through 12th grade (1). The U.S. Department of Agriculture's (USDA) Nutrition Education and Training (NET) Program urges "nutrition education {to} be a major educational component of all child nutrition programs and offered in all schools, child care facilities, and summer sites" by the year 2000 (2). Because diet influences the potential for learning as well as health, an objective of the first national education goal is that children "receive the nutrition and health care needed to arrive at school with healthy minds and bodies" (3). The recommendations in this report are intended to help personnel and policymakers at the school, district, state, and national levels meet the national health objectives and education goals by implementing school-based nutrition education policies and programs. This report may also be useful to students, to parents, and to personnel in local and state health departments, community-based health and nutrition programs, pediatric clinics, and training institutions for teachers and public health professionals. These recommendations complement CDC guidelines for school health programs to prevent the spread of acquired immunodeficiency syndrome (AIDS) (4), to prevent tobacco use and addiction (5), and to promote physical activity (6). In this report, nutrition education refers to a broad range of activities that promote healthy eating behaviors. The nutrition education guidelines focus largely on classroom instruction, but they are relevant to all components of a comprehensive school health program -- health education; a healthy environment; health services; counseling, psychological, and social services; integrated school and community efforts; physical education; nutrition services; and school-based health promotion for faculty and staff (7). Although the meals served by school food service programs are an important part of a school health program, this report does not provide specific recommendations related to purchasing and preparing food for school meals. Detailed information on this topic is available from many other publications (8-19) and information sources (see Appendix A). These guidelines also do not address the specific nutrition education and counseling needs of pregnant adolescents (20,21) or young persons with special needs (22-28). These guidelines are based on a synthesis of research, theory, and current practice and are consistent with the principles of the national health education standards (29), the opportunity-to-learn standards for health education (29), the position papers of leading voluntary organizations involved in child nutrition (30), and the national action plan to improve the American diet (31). To develop these guidelines, CDC convened meetings of experts in nutrition education, reviewed published research, considered the recommendations of national policy documents (1,32-35), and consulted with experts from national, federal, and voluntary organizations. EFFECTS OF DIET ON THE HEALTH, GROWTH, AND INTELLECTUAL DEVELOPMENT OF YOUNG PERSONS School-based nutrition education can improve dietary practices that affect young persons' health, growth, and intellectual development. Immediate effects of unhealthy eating patterns include undernutrition, iron deficiency anemia, and overweight and obesity. Undernutrition Even moderate undernutrition can have lasting effects on children's cognitive development and school performance (36). Chronically undernourished children attain lower scores on standardized achievement tests, especially tests of language ability (37). When children are hungry or undernourished, they have difficulty resisting infection and therefore are more likely than other children to become sick, to miss school, and to fall behind in class (36,37); they are irritable and have difficulty concentrating, which can interfere with learning (38); and they have low energy, which can limit their physical activity (38). Some reports have estimated that millions of children in the United States experience hunger over the course of a year (39), but no scientific consensus currently exists on how to define or measure hunger (1). Skipping breakfast can adversely affect children's performance in problem-solving tasks (40-42). A study of low-income elementary school students indicated that those who participated in the School Breakfast Program had greater improvements in standardized test scores and reduced rates of absence and tardiness than did children who qualified for the program but did not participate (43). Twelve percent of students reported skipping breakfast the day before one national survey was taken (44); 40% of 8th- and 10th-grade students in another study reported having eaten breakfast on less than or equal to 2 days the week before the survey (45). Strategies to encourage adequate nutrition among young persons include the following:
Iron Deficiency Anemia Iron deficiency anemia is the most common cause of anemia in the United States (33). Iron deficiency hampers the body's ability to produce hemoglobin, which is needed to carry oxygen in the blood. This deficiency can increase fatigue, shorten attention span, decrease work capacity, reduce resistance to infection, and impair intellectual performance (33,46). Among school-age youths, female adolescents are at greatest risk for iron deficiency. Approximately 1% of elementary school-age children and 2%-4% of adolescent girls ages 12-19 years show evidence of iron deficiency anemia (47). To prevent iron deficiency, children and adolescents should eat adequate amounts of foods high in iron and in vitamin C, which helps the body absorb iron efficiently (33). Overweight and Obesity * Overweight and obesity are increasing among children and adolescents in the United States (48-52). The prevalence of overweight among youths ages 6-17 years in the United States has more than doubled in the past 30 years; most of the increase has occurred since the late 1970s (52). Approximately 4.7 million, or 11%, of youths ages 6-17 years are seriously overweight (52). Obesity in young persons is related to elevated blood cholesterol levels (53-56) and high blood pressure (57-59), and some very obese youths suffer from immediate health problems (e.g., respiratory disorders, orthopedic conditions, and hyperinsulinemia) (60). Being overweight during childhood and adolescence has been associated with increased adult mortality (61,62). Furthermore, obese children and adolescents are often excluded from peer groups and discriminated against by adults, experience psychological stress, and have a poor body image and low self-esteem (63,64). Increased physical activity and appropriate caloric intake are recommended for preventing and reducing obesity (35). CDC's guidelines for school and community health programs to promote physical activity among youths address strategies for increasing physical activity among young persons (6). Unsafe Weight-Loss Methods Many young persons in the United States practice unsafe weight-loss methods. Deliberately restricting food intake over long periods can lead to poor growth and delayed sexual development (65). Data from one study indicated that the rate of smoking initiation is higher for adolescent girls who diet or who are concerned about their weight than for nondieters or girls having few weight concerns (66), and another study indicated that many white female high school students who smoke report using smoking to control their appetite and weight (67). Harmful weight loss practices have been reported among girls as young as 9 years old (68,69). Young persons involved in certain competitive sports and dancing are particularly at risk for unsafe weight control practices (70). A national survey of 8th- and 10th-grade students found that 32% skipped meals, 22% fasted, 7% used diet pills, 5% induced vomiting after meals, and 3% used laxatives to lose weight (45). Children and adolescents should learn about the dangers of unsafe weight-loss methods and about safe ways to maintain a healthy weight. The emphasis of society in the United States on thinness should be challenged, and young persons need to develop a healthy body image (71). Eating Disorders Eating disorders (e.g., anorexia nervosa and bulimia nervosa) are psychological disorders characterized by severe disturbances in eating behavior. Anorexia nervosa is characterized by a refusal to maintain a minimally normal body weight, and bulimia nervosa is characterized by repeated episodes of binge eating followed by compensatory behaviors such as self-induced vomiting (72). Eating disorders often start in adolescence, and greater than 90% of cases occur among females (72). Anorexia nervosa and bulimia nervosa affect as many as 3% of adolescent and young adult females, and the incidence of anorexia nervosa appears to have increased in recent decades (72). Compared with adolescents who have normal eating patterns, adolescents who have eating disorders tend to have lower self-esteem; a negative body image; and feelings of inadequacy, anxiety, social dysfunction, depression, and moodiness (73). Eating disorders can cause many severe complications, and mortality rates for these disorders are among the highest for any psychiatric disorder (74). Persons who have eating disorders should receive immediate medical and psychological treatment. Dental Caries Dental caries is perhaps the most prevalent of all diseases (1). It affects 50.1% of youths ages 5-17 years and 84.4% of youths age 17 years (75). More than 50 million hours of school time are lost annually because of dental problems or dental visits (76). Dental caries is a progressive disease, which, if left untreated, can result in acute infections, pain, costly treatment, and tooth loss. A strong link exists between sugar consumption and dental caries (33). To prevent dental caries, children and adolescents should drink fluoridated water, use fluoridated toothpaste, brush and floss their teeth regularly, have dental sealants applied to the pits and fissures of their teeth, and consume sugars in moderation (1). EFFECTS OF CHILDHOOD EATING PATTERNS ON CHRONIC DISEASE RISKS OF ADULTS Nutrition education also should focus on preventing children and adolescents from developing chronic diseases during adulthood. Some of the physiological processes that lead to diet-related chronic disease begin in childhood. For example, autopsy studies have demonstrated that early indicators of atherosclerosis (the hardening of the arteries that is the most common cause of coronary heart disease {CHD}) begin in youth (77-83) and are related to blood cholesterol levels in young persons (79,81-83). Unhealthy eating practices that contribute to chronic disease are established early in life; young persons having unhealthy eating habits tend to maintain these habits as they age (84). Thus, it is efficacious to teach persons healthy eating patterns when they are young; high-risk eating behaviors and physiological risk factors are difficult to change once they are established during youth. Diet-related risk factors for cardiovascular disease (e.g., high blood cholesterol level, high blood pressure, and overweight) are common in youths in the United States (34,52,85-90). Compared with their peers, children and adolescents who have high blood cholesterol (34,91-96), have high blood pressure (97,98), or are obese (91,99-103) are more likely to have these risk factors during adulthood. Poor diet and inadequate physical activity together account for at least 300,000 deaths in the United States annually and are second only to tobacco use as the most prominent identifiable contributor to premature death (104). Interventions that promote healthy eating and physical activity behaviors during childhood and adolescence may not only prevent some of the leading causes of illness and death but also decrease direct health-care costs and improve quality of life. Diet is a known risk factor for the development of the nation's three leading causes of death: CHD, cancer, and stroke (33). Other health problems of adulthood associated with diet are diabetes, high blood pressure, overweight, and osteoporosis. Coronary Heart Disease CHD kills more persons in the United States than any other disease does (1). Diet-related risk factors for CHD include high blood cholesterol, high blood pressure, and obesity. These risk factors can be reduced by consuming less fat (particularly saturated fat) and cholesterol and by increasing physical activity (105). Cancer One out of every five deaths in the United States is attributable to cancer (106). Dietary factors have been associated with several types of cancer, including colon, breast, and prostate (33). All cancer deaths in the United States might be reduced as much as 35% through dietary changes (107,108). The risk for some types of cancer may be reduced by maintaining a healthy weight; limiting consumption of fat, alcohol, and salt-cured, salt-pickled, or smoked foods; and eating more foods that protect the body against cancer (fruits, vegetables, whole grain cereals, and other high-fiber foods) (109). The National Cancer Institute advises eating at least five servings of fruits and vegetables each day (110). Stroke Cerebrovascular disease, or stroke, is the third leading cause of death in the United States and a major cause of illness and disability (111). The most important risk factor for stroke is high blood pressure, which often can be controlled or prevented by adopting a healthy diet and maintaining a healthy weight (112). The risk for stroke can be reduced by consuming less sodium, increasing physical activity, and maintaining a healthy body weight. Diabetes Diabetes is the seventh leading cause of death in the United States (104). CHD is two to four times more common and stroke is two to six times more common in persons who have diabetes than in persons who do not have diabetes (113). Diabetes can lead to blindness, kidney disease, and nerve damage (113). Non-insulin-dependent diabetes mellitus, which affects approximately 90% of persons who have diabetes, is often associated with obesity (114). Maintaining a desirable body weight through physical activity and modest caloric restriction is important in preventing diabetes and controlling its complications (114). High Blood Pressure High blood pressure is a major cause of CHD, stroke, and kidney failure. About one in four adults in the United States has high blood pressure (115). Persons who have high blood pressure have three to four times the risk of developing CHD and as much as seven times the risk of stroke as do those who have normal blood pressure (116). Persons can reduce their risk for high blood pressure by consuming less sodium, increasing physical activity, and maintaining a healthy body weight. A diet high in potassium may help reduce the risk of high blood pressure (117). Overweight In the United States, about one in three adults is overweight (118), and these persons are at increased risk for CHD, some types of cancer, stroke, diabetes mellitus, high blood pressure, and gallbladder disease (33). Overall risk for premature death is increased by excess weight; the risk increases as severity of overweight increases (33). The best way to lose weight is to increase physical activity and control caloric intake, preferably by adopting a diet that is low in fat and high in vegetables, fruits, and grains (35). Osteoporosis Osteoporosis is a decrease in the amount of bone so severe that the bone fractures easily. About 1.3 million bone fractures, including many fatal hip fractures, occur per year in persons greater than or equal to 45 years of age (33). Low dietary calcium, a mineral essential for bone growth, may be associated with an increased risk for osteoporosis (33). For females especially, eating enough calcium is particularly important during childhood, adolescence, and young adulthood -- when bones approach their maximum density -- to reduce the risk for osteoporosis later in life (1,119- 122). Regular weight-bearing exercises also can help prevent osteoporosis (33). GUIDELINES FOR HEALTHY EATING To prevent certain diseases and to promote good health, persons greater than 2 years of age should follow the seven recommendations that constitute the Dietary Guidelines for Americans (35). These guidelines are developed by the USDA and USDHHS and are published every 5 years. They are based on extensive reviews of hundreds of studies conducted over many years and represent the best current advice that nutrition scientists can give. The guidelines are consistent with dietary recommendations made by major health promotion organizations, including the National Research Council (32), the National Cholesterol Education Program of the National Institutes of Health (34,105), the National Cancer Institute (109), the American Cancer Society (123), and the American Heart Association (124). The principles contained in the Dietary Guidelines for Americans should be the primary focus of school-based nutrition education. By enabling young persons to adopt practices consistent with the guidelines, schools can help the nation meet its health objectives (1), which were designed to guide health promotion and disease prevention policy and programs at the federal, state, and local level throughout the 1990s. Objective 2.19 is to "increase to at least 75 percent the proportion of the Nation's schools that provide nutrition education from preschool through 12th grade, preferably as part of quality school health education" (1). The six relevant dietary guidelines are (a) eat a variety of foods; (b) balance the food you eat with physical activity -- maintain or improve your weight; (c) choose a diet with plenty of grain products, vegetables, and fruits; (d) choose a diet low in fat, saturated fat, and cholesterol; (e) choose a diet moderate in sugars; and (f) choose a diet moderate in salt and sodium. (The seventh recommendation concerns adults and alcoholic beverages.) Enabling children and adolescents to follow these guidelines can help the nation achieve these national health objectives for the year 2000 (1): 2.3 Reduce overweight to a prevalence of less than or equal to 20% among people aged 20 and older and less than or equal to 15% among adolescents aged 12 through 19. 2.5 Reduce average dietary fat intake to less than or equal to 30% of calories and average saturated fat intake to less than or equal to 10% of calories among people aged two and older. 2.6 Increase complex carbohydrates and fiber-containing foods in the diets of adults to five or more daily servings for vegetables (including legumes) and fruits and to six or more daily servings for grain products. 2.7 Increase to greater than or equal to 50% the proportion of overweight people aged 12 and older who have adopted sound dietary practices combined with regular physical activity to attain an appropriate body weight. 2.8 Increase calcium intake so greater than or equal to 50% of youth aged 12 through 24 and greater than or equal to 50% of pregnant and lactating women consume three or more servings daily of foods rich in calcium, and greater than or equal to 50% of people aged greater than or equal to 25 consume two or more servings daily. 2.9 Decrease salt and sodium intake so that greater than or equal to 65% of home meal preparers prepare foods without adding salt, greater than or equal to 80% of people avoid using salt at the table, and greater than or equal to 40% of adults regularly purchase foods modified or lower in sodium. The Food Guide Pyramid (Figure_1) was designed by the USDA and USDHHS to help persons follow the Dietary Guidelines for Americans. Schools can use the pyramid to illustrate the concepts of variety (eat different foods from among and within the food groups), moderation (limit the consumption of foods high in fat and added sugars), and proportionality (eat relatively greater amounts of foods from the groups that are lower in the pyramid: grains, vegetables, and fruits) (125). Other educational materials supplement the pyramid by listing low-fat choices within each food group (35). EATING BEHAVIORS OF CHILDREN AND ADOLESCENTS IN THE UNITED STATES Many young persons in the United States do not follow the recommendations of the Dietary Guidelines for Americans or the Food Guide Pyramid. On average, children and adolescents consume too much fat, saturated fat, and sodium and not enough fruits, vegetables, or calcium (44,126-129; CDC, unpublished data). Children and adolescents obtain 33%-35% of their calories from fat and 12%-13% from saturated fat (above the recommended levels of 30% and 10%, respectively) (44,128,129). Only 16% of children ages 6-11 years and 15% of adolescents ages 12-19 years meet the recommendation for total fat intake; only 9% of children and 7% of adolescents meet the recommendation for saturated fat intake (130). Almost one-half of 8th- and 10th-grade students eat three or more snacks a day, and most of these snacks are high in fat, sugar, or sodium (45). Unpublished data from CDC's 1993 Youth Risk Behavior Survey indicated that, on the day before the survey, 41% of high school students in the United States ate no vegetables and 42% ate no fruits (127) (Appendix B). An analysis of a nationally representative sample of youths ages 2-18 years indicated that, over a 3-day period, the youths ate only 3.6 servings of fruits and vegetables daily and that fried potatoes accounted for a large proportion of the vegetables consumed, 20.4% of the youths ate the recommended five or more servings of fruits and vegetables daily, 50.8% ate fewer than one serving of fruit per day, and 29.3% ate fewer than one serving per day of vegetables that were not fried (131). Adolescent females eat considerably less calcium and iron than recommended by the Food and Nutrition Board of the National Research Council (126,129). Children and adolescents appear to be familiar with the general relationship between nutrition and health but are less aware of the relationship between specific foods and health. For example, young persons understand the importance of limiting fat, cholesterol, and sodium in one's diet, but they do not know which foods are high in fat, cholesterol, sodium, or fiber (45,132,133). One study indicated that adolescents were well-informed about good nutrition and health but did not use their knowledge to make healthy food choices (134). THE NEED FOR SCHOOL-BASED NUTRITION EDUCATION Young persons need nutrition education to help them develop lifelong eating patterns consistent with the Dietary Guidelines for Americans and the Food Guide Pyramid. Schools are ideal settings for nutrition education for several reasons:
School-based nutrition education is particularly important because today's children and adolescents frequently decide what to eat with little adult supervision (139). The increase in one-parent families or families having two working parents and the availability of convenience foods and fast-food restaurants inhibit parents' monitoring of their children's eating habits. Young persons' food choices are influenced by television advertisements for low-nutritive foods. Young persons see about one food advertisement for every 5 minutes of Saturday morning children's shows (140). Most of the foods advertised during children's programming are high in fat, sugar, or sodium; practically no advertisements are for healthy foods such as fruits and vegetables (140-142). Studies have indicated that, compared with those who watch little television, children and adolescents who watch more television are more likely to have unhealthy eating habits and unhealthy conceptions about food (143), ask their parents to buy foods advertised on television (144), and eat more fat (145). Some studies of young persons have found that television watching is directly associated with obesity (146-149). Because youths in the United States spend, on average, more than 20 hours a week watching television (150) -- more time over the course of the year than they are in school (141) -- school-based programs should help counter the effect of television on young persons' eating habits. Schools are a critical part of the social environment that shapes young persons' eating behaviors and can therefore play a large role in helping improve their diet. However, schools cannot achieve this goal on their own when the cultural milieu has a large influence on food-related beliefs, values, and practices (30,138). Families, food stores, restaurants, the food industry, religious institutions, community centers, government programs, and the mass media must also support the principles of the Dietary Guidelines for Americans. The USDA's Team Nutrition (see Appendix A) seeks to gain the support of many sectors of society for improving the diet of young persons by creating innovative public and private partnerships that promote healthy food choices through the media, schools, families, and community (151). PROMOTING HEALTHY EATING THROUGH A COMPREHENSIVE SCHOOL HEALTH PROGRAM In the school environment, classroom lessons alone might not be enough to effect lasting changes in students' eating behaviors (30); students also need access to healthy food and the support of persons around them (137). The influence of school goes beyond the classroom and includes normative messages from peers and adults regarding foods and eating patterns. Students are more likely to receive a strong, consistent message when healthy eating is promoted through a comprehensive school health program. A comprehensive school health program empowers students with not only the knowledge, attitudes, and skills required to make positive health decisions but also the environment, motivation, services, and support necessary to develop and maintain healthy behaviors (152). A comprehensive school health program includes health education; a healthy environment; health services; counseling, psychological, and social services; integrated school and community efforts; physical education; nutrition services; and a school-based health program for faculty and staff (7). Each component can contribute to integrated efforts that promote healthy eating. For example, classroom lessons on nutrition can be supported by
RECOMMENDATIONS FOR SCHOOL HEALTH PROGRAMS PROMOTING HEALTHY EATING Based on the available scientific literature, national nutrition policy documents, and current practice, these guidelines provide seven recommendations for ensuring a quality nutrition program within a comprehensive school health program. These recommendations address school policy on nutrition, a sequential, coordinated curriculum, appropriate and fun instruction for students, integration of school food service and nutrition education, staff training, family and community involvement, and program evaluation. Strategies that schools can use to achieve these recommendations are available (Appendix C). However, local school systems need to assess the nutrition needs and issues particular to their communities, and they need to work with key school- and community-based constituents, including students, to develop the most effective and relevant nutrition education plans for their communities. Vigorous, coordinated, and sustained support from communities, local and state education and health agencies, institutions of higher education, and national organizations also is necessary to ensure success (29).
Recommendation 1. Policy: Adopt a coordinated school nutrition policy that promotes healthy eating through classroom lessons and a supportive school environment. Rationale for the Policy A coordinated school nutrition policy, particularly as part of an overall school health policy, provides the framework for implementing the other six recommendations and ensures that students receive nutrition education messages that are reinforced throughout the school environment. For example, such a policy would address nutrition education classes; school lunch and breakfast; classroom snacks and parties; use of food to reward or discipline; and food sold in vending machines, at school stores, snack bars, sporting events, and special activities, and as part of fundraising activities. The school environment can powerfully influence students' attitudes, preferences, and behaviors related to food (137). Without a coordinated nutrition policy, schools risk negating the health lessons delivered in the classroom and cafeteria by allowing actions that discourage healthy eating behaviors. Developing the Policy A school nutrition policy should be a brief document that incorporates input from all relevant constituents of the school community: students, teachers, coaches, staff, administrators, food service personnel, nurses, counselors, public health professionals, and parents. The policy should meet local needs and be adapted to the health concerns, food preferences, and dietary practices of different ethnic and socioeconomic groups. Technical assistance for assessing nutrition education needs is available through the state NET Program (155). Schools might consider using one or more of the following techniques to assess their particular needs:
The policy plan should include means of obtaining follow-up input from all parties and means of revising the plan as needed. Student involvement is critical to the success of a nutrition policy. A nutrition advisory committee or a nutrition subcommittee of the school health advisory council having student members can develop and promulgate a coordinated school nutrition policy. Technical assistance in forming a school nutrition advisory committee is available from the American School Food Service Association (Appendix A). Successful implementation of a nutrition policy also requires the active support of school and district educational leadership. Content of the Policy The written policy should describe the importance of the nutrition component within the comprehensive school health program. This section can briefly describe the role of good nutrition in promoting childhood growth, health, and learning; discuss the role of child and adolescent nutrition in reducing the risk for chronic diseases of adulthood; identify the importance of establishing a school environment that supports healthy eating choices by young persons; and generate support for the policy by identifying how improvements in student nutrition can satisfy the needs of different constituents of the school community (e.g., students, teachers, and food service personnel). An optimal policy on nutrition should publicly commit the school to providing adequate time for a curriculum on nutrition, serving healthy and appealing foods at school, developing food-use guidelines for teachers, supporting healthy school meals, and establishing links with nutrition service providers. Curriculum. Adequate time should be allocated for nutrition education throughout the preschool, primary, and secondary school years as part of a sequential, comprehensive school health education program. In addition, teachers should be adequately trained to teach nutrition and be provided with ongoing in-service training. Healthy ** and appealing foods. Healthy and appealing foods should be available in meals, a la carte items in the cafeteria, snack bars, and vending machines (Exhibit 1) (Table_1); as classroom snacks; and at special events, athletic competitions, staff meetings, and parents' association meetings. In addition, schools should discourage the sale of foods high in fat, sodium, and added sugars (e.g., candy, fried chips, and soda) on school grounds and as part of fundraising activities. Although selling low-nutritive foods may provide revenue for school programs, such sales tell students that it is acceptable to compromise health for financial reasons (158). The school thereby risks contradicting the messages on healthy eating given in class. If schools contract with food service management companies to supply meals, the contractors should be required to serve appealing, low-fat, low-sodium meals that comply with the standards of the Dietary Guidelines for Americans. Food use guidelines for teachers. Schools should discourage teachers from using food for disciplining or rewarding students. Some teachers give students low-nutritive foods, such as candy, as a reward for good behavior, and punish misbehaving students by denying a low-nutritive treat (159). These practices reinforce students' preferences for low-nutritive foods and contradict what is taught during nutrition education. Schools should recommend that both teachers and parents serve healthy party snacks and treats (160). Support for healthy school meals. Starting with the 1996-1997 school year, schools will be required to serve meals that comply with the standards of the Dietary Guidelines for Americans (154). To encourage students to participate in school meal programs and to make healthy choices in cafeterias, schools can use marketing-style incentives and promotions (13,14,135,161); use healthy school meals as examples in class; educate parents about the value of healthy school meals; involve students and parents in planning meals; and have teachers, administrators, and parents eat in the cafeteria and speak favorably about the healthy meals available there. Students should also be given adequate time and space to eat meals in a pleasant and safe environment (162). Links with nutrition service providers. Schools should establish links with qualified public health and nutrition professionals who can provide screening, referral, and counseling for nutritional problems (30,163); inform families about supplemental nutrition services available in the community, such as WIC (164), food stamps, local food pantries, the Summer Food Service Program, and the Child and Adult Care Food Program; and implement nutrition education and health promotion activities for school faculty, other staff, school board members, and parents. These links can help prevent and resolve nutritional problems that can impair a student's capacity to learn, demonstrate the value placed on good nutrition for the entire school community, and help adults serve as role models for school-age youths. Recommendation 2. Curriculum for nutrition education: Implement nutrition education from preschool through secondary school as part of a sequential, comprehensive school health education curriculum designed to help students adopt healthy eating behaviors. Nutrition Education as Part of a Comprehensive School Health Education Program Nutrition education should be part of a comprehensive health education curriculum that focuses on understanding the relationship between personal behavior and health. This curriculum should give students the knowledge and skills they need to be "health literate," as delineated by the national health education standards (29) (Exhibit 2) (Table_2). The comprehensive health education approach is important to nutrition education because
Linking nutrition and physical activity is particularly important because of the rising proportion of overweight youths in the United States. Nutrition education lessons should stress the importance of combining regular physical activity with sound nutrition as part of an overall healthy lifestyle. Physical education classes, in turn, should include guidance in food selection (6). Sequential Lessons and Adequate Time Students who receive more lessons on nutrition have more positive behavioral changes than students who have fewer lessons (166,167). To achieve stable, positive changes in students' eating behaviors, adequate time should be allocated for nutrition education lessons. The curriculum should be sequential from preschool through secondary school; attention should be paid to scope and sequence. When designing the curriculum, schools should assess and address their students' needs and concerns. A curriculum targeted to a limited number of behaviors might make the most effective use of a scarce instructional time available for nutrition education (136). To maximize classroom time, nutrition education can be integrated into the lesson plans of other school subjects; for example, math lessons could analyze nutrient intake or reading lessons could feature texts on nutrition (168). Little research on the integrated approach has been conducted (137), but embedding information on nutrition in other courses probably reinforces the goals of nutrition education. However, the exclusive use of an integrative approach might sacrifice key elements of an effective nutrition education program (e.g., adequate time, focusing on behaviors and skill-building, attention to scope and sequence, and adequate teacher preparation) (137). Therefore, integration into other courses can complement but should not replace sequential nutrition education lessons within a comprehensive school health education curriculum. Classroom time can be maximized also by having nutrition education lessons use skills learned in other classes (e.g., math or language arts) (169-171). Organizations and agencies can supply information on specific nutrition education curricula and materials (Appendix A). The USDA's NET Program provides technical assistance in school-based nutrition education (2,172). The Food and Nutrition Information Center of USDA's National Agricultural Library provides information on nutrition education evaluation and resources and serves as a national depository and lending library for NET materials. Nutritionists at some organizations can also answer specific nutrition content questions (Appendix A). Focusing on Promoting Healthy Eating Behaviors The primary goal of nutrition education should be to help young persons adopt eating behaviors that will promote health and reduce risk for disease. Knowing how and why to eat healthily is important, but knowledge alone does not enable young persons to adopt healthy eating behaviors (137). Cognitive-focused curricula on nutrition education typically result in gains in knowledge but usually have little effect on behavior (173-178). Behaviorally based education encourages specific healthy eating behaviors (e.g., eating less fat and sodium and eating more fruits and vegetables) (136,179); however, it does not detail the technical and scientific knowledge on which dietary recommendations are based and, therefore, might not fulfill science education requirements (180). The strategies listed in Appendix C can be used as central concepts in a behaviorally based nutrition education program. Several programs using a behavioral approach have achieved significant (p less than 0.05), positive changes in students' eating behaviors (167,181-190). Compared with students in control schools, students in some behaviorally based health and nutrition education programs had significant (p less than 0.05), favorable changes in serum cholesterol levels (167,188,191), blood pressure level (167,191), and body mass index (184). Although most of the behaviorally oriented programs did not achieve all their behavioral aims -- perhaps because of the limited amount of curriculum time (136) -- current scientific knowledge indicates that a focus on behavior is a key determinant in the success of nutrition education programs (136-138). Recommendation 3. Instruction for students: Provide nutrition education through developmentally appropriate, culturally relevant, fun, participatory activities that involve social learning strategies. Developmentally Appropriate and Culturally Relevant Activities Different educational strategies should be used for young persons at different stages of cognitive development. Regardless of the amount and quality of teaching they receive, young elementary schoolchildren might not fully understand abstract concepts (e.g., the nutrient content of foods or the classification of foods into groups) (192-194). Nutrition education for young children should focus on concrete experiences (e.g., increasing exposure to many healthy foods and building skills in choosing healthy foods) (169). More abstract associations between nutrition and health become appropriate as children approach middle school. By this age, children can understand and act on the connection between eating behaviors and health (137,194). Nutrition education for middle and high school students should focus on helping students assess their own eating behaviors and set goals for improving their food selection (138,195). Lessons for older children should emphasize personal responsibility, decision-making skills, and resisting negative social pressures (183,185,187,189). Nutrition education presents opportunities for young persons to learn about and experience cultural diversity related to food and eating. Students from different cultural groups have different health concerns, eating patterns, food preferences, and food-related habits and attitudes. These differences need to be considered when designing lesson plans or discussing food choices. Nutrition education can succeed only when students believe it is relevant to their lives. Active Learning and an Emphasis on Fun The context in which students learn about healthy eating behaviors and the feelings students associate with healthy foods are key factors in determining their receptivity to nutrition education. Students are more likely to adopt healthy eating behaviors when
Computer-based lessons on nutrition can also be effective (198), especially when teacher time is limited or when student self-assessment is appropriate. Interactive, highly entertaining, and well-designed computer programs are now available to help young persons learn healthy food selection skills and assess their own diets (199,200). Computer-based lessons allow students to move at their own pace and can capture their attention. Social Learning Techniques Most of the nutrition education programs that have resulted in behavioral change have used teaching strategies based on social learning theory (195,201-205). In such lessons, increasing student knowledge is only one of many objectives. Social learning instruction also emphasizes
Recommendation 4. Integration of school food service and nutrition education: Coordinate school food service with nutrition education and with other components of the comprehensive school health program to reinforce messages on healthy eating. The school cafeteria provides a place for students to practice healthy eating. This experience should be coordinated with classroom lessons to allow students to apply critical thinking skills taught in the classroom (2,8,9,11-15,18,169,178,206). School food service personnel can
In addition, classroom teaching can complement the goals of the school food service. For example, teachers can help food service managers by teaching students about the importance of nutritious school meals and getting feedback from students on new menu items developed to meet the goals set by USDA's School Meals Initiatives for Healthy Children (154). To ensure consistent nutrition messages from the school, food service personnel should work closely with those responsible for other components of the school health program. For example, the personnel can
Recommendation 5. Training for school staff: Provide staff involved in nutrition education with adequate preservice and ongoing in-service training that focuses on teaching strategies for behavioral change. Training in nutrition and health education can increase the extent to which teachers implement a curriculum (207-209), which in turn affects the likelihood that students' eating behaviors will change (167,207). All elementary school teachers as well as secondary school teachers in disciplines such as home economics, family and consumer sciences, language arts, physical education, and science should receive nutrition education training. State NET Programs can provide technical assistance for training teachers in nutrition education (Appendix A). Training should address content and teaching strategies. Because classroom teachers often need more help with innovative nutrition teaching techniques than with content (195,210), training should focus on giving teachers the skills they need to use the nonlecture, active learning methods discussed previously (195). Training programs are most effective if they
Teachers should understand the importance of fully implementing the selected curriculum and become familiar with its underlying theory and concepts. Training should also help teachers assess and improve their own eating practices and make them aware of the behavioral messages they give as role models (213). Continuing education activities in nutrition education should be offered to food service personnel so this staff can reinforce classroom instruction through the school meal program and help shape the school's nutrition policy. State NET Programs and the National Food Service Management Institute provide technical assistance and training seminars for school nutrition professionals (see Appendix A). Administrative support is also critical to implementing a new program (214). Training for school administrators can help gain their support for nutrition education. Health promotion services for all school staff can positively affect their eating behaviors and their effectiveness in teaching healthy eating behaviors (180,215,216). Recommendation 6. Family and community involvement: Involve family members and the community in supporting and reinforcing nutrition education. The attitudes and behaviors of parents and caretakers directly influence children's and adolescents' choice of foods (217,218). Parents control most of the food choices available at home, so changing parents' eating behaviors may be one of the most effective ways to change their children's eating behaviors. Involving parents in a nutrition education curriculum at the elementary school level can enhance the eating behaviors of both the students (181,219-221) and the parents (181,219,222). Although parental involvement can enhance the effects of nutrition education programs at the elementary school level, it is not known whether involving parents at the secondary school level helps improve the students' eating behaviors. For older youths, self-assessment (185,189,198) and peer educators (187) might be more influential than parental involvement (137). Parents are usually more receptive to activities that can be done at home than to those that require their attendance at the school (223,224). To involve parents and other family members in nutrition education, schools can
Through school health advisory councils or through direct contact with community organizations, schools can engage community resources and services to respond to the nutritional needs of students (225,226). Schools can also participate in community-based nutrition education campaigns sponsored by public health agencies or voluntary organizations. Students are most likely to adopt healthy eating behaviors if they receive consistent messages through multiple channels (e.g., home, school, community, and the media) and from multiple sources (e.g., parents, peers, teachers, health professionals, and the media) (225). Recommendation 7. Program evaluation: Regularly evaluate the effectiveness of the school health program in promoting healthy eating, and change the program as appropriate to increase its effectiveness. Policymakers should regularly review the effectiveness of the school nutrition program. All groups affected by the program should have the opportunity to provide input. Assessment of nutrition programs and policies should include whether
Schools might also consider measuring the effects of their programs and policies on self-reported eating behaviors; key variables that influence behavior, such as knowledge, attitudes, self-confidence, and behavioral intentions; and in-school eating behaviors that are easy to assess, such as participation in school food service programs and the number of students choosing healthy alternatives in the cafeteria (e.g., salad bars or low-fat milk). Schools can consult with the state NET Program or with evaluation specialists at universities, school districts, or the state departments of education or health to identify methods and materials for evaluating the effectiveness of their program (227,228). Valid evaluations can increase parent and community support for school programs, help schools reward teachers for exceptional work, and support grant applications for enhancing school health programs. CONCLUSION To ensure a healthy future for our children, school-based nutrition education programs must become a national priority. These programs should be part of comprehensive school health programs and reach students from preschool through secondary school. School leaders, community leaders, and parents must commit to implementing and sustaining nutrition education programs within the schools. Such support is crucial to promoting healthy eating behaviors. The seven recommendations for school-based nutrition education presented in this report provide the framework for establishing such programs. By adopting these recommendations, schools can help ensure that all school-age youths attain their full educational potential and good health. References
* Obesity refers to an excess of total body fat. Body fat content is usually estimated by one of two techniques, measuring skinfold thickness or computing the ratio of body weight to height. Researchers who use weight-to-height ratios tend to use the term "overweight" instead of "obesity." Although weight-to-height ratios correlate highly with body fat, they do not distinguish between body fat and lean body tissue: excess fat tissue is generally assumed to account for the additional weight, but excess weight can also include lean body mass or a large body frame (33). ** As defined by the U.S. Food and Drug Administration (156,157) in its food label regulations, a "healthy" food must be low in fat (less than or equal to 3 g per serving), be low in saturated fat (less than or equal to 1 g per serving), contain limited amounts of cholesterol (less than or equal to 60 mg per serving for a single-item food), and contain limited amounts of salt (less than or equal to 480 mg per serving until 1998, when the criterion for a single-item food will decrease to less than or equal to 360 mg per serving). In addition, single-item foods that are not raw fruits or vegetables must provide greater than or equal to 10% of the daily value of one or more of the following nutrients: vitamin A, vitamin C, iron, calcium, protein, and fiber. Criteria for products that include more than one type of food (e.g., macaroni and cheese) vary depending on the food. *** When serving food, teachers must use hygienic food handling practices and consider possible food allergies and religious prohibitions; the food service director can help in this area. Figure_1 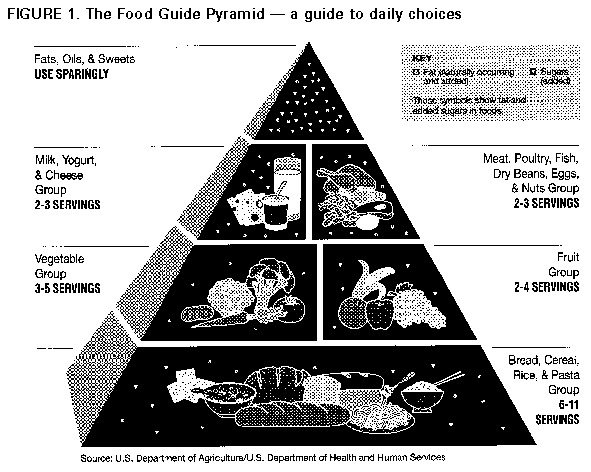 Return to top. Table_1 Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size.
EXHIBIT 1: Sample List of Vending Machine Foods Low in Saturated Fat (34)
==================================================================================
Canned fruit
Fresh fruit (e.g., apples and oranges) *
Fresh vegetables (e.g., carrots)
Fruit juice and vegetable juice
Low-fat crackers and cookies, such as fig bars and gingersnaps
Pretzels
Bread products (e.g., bread sticks, rolls, bagels, and pita bread)
Ready-to-eat, low-sugar cereals
Granola bars made with unsaturated fat
Low-fat (1%) or skim milk *
Low-fat or nonfat yogurt *
Snack mixes of cereal and dried fruit with a small amount of nuts and seeds **
Raisins and other dried fruit **
Peanut butter and low-fat crackers ***
----------------------------------------------------------------------------------
* These foods are appropriate if the vending machine is
refrigerated.
** Some schools might not want to offer these items because these
foods can contribute to dental caries.
*** Some schools might not want to offer peanut butter; although it
is low in saturated fatty acids, peanut butter is high in total
fat.
==================================================================================
Return to top. Table_2 Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size. EXHIBIT 2: National Health Education Standards (29) ====================================================================== 1. Students will comprehend concepts related to health promotion and disease prevention. 2. Students will be able to access valid health information and health-promoting products and services. 3. Students will be able to practice health-enhancing behaviors and reduce health risks. 4. Students will analyze the influence of culture, media, technology, and other factors on health. 5. Students will be able to use interpersonal communication skills to enhance health. 6. Students will be able to use goal-setting and decision-making skills to enhance health. 7. Students will be able to advocate for personal, family, and community health. ====================================================================== Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|