 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Recommendations for Prevention and Control of Tuberculosis Among Foreign-Born Persons Report of the Working Group on Tuberculosis Among Foreign-Born PersonsSummary During 1986-1997, the number of tuberculosis (TB) cases among foreign-born persons in the United States increased by 56%, from 4,925 cases (22% of the national total) to 7,702 cases (39% of the national total). As the percentage of reported TB cases among foreign-born persons continues to increase, the elimination of TB in the United States will depend increasingly on the elimination of TB among foreign-born persons. On May 16-17, 1997, CDC convened a working group of state and city TB-control program staff, as well as representatives from CDC's Division of TB Elimination and Division of Quarantine, to outline problems and propose solutions for addressing TB among foreign-born persons. The Working Group on Tuberculosis Among Foreign-Born Persons considered a) epidemiologic profiles of TB cases among foreign-born persons, b) case finding, screening, and preventive therapy for the foreign born, c) TB diagnosis and management for the foreign born, d) opportunities for collaborations with community-based organizations (CBOs) to address TB among the foreign born, and e) TB-related training needs. The Working Group's deliberations and the resulting recommendations for action by federal agencies, state and local TB-control programs, CBOs, and private health-care providers form the basis of this report. For each of the five topics of discussion, the group identified key issues, problems, and constraints and suggested solutions in the form of recommendations, which are detailed in this report. The Working Group made the following recommendations:
INTRODUCTION In 1986, CDC began collecting information on place of birth for those persons residing in the United States who have been reported to be infected with tuberculosis (TB). National surveillance data for the decade that followed indicate that the number of TB cases among persons born in other countries increased from 4,925 in 1986 to 7,702 in 1997, and that the percentage of foreign-born cases increased from 22% to 39% of the national total. In Canada and several European countries, foreign-born persons now account for more than half of TB cases. If current U.S. trends continue through the next decade, more than half of TB cases are likely to occur among the foreign born. BACKGROUND Immigration Trends The increase in TB cases among foreign-born persons over the past decade is partly attributable to increased immigration (Figure_1). The largest wave of immigration in U.S. history occurred in the early 1900s; by 1910, 14% of all U.S. residents were foreign born. Immigration declined during the next two decades, reached a low during the Great Depression (1929-1939), and then gradually increased until the mid-1980s. A peak occurred in 1986, when the Immigration Reform and Control Act was passed and persons who had entered the country illegally were allowed to legalize their status. In 1996, the most recent year for which immigration figures are available, 915,900 persons were granted permanent residence (1). In addition, an estimated 275,000 undocumented aliens arrive annually. In 1996, an estimated 24.6 million foreign-born persons resided in the United States, representing 9% of the total population (2). Another factor in the increase in TB cases among foreign-born persons is changing trends in countries of origin. Immigration has been increasing from Asia and the Latin Americas, where TB rates are 5-20 times higher than those in the United States. In 1994, 25% of the 24 million foreign-born persons in the United States were from Asia and 42% from Latin America, including 6 million persons from Mexico (2). In recent years, Asian-born persons have accounted for an increasing percentage of new immigrants; in 1995, 37% of new arrivals were from Asia (3). After Mexico, the top two countries of birth among immigrants in that year were the Philippines and Vietnam. The foreign-born population is concentrated in some areas in the United States. Forty-three percent of such persons live in California (34%) or New York (9%). Florida, Texas, New Jersey, and Illinois each have 5%-8% of the total foreign-born population (2). In 1995, two thirds of immigrants indicated California, New York, Florida, Texas, New Jersey, and Illinois as their intended residence at the time of immigration, and approximately one fourth of all new immigrants indicated an intent to live in Los Angeles or New York City (3). Characteristics of TB Cases Among Foreign-Born Persons The composition of TB cases among foreign-born persons reflects immigration patterns and trends. In 1997, Mexico was the country of origin for 22% of immigrants with TB, with the Philippines (14%) and Vietnam (11%) the next most common countries of birth. India, China, Haiti, and Korea each accounted for 3%-6% of the total. Together, these seven countries accounted for two thirds of TB cases among foreign-born persons in the United States. As expected, most TB cases among foreign-born persons are reported from the states with the most immigrants. In 1997, 66% of all TB cases among foreign-born persons were reported from California (36% of the national total), New York (15%), Texas (8%), Florida (5%), New Jersey (4%), Illinois (3%), Washington (2%), Massachusetts (2%), Virginia (2%), and Hawaii (2%) (Table_1). In 1997, TB cases among foreign-born persons were examined as a proportion of total TB cases in each state. A total of 66% of TB cases occurred among foreign-born persons in California and 51% in New York. Even in states with relatively few cases among the foreign born (e.g., Minnesota and Rhode Island), approximately 60% of TB cases in 1997 were among persons born outside the United States. Most TB cases among foreign-born persons are likely the result of reactivation of remotely acquired infection, although some transmission is probably occurring in the United States. Studies using the restriction-fragment-length polymorphism (RFLP) technique document transmission to the foreign born by others who are foreign born or U.S. born (4); other studies document high percentages of cases among the children of the foreign born (5). For all immigrant groups, the disease risk appears highest in the first years after U.S. arrival (Figure_2). Among some groups, the risk decreases rapidly over time, whereas for others, it remains high for up to 20 years (6). The risk for disease among the foreign born also appears related to chronological age and age at immigration; younger persons and those who immigrated at younger ages are at lower risk for subsequent infection with TB. The number of foreign-born persons in the United States with TB infection is unknown. However, based on the World Health Organization (WHO) estimate that one third of the world's population is infected, more than 7 million foreign-born persons in the United States might be at risk for reactivation of remotely acquired infection. PRIORITIES FOR ELIMINATING TB IN THE UNITED STATES As the percentage of reported TB cases among foreign-born persons continues to grow, the elimination of TB in the United States will depend increasingly on the elimination of TB among the foreign born. Although this factor presents challenges and requires a flexible approach, the priorities of TB control remain the same
of treatment; b) tracing the contacts of those with active disease and evaluating each contact's status regarding TB infection and disease; and c) screening persons at high risk for infection, providing preventive therapy to eligible candidates, and ensuring completion of that preventive therapy (7). TB Case Finding, Screening, and Preventive Therapy In the United States, TB screening is required for a) immigrants and refugees applying for permanent legal status and b) persons of foreign birth (e.g., business persons, students, and dependents) who entered the country on nonimmigrant visas and want to adjust their immigration status to legal permanent resident. Each year, active case finding is conducted on approximately 800,000 persons applying for long-term residence. In recent years, approximately half have been screened overseas and half in the United States. Immigrants and refugees who want to enter the United States are screened overseas by local physicians designated by U.S. consuls. Persons with suspected TB disease are assigned a specific classification -- Class A, B1, B2, or B3. The screening procedure consists of initial radiologic screening for persons aged greater than 15 years followed by sputum smear microscopy for acid-fast bacilli (AFB) in those whose radiographs are compatible with active TB. Persons who are AFB-smear-positive (designated Class A) must be treated before departure. Those who are smear-negative, but whose radiographs are compatible with active TB (Class B1) or with inactive disease (Class B2), are referred to a health department in the state of their intended residence for further evaluation. (Those persons with abnormal radiographs indicating calcified granulomas not indicative of active TB are Class B3 and are not referred for additional evaluation.) U.S. screening practices differ from those of other industrialized countries, which require negative cultures. The yield of the overseas screening process has been well documented; 3%-14% of the approximately 6,000 Class B1 immigrants and 0.4%-4% of the 12,000 Class B2 immigrants who enter the country each year are infected with active TB after arrival in the United States (8). Of those without evidence of active TB, many have positive tuberculin skin tests and radiologic abnormalities compatible with old TB; these persons are at high risk for reactivation and are candidates for preventive therapy regardless of age. A study in Seattle determined that approximately half of Class B1 immigrants and one fourth of Class B2 immigrants were considered candidates for preventive therapy (9). Limited information exists concerning the practices of health departments in pursuit of preventive therapy for these groups because, to date, no systematic studies have been conducted on the subject. Applicants already in the United States must be screened and found free of infectious TB before they can adjust their immigration status. Screening must be performed by physicians designated as "civil surgeons" by the U.S. Department of Justice/Immigration and Naturalization Service (INS). The procedure consists of an initial tuberculin skin test. If the reaction size is greater than or equal to 5 mm, a chest radiograph is required. Persons whose results are compatible with TB must be referred to a health department for treatment. Referral for possible preventive therapy also is recommended for persons with skin-test reactions of greater than or equal to 10 mm. In contrast to the overseas program, less data are available regarding the yield of the U.S. screening program. One program in Denver -- where the health department physician was the INS-appointed civil surgeon performing TB examinations -- detected an active TB rate of 40/100,000, which was similar to the rate in the country of origin for most of those tested. The study also identified several candidates for preventive therapy for whom the completion rate was higher than for candidates identified by other means (10). The number of foreign-born persons who are screened and treated for TB infection through mechanisms other than formal immigration processes is not known. Contact tracing, an important component of the U.S. strategy for TB control, is a possible case-finding mechanism. However, limited information is available on the usefulness of this approach in identifying either persons suspected of having TB or persons who are at high risk for preventive therapy among the foreign born. A study in Seattle documented that the yield for both the number of contacts and the number of tuberculin-skin-test-positive contacts was higher among the foreign born than among the U.S. born in the area, but the study population was too small to assess the usefulness of contact tracing as a case-finding tool among the foreign born (9). TB-control programs have tried to identify foreign-born preventive-therapy candidates through several other means, including screening migrant farm laborers, school entrants, and participants in English-as-a-second-language (ESL) programs. However, few of these efforts have been evaluated to assess the potential yield. Efforts to provide screening and preventive therapy for the foreign born are limited. Averting future cases of TB requires linking screening programs to prevention services. However, few resources are available to health departments for large-scale prevention efforts for foreign-born persons. Also, persons who do not consider themselves ill and who are from countries where TB is regarded as a stigma might be reluctant to begin or complete preventive therapy (11). TB-control programs in the United States also must strive to overcome perceptions about tuberculin-skin-test results among persons who have been vaccinated previously against TB. Many countries vaccinate infants with BCG (live attenuated vaccine) as part of their TB-control programs. For those persons, tuberculin sensitivity is highly variable and depends on the strain of BCG used, the population vaccinated, and the recency of vaccination because reactivity wanes over time (12). Moreover, no reliable method exists to distinguish tuberculin reactions caused by BCG from those caused by natural infections. Thus, some U.S. health-care providers are reluctant to perform tuberculin skin tests on foreign-born patients with previous BCG vaccinations because they think that substantial reactions are likely to be falsely positive. Screening programs also are hindered by the unknown role of environmental mycobacteria in other parts of the world in producing false-positive reactions and by the cultural barriers to providing services to persons who do not consider themselves ill and who are from countries where TB is regarded as a stigma. Finally, the high levels of isoniazid (INH) resistance in many countries of origin raise questions about the usefulness of INH preventive therapy among foreign-born populations. TB Diagnosis Data regarding the timeliness of TB diagnosis after the onset of symptoms are not routinely collected for either U.S.- or foreign-born populations. Compared with U.S.-born patients, a higher percentage of foreign-born patients have extrapulmonary TB only. Among foreign-born patients with pulmonary TB, the percentage diagnosed on clinical criteria alone is higher than among U.S.-born patients (14% versus 10%) (13). Drug Resistance Drug-resistance rates are higher among foreign-born populations than among the U.S. born. In a recent study of drug resistance based on national TB surveillance data for 1993-1996, levels of INH resistance were higher among TB patients born in Vietnam (18.3%), the Philippines (14.7%), and Mexico (9.8%) than among U.S.-born TB patients (6.4%) (14). Levels of resistance to INH and rifampin for the three groups were 2.1%, 2.1%, and 1.9%, respectively, which is similar to the rate of 2.0% for those born in the United States. Among foreign-born TB patients from the three countries, resistance levels were higher in new arrivals than in long-term residents. TB Treatment Outcomes The outcome of TB treatment is slightly better for foreign-born patients than for U.S.-born patients (15). Among the foreign-born community, levels of completion vary by country of origin, but among all the major immigrant groups, completion rates equal or exceed those of TB cases among U.S.-born patients. TB-HIV Coinfection In the United States, HIV has not played a major role in TB cases among foreign-born persons in most areas. The only exception is persons from Haiti. Recent studies conducted in southern Florida indicated that half of the Haitians infected with TB among those aged 25-44 years were also HIV positive (16). The low incidence of HIV among foreign-born persons with TB might be partly attributable to the U.S. law prohibiting persons with HIV infection from applying for overseas immigration (17). Also, injecting-drug use has not emerged as a major problem among the foreign-born population. However, areas (e.g., San Diego) that are experiencing increasing drug use among the foreign born have noted a corresponding increase in HIV prevalence among foreign-born TB patients in recent years (personal communication, Kathleen Moser, M.D., M.P.H., San Diego Department of Health, May 1997). OVERVIEW OF THE WORKING GROUPS REPORT Given the issues outlined previously, the Working Group on Tuberculosis Among the Foreign Born was responsible for a) delineating the most important policy and programmatic needs related to TB among foreign-born persons and b) providing recommendations for action by CDC and other federal agencies, health departments, community-based organizations (CBOs), and private health-care providers to enhance control efforts. The group's deliberations centered on five topics --
The remainder of this report is organized around these topics, with discussion of key issues related to each, followed by the recommendations of the Working Group. DEVELOPING EPIDEMIOLOGIC PROFILES OF TB CASES AMONG FOREIGN-BORN PERSONS Issues Because the characteristics of foreign-born populations and TB cases among the foreign born differ among public health jurisdictions in the United States, TB-control efforts must be tailored to meet local needs. These efforts require developing detailed epidemiologic profiles of TB cases among the foreign born. TB-control program staff need to know the characteristics and outcomes of foreign-born patients with TB in their jurisdictions. They also need information on sources of medical care in communities of the foreign born, care-seeking behaviors, delays in seeking care, community organizations or structures with access to specific foreign-born populations, sources of interpreter services, and sources of culturally appropriate health information. Recommendations for Developing Epidemiologic Profiles of TB Cases Among Foreign-Born Persons CDC
Health Departments and TB-Control Programs
CASE FINDING, SCREENING, AND PREVENTIVE THERAPY Case Finding and Contact Tracing Issues Active case finding can help identify cases of TB among foreign-born persons whose access to health-care services might be more limited than that of persons born in the United States. However, the yield of such case-finding efforts is influenced by the following factors:
Other factors, (e.g., return travel to the country of origin, HIV status, living conditions, and family constellation) also can affect contact tracing. All of these factors need to be considered in deciding which groups, if any, should be the target of active case-finding efforts. Contact tracing is one form of active case finding and is an important component of TB-control efforts in the United States, regardless of a patient's country of origin. Although the intent and methods of contact tracing for foreign-born persons do not differ substantially from those for persons born in the United States, contact investigations among foreign-born persons might have different dynamics. For example, determining if transmission has occurred among "close" household contacts can be difficult because of the high background prevalence of positive tuberculin reactions. Expanding the contact investigation to those other than close household contacts requires additional time, effort, and resources. Recommendations for Case Finding and Contact Tracing CDC
Health Departments and TB-Control Programs
Priority 1 -- Immigrants with Class A TB. Health departments should ensure that these patients are located, evaluated, and treated appropriately. Priority 2 -- Immigrants with Class B1 or B2 TB. Currently, no federal regulations exist that prescribe follow-up procedures for those who have suspicious chest radiographs but negative sputum smears, although those persons are reported to state health departments by federal authorities. The number who are actually evaluated nationally is unknown, but in health departments where assessments have been made, the percentage has been reported to range from 63% to approximately 95% (8). Each state and local TB-control program should therefore have an active process to ensure that all Class B1 and B2 immigrants are located, evaluated, and treated appropriately. Programs should develop a notification process (e.g., timely transfer of Class B1 and B2 forms to the health department with a prescribed "window" for action). Priority 3 -- Other Groups at High Risk. The next priority should be older immigrants (especially those aged greater than 55 years), immigrants from countries with high rates of TB, immigrants from high-risk areas who have been in the United States less than 5 years, and/or other groups that are "producing" cases, as documented in the epidemiologic profile.
Providers
Screening and Preventive Therapy Issues A substantial number of foreign-born persons are from countries where the prevalence of TB is many times higher than that reported for the United States. CDC estimates that at least 7 million foreign-born persons in the United States are infected with TB and that 140,000-210,000 (2%-3%) will develop disease after immigration unless they complete a regimen of preventive treatment. Screening and providing preventive therapy to foreign-born persons are hindered by the large number of persons to be screened, difficulties in diagnosis, difficulties in gaining access to persons who should be screened, cultural and linguistic barriers, and the perceived difficulty in interpreting tuberculin skin tests among persons who have received BCG vaccine. In health departments already serving large numbers of TB patients, efforts to initiate large-scale screening programs to identify additional foreign-born persons with TB infection might be impeded by insufficient resources to ensure completion of preventive therapy. As of the publication of this report, data are scarce regarding the rate of completion of preventive therapy among foreign-born persons with TB infection. Lack of data thwarts efforts to evaluate the cost-effectiveness of screening and prevention programs or to measure or predict the impact of DOPT on completion rates, the impact of directly observed therapy (DOT) for index cases on the preventive therapy completion rates of their contacts, or the impact of more extensive screening programs. Data are also lacking on the contribution of civil surgeons in identifying candidates for preventive therapy, providing preventive therapy to foreign-born patients, and referring patients to local health departments for evaluation. Some physicians do not place tuberculin-reactive foreign-born patients on preventive therapy because the physicians attribute positive skin-test results to prior BCG vaccination. Some foreign-born candidates might not be started on preventive therapy because physicians find difficulty in convincing patients of the value of this health intervention (18). Physicians and patients have concerns about potential adverse effects or toxicity associated with preventive therapy. Recommendations for Screening and Preventive Therapy CDC Screening --
Completion of Preventive Therapy --
Health Departments and TB-Control Programs Screening --
Completion of Preventive Therapy --
DIAGNOSING AND MANAGING TB Recognizing TB Issues In their pursuit of health care in the United States, foreign-born persons encounter many barriers that can impede the recognition of TB (e.g., language and cultural differences, which hinder communication between foreign-born patients and health-care providers). Moreover, many foreign-born patients are unaware of how to gain access to the health-care system. Even when they access health care, they often are ineligible for employee-based health insurance or Medicaid and cannot afford to purchase private insurance. Attitudes and behaviors can pose other impediments to the recognition of disease among the foreign born. Because of the social stigma of TB or cultural beliefs about disease causation, progression, and treatment, some foreign-born persons might deny the presence of symptoms or known disease. They might delay seeking care even when illness is recognized because of other priorities in their lives (e.g., securing food and shelter, job responsibilities, and family concerns). Undocumented persons (e.g., illegal border crossers and visa "over-stayers") might delay diagnosis and treatment because of fear of detection and possible deportation. Delays can result in diagnosis of disease at more advanced stages, which translates into the possible need for hospitalization and more expensive care, as well as prolonged periods of infectiousness and a greater likelihood of disease transmission. Medical providers and laboratories also can impede or delay disease recognition. Foreign-born patients might seek care from medical providers who are not fully aware of, or up-to-date on, the latest CDC and ATS guidelines for TB diagnosis and treatment. Persons of foreign origin who enter the country on nonimmigrant visas create specific problems. Unlike immigrants and refugees, nonimmigrant business persons, students, and dependents are not required to be medically evaluated for TB before entering the country. If they later want to adjust their immigration status to that of legal permanent resident while remaining in the United States, they are required to be screened by a civil surgeon designated by INS. Civil surgeons have valid U.S. medical licenses but have no other TB-related educational or training requirements and receive no postdesignation monitoring or required continuing education. In most areas of the country, a lack of coordination and communication exists between civil surgeons and state and local health departments. Recommendations for Recognizing TB CDC
Health Departments and TB-Control Programs
Completing Treatment Issues Problems related to completion of treatment center on nonadherence, inadequate tracking systems, information gaps, and drug resistance. Nonadherence to treatment is a major problem in TB-control programs worldwide. Adherence is impeded by the same cultural and economic barriers that hinder timely diagnosis of disease among foreign-born persons. Tracking and communication networks also are inadequate. Some foreign-born persons (e.g., migrant and seasonal farm workers) are very mobile and move among countries and states and across the U.S.-Mexico border while under treatment. Completion of treatment in these cases is impeded by the lack of efficient tracking and referral systems. Similarly, foreign-born patients sometimes return to their country of origin before completion of treatment, with no follow-up of care. Essentially no communication exists between TB controllers in the United States and their counterparts in foreign countries, with the exception of the U.S.-Mexico border region where lines of communication are being established. TB treatment is also hindered by gaps in information. U.S. health-care providers have little information on current medical guidelines for TB treatment and diagnosis in the developing world. Even U.S. TB controllers are not knowledgeable about the screening procedures and treatment regimens used in the countries of origin for many of their foreign-born patients. In addition, scant program data are available on the common barriers to adherence affecting foreign-born subpopulations in the United States and even less on the unique problems related to adherence among specific groups within foreign-born subpopulations. Although data regarding completion of treatment are collected via the national RVCT system, the data have not been analyzed by subpopulation or region to help define the scope and magnitude of adherence issues among the foreign born. Foreign-born patients who were treated in their home countries pose special problems. U.S. physicians who treat foreign-born persons with TB are rarely able to obtain medical records from countries where the patients were treated previously. If the records are available, the medical information is likely to be in an unfamiliar language or format. National TB-control program reports from countries that are sources of large numbers of TB cases among the foreign born often lack reliable data regarding rates of relapse, drug resistance, and completion of therapy. Finally, because resources and infrastructure for TB-control programs are severely limited in many foreign countries, persons treated for TB in these countries might receive inadequate or incomplete treatment. This puts foreign-born persons at greater risk for disease recurrence with drug-resistant strains, which complicates and lengthens the course of treatment. Some persons with multiple resistant strains are chronically ill and persistently infectious. Although the total number of these patients with treatment-resistant TB is small, the cost associated with their medical care is many times that of patients with drug-susceptible disease. Treating these patients can severely strain local health department resources, especially because foreign-born populations are disproportionately underinsured or uninsured. Recommendations for Completing Treatment CDC
Health Departments and TB-Control Programs
COLLABORATING WITH CBOs Issues CBOs and health departments can be strong partners in efforts to prevent and control TB among foreign-born persons who are at high risk for the disease. However, in many communities, health departments and relevant CBOs have little or no contact and thus lose opportunities to maximize their effectiveness. Also, many health-service CBOs have limited understanding of TB-related issues and often are unable or unwilling to provide screening and preventive therapy. Recommendations for Collaborating with CBOs Health Departments and TB-Control Programs
TRAINING NEEDS Issues Some problems associated with TB among the foreign born stem from communication barriers, cultural and cognitive dissonance between providers and patients, and gaps in provider training. Foreign-born patients might not know how to gain access to the health-care system. Providing TB prevention and control services to foreign-born persons might be impeded by linguistic, ethnic, cultural, socioeconomic, or other differences between patients and health workers. Foreign-born health-care providers might be uninformed about the latest U.S. recommendations and practices related to TB and, thus, be unable to provide optimal diagnostic services, preventive therapy, and management to the foreign born. TB-related training and educational efforts to support and strengthen TB-control activities need to be linked closely to the overall TB-control strategies for the foreign born. When foreign-born populations are identified and health-care providers for these populations are defined, training efforts can be developed and implemented. Education should be targeted to providers, patients, and community workers. Recommendations for Training Needs Health Departments and TB-Control Programs
CONCLUSION This report presents a plan for federal, state, and local TB-control programs to address TB among the foreign-born population residing in the United States. Not all TB-control programs will have the resources to implement all aspects of this plan, and some TB-control programs will not have the same issues identified in this report. However, these recommendations can provide assistance in identifying programmatic gaps and in establishing priories for a TB-control and prevention plan that will yield the greatest positive results for foreign-born persons. References
* CDC funds three model TB centers -- San Francisco's Francis J. Curry National TB Center; New York City's Charles P. Felton National TB Center at Harlem Hospital; and Newark's New Jersey Medical School National TB Center. These model centers provide comprehensive and coordinated state-of-the-art diagnostic, treatment, prevention, and patient education services for those persons infected with TB, those suspected of being infected, their contacts, and other persons at risk for TB.
** Sponsored by the University of Washington's Harborview Medical
Center in Seattle, EthnoMed is a database containing medical and
cultural information about refugee groups (Internet website,
Table_1 Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size.
TABLE 1. Tuberculosis cases among U.S.- and foreign-born persons -- United States, 1997
==========================================================================================================
U.S.-born Foreign-born
persons persons* Unknown
--------------- --------------- --------------
State Total cases No. % No. % No. %
----------------------------------------------------------------------------------------------------------
United States 19,851 11,898 59.9 7,702 38.8 251 1.3
Alabama 405 384 94.8 21 5.2 0 0
Alaska 78 60 76.9 18 23.1 0 0
Arizona 296 185 62.5 109 36.8 2 0.7
Arkansas 200 182 91.0 16 8.0 2 1.0
California 4,056 1,243 30.6 2,795 68.9 18 0.4
Colorado 94 43 45.7 48 51.1 3 3.2
Connecticut 128 74 57.8 54 42.2 0 0
Delaware 39 26 66.7 13 33.3 0 0
District of Columbia 110 86 78.2 17 15.5 7 6.4
Florida 1,400 988 70.6 408 29.1 4 0.3
Georgia 696 570 81.9 115 16.5 11 1.6
Hawaii 167 41 24.6 126 75.4 0 0
Idaho 15 6 40.0 9 60.0 0 0
Illinois 974 727 74.6 223 22.9 24 2.5
Indiana 168 143 85.1 24 14.3 1 0.6
Iowa 74 37 50.0 34 45.9 3 4.1
Kansas 78 42 53.8 23 29.5 13 16.7
Kentucky 198 184 92.9 14 7.1 0 0
Louisiana 406 380 93.6 23 5.7 3 0.7
Maine 21 16 76.2 5 23.8 0 0
Maryland 340 208 61.2 132 38.8 0 0
Massachusetts 268 83 31.0 185 69.0 0 0
Michigan 374 320 85.6 54 14.4 0 0
Minnesota 161 46 28.6 114 70.8 1 0.6
Mississippi 245 235 95.9 10 4.1 0 0
Missouri 248 197 79.4 51 20.6 0 0
Montana 18 15 83.3 3 16.7 0 0
Nebraska 22 11 50.0 11 50.0 0 0
Nevada 112 56 50.0 56 50.0 0 0
New Hampshire 17 8 47.1 9 52.9 0 0
New Jersey 718 379 52.8 339 47.2 0 0
New Mexico 71 51 71.8 20 28.2 0 0
New York 2,265 1,119 49.4 1,146 50.6 0 0
North Carolina 463 393 84.9 70 15.1 0 0
North Dakota 12 7 58.3 5 41.7 0 0
Ohio 286 226 79.0 59 20.6 1 0.3
Oklahoma 212 169 79.7 28 13.2 15 7.1
Oregon 161 94 58.4 67 41.6 0 0
Pennsylvania 528 399 75.6 123 23.3 6 1.1
Rhode Island 38 13 34.2 23 60.5 2 5.3
South Carolina 328 308 93.9 20 6.1 0 0
South Dakota 19 18 94.7 1 5.3 0 0
Tennessee 467 423 90.6 43 9.2 1 0.2
Texas 1,992 1,234 61.9 626 31.4 132 6.6
Utah 36 16 44.4 20 55.6 0 0
Vermont 6 4 66.7 2 33.3 0 0
Virginia 350 205 58.6 143 40.9 2 0.6
Washington 305 114 37.4 191 62.6 0 0
West Virginia 54 51 94.4 3 5.6 0 0
Wisconsin 130 78 60.0 52 40.0 0 0
Wyoming 2 1 50.0 1 50.0 0 0
----------------------------------------------------------------------------------------------------------
* Persons born outside the United States, American Samoa, Federated States of Micronesia,
Guam, Marshall Islands, Midway Island, Northern Mariana Islands, Puerto Rico, Republic of
Palau, U.S. Minor Outlying Islands, U.S. Miscellaneous Pacific Islands, and U.S. Virgin Islands.
Source: CDC. Reported tuberculosis in the United States, 1997. Atlanta, GA: US Department of
Health and Human Services, CDC National Center for HIV, STD, and TB Prevention, July 1998.
==========================================================================================================
Return to top. Figure_1 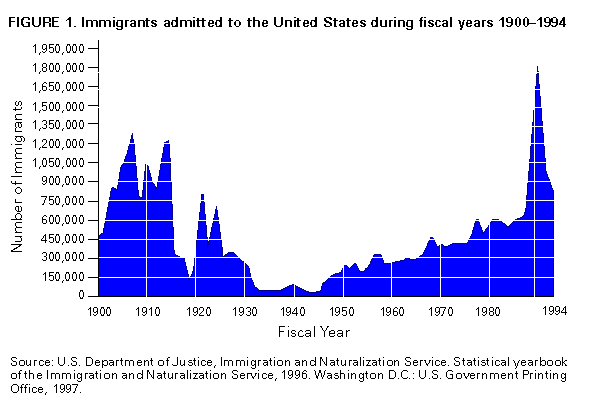 Return to top. Figure_2 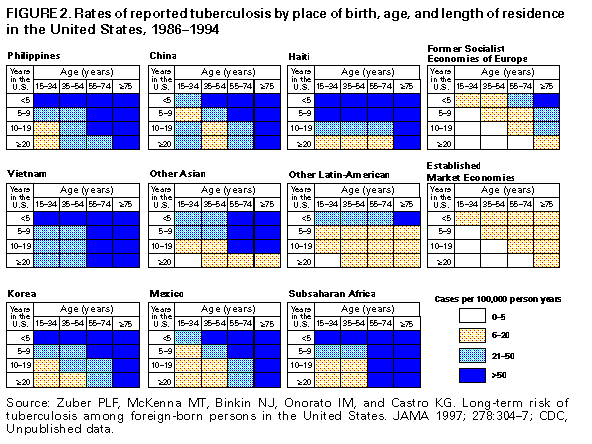 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/05/98 |
|||||||||
This page last reviewed 5/2/01
|