 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Unintentional Non--Fire-Related Carbon Monoxide Exposures --- United States, 2001--2003Carbon monoxide (CO) is a colorless, odorless, poisonous gas that results from incomplete combustion of fuels (e.g., natural or liquefied petroleum gas, oil, wood, coal, or other fuels). CO sources (e.g., furnaces, generators, gas heaters, and motor vehicles) are common in homes or work environments and can put persons at risk for CO exposure and poisoning. Most signs and symptoms of CO exposure are nonspecific (e.g., headache or nausea) and can be mistakenly attributed to other causes, such as viral illnesses. Undetected or unsuspected CO exposure can result in death (1). To examine fatal and nonfatal unintentional, non--fire-related CO exposures, CDC analyzed 2001--2003 data on emergency department (ED) visits from the National Electronic Injury Surveillance System All Injury Program (NEISS-AIP) and 2001--2002 death certificate data from the National Vital Statistics System (NVSS). During 2001--2003, an estimated 15,200 persons with confirmed or possible non--fire-related CO exposure were treated annually in hospital EDs. In addition, during 2001--2002, an average of 480 persons died annually from non--fire-related CO poisoning. Although males and females were equally likely to visit an ED for CO exposure, males were 2.3 times more likely to die from CO poisoning. Most (64%) of the nonfatal CO exposures occurred in homes. Efforts are needed to educate the public about preventing CO exposure. NEISS-AIP is operated by the U.S. Consumer Product Safety Commission and collects data regarding initial ED visits for all types and causes of injuries (2). Data are drawn from a nationally representative subsample of 66 of 100 NEISS hospitals that were selected as a stratified probability sample of hospitals in the United States and its territories. NEISS-AIP provides data on approximately 500,000 injury-related and consumer-product--related ED cases each year. Nonfatal cases were defined as those recorded at an NEISS-AIP hospital as CO exposure or CO poisoning. An incident was identified as a case if 1) the intent of injury was unintentional or undetermined, 2) the principal diagnosis by a physician was "poisoning" or "anoxia," and 3) the consumer product indicated was "CO detector" or "CO poisoning (source unknown)" or a brief narrative abstracted from the medical record indicated either CO exposure or CO poisoning. Fire-related (i.e., burn and smoke inhalation) cases were excluded. In addition, because death data are not captured completely by NEISS-AIP, persons who were dead on arrival or who died in the ED also were excluded. Data for all cases were reviewed independently by two CDC epidemiologists to confirm they met the case criteria. Narratives were also reviewed to determine CO source, exposure status (on the basis of physician diagnosis), and symptoms reported. Each case was assigned a sample weight on the basis of the inverse of the probability of selection; these weights were summed to provide national estimates of nonfatal CO exposures. Estimates were based on weighted data for 778 patients with confirmed or possible CO exposure treated at NEISS-AIP hospital EDs during 2001--2003. Three years of data were necessary to provide stable rates. Confidence intervals (CIs) were calculated by using a direct variance estimation procedure that accounted for the sample weights and complex sample design. Because CO source and symptoms were undetermined for a high percentage of cases, data on these factors were based on unweighted data for NEISS-AIP cases and thus are not nationally representative. Death certificate data were obtained from NVSS (3). Using multiple-cause-of-death files from the National Center for Health Statistics (NCHS) (3), CO poisoning deaths were defined as those with any mention on the death certificate of International Classification of Diseases, Tenth Revision (ICD-10) code T58 ("Toxic effect of carbon monoxide") as a leading or contributing cause of death and an ICD-10 underlying-cause-of-death code of X47 ("Accidental poisoning by and exposure to other gases or vapors") or Y17 ("Poisoning by and exposure to other gases or vapors, undetermined intent"). NVSS is a complete census of all deaths and therefore is not subject to sampling error; however, CIs were calculated to account for random error (3). The case-fatality rate (CFR) was calculated as the number of CO deaths divided by the sum of CO deaths and nonfatal CO exposures multiplied by 100. Rates were calculated by using 2001--2003 U.S. census bridged-race population estimates from NCHS (4). During 2001--2003, an estimated 15,200 persons were treated annually in EDs for nonfatal, unintentional, non--fire-related CO exposure, and, during 2001--2002, an average of 480 persons died each year from unintentional, non--fire-related CO exposure (Table 1). The nonfatal rate for CO exposure was highest for children aged <4 years (8.2 per 100,000 population), whereas the CO death rate was highest for adults aged >65 years (0.32). Adults aged >65 years accounted for 23.5% of CO poisoning deaths. The nonfatal rate was similar for males and females; in contrast, the death rate for males was 2.7 times that for females. The CFR increased with age, from 0.6% for children aged <4 years to 5.5% for adults aged 55--64 years; also, the CFR for males was 2.3 times that for females. The death rate was highest for non-Hispanic whites and blacks (0.17 per 100,000). Eleven percent of those treated in EDs were either hospitalized or transferred to another hospital for specialized care. The annualized incidence of fatal and nonfatal CO exposures occurred more often during the fall and winter months, with the highest numbers occurring during December (56 fatal and 2,157 nonfatal exposures) and January (69 fatal and 2,511 nonfatal exposures). The annualized incidence was substantially lower during the summer months, with 21 fatal and 510 nonfatal exposures occurring during June and 22 fatal and 524 nonfatal exposures occurring during July. The majority (64.3%) of nonfatal CO exposures were reported to occur in homes; 21.4% occurred in public facilities and areas. Narratives abstracted from the medical records of NEISS-AIP cases indicated that 18.5% of CO exposure incidents were associated with faulty furnaces (Table 2). An additional 9% were associated with motor vehicles. CO poisonings were diagnosed in approximately half of the NEISS-AIP cases, of which 73% had symptoms noted in the medical record (Table 2). The most common symptoms experienced were headache (37.5%), dizziness (18.0%), and nausea (17.3%). Severer symptoms were reported less often, including loss of consciousness (7.7%), shortness of breath (6.7%), and loss of muscle control (3.5%). According to medical records, 9.3% of patients in the NEISS-AIP sample reported that they had a CO detector at home, and 100% of those indicated that the detector had alerted them to the presence of CO. Reported by: M Vajani, MPH, JL Annest, PhD, Office of Statistics and Programming; M Ballesteros, PhD, J Gilchrist, MD, Div of Unintentional Injury Prevention, National Center for Injury Prevention and Control; A Stock, PhD, Div of Environmental Hazards and Health Effects, National Center for Environmental Health, CDC. Editorial Note:Data in this report indicate that, each year, approximately 15,000 U.S. residents visit EDs for unintentional, non--fire-related CO exposure and approximately 500 die from unintentional, non--fire-related CO poisoning. Primary CO sources were home appliances, and the majority of exposures occurred during the fall and winter months, when persons are more likely to use gas furnaces and heaters. During warmer months, boating activities might also be a source of exposure (5). This analysis also determined that males are more likely to die from CO poisoning than females, which is consistent with previous findings (6--8). Males might be exposed to higher CO levels during high-risk activities, such as working indoors or in enclosed garages with combustion-engine--driven tools (e.g., generators or power washers) (7). The CO poisoning death rate was highest among persons aged >65 years, likely attributable to their being at higher risk for undetected CO exposure because symptoms often resemble those associated with other health conditions common among older persons (9). The findings in this report are subject to at least three limitations. First, data on sources of CO exposure and symptoms of persons with CO poisoning were missing for a substantial percentage of cases. Second, national estimates of nonfatal injuries are based solely on persons treated in EDs and do not include those treated in outpatient settings or not treated at all. Finally, although risks for CO exposure vary by state and locality (e.g., because of differences in winter weather conditions), NEISS-AIP provides only national estimates and not state or local estimates. Primary prevention of residential CO exposure can be accomplished through simple precautions (Box). Although residential CO detectors are important for early detection of CO, they should be considered a secondary prevention method. High oil and gas prices and power outages during winter months can contribute to consumer use of improperly vented heating sources. Public education campaigns, especially during winter months, combined with provision of battery-operated CO detectors for low-income persons, might reduce CO poisonings (10). Previous studies also suggest a need for multilingual educational campaigns to reach non--English-speaking populations (10). Acknowledgments This report is based on data contributed by T Schroeder, MS, C Irish, and other staff members, Div of Hazard and Injury Data Systems, US Consumer Product Safety Commission. References
Table 1 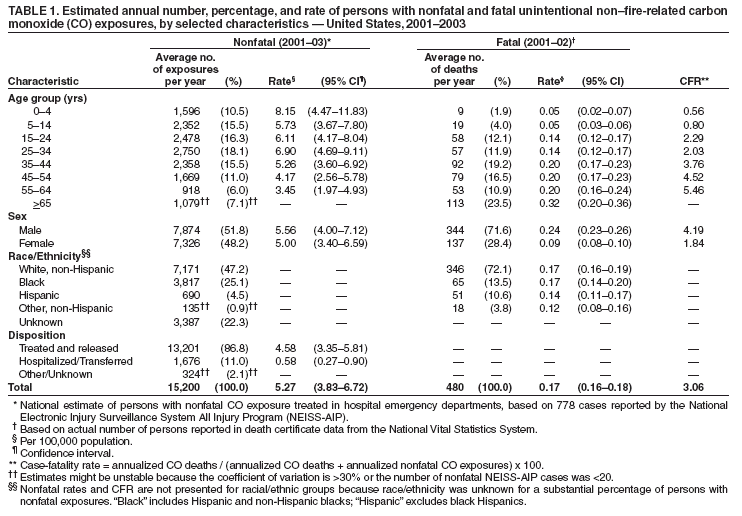 Return to top. Table 2  Return to top. Box  Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 1/20/2005 |
|||||||||
This page last reviewed 1/20/2005
|