 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Achievements in Public Health, 1900-1999: Control of Infectious DiseasesDeaths from infectious diseases have declined markedly in the United States during the 20th century (Figure 1). This decline contributed to a sharp drop in infant and child mortality (1,2) and to the 29.2-year increase in life expectancy (2). In 1900, 30.4% of all deaths occurred among children aged less than 5 years; in 1997, that percentage was only 1.4%. In 1900, the three leading causes of death were pneumonia, tuberculosis (TB), and diarrhea and enteritis, which (together with diphtheria) caused one third of all deaths (Figure 2). Of these deaths, 40% were among children aged less than 5 years (1). In 1997, heart disease and cancers accounted for 54.7% of all deaths, with 4.5% attributable to pneumonia, influenza, and human immunodeficiency virus (HIV) infection (2). Despite this overall progress, one of the most devastating epidemics in human history occurred during the 20th century: the 1918 influenza pandemic that resulted in 20 million deaths, including 500,000 in the United States, in less than 1 year--more than have died in as short a time during any war or famine in the world (3). HIV infection, first recognized in 1981, has caused a pandemic that is still in progress, affecting 33 million people and causing an estimated 13.9 million deaths (4). These episodes illustrate the volatility of infectious disease death rates and the unpredictability of disease emergence. Public health action to control infectious diseases in the 20th century is based on the 19th century discovery of microorganisms as the cause of many serious diseases (e.g., cholera and TB). Disease control resulted from improvements in sanitation and hygiene, the discovery of antibiotics, and the implementation of universal childhood vaccination programs. Scientific and technologic advances played a major role in each of these areas and are the foundation for today's disease surveillance and control systems. Scientific findings also have contributed to a new understanding of the evolving relation between humans and microbes (5). CONTROL OF INFECTIOUS DISEASES Sanitation and Hygiene The 19th century shift in population from country to city that accompanied industrialization and immigration led to overcrowding in poor housing served by inadequate or nonexistent public water supplies and waste-disposal systems. These conditions resulted in repeated outbreaks of cholera, dysentery, TB, typhoid fever, influenza, yellow fever, and malaria. By 1900, however, the incidence of many of these diseases had begun to decline because of public health improvements, implementation of which continued into the 20th century. Local, state, and federal efforts to improve sanitation and hygiene reinforced the concept of collective "public health" action (e.g., to prevent infection by providing clean drinking water). By 1900, 40 of the 45 states had established health departments. The first county health departments were established in 1908 (6). From the 1930s through the 1950s, state and local health departments made substantial progress in disease prevention activities, including sewage disposal, water treatment, food safety, organized solid waste disposal, and public education about hygienic practices (e.g., foodhandling and handwashing). Chlorination and other treatments of drinking water began in the early 1900s and became widespread public health practices, further decreasing the incidence of waterborne diseases. The incidence of TB also declined as improvements in housing reduced crowding and TB-control programs were initiated. In 1900, 194 of every 100,000 U.S. residents died from TB; most were residents of urban areas. In 1940 (before the introduction of antibiotic therapy), TB remained a leading cause of death, but the crude death rate had decreased to 46 per 100,000 persons (7). Animal and pest control also contributed to disease reduction. Nationally sponsored, state-coordinated vaccination and animal-control programs eliminated dog-to-dog transmission of rabies. Malaria, once endemic throughout the southeastern United States, was reduced to negligible levels by the late 1940s; regional mosquito-control programs played an important role in these efforts. Plague also diminished; the U.S. Marine Hospital Service (which later became the Public Health Service) led quarantine and ship inspection activities and rodent and vector-control operations. The last major rat-associated outbreak of plague in the United States occurred during 1924-1925 in Los Angeles. This outbreak included the last identified instance of human-to-human transmission of plague (through inhalation of infectious respiratory droplets from coughing patients) in this country. Vaccination Strategic vaccination campaigns have virtually eliminated diseases that previously were common in the United States, including diphtheria, tetanus, poliomyelitis, smallpox, measles, mumps, rubella, and Haemophilus influenzae type b meningitis (8). With the licensure of the combined diphtheria and tetanus toxoids and pertussis vaccine in 1949, state and local health departments instituted vaccination programs, aimed primarily at poor children. In 1955, the introduction of the Salk poliovirus vaccine led to federal funding of state and local childhood vaccination programs. In 1962, a federally coordinated vaccination program was established through the passage of the Vaccination Assistance Act--landmark legislation that has been renewed continuously and now supports the purchase and administration of a full range of childhood vaccines. The success of vaccination programs in the United States and Europe inspired the 20th-century concept of "disease eradication"--the idea that a selected disease could be eradicated from all human populations through global cooperation. In 1977, after a decade-long campaign involving 33 nations, smallpox was eradicated worldwide--approximately a decade after it had been eliminated from the United States and the rest of the Western Hemisphere. Polio and dracunculiasis may be eradicated by 2000. Antibiotics and Other Antimicrobial Medicines Penicillin was developed into a widely available medical product that provided quick and complete treatment of previously incurable bacterial illnesses, with a wider range of targets and fewer side effects than sulfa drugs. Discovered fortuitously in 1928, penicillin was not developed for medical use until the 1940s, when it was produced in substantial quantities and used by the U.S. military to treat sick and wounded soldiers. Antibiotics have been in civilian use for 57 years (see box 1) and have saved the lives of persons with streptococcal and staphylococcal infections, gonorrhea, syphilis, and other infections. Drugs also have been developed to treat viral diseases (e.g., herpes and HIV infection); fungal diseases (e.g., candidiasis and histoplasmosis); and parasitic diseases (e.g., malaria). The microbiologist Selman Waksman led much of the early research in discovering antibiotics (see box 2). However, the emergence of drug resistance in many organisms is reversing some of the therapeutic miracles of the last 50 years and underscores the importance of disease prevention. TECHNOLOGIC ADVANCES IN DETECTING AND MONITORING INFECTIOUS DISEASES Technologic changes that increased capacity for detecting, diagnosing, and monitoring infectious diseases included development early in the century of serologic testing and more recently the development of molecular assays based on nucleic acid and antibody probes. The use of computers and electronic forms of communication enhanced the ability to gather, analyze, and disseminate disease surveillance data. Serologic Testing Serologic testing came into use in the 1910s and has become a basic tool to diagnose and control many infectious diseases. Syphilis and gonorrhea, for example, were widespread early in the century and were difficult to diagnose, especially during the latent stages. The advent of serologic testing for syphilis helped provide a more accurate description of this public health problem and facilitated diagnosis of infection. For example, in New York City, serologic testing in 1901 indicated that 5%-19% of all men had syphilitic infections (9). Viral Isolation and Tissue Culture The first virus isolation techniques came into use at the turn of the century. They involved straining infected material through successively smaller sieves and inoculating test animals or plants to show the purified substance retained disease-causing activity. The first "filtered" viruses were tobacco mosaic virus (1882) and foot-and-mouth disease virus of cattle (1898). The U.S. Army Command under Walter Reed filtered yellow fever virus in 1900. The subsequent development of cell culture in the 1930s paved the way for large-scale production of live or heat-killed viral vaccines. Negative staining techniques for visualizing viruses under the electron microscope were available by the early 1960s. Molecular Techniques During the last quarter of the 20th century, molecular biology has provided powerful new tools to detect and characterize infectious pathogens. The use of nucleic acid hybridization and sequencing techniques has made it possible to characterize the causative agents of previously unknown diseases (e.g., hepatitis C, human ehrlichiosis, hantavirus pulmonary syndrome, acquired immunodeficiency syndrome [AIDS], and Nipah virus disease). Molecular tools have enhanced capacity to track the transmission of new threats and find new ways to prevent and treat them. Had AIDS emerged 100 years ago, when laboratory-based diagnostic methods were in their infancy, the disease might have remained a mysterious syndrome for many decades. Moreover, the drugs used to treat HIV-infected persons and prevent perinatal transmission (e.g., replication analogs and protease inhibitors) were developed based on a modern understanding of retroviral replication at the molecular level. CHALLENGES FOR THE 21ST CENTURY Success in reducing morbidity and mortality from infectious diseases during the first three quarters of the 20th century led to complacency about the need for continued research into treatment and control of infectious microbes (10). However, the appearance of AIDS, the re-emergence of TB (including multidrug-resistant strains), and an overall increase in infectious disease mortality during the 1980s and early 1990s (Figure 1) provide additional evidence that as long as microbes can evolve, new diseases will appear. The emergence of new diseases underscores the importance of disease prevention through continual monitoring of underlying factors that may encourage the emergence or re-emergence of diseases. Molecular genetics has provided a new appreciation of the remarkable ability of microbes to evolve, adapt, and develop drug resistance in an unpredictable and dynamic fashion (see box 3). Resistance genes are transmitted from one bacterium to another on plasmids, and viruses evolve through replication errors and reassortment of gene segments and by jumping species barriers. Recent examples of microbial evolution include the emergence of a virulent strain of avian influenza in Hong Kong (1997-98); the multidrug-resistant W strain of M. tuberculosis in the United States in 1991 (11); and Staphylococcus aureus with reduced susceptibility to vancomycin in Japan in 1996 (12) and the United States in 1997 (13,14). For continued success in controlling infectious diseases, the U.S. public health system must prepare to address diverse challenges, including the emergence of new infectious diseases, the re-emergence of old diseases (sometimes in drug-resistant forms), large foodborne outbreaks, and acts of bioterrorism. Ongoing research on the possible role of infectious agents in causing or intensifying certain chronic diseases (including diabetes mellitus type 1, some cancers [15-17], and heart conditions [18,19 ]) also is imperative. Continued protection of health requires improved capacity for disease surveillance and outbreak response at the local, state, federal, and global levels; the development and dissemination of new laboratory and epidemiologic methods; continued antimicrobial and vaccine development; and ongoing research into environmental factors that facilitate disease emergence (20). Reported by: National Center for Environmental Health; National Center for Health Statistics; National Center for Infectious Diseases, CDC. References
Figure 1 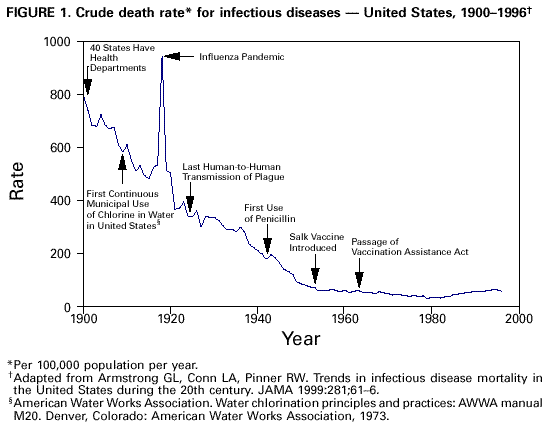 Return to top. Figure 2 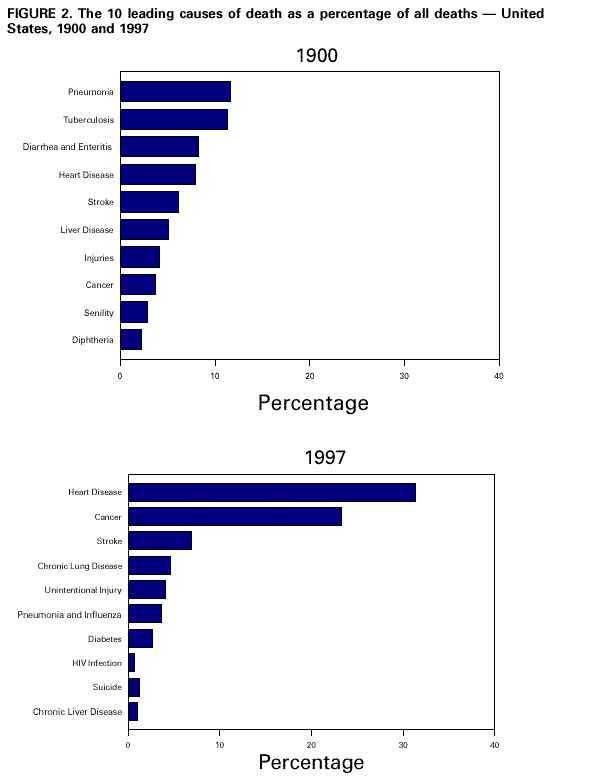 Return to top. Box 1
1. The First American Civilian Saved by Penicillin
The first U.S. civilian whose life was saved by penicillin died in June 1999 at the
age of 90 years. In March 1942, a 33-year-old woman was hospitalized for a month
with a life-threatening streptococcal infection at a New Haven, Connecticut, hospital.
She was delirious, and her temperature reached almost 107 F (41.6 C). Treatments
with sulfa drugs, blood transfusions, and surgery had no effect.
As a last resort, her doctors injected her with a tiny amount of an obscure experimental
drug called penicillin. Her hospital chart, now at the Smithsonian Institution,
indicates a sharp overnight drop in temperature; by the next day she was no
longer delirious. She survived to marry, raise a family, and meet Sir Alexander
Fleming, the scientist who discovered penicillin. In 1945, Fleming was awarded the
Nobel Prize in Physiology and Medicine, along with Ernst Chain and Howard Florey,
who helped develop penicillin into a widely available medical product.
Return to top. Box 2
2. Selman Abraham Waksman, Ph.D.
In 1943, Selman Abraham Waksman (July 22, 1888-August 16, 1973) led a team
of Rutgers University researchers that isolated streptomycin, the first antibiotic
effective against tuberculosis (TB) in humans. In 1952, Waksman received the Nobel
Prize for this discovery.
Waksman grew up in the small Russian village of Novaya Priluka. In 1910, he
settled in New Jersey, where a cousin operated a small farm. An interest in scientific
farming brought him to nearby Rutgers College of Agriculture, where he
earned a bachelor's degree in science in 1915 and a master's degree a year later. He
completed his doctorate at the University of California, Berkeley, in 2 years, and
returned to Rutgers to take a position as lecturer in soil microbiology.
Waksman preferred the term "microbiology" to the conventional "bacteriology"
because "not the bacteria but the fungi and the actinomycetes formed my major
interests among the microorganisms" (1). By the 1930s, he was a leading figure in
microbiology, attracting talented graduate students, including René‚ Dubos, whose
work led to the discovery in 1939 of gramicidin, the first clinically useful topical
antibiotic.
Dubos' success and the introduction of penicillin prompted Waksman to put his
graduate students and assistants to work looking for antibiotics. In 1943,
a Waksman student, Albert Schatz, isolated streptomycin. In 1944, clinical trials
demonstrated the drug's effectiveness against gram-negative bacteria including
Mycobacterium tuberculosis. Despite substantial problems with toxicity and drug
resistance, streptomycin soon formed the foundation of multidrug therapies for TB.
With the introduction and use of antibiotics, mortality of TB was reduced
drastically. In the United States, from 1945 to 1955, TB mortality decreased from
39.9 deaths per 100,000 population (2) to 9.1. Around the world, TB remained
(and remains) a substantial health problem, but until the emergence of multidrug-
resistant TB, many in the United States shared Waksman's optimism, expressed in
1964, that "the final chapter of the battle against tuberculosis appears to be at
hand" (3).
References
1. Waksman S. My life with the microbes. New York, New York: Simon and Schuster, 1954:100.
2. Groves RD, Hetzel AM. Vital statistics rates in the United States, 1940-1960. Washington,
DC: National Center for Health Statistics, 1968 (PHS publication no. 1677).
3. Waksman S. The conquest of tuberculosis. Berkeley, California: University of California
Press, 1964:193.
Selected Bibliography
Dowling HF. Fighting infection: conquests of the twentieth century. Cambridge, Massachusetts:
Harvard University Press, 1977.
Levy SB. The antibiotic paradox: how miracle drugs are destroying the miracle. New York,
New York: Plenum Press, 1992.
Ryan F. The forgotten plague: how the battle against tuberculosis was won--and lost. Boston,
Massachusetts: Little, Brown, 1993.
Return to top. Box 3 3. New Modes of Disease Transmission Created by 20th-Century Technology · The bacteria that cause legionnaires disease have been spread through modern ventilation systems. · Human immunodeficiency virus and hepatitis C virus have been spread through transfusions of unscreened blood. · Foodborne diseases, such as salmonellosis and Escherichia coli O157 infection, have been spread on centrally processed foods distributed simultaneously to many states or countries. · Airplanes have replaced ships as major vehicles of international disease spread. · More people are traveling to tropical rain forests and other wilderness habitats that are reservoirs for insects and animals that harbor unknown infectious agents. This incursion is due to economic development (e.g., mining, forestry, and agriculture) and an expanded tourist trade that caters to persons who wish to visit undeveloped areas. · In the United States, increasing suburbanization and the reversion of agricultural land to secondary growth forest has brought people into contact with deer that carry ticks infected with Borrelia burgdorferi, the causative agent of Lyme disease, and has brought household pets into contact with rabies-infected raccoons. · The increased development and use of antimicrobial agents has hastened the development of drug resistance. · People whose immunologic and other host defenses have been impaired by modern medical treatments (e.g., bone marrow or solid organ transplants, chemotherapy, chronic corticosteroid therapy, renal dialysis, or indwelling medical devices) are more likely to acquire opportunistic infections. Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 7/29/99 |
|||||||||
This page last reviewed 5/2/01
|