 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Strategies for Reducing Morbidity and Mortality from Diabetes Through Health-Care System Interventions and Diabetes Self-Management Education in Community SettingsA Report on Recommendations of the Task Force on Community Preventive ServicesTask Force on Community Preventive Services* July 1, 2001 CHAIR VICE-CHAIR MEMBERS Mindy Thompson Fullilove, M.D. Fernando A. Guerra, M.D., M.P.H. Alan R. Hinman, M.D., M.P.H. George J. Isham, M.D. Garland H. Land, M.P.H. Charles S. Mahan, M.D. Patricia Dolan Mullen, Dr.P.H. Patricia A. Nolan, M.D., M.P.H. Susan C. Scrimshaw, Ph.D. Steven M. Teutsch, M.D., M.P.H. Robert S. Thompson, M.D. CONSULTANTS Robert S. Lawrence, M.D. J. Michael McGinnis, M.D. Lloyd F. Novick, M.D., M.P.H. Summary Reducing morbidity and mortality and improving quality of life for persons with diabetes is an ongoing challenge for health-care providers and organizations and public health practitioners. Interventions are available that focus on persons with diabetes, health-care systems, families, and public policies. The Task Force on Community Preventive Services (the Task Force) has conducted systematic reviews of seven population-oriented interventions that can be implemented by health-care organizations and communities. Two of these interventions focus on health-care systems (disease and case management), and five focus on persons with diabetes (diabetes self-management education delivered in community settings). On the basis of these reviews, the Task Force has made recommendations regarding use of these seven interventions. The Task Force strongly recommends disease and case management in health-care systems for persons with diabetes. Diabetes self-management education is recommended in community gathering places (e.g., community centers or faith institutions) for adults and in the home for children and adolescents with type 1 diabetes. Evidence was insufficient to recommend diabetes self-management education interventions in other settings (i.e., schools, work sites, and recreational camps) or in the home for adults with type 2 diabetes. This report provides additional information regarding these recommendations, briefly describes how the reviews were conducted, provides sources of full reviews of interventions and information to assist in applying the interventions locally, and describes additional diabetes-related work in progress. BACKGROUNDDiabetes mellitus (diabetes) is a prevalent, costly condition associated with substantial morbidity and mortality. In 1997, approximately 15.7 million persons in the United States (5.9% of the total population) had diabetes (1); of these persons, an estimated 5.4 million persons have diabetes, but it is undiagnosed. Diabetes prevalence is increasing; 789,000 new cases are diagnosed annually (1). Diabetes prevalence increases with age, varying from 0.16% among persons aged <20 years to 18.4% among those aged >65 years (1). Prevalence is also higher among minority populations. For persons aged >20 years, diabetes prevalence is 7.8% among non-Hispanic whites, 10.8% among non-Hispanic blacks, 10.6% among Mexican Americans, and 9.0% among American Indians and Alaska Natives (1). In 1996, diabetes was the seventh leading cause of death in the United States (1). Death rates are twice as high among middle-aged persons (i.e., persons aged 45--60 years) with diabetes than among those without diabetes. Mortality from diabetes is related primarily to heart disease. Adults with diabetes have heart disease death rates approximately 2--4 times higher than adults without diabetes (1). Other complications also lead to increased morbidity and mortality rates. Risk for stroke is 2--4 times higher among persons with diabetes (1). Diabetes is the leading cause of new cases of blindness among adults aged 20--74 years (1) and the leading cause of end-stage renal disease, accounting for approximately 40% of new cases (1). Approximately 60%--70% of persons with diabetes have neuropathy, and >50% of lower limb amputations in the United States occur among persons with diabetes (1). Pregnancy-related deaths occur twice as often among women with diabetes than among those without (1). Diabetes-related costs to U.S. health-care systems are substantial. In 1997, total direct and indirect costs were estimated at $98 billion (2). Diabetes management is complex and difficult from the patient's perspective as well as the provider's, and evidence exists that levels of care are suboptimal (3,4). Lifestyle behaviors (e.g., diet and physical activity) are difficult to change, and healthy behaviors are difficult to maintain for long periods (5). Daily medication regimens, insulin injection, and blood glucose monitoring are complex and uncomfortable. Moreover, substantial time and money is needed to manage diabetes. For successful management, persons with diabetes need adequate patient education and social support. Providers encounter high usage rates and resource consumption by persons with diabetes, and collaborating with patients to achieve behavior change can be frustrating for providers. Providers need support from health-care systems to educate, monitor, and manage patients with diabetes, and coordination is needed among patients, providers, health-care delivery systems, and communities. Reducing morbidity and mortality and improving quality of life for persons with diabetes is a critical public health objective. As part of the Healthy People 2010 initiative (6), goals have been set to prevent diabetes, increase early diagnosis, increase screening rates for diabetes complications, and decrease morbidity and mortality (Table 1). This review focuses on population-oriented strategies that can be implemented by communities and health-care systems to improve the care of persons with diabetes. By implementing interventions reported to be effective, policy makers and health-care and public health providers can help their communities achieve health goals while using community resources efficiently. This report and other related publications provide guidance from the Task Force on Community Preventive Services (the Task Force) for decision makers in state and local health departments, managed care organizations, purchasers of health care, persons responsible for funding public health programs, and others who have an interest in or responsibility for improving the health and well-being of persons with diabetes. Primary prevention is the ideal way to minimize morbidity and mortality from diabetes. For type 2 diabetes, prevention most often consists of weight control and adequate physical activity (7,8). These two topics will be addressed in other reviews in the Guide to Community Preventive Services: Systematic Reviews and Evidence-Based Recommendations (the Community Guide). INTRODUCTIONThe independent, nonfederal Task Force is developing the Community Guide with the support of the U.S. Department of Health and Human Services (DHHS) and in collaboration with public and private partners. CDC and other federal agencies provide staff support to the Task Force for development of the Community Guide. However, the recommendations presented in this report were developed by the Task Force and are not necessarily the recommendations of CDC or DHHS. This report is the fourth that has been completed for the Community Guide, a resource that will include multiple systematic reviews focusing on specific diseases, disabilities, and injuries and ways to promote healthy behaviors and environments. Previous published reports include vaccine-preventable diseases (9--13), tobacco use prevention and control (14,15), and motor vehicle occupant injury (16). This report provides an overview of the process used by the Task Force to select and review evidence. It also summarizes the recommendations of the Task Force regarding two health-care system interventions that focus on diabetes and five interventions to increase diabetes self-management education in community settings. In 2002, a full report will be published in the American Journal of Preventive Medicine that will include the recommendations; supporting evidence (i.e., summaries of the body of evidence and discussions of applicability, additional benefits, potential harms, and existing implementation barriers); costs, cost-benefits, and cost-effectiveness (when available); and remaining research questions. In addition to the seven interventions reviewed in this report, reviews are under way for five additional health-care system interventions as well as for interventions involving family education and public policy. These will be included in future publications. This review did not examine evidence of the effectiveness of clinical care interventions focused on the individual patient. Recommendations regarding clinical care can be obtained from the American Diabetes Association (17). The U.S. Preventive Services Task Force has made recommendations regarding screening (18). METHODSThe Community Guide's methods for conducting systematic reviews and linking evidence to recommendations have been described elsewhere (19). In brief, for each Community Guide topic, a systematic review development team representing diverse disciplines, backgrounds, and work settings conducts reviews by
For the systematic review of diabetes interventions, the team initially focused on two priority areas: health-care system interventions for optimizing care for persons with diabetes and diabetes self-management education interventions in community settings. These areas were selected by consultants* representing diverse experience. They generated a comprehensive list of strategies and created a priority list of interventions for review based on the a) importance of interventions in decreasing morbidity and mortality and in improving quality of life for persons with diabetes; b) potential cost-effectiveness of the intervention; c) lack of clarity regarding the effectiveness of an intervention; and d) feasibility of implementing the interventions in routine public health practice. New models of health-care delivery have emerged in the last decade in response to the failure of traditional models to meet the needs of persons with diabetes and in response to societal changes that include changing demographics, new technology, a shift in the focus of patient care toward quality of life and other patient-oriented outcomes, a demand for minimization of medical errors and iatrogenic injury, and limited health-care resources. Two new models of care delivery, disease and case management, are reviewed in this report. Disease management is defined in the clinical setting as an organized, proactive, multicomponent approach to health-care delivery, involving all members of a population having a specific disease (or a subset of that population with specific risk factors). Care is focused on, and integrated across, the spectrum of the disease and its complications, prevention of comorbid conditions, and relevant aspects of the delivery system. Goals include improving short- and long-term health or economic outcomes or both among persons with the disease. Effectiveness of multicomponent disease-management interventions, and not that of each component, was examined in this review. Case management is a set of activities whereby the needs of patients at risk for excessive resource usage, suboptimal outcomes, or suboptimal coordination of services are identified and addressed through improved planning, coordination, and provision of care (20). Case management involves assigning authority to one professional (i.e., the case manager) who is not the provider of direct health care and who oversees and is responsible for all case management activities. Case management can exist as a single-component intervention, be combined with other clinical care interventions (e.g., practice guidelines or patient reminders), or be part of a disease management intervention. Diabetes self-management education is the process of teaching persons to manage their disease (21). Five related interventions were examined in this review. Community settings are key potential sites for diabetes self-management education interventions. Traditional clinical settings might not be ideal for educating persons with diabetes, but the home can be a good setting for self-management education for multiple reasons: teaching lifestyle changes, including diet, is better facilitated in the home, and teaching self-monitoring of blood glucose is aided by addressing concerns in the environment where the procedure is being performed. Cultural concerns can be addressed in the home as well. Home training might be easier for persons with disabilities or with other difficulties in attending clinic settings. Diabetes self-management education interventions in the home include home visits by a health-care professional or lay health-care worker and computer-assisted instruction or electronic connection to the clinic for advice and feedback (e.g., downloading results of self-monitoring of blood glucose). Community settings include community centers, libraries, private (nonclinical) facilities, and faith institutions. These settings might be more convenient and comfortable than clinic settings for diabetes self-management education. To be included in the reviews of effectiveness, studies had to a) be primary investigations of interventions selected for evaluation; b) be published in English; c) be conducted in established market economies;** d) provide information regarding >1 outcomes of interest that were preselected by the team; and e) meet minimum quality standards (22). All types of comparative study designs (i.e., randomized controlled trials, preintervention versus postintervention designs, times series, and cohort studies) were included in the reviews (19). For each intervention reviewed, the team developed an analytic framework indicating possible causal links between the intervention and predefined outcomes of interest that are linked to improved health outcomes. The Task Force concluded that the link is sufficiently strong between the behavioral and short-term health outcomes and long-term effects on morbidity, mortality, and quality of life. Therefore, intervention evaluations in this review focused on evidence of effectiveness of interventions in improving patient and provider behaviors, as well as short- and long-term patient health outcomes, as discussed in the following:
Each study that met the inclusion criteria was evaluated by using a standardized abstraction form (19), and each was assessed for study design suitability and threats to internal validity (19). On the basis of the number of threats to validity, studies were characterized as having good, fair, or limited quality of execution (19), and only studies with good or fair execution were included in the review. A summary effect measure (i.e., the difference between the changes observed in the intervention and comparison groups, if the study design used a comparison group) was calculated for outcomes of interest. Interquartile ranges were determined as an index of variability when >7 studies were available in the body of evidence. Pooled estimates of effect were calculated if a sufficient number of studies with comparable outcomes existed and if exploratory data analysis revealed diverse results in the body of literature or confidence intervals overlapped zero. Point estimates of effect were calculated with both fixed and random effects models by using the inverse of the variance of the net change in GHb as the study weight. Computation of the between-study variance for the random effects model was obtained by using a recommended formula (47) and using estimates of within-group correlation (rho) of 0.25, 0.5, and 0.75. The pooled estimates presented are from random effects models, with rho equaling 0.75 and 95% confidence intervals. Evidence of effectiveness is characterized as strong, sufficient, or insufficient on the basis of the number of available studies, the suitability of study designs for evaluating effectiveness, the quality of execution of the studies, the consistency of the results, and the effect size (19). The Community Guide uses systematic reviews to evaluate the evidence of intervention effectiveness, and the Task Force makes recommendations on the basis of the review findings (19). The strength of each recommendation is based on the strength of the evidence of effectiveness (e.g., an intervention is strongly recommended when strong evidence of effectiveness exists, and an intervention is recommended when sufficient evidence exists) (19). Other types of evidence also can affect recommendations. For example, evidence of harms resulting from an intervention might lead to a recommendation that the intervention not be used if adverse effects outweigh improved outcomes. Although the option exists, the Task Force has yet to use economic information to modify recommendations. A finding of insufficient evidence of effectiveness should not be interpreted as evidence of ineffectiveness. Identification of interventions for which evidence of effectiveness is insufficient is critical for identifying areas of uncertainty and research agendas. In contrast, adequate evidence of ineffectiveness would lead to a recommendation that the intervention not be used. RESULTSBy using computerized databases, reviews of reference lists from included studies, and consultation with diabetes specialists, the review team identified 105 studies that met the inclusion criteria for the seven interventions that the Task Force evaluated for this report. Of those 105 studies, 35 were excluded on the basis of limitations in their execution and were not considered further. The remaining 70 studies were included in the review,*** and the Task Force recommendations presented in this report are based on those studies. On the basis of the evidence of effectiveness, the Task Force either strongly recommends or recommends four of the seven strategies evaluated (Table 2): disease management and case management in health-care systems, diabetes self- management education in the home for children and adolescents with type 1 diabetes, and self-management education in community gathering places for adults with diabetes. The Task Force found insufficient evidence on which to make a recommendation for or against diabetes education for school personnel or self-management education at work sites and in recreational camps. Results are presented for the preselected outcomes where data are available. For certain outcomes (e.g., aspirin use, physical activity, cardiac events, and mortality), no data were available in studies that met inclusion criteria. Summary tables of the reviews of economic evidence are available at <http://www.thecommunityguide.org> (accessed July 16, 2001). USING THESE RECOMMENDATIONS IN COMMUNITIES AND HEALTH-CARE SYSTEMSGiven the substantial public health burden of diabetes, improving care for persons with diabetes should be relevant in the majority of communities and health-care systems. In selecting and implementing interventions, communities and health-care systems should strive to develop a comprehensive strategy to promote healthy lifestyles (e.g., increased physical activity, improved nutrition, and reduced tobacco use) and to help persons with diabetes and their health-care providers and systems to improve glycemic control, decrease diabetes complications and mortality, and improve quality of life. Choosing interventions that have been shown to work and that are well-matched to local needs and capabilities and then implementing those interventions are vital steps toward improving outcomes for persons with diabetes. In setting priorities for selecting interventions to meet local objectives, recommendations and other evidence provided in the Community Guide should be considered in combination with local information (e.g., resource availability, administrative structures, and the economic, social, and regulatory environments of organizations and practitioners). Information regarding applicability can be used to assess intervention usefulness for each setting or population. Though currently sparse, economic information (to be provided in the full report in 2002) might be useful in identifying resource requirements for interventions and interventions that meet public health goals more efficiently than other available options. If local goals and resources permit, strongly recommended and recommended interventions should be initiated or increased. Communities and health-care systems should first assess the prevalence of diabetes and associated complications in the community or organization and the level of care and education provided to persons with diabetes. Care levels can be compared with guidelines and treatment goals that are based on scientific opinions from health organizations (e.g., the American Diabetes Association) (17). Community approaches can then be developed to address health disparities and improve care and quality of life. The Task Force strongly recommends disease and case management to improve system-level (e.g., provider monitoring) and patient (e.g., glycemic control) outcomes. Resources and infrastructure required to implement these interventions can be substantial. Letting organizations implement components of disease management might be more feasible. Identification of the population and practice guidelines could be implemented initially, then followed by other strategies (e.g., case management). Strategies need not be sophisticated. For example, initial identification of the population could be achieved through verbal communication with providers and patients, and the information systems for monitoring could be paper records or electronic spreadsheets. The Task Force recommends diabetes self-management education in the home for children and adolescents with diabetes and in community gathering places for adults. Interventions in these settings are not intended to replace clinic-based ones, but rather to complement them when community settings are more feasible or desirable for the patient. Communication and collaboration between educators and health-care providers are essential. Insufficient evidence exists on which to base recommendations for or against diabetes self-management education at recreational camps and work sites and educating school personnel regarding diabetes. In summary, health-care system and diabetes self-management education interventions exist that are effective in improving health outcomes. Community- and health-care system-based efforts are needed to deliver optimal care for persons with diabetes and to achieve Healthy People 2010 goals. The systematic reviews that led to the recommendations discussed in this report should be useful to researchers and scientific organizations in identifying directions for future research. The reader is reminded that the Task Force decision not to make recommendations regarding certain interventions does not imply that the interventions were ineffective. Rather, that decision reflects the fact that an insufficient number of high-quality studies existed upon which to base a recommendation. These areas need further research. ADDITIONAL INFORMATION REGARDING THE COMMUNITY GUIDEAdditional Community Guide systematic reviews of oral health, sexual behavior, physical activity, cancer, and the sociocultural environment are being developed, and the results of each review will be published as it is completed. A compilation of the reviews will be published in book form. Additional information regarding the Task Force and the Community Guide is available at <http://www.thecommunityguide.org> (accessed July 16, 2001). References****1. CDC/National Center for Chronic Disease Prevention and Health Promotion. National diabetes fact sheet. Atlanta, GA: US Department of Health and Human Services, CDC, 2000. Available at <http://www.cdc.gov/diabetes/pubs/facts98.htm>. Accessed July 17, 2001. 2. American Diabetes Association. Economic consequences of diabetes mellitus in the U.S. in 1997. Diabetes Care 1998;21:296--309. 3. Glasgow RE, Strycker LA. Preventive care practices for diabetes management in two primary care samples. Am J Prev Med 2000;19:9--14. 4. Peters AL, Legoretta AP, Ossorio RC, Davidson MB. Quality of outpatient care provided to diabetic patients: a health maintenance organization experience. Diabetes Care 1996;19: 601--6. 5. Norris SL, Engelgau MM, Venkat Narayan KM. Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care 2001;24:561--87. 6. US Department of Health and Human Services. Healthy people 2010. 2nd ed. Washington, DC: US Government Printing Office, 2000. 7. Pan X-R, Li G-W, Hu Y-H, et al. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance: the Da Qing IGT and diabetes study. Diabetes Care 1997;20:537--44. 8. Tuomilehto J, Lindström J, Eriksson JG, et al. for the Finnish Diabetes Prevention Study Group. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001;344:1343--50. 10. Task Force on Community Preventive Services. Recommendations regarding interventions to improve vaccination coverage in children, adolescents, and adults. Am J Prev Med 2000;18(1S):92--6. 11. Shefer A, Briss P, Rodewald L, et al. Improving immunization coverage rates: an evidence-based review of the literature. Epidemiol Rev 1999;21:96--142. 12. Briss PA, Rodewald LE, Hinman AR, et al., and the Task Force on Community Preventive Services. Reviews of evidence regarding interventions to improve vaccination coverage in children, adolescents, and adults. Am J Prev Med 2000;18(1S):97--140. 13. Hopkins DP, Briss PA, Ricard CJ, et al., and the Task Force on Community Preventive Services. Reviews of evidence regarding interventions to reduce tobacco use and exposure to environmental tobacco smoke. Am J Prev Med 2001;20(2S):16--66. 14. Task Force on Community Preventive Services. Recommendations regarding interventions to reduce tobacco use and exposure to environmental tobacco smoke. Am J Prev Med 2001;20(2S):10--5. 17. American Diabetes Association. American Diabetes Association: clinical practice recommendations 2001. Diabetes Care 2001;24(Suppl 1):S1--133. 18. US Preventive Services Task Force. Screening for diabetes mellitus. In: Guide to clinical preventive services. 2nd ed. Alexandria, Virginia: International Medical Publishing, Inc., 1996;193--208. 19. Briss PA, Zaza S, Pappaioanou M, et al., and the Task Force on Community Preventive Services. Developing an evidence-based Guide to Community Preventive ServicesCmethods. Am J Prev Med 2000;18(1S):35--43. 20. Smith JC, Greer NL for the Technology Assessment Committee. Case management for chronic illness, the frail elderly, and acute myocardial infarction. Bloomington, MN: Institute for Clinical Systems Integration, 1998. Technology Assessment Report (TA #44). 21. Task Force to Revise the National Standards. National standards for diabetes self-management education programs. Diabetes Educator 1995;21:189--93. 22. American Diabetes Association. Standards of medical care for patients with diabetes mellitus. Diabetes Care 2001;24(Suppl 1):S33--55. 23. American Diabetes Association. Tests of glycemia in diabetes. Diabetes Care 2001;24 (Suppl 1):S80--2. 24. Evans JMM, Newton RW, Ruta DA, MacDonald TM, Stevenson RJ, Morris AD. Frequency of blood glucose monitoring in relation to glycaemic control: observational study with diabetes database. BMJ 1999;319:83--6. 25. Diabetes Control and Complications Trial Research Group. Effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993;329:977--86. 26. Ohkubo Y, Kishikawa H, Araki E, et al. Intensive insulin therapy prevents the progression of diabetic microvascular complications in Japanese patients with non-insulin-dependent diabetes mellitus: a randomized prospective 6-year study. Diabetes Res Clin Pract 1995;28:103--17. 27. Wake N, Hisashige A, Katayama T, et al. Cost-effectiveness of intensive insulin therapy for type 2 diabetes: a 10-year follow-up of the Kumamoto study. Diabetes Res Clin Pract 2000;48:201--10. 28. Reaven GM, Staff of the Palo Alto GRECC Aging Study Unit. Beneficial effect of moderate weight loss in older patients with nonBinsulin-dependent diabetes mellitus poorly controlled with insulin. J Am Geriatr Soc 1985;33:93--5. 29. Wing RR, Koeske R, Epstein LH, Nowalk MP, Gooding W, Becker D. Long-term effects of modest weight loss in type II diabetic patients. Arch Intern Med 1987;147:1749--53. 30. Watts NB, Spanheimer RG, DiGirolamo M, et al. Prediction of glucose response to weight loss in patients with nonBinsulin-dependent diabetes mellitus. Arch Intern Med 1990;150:803--6. 31. American Diabetes Association. Nutrition recommendations and principles for people with diabetes mellitus. Diabetes Care 2001;24(Suppl 1):S44--7. 32. Early Treatment Diabetic Retinopathy Study Research Group. Early photocoagulation for diabetic retinopathy: ETDRS Report Number 9. Ophthalmology 1991;98:766--85. 33. American Diabetes Association. Aspirin therapy in diabetes. Diabetes Care 2001;24 (Suppl 1):S62--3. 34. American Diabetes Association. Diabetes mellitus and exercise. Diabetes Care 2001;24(Suppl 1):S51--5. 35. American Diabetes Association. Smoking and diabetes. Diabetes Care 2001;24 (Suppl 1):S64--5. 36. UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998;352:837--53. 37. UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 1998;317:703--13. 38. Fontbonne A, Eschwege E, Cambien F, et al. Hypertriglyceridaemia as a risk factor of coronary heart disease mortality in subjects with impaired glucose tolerance or diabetes: results from the 11-year follow-up of the Paris Prospective Study. Diabetologia 1989;32: 300--4. 39. Bild DE, Selby JV, Sinnock P, Browner WS, Braveman P, Showstack JA. Lower-extremity amputation in people with diabetes: epidemiology and prevention. Diabetes Care 1989;12:24--30. 40. Rith-Najarian SJ, Stolusky T, Gohdes DM. Identifying diabetic patients at high risk for lower-extremity amputation in a primary health care setting: a prospective evaluation of simple screening criteria. Diabetes Care 1992;15:1386--9. 41. American Diabetes Association. Preventive foot care in people with diabetes. Diabetes Care 2001;24(Suppl 1):S56--7. 42. American Diabetes Association. Management of dyslipidemia in adults with diabetes. Diabetes Care 2001;24(Suppl 1):S58--61. 43. Ravid M, Lang R, Rachmani R, Lishner M. Long-term renoprotective effect of angiotensin-converting enzyme inhibition in nonBinsulin-dependent diabetes mellitus: a 7-year follow-up study. Arch Intern Med 1996;156:286--9. 44. American Diabetes Association. Diabetic retinopathy. Diabetes Care 2001;24(Suppl 1): S73--6. 45. Bakris GL, Williams M, Dworkin L, et al. Preserving renal function in adults with hypertension and diabetes: a consensus approach. Am J Kidney Dis 2000;36:646--61. 46. American Diabetes Association. Diabetic nephropathy. Diabetes Care 2001;24(Suppl 1): S69--72. 47. DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials 1986;7:177--88. *Consultants for the systematic reviews were Tanya Agurs-Collins, Ph.D., Howard University Cancer Center, Washington, DC; Ann Albright, Ph.D., California Department of Health Services, Sacramento, California; Pam Allweiss, M.D., Lexington, Kentucky; Norman Anderson, Ph.D., National Institutes of Health, Bethesda, Maryland; Elizabeth Barrett-Connor, M.D., University of California San Diego, LaJolla, California; Sharon Brown, Ph.D., University of Texas, Austin, Texas; Richard Eastman, M.D., Cygnus, San Francisco, California; Luis Escobedo, M.D., New Mexico Department of Health, Las Cruces, New Mexico; Wilfred Fujimoto, M.D., University of Washington, Seattle, Washington; Maureen Harris, Ph.D., M.P.H., National Institutes of Health, Bethesda, Maryland; Deborah Hinnen, M.N., Via Christi Regional Medical Center, Wichita, Kansas; Roland Hiss, M.D., University of Michigan, Ann Arbor, Michigan; Richard Kahn, Ph.D., University of California San Diego, La Jolla, California; Shiriki Kumanyika, Ph.D., University of Pennsylvania, Philadelphia, Pennsylvania; David Marrerro, Ph.D., Indianapolis University, Indianapolis, Indiana; Marjorie Mau, M.D., Honolulu, Hawaii; Kathy Mulcahy, M.S., INOVA Diabetes Center, Fairfax, Virginia; Frieda Outlaw, Ph.D., University of Pennsylvania, Philadelphia, Pennsylvania; Nicolaas Pronk, Ph.D., Health Partners, Minneapolis, Minnesota; Laverne Reid, Ph.D., M.P.H., North Carolina Central University, Durham, North Carolina; Yvette Roubideaux, M.D., M.P.H., University of Arizona, Tuscon, Arizona; Angela Weaver, Ph.D., Grambling State University, Grambling, Louisiana; Kimberydawn Wisdom, M.D., M.S., University of Michigan, Detroit, Michigan; Rena Wing, Ph.D., Brown University, Providence, Rhode Island. **Established market economies as defined by the World Bank are Andorra, Australia, Austria, Belgium, Bermuda, Canada, Channel Islands, Denmark, Faeroe Islands, Finland, France, Former Federal Republic of Germany, Germany, Gibraltar, Greece, Greenland, Holy See, Iceland, Ireland, Isle of Man, Italy, Japan, Liechtenstein, Luxembourg, Monaco, the Netherlands, New Zealand, Norway, Portugal, San Marino, Spain, St. Pierre and Miquelon, Sweden, Switzerland, the United Kingdom, and the United States. ***Additional information regarding qualifying studies is available at <http://www.thecommunityguide.org> (accessed July 16, 2001). ****All MMWR references are available on the Internet at <http://www.cdc.gov/mmwr/>. Use the search function to find specific articles. Table 1 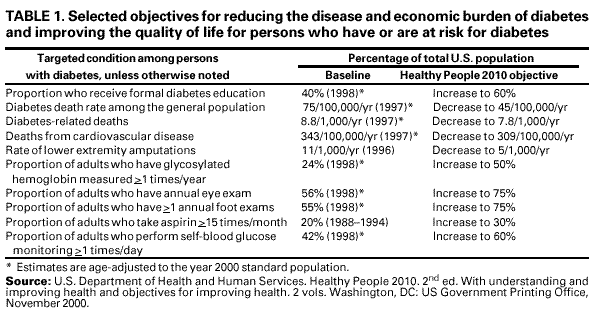 Return to top. Table 2 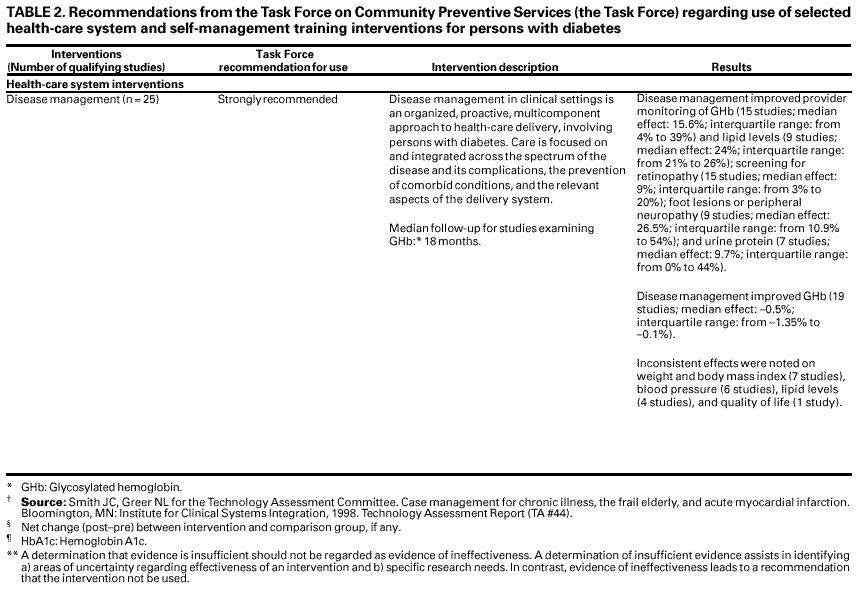 
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/10/2001 |
|||||||||
This page last reviewed 8/10/2001
|