 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Economic Costs Associated with Mental Retardation, Cerebral Palsy, Hearing Loss, and Vision Impairment --- United States, 2003Please note: An erratum has been published for this article. To view the erratum, please click here. Developmental disabilities (DDs) are chronic conditions that initially manifest in persons aged <18 years and result in impairment of physical health, mental health, cognition, speech, language, or self-care (1). The majority of persons with DDs require long-term supportive care or services. In 2003, RTI International (Research Triangle Park, North Carolina) and CDC analyzed data from multiple surveys and reports to estimate the direct and indirect economic costs associated with four DDs in the United States (2). On the basis of that analysis, estimated lifetime costs in 2003 dollars are expected to total $51.2 billion for persons born in 2000 with mental retardation, $11.5 billion for persons with cerebral palsy, $2.1 billion for persons with hearing loss, and $2.5 billion for persons with vision impairment. These estimates underscore the need for effective primary and secondary prevention measures (e.g., newborn screening for hearing and metabolic disorders and smoking-cessation counseling for pregnant women) to reduce the costs associated with DDs. The four DDs chosen for analysis were selected because of the availability of reliable prevalence estimates and diagnoses recorded in national health-care databases. Autism was not included in this analysis because of major gaps in available cost data; CDC is exploring methods to collect reliable cost information regarding autism. Detailed descriptions of the methods and data sources used in the analysis have been reported previously (2). Standard cost-of-illness methods using a societal perspective were followed; cost estimates represent the costs attributable to DDs above ordinary costs incurred by unaffected persons in the U.S. population. Direct medical and nonmedical costs (e.g., physician visits, inpatient hospital stays, assistive devices, and home and automobile modifications) were identified from data collected by the 1994--1995 National Health Interview Survey (NHIS). For medical care, unit costs were calculated from the 1987 National Medical Expenditure Survey (NMES) and the 1995 Healthcare Cost and Utilization Project (HCUP) of the Agency for Healthcare Research and Quality, adjusting for inflation by using the medical component of the Consumer Price Index. Special education costs were estimated on the basis of use of special education by elementary school--aged children with any of the four DDs tracked by CDC's Metropolitan Atlanta Developmental Disabilities Surveillance Program (MADDSP). Special education costs were updated for this report on the basis of a recent report from the Special Education Expenditure Project for the 1999--2000 school year (3) and adjusted for inflation by using the Employment Compensation Index for state and local government employees. Indirect costs were calculated by estimating the value of productivity losses in workplaces and households that occur when persons with DDs die prematurely, are unable to work, or are limited in the amount or type of work they can perform. Estimates of excess premature deaths were calculated for persons with each DD aged 10--20 years and for adults with mental retardation and cerebral palsy; average survival rates for the U.S. population were assumed for adults with vision impairment and hearing loss (2). The number of excess deaths was multiplied by the present value of the sum of expected lifetime earnings, fringe benefits, and household services. The percentages of persons with each DD who reported being unable to work or being limited in work was determined by using the 1994--1995 NHIS-Disability Survey. Percentage reductions in earnings for adults with each DD who reported being limited in work were derived from the U.S. Census Bureau's Survey on Income and Program Participation. The size of the 2000 cohort for each DD was estimated by multiplying prevalences from MADDSP by the number of live-born infants in the United States in 2000. MADDSP is the only ongoing, population-based program in the United States that tracks children with mental retardation, cerebral palsy, hearing loss, vision impairment, and autism. The program provides reliable data on the prevalence of these conditions (1). Per-person cost estimates were developed for each of the four DDs in six age groups. Present value estimates were derived by discounting future costs back to 2003 dollars based on a 3% discount rate. Average lifetime costs per person were estimated at $1,014,000 for persons with mental retardation, $921,000 for persons with cerebral palsy, $417,000 for persons with hearing loss, and $566,000 for persons with vision impairment (Table). Indirect costs accounted for the largest percentage (range: 63%--81%) of total costs associated with each DD. Total direct costs (i.e., direct medical plus direct nonmedical) amounted to approximately $12.3 billion for persons with mental retardation, $2.2 billion for persons with cerebral palsy, $770 million for persons with hearing loss, and $570 million for persons with vision impairment. Among total direct costs, special education accounted for a substantial percentage (range: 42%--82%) for each DD. Reported by: A Honeycutt, PhD, L Dunlap, MA, H Chen, MA, G al Homsi, MA, RTI International, Research Triangle Park, North Carolina. S Grosse, PhD, D Schendel, PhD, National Center on Birth Defects and Developmental Disabilities, CDC. Editorial Note:The costs associated with DDs in the United States highlight the need for strategies to reduce the prevalence of these conditions and prevent development of secondary conditions. Direct lifetime costs associated with mental retardation alone are estimated to exceed $12 billion. By comparison, direct costs associated with asthma, a chronic illness with a prevalence rate approximately six times that of mental retardation, have been estimated at $9 billion (4). Certain public health measures (e.g., newborn screening for metabolic disorders) have proven effective in preventing cases of mental retardation and other DDs (5). In addition, low birthweight (LBW) is a known risk factor for mental retardation and other DDs (6), and maternal smoking and alcohol consumption are risk factors for both LBW and mental retardation (7). Smoking-cessation counseling targeted to pregnant women has proven effective in preventing LBW (8), and strategies to reduce alcohol use before pregnancy are being tested. Lifetime indirect costs (i.e., productivity losses) associated with DDs were estimated at two to five times the amount of direct costs, suggesting the need to address the physical, social, and economic factors that limit the functional participation of persons with DDs. Certain screenings and interventions for children with DDs can improve functional participation. Early intervention for children with hearing loss has been associated with higher language development scores (9), and newborn hearing screening is projected to be cost-effective because of anticipated gains in lifetime earnings (10). The findings in this report are subject to at least four limitations. First, survey data were based on reports from family members and could not be used to characterize degree of DD severity. Second, cost estimates for specific DDs included comorbidities; total costs incurred by a person with mental retardation and cerebral palsy were assigned to both conditions. Third, certain costs (e.g., caregiver, family out-of-pocket, hospital outpatient, emergency department, and residential care for persons not living in households) were excluded because of limited data. Approximately 8% of persons with mental retardation reside in institutions or group homes (2). Finally, DD prevalences were based on data from MADDSP and might not be representative of national prevalences. Despite the magnitude of the direct-cost estimates in this report, they reflect only present use of medical and support services by persons with the four DDs. Additional studies are needed to measure other economic costs, such as those associated with treating psychosocial problems that can accompany a DD and to determine to what extent such treatment might be constrained by insurance reimbursement practices. Without such constraints, the cost estimates in this report might be substantially higher if optimal care is to be provided for persons with these DDs. References
Table 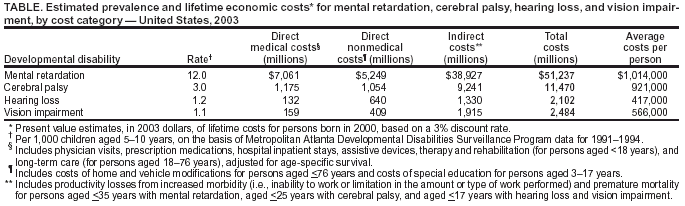 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 1/29/2004 |
|||||||||
This page last reviewed 1/29/2004
|