

|

|

Volume 5: No.
1, January 2008
COMMUNITY CASE STUDY
Translating a Community-Based Motivational Support Program to Increase Physical Activity
Among Older Adults With Diabetes at Community Clinics: A Pilot Study of Physical Activity for a Lifetime of Success (PALS)
Odette Batik, MD, MPH, Elizabeth A. Phelan, MD, MS, Julie A. Walwick, MSW, Grace Wang, MD, MPH, James P. LoGerfo, MD, MPH
Suggested citation for this article: Batik O, Phelan EA, Walwick
JA, Wang G, LoGerfo JP. Translating a
community-based, motivational support program to increase physical activity
among
older adults with diabetes at community clinics: a pilot study of Physical Activity for a
Lifetime of Success (PALS). Prev Chronic Dis 2008;5(1).
http://www.cdc.gov/pcd/issues/2008/
jan/07_0142.htm. Accessed [date].
PEER REVIEWED
Abstract
Background
Regular physical activity is an important goal for elders with chronic health conditions.
Context
This report describes Physical Activity for a Lifetime of Success (PALS), an
attempt to translate a motivational support program for physical activity,
Active Choices, for use by a group of diverse, low-income, community-dwelling elders with diabetes.
Methods
PALS linked physical activity assessment and brief counseling by primary care providers with a structured referral to a community-based motivational telephone support program delivered by older adult volunteers. People with diabetes aged 65
years or older who were receiving care at two community clinics were randomized to receive either immediate or delayed
intervention. The main intended outcome measure was physical activity level; the secondary outcome measure was mean hemoglobin A1c.
Consequences
One-third of those offered referral to the PALS program in the clinic setting declined. Another 44% subsequently declined enrollment or were unreachable by the support center. Only 14 (21%) of those offered referral enrolled in the program. Among these 14, the
percentage who were sufficiently active was higher at follow-up than at enrollment, though
not significantly so. Using an intent-to-treat analysis, which included all randomized clinic patients, we found no significant change in mean hemoglobin A1c for the intervention group compared with controls.
Interpretation
A community-based referral and support program to increase physical activity among elderly, ethnically diverse, low-income people with diabetes, many of whom are not English-speaking, may be thwarted by unforeseen barriers. Those who enroll and participate in the
PALS program appear to increase their level of physical activity.
Back to top
Background
Despite the significant benefits of regular physical activity for older adults (1-3), the majority are not optimally active (4). Although older adults with diabetes have even more reason to be active
than younger adults, their levels of activity also are low (5). Thus, encouragement and monitoring of physical activity by primary care providers has been recognized as a key indicator of quality of care for patients
with diabetes (6).
Lack of adequate physical activity among people with diabetes raises the question of how clinicians can best improve
the activity levels of their patients. Although it is not clear whether physician counseling is effective in increasing physical activity levels (7), such counseling with trained educators providing in-person follow-up or
telephone support has shown promise (3,7).
These observations formed the background for the project described here, Physical Activity for a Lifetime of Success (PALS). The PALS program links clinics to a senior center-based program modeled after the Active Choices program (8). The Active Choices model is a 6-month program in which community agencies assist individuals in engaging in a physical activity program. This model has been
shown to increase caloric expenditure in young and middle-aged adults. However, it has not been evaluated in a diverse or low-income population of older adults with diabetes (8). Thus, the goal of
our study was to attempt to translate a variant of the Active Choices program to older, low-income, ethnically diverse people with diabetes in partnership with community clinics.
Back to top
Context
Setting
We conducted our study in the Southeast Seattle neighborhood from March 1, 2005, through July 31, 2006. This neighborhood is largely below the median income for the city and the surrounding county (King County), and when the study began, most of the population aged 65
years or older was from races other than white. An earlier study had demonstrated that the neighborhood had sufficient resources (i.e., older adult-oriented physical activity programs, exercise facilities) to support physical activity for older adults, but
demand for such programs was relatively low (9). Before this intervention, the
University of Washington’s (UW’s) Health Promotion Research Center had also been
promoting opportunities for seniors to be active (10). While the PALS study was in progress, the research center undertook a related effort to
reduce common barriers to physical activity (11).
We decided that developing a program that enhanced existing efforts to improve care of people with diabetes would be most sustainable.
After reviewing evidence-based support programs, we chose to import the Active Choices program (8) in a modified format and rename it Physical Activity for a Lifetime of Success, or PALS. The organizations involved
were two community clinics, the neighborhood senior center, a community social services provider, and the UW’s Health Promotion Research Center.
PALS was made available for referral through primary care providers (PCPs). The community clinics had an ongoing quality assurance program, including
participation in a collaborative care model to monitor their patients with diabetes (6). An electronic registry had been in place for several years to provide reminders, including a record field addressing physical activity (6). In July 2004, the community clinics adopted the Seattle Rapid Assessment of Physical Activity (RAPA)
program (12) to assess physical activity levels for all their older patients
with diabetes.
All community partners contributed to the PALS project design. We obtained institutional review board approval from UW. Before the start of the study, participating community clinics mailed a letter to all eligible participants to inform them of the project.
Participants
All patients with diabetes aged 65 years or older who had visited a clinic within the
previous 18 months were eligible to participate. No a priori clinical reasons for exclusion were defined, but PCPs eliminated any patients who they determined would not be medically suitable because of comorbidities. Comorbidities that precluded participation were profound dementia, severe congestive heart failure, decompensated psychiatric illness, and terminal malignancy. Some patients were excluded because of a lack of interpreter services. Lack of telephone access was also a reason for exclusion.
Recruitment
The PCP referred patients to the PALS program during routine appointments. Patients completed the RAPA questionnaire at their first visit following the start of the study period. This prompted the PCP to review the patient’s physical activity level and discuss the benefits of physical activity. The PCP then developed a prescription for physical activity (sample prescription available at
http://depts.washington.edu/hprc/docs/parx.pdf *)
in collaboration with the patient. To avoid making the process overly complex,
we did not formally assess motivational readiness to exercise.
After developing the physical activity prescription, the PCP asked the patient if he or she would be receptive to contact by the PALS community support program. Patients who expressed interest signed a consent
form permitting the sharing of their name, contact information, and exercise prescription with community partners. A referral was then faxed to the PALS project coordinator, who arranged an intake interview. If a person decided to participate, additional consent was obtained on the first visit to the senior center.
Delayed intervention group
All clinic patients, regardless of group assignment and interest in participating in the PALS program, received a guide to local activity resources, as well as handouts about the benefits of exercise, tips on safety, and strength and balance exercises.
Back to top
Methods
Physical activity intervention
The PALS program was a motivational support program delivered by older adult volunteers over the telephone. The theoretical framework underlying the program on which PALS is modeled, Active Choices (8), is behavioral, incorporating principles of self-efficacy and tailoring support to an individual’s readiness to change. We adapted the Active Choices program in several ways. First, we streamlined volunteer training materials and reduced the literacy level of participant materials. Second, we focused on increasing physical activity levels rather than on heart-rate goals. Third, we
hired a PALS coordinator who conducted intake interviews. Fourth, the staff of the neighborhood senior center recruited telephone volunteers from among active older adults already engaged in senior center programs. Training for telephone volunteers was conducted by Active Choices staff who consulted on the PALS project and, later, by the senior center program coordinator.
We made ongoing telephone support available to participants. Except for an initial interview and intake conducted at the senior center, the client participant chose the site to carry out his or her physical activity plan and could include any combination of home- and community-based programs. Participants were encouraged to continue with the PALS program for a minimum of 6 months. Certain barriers to increasing activity were reduced: fees were waived for EnhanceFitness classes (a community-based group exercise program for older adults that originated in the Seattle area) (13),
and transportation was offered to group walking sites.
PALS program staffing
The PALS program was staffed by a half-time project coordinator employed by Senior Services of Seattle/King County and was based at the senior center. Primary skills sought in the coordinator were an ability to communicate effectively, a genuine interest in working with older adults, experience in engaging and motivating volunteers, and a personal commitment to being physically active.
Randomization
Clinic patients with diabetes were offered the program in a staggered manner, with one
set of patients randomly allocated to a group offered PALS participation early, and another to one offered PALS
1 year later. Eligible participants were identified from the diabetes registries of each of the participating community clinics and randomly assigned to the immediate intervention group or to the
1-year, delayed intervention group. People with diabetes who reached age 65 or
who newly established care at the beginning of the study were also randomized to the immediate or delayed intervention
groups. Those who became newly eligible later in the study period were added to the delayed intervention group. Both these groups of patients are referred to here as “late-added participants.”
Outcome measurements
The primary outcome measure for the PALS study was the participant’s level of physical activity, as measured by the RAPA questionnaire (12). RAPA scores of 1–3 correspond to minimal physical activity, scores of 4
and 5 are suboptimal but consistent with some potential health benefit (4), and scores of 6
and 7 are consistent with the U.S. Surgeon General’s recommendations (14) for optimal physical activity. RAPA assessments were completed upon enrollment and again at 6
or more months following enrollment.
Our secondary outcome measure was average hemoglobin A1c (HbA1c), which was assessed within 6 months of commencement of the study and at follow-up clinic visits 6 months or more after the study began.
Data analysis
We assessed differences between the two study groups at baseline with two sample t tests for continuous variables and chi-square tests for dichotomous variables.
We used the McNemar test for matched pairs to assess differences between RAPA scores at enrollment and at follow-up.
Back to top
Consequences
Characteristics of participants randomized to immediate and delayed intervention groups
Table 1 shows baseline
characteristics of eligible participants, by intervention group. Those
randomized to the immediate intervention group were significantly older than
those in the delayed intervention group, because many of those who “aged in” on turning age 65 (late-added participants) were added to the delayed intervention group. The groups were otherwise well balanced with respect
to sex, race, and language, as well as baseline RAPA scores and HbA1c values. Age, blood pressure, body mass index, or HbA1c
did not differ significantly between those who enrolled in PALS and those who did not.
Success of attempt to recruit community-based, sedentary older adults
Fourteen of sixty-five persons who were offered the program enrolled (Figure).
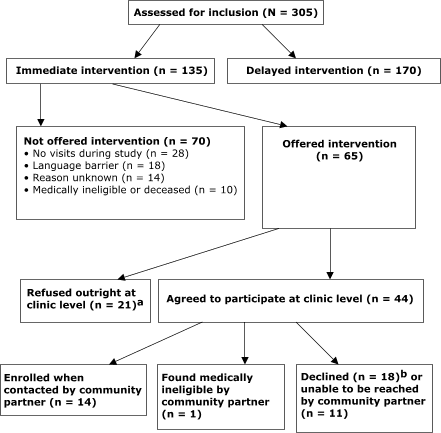
Figure. Participant flow, PALS study, 2005 – 2006. [A text description of this figure is also available.]
a Reasons for outright refusal were lack of
interest, feeling at an age for rest rather than physical activity, feeling
already active enough, perceived ill health and consequent inability to be more
active, depression, unfamiliarity with the senior center, and uneasiness about
having a telephone call from a stranger.
b Reasons for declining after initially agreeing to participate were
lack of interest, too busy, other issues of higher priority, and
difficulty comprehending English.
Impact of PALS on physical activity levels and HbA1c results
Among the 14 PALS participants, the percentage who were sufficiently active
increased, although not significantly (Table 2).
Change of HbA1c levels did not differ significantly between immediate intervention
participants (average HbA1c decline, 0.1%) and delayed intervention participants (average HbA1c decline, 0.3%).
Barriers and facilitators encountered
Time constraints inherent in the outpatient visit were a probable barrier to providers’ offering the intervention. This factor may have been responsible for the 20% of potential participants who were never offered the intervention. Opportunities to discuss physical activity during a visit to a health care provider were frequently limited by a more acute medical issue.
Lessons learned
Clinic visits may not be an ideal environment in which to engage participants. In addition, motivating seniors to begin exercising is a major challenge.
Subsequent steps
Because clinic visits may not be ideal settings for engaging participants, UW
researchers and community clinics discontinued recruiting during clinic visits. The community clinics’ health educator became responsible for contacting patients with diabetes to invite them to participate in PALS. The clinics also lowered the eligibility age for PALS to
50 years.
We are considering conducting focus groups with patients who did not enroll in PALS to understand barriers that prevented them from enrolling and to solicit their ideas about delivering such a program. In addition, we are considering obtaining feedback from PCPs on their perceptions of PALS and perspectives on offering it to patients.
Feedback to community
We have shared the findings from this study with key physician providers at each of the community clinics.
We also have discussed the findings with the director of the senior center.
Back to top
Interpretation
This analysis of an attempt to engage low-income, ethnically diverse older adults in a community-based, motivational physical activity support program yielded two main findings: 1) participation rates among those eligible
were low overall and 2) the program had some impact on physical activity levels among those who did enroll.
Participation rates for PALS appear to be similar to those of a comparable
program. An Active Choices intervention had 45%–53% participation after clients
expressed interest in the program (15). In our study, 14 (44%) of 32 clients who were willing to discuss the program and whom we were able to contact
agreed to participate.
The low participation rates in PALS
may have several explanations. First, of the half of those assigned to the intervention group who were never offered the intervention, 40% were not offered it because they
did not visit the clinic during the study period. Another 25% lacked needed interpreter services, and 14% were medically unable
to participate. In efficacy studies of physical activity (3), people who did not
speak fluent English or who had medical limitations are excluded at the outset; however, our goal in this evaluation was to use a real-world approach that could be replicated in clinical settings.
That is, we attempted to offer the program broadly with as few a priori exclusions as possible.
A second major reason for low participation rates was that 30% of those offered the intervention declined participation outright.
They offered several reasons for declining (Figure): lack of interest, feeling at an age for rest rather than physical activity, feeling already active enough, perceived ill health and consequent inability to be more active, depression,
unfamiliarity with the senior center, and uneasiness about having a telephone call from a stranger. Low participation also may have been related to cultural issues.
The third major reason for low participation was the 70% of those who agreed to participate were never reached by the study coordinator or
declined participation when reached. Reasons may have included moving from the area or a desire to please their PCP by agreeing to participate when they had no intention of doing so. Specific reasons
offered for declining when contacted by the PALS coordinator (Figure) were lack
of interest, too busy, other higher priorities, and difficulty understanding
English.
Participants who enrolled in PALS appeared to improve their level of physical activity. However, our numbers are small, so this finding should be interpreted with caution. Further study of the PALS model involving larger numbers of older adults
is warranted.
In addition to the small number of participants, our study has several other limitations, the most important of which derive from grafting a translational research project such as PALS onto a community clinics’ ongoing quality improvement effort. We were dependent on the PCPs’ routine clinical behavior. For this reason we did not have completed RAPA questionnaire scores on all eligible clients and so were unable to conduct an
intent-to-treat analysis of our physical activity measure. This contrasts with traditional research studies in which baseline levels of physical activity are assessed for all who agree to participate. Although the RAPA questionnaire was designed to be a simple, self-administered form, many patients needed assistance to complete it because of low literacy or
lack of fluency in
English. Clinic staff were often unable to assist because of other demands on their time.
These results indicate that a community-based program designed to increase physical activity may confront
substantial challenges when offered to ethnically diverse, low-income, elderly adults with diabetes, even when some identified barriers, such as fees for the EnhanceFitness program and lack of transportation, have been minimized. The impact of an ongoing quality assurance program to assess
physical activity in a primary care clinic population remains to be determined.
Other recent practice-based studies attempting similar translational research for other aspects of diabetes care have found little or no differences in outcomes, despite monitoring of key measures of quality of diabetes care with feedback to providers and patients and improvement in care processes. The lack of impact of these studies on key health outcomes may be related to the
usual attempt in translational research to reach a representative sample of the population under study rather than (as in
efficacy trials) a carefully selected subgroup that meets a clear set of inclusion and exclusion criteria (16).
Over time, as the importance of physical activity is repeatedly discussed, participation among
people who initially were uninterested in increasing physical activity may improve. If the goal of enhancing physical activity among the elderly is to be achieved, exploration of the barriers to activity among those who declined to participate in our program would be valuable information for
improving future programs.
Back to top
Acknowledgments
We extend special thanks to Marcus Rempel and Janelle Walhout, physician leaders with the Puget Sound Neighborhood Health Centers, for their involvement with and support of this project. This publication was supported by Cooperative Agreement Number 1-U48-DP-000050 from the Centers for Disease Control and Prevention.
Back to top
Author Information
Corresponding Author: Elizabeth A. Phelan, MD, MS, University of Washington Health Promotion Research Center, 1107 NE 45th Street, Suite 200, Box 354804, Seattle, WA 98105. Telephone: (206) 744-9112. E-mail: phelane@u.washington.edu.
Author Affiliations: Odette Batik, Puget Sound Neighborhood Health Centers, Seattle, Washington; Julie A. Walwick, Health Promotion Research Center, Department of Health Services, School of Public Health and Community Medicine, University of Washington, Seattle, Washington; Grace Wang, Puget Sound Neighborhood Health Centers, Seattle, Washington; James P. LoGerfo, Health Promotion Research Center, Department of Health Services, School of Public Health and Community Medicine, University of Washington, Seattle, Washington.
Back to top
References
- Taylor AH, Cable NT, Faulkner G, Hillsdon M, Narici M, Van Der Bij AK.
Physical activity and older adults: a review of health benefits and the effectiveness of interventions. J Sports Sci 2004;22(8):703-25.
- Larson EB, Wang L, Bowen JD, McCormick WC, Teri L, Crane P, et al.
Exercise is associated with reduced risk for incident dementia among persons 65 years of age and older. Ann Intern Med 2006;144(2):73-81.
- Kerse N, Elley CR, Robinson E, Arroll B.
Is physical activity counseling effective for older people? A cluster randomized, controlled trial in primary care. J Am Geriatr Soc 2005;53(11):1951-6.
- Schoenborn CA, Vickerie JL, Powell-Griner E.
Health characteristics of adults 55 years of age and over: United States, 2000-2003. Adv Data 2006(370):1-31.
- Arcury TA, Snively BM, Bell RA, Smith SL, Stafford JM, Wetmore-Arkader LK, et al.
Physical activity among rural older adults with diabetes. J Rural Health 2006;22(2):164-8.
- Daniel DM, Norman J, Davis C, Lee H, Hindmarsh MF, McCulloch DK, et al.
A state-level application of the chronic illness breakthrough series: results from two collaboratives on diabetes in Washington
state. Jt Comm J Qual Saf 2004;30(2):69-79.
- U.S. Preventive Services Task Force.
Behavioral counseling in primary care to promote physical activity: recommendation and rationale. Ann Intern Med 2002;137(3):205-7.
- Hooker SP, Seavey W, Weidmer CE, Harvey DJ, Stewart AL, Gillis DE, et al.
The California active aging community grant program: translating science into practice to promote physical activity in older adults. Ann Behav Med 2005;29(3):155-65.
- Hughes SL, Williams B, Molina LC, Bayles C, Bryant LL, Harris JR, et al.
Characteristics of physical activity programs for older adults: results of a multisite survey. Gerontologist 2005;45(5):667-75.
- Belza B, Walwick J, Shiu-Thornton S, Schwartz S, Taylor M, LoGerfo J. Older adult perspectives on physical activity and exercise: voices from multiple cultures. Prev Chronic Dis
2004;1(4).
http://www.cdc.gov/pcd/issues/2004/oct/04_0028.htm.
- Prohaska T, Belansky E, Belza B, Buchner D, Marshall V, McTigue K, et al.
Physical activity, public health, and aging: critical issues and research priorities. J Gerontol B Psychol Sci Soc Sci 2006;61(5):S267-73.
- Topolski TD, LoGerfo J, Patrick DL, Williams B, Walwick J, Patrick MB. The Rapid Assessment of Physical Activity (RAPA) among older adults. Prev Chronic Dis 2006;3(4).
http://www.cdc.gov/pcd/issues/2006/oct/06_0001.htm.
- Belza B, Shumway-Cook A, Phelan EA, Williams B, Snyder SJ, LoGerfo JP. The effects of a community-based exercise program on function and health in older adults: The EnhanceFitness Program. J Appl Gerontol 2006;25(4):291-306.
- Physical activity and health: a report of the Surgeon General. Atlanta
(GA): U.S. Department of Health and Human Services, Centers for Disease Control and
Prevention; 1996. http://www.cdc.gov/nccdphp/sgr/contents.htm. Accessed
September 15, 2007.
- Wilcox S, Dowda M, Griffin SF, Rheaume C, Ory MG, Leviton L, et al.
Results of the first year of active for life: translation of 2 evidence-based physical activity programs for older adults into community settings. Am J Public Health 2006;96(7):1201-9.
- Landon BE, Hicks LS, O'Malley AJ, Lieu TA, Keegan T, McNeil BJ, et al.
Improving the management of chronic disease at community health centers. N Engl J Med 2007;356(9):921-34.
Back to top
|
|
