Volume
8: No. 6, November 2011
Karen Hye-cheon Kim Yeary, PhD; Carol E. Cornell, PhD; Jerome Turner; Page Moore, PhD; Zoran Bursac, PhD; T. Elaine Prewitt, DrPH; Delia Smith West, PhD
Suggested citation for this article: Yeary KH, Cornell CE, Turner J, Moore P, Bursac Z, Prewitt TE, West DS. Feasibility of an evidence-based weight loss intervention for a faith-based, rural, African American population. Prev Chronic Dis
2011;8(6):A146.
http://www.cdc.gov/pcd/issues/2011/nov/10_0194.htm. Accessed [date].
PEER REVIEWED
Abstract
Background
African Americans and rural residents are disproportionately affected by obesity. Innovative approaches to address obesity that are sensitive to the issues of rural African Americans are needed. Faith-based and community-based participatory approaches show promise for engaging racial/ethnic minorities to change health outcomes, but few faith-based weight loss interventions have used a
community-based participatory approach.
Community Context
A faith-based weight loss intervention in the Lower Mississippi Delta arose from a 5-year partnership between academic and community partners representing more than 30 churches and community organizations.
Methods
Community and academic partners translated the 16 core sessions of the Diabetes Prevention Program for rural, church-going African American adults. The feasibility of the lay health advisor–led delivery of the 16-week (January-May 2010), 16-session, adapted intervention was assessed in 26 participants from 3 churches by measuring recruitment, program retention, implementation ease, participant outcomes, and program satisfaction.
Outcome
Twenty-two of 26 participants
(85%) provided 16-week follow-up data. Lay health advisors reported that all program components were easy to implement except the self-monitoring component. Participants lost an average of 2.34
kg from baseline to 16-week follow-up, for a mean weight change of −2.7%. Participants reported enjoying the spiritual and group-based aspects of the
program and having difficulties with keeping track of foods consumed. The intervention engaged community partners in research, strengthened community-academic partnerships, and built community capacity.
Interpretation
This study demonstrates the feasibility of delivering this adapted intervention by lay leaders through rural churches.
Back to top
Background
African Americans (1) and rural residents (2) are disproportionately affected by obesity. To combat health disparities, innovative approaches to address obesity that are sensitive to the issues of rural African Americans are needed. Current approaches acknowledge the potential impact of faith-based interventions (3,4) in rural African American communities. Although faith-based obesity interventions have been implemented with some success (4), studies have focused on urban settings and have
not used evidence-based behavioral weight loss methods. A community-based participatory research (CBPR) approach can inform the development of programs for African Americans that incorporate sociocultural factors associated with obesity (5) in the context of addressing health disparities. In a CBPR approach, community and academic partners contribute their insights and strengths to all aspects of the collaborative research process (6). However, few weight loss interventions for
racial/ethnic minorities have used CBPR (7). This article describes a CBPR faith-based weight loss intervention developed by a community-academic partnership representing the University of Arkansas for Medical Sciences (UAMS) and more than 30 churches and community organizations in the Arkansas Lower Mississippi Delta (LMD).
Back to top
Community Context
The WORD (Wholeness, Oneness, Righteousness, Deliverance) intervention took place in the Arkansas LMD, a rural region bordering the Mississippi River (8). Rates of chronic disease are higher in the LMD than in the rest of the nation (9), and LMD counties have higher rates of obesity than non-LMD counties (10). Moreover, racial/ethnic minorities living in the LMD have a higher prevalence of diabetes, obesity, and
high blood pressure compared with whites (10).
The WORD’s objective was to adapt an evidence-based weight loss intervention for a faith-based, rural population and to test the feasibility of its delivery by lay leaders to African American adults. Another objective was to use a CBPR approach in developing, implementing, and evaluating the intervention (Figure).
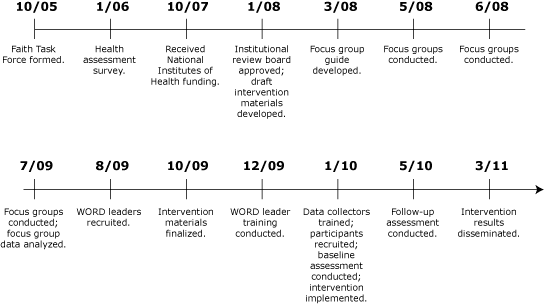
Figure. The WORD (Wholeness, Oneness, Righteousness,
Deliverance) Intervention Time Line, Arkansas,
2010. [A
text description of this figure is also available.]
Back to top
Methods
Community engagement
As an LMD pastor for 17 years, Pastor Jerome Turner had observed the poor health of the communities he served. Karen Hye-cheon Kim Yeary,
PhD, approached Pastor Turner in early 2005 to discuss forming partnerships with
faith communities to improve health. As a team, Pastor Turner and Dr Yeary met with a group of pastors and interested partners to create the Faith Task Force, which represents more than 30 African American and white LMD churches of various Protestant denominations, local
government agencies, community-based organizations, and UAMS. The Faith Task Force is a community-academic partnership that connects faith and health to improve the health of faith communities
(Appendix 1).
The WORD intervention development process
The Faith Task Force engaged a convenience sample of LMD churches to identify health concerns and programs implemented. Participant churches identified physical activity, nutrition, and obesity as primary health concerns. Although few churches had existing health promotion activities, all expressed interest in implementing a health program. On the basis of these findings, the Faith Task Force chose to focus The WORD on obesity and related health behaviors and to adapt the weight loss
intervention for African American adults, given the marked racial/ethnic health disparities in the area. The UAMS
Institutional Review Board approved the project.
Academic members of the Faith Task Force introduced evidence-based materials from the Diabetes Prevention Program (DPP) (11) and The WORD in North Carolina (7)
to develop the intervention. The DPP has produced significant weight loss and health improvements in African American populations (11). Academic and community partners worked together to culturally adapt the DPP curriculum using The WORD in North Carolina.
That study identified sociocultural
factors related to obesity in rural, church-going African American adults to create and pilot test a culturally appropriate weight loss intervention. The complex interactions between the economic, educational, and historical environment in rural areas, compounded by racial/ethnic disparities, may create a rural culture that reinforces negative health behaviors (2). The WORD in North Carolina identified aspects of rural culture such as the role of social networks and support that facilitate or
hinder health behaviors and spiritual ideas such as drawing strength from one’s faith to encourage positive health choices.
In adapting the DPP, community members of the Faith Task Force examined materials (eg, faith-based themes,
Scripture) and methods (eg,
lay health advisor model, group-based format) from The WORD in North Carolina and incorporated culturally appropriate components for their community to produce The WORD. Community partners also provided insider knowledge of
the rural African American faith culture to further adapt the intervention, including the addition of Bible studies and further
Scriptures. After Faith Task Force members said a broader focus on health would have more community appeal than an exclusive focus on weight loss, the Faith Task Force translated the intervention to emphasize healthy weight and related behaviors to prevent chronic disease.
The intervention was based on social cognitive theory (12) and social support and network models (13). The project placed greater emphasis on social environment dimensions of
social cognitive theory (peers, friends, family) than traditional behavioral weight control programs and engaged social relationships
by using a
lay health advisor model for weight loss promotion. Engaging and building on current social networks through the training of community members was hypothesized to lend to greater cultural sensitivity (ie,
spirituality, African American race, rurality). Likewise, the lay health
advisor model targets several components of social cognitive theory, including the trained community member as a model for observational learning and the ability of
lay health advisors to convey greater salience for behavior change to influence outcome expectations.
Focus groups
Focus groups were conducted to refine the program materials. Academic partners created an initial draft of the focus-group guide, which contained questions about the materials’ clarity, usefulness, appeal, and readability. Community partners then refined the guide.
Community Faith Task Force members led recruitment efforts for focus group
participants. Dr Yeary and Pastor Turner co-led 4 groups with pastors, Sunday school teachers, parishioners, and church leaders, in which draft intervention materials were presented and perceptions about the materials solicited.
Dr Yeary used the thematic analysis method to analyze the focus group data.
Dr Yeary and Pastor Turner discussed coding decisions and emergent findings until they reached an agreement
on common themes and codes (14). To ensure the credibility of inferences, the Faith Task Force reviewed and discussed the findings. Faith Task Force members revised the intervention and curriculum to incorporate the focus group findings and used the refined curriculum to examine the feasibility of delivering this faith-based weight loss program through churches in the Arkansas LMD.
Intervention feasibility testing
The WORD was conducted in 3 small, rural, African American churches in the LMD. Two churches whose pastors were members of the Faith Task Force volunteered to participate in the pilot intervention. The Faith Task Force recruited 1 additional church through word of mouth. The 3 churches represented 172 members, whose ages ranged from 1 to 91 years. An
estimated 135 members met the eligibility criteria (African American, aged
≥21 y, body mass index [BMI] ≥25 kg/m2, associated with a
participating church, no medical problems that would contraindicate
participation, not taking medication that would affect weight loss, and not
pregnant or lactating).
After extensive discussion within the Faith Task Force about suitable characteristics for WORD leaders, the pastor of each participating church identified potential candidates and invited them to an informational meeting. The recruitment goal was
6 WORD leaders (2 from each church). WORD leaders received a stipend for delivering the program.
WORD leaders received a 20-hour training that built knowledge about healthy
weight, weight-related health behaviors, faith and health, and behavioral
strategies through experiential learning. The training also included skills in
group facilitation and behavior change promotion. TurningPoint 2008 (Turning Technologies, Youngstown, Ohio) was used to facilitate interactive training and to assess WORD leaders’ knowledge and understanding of key concepts.
To complete the training, WORD leaders needed to score at least 80% on a final examination.
Participants
The study goal was to recruit 10 African American adults (BMI ≥25 kg/m²) per church, for a total of 30 participants. WORD leaders in collaboration with the Faith Task Force recruited participants through word of mouth, church announcements, and flyers. The Faith Task Force invited interested participants to an orientation visit, at which eligibility was confirmed and informed consent obtained. Participants received gift cards for completing assessments.
Intervention implementation and feasibility evaluation
Using the curriculum developed by the Faith Task Force, WORD leaders led small groups of parishioners in 90-minute weekly sessions to address faith and health, healthy eating, physical activity, behavioral strategies to achieve weight control, and overcoming barriers to change. Participants received self-monitoring diaries to record daily dietary intake, physical activity, and time with God between group sessions. WORD leaders reviewed the diaries weekly and returned them with feedback and
positive reinforcement.
Dr Yeary trained and certified 4 members of the Faith Task Force to collect self-report data during a 2-day, 8-hour training that incorporated didactic instruction and practice. Data collectors with previous training in the collection of anthropometric data used a Tanita scale
(Tanita Corporation, Tokyo, Japan) and a stadiometer to
measure the weight and height of all participants.
During a series of meetings, the Faith Task Force discussed which outcomes to assess. Academic partners then created a list of possible domains, offering several scale and item options for domains
that rely on self-report measurement. The Faith Task Force collaboratively selected the specific items to include in the evaluation. Trained community data collectors administered measures at baseline and 16-week follow-up that included demographics, body weight, and height to calculate
BMI (the primary outcome), and dietary, physical activity, and psychosocial measures. Physical activity was assessed
by using a 16-item checklist validated in African Americans. Frequency and duration of different types of activity permitted calculating data from the checklist on metabolic equivalent task (MET) hours per week (15). Percentage of calories from fat was assessed by the National Cancer Institute Quick Food Scan, which reported significant positive correlations between the scan and a
24-hour recall in a multisite community intervention trial that included a site consisting predominately of African Americans (16). Scales developed by Sallis et al (17,18) assessed self-efficacy (18) and social support (17) for healthy dietary and exercise behaviors.
ANOVA models examined the equality of means for baseline demographic, anthropometric, health behavior, and psychosocial variables between the 3 churches. To determine whether means for anthropometric, health behavior, and psychosocial variables differed significantly from baseline to 16-week follow-up, paired t tests
were used (SAS version 9.1, SAS Institute, Cary, North Carolina). Subgroup analyses examined outcomes among participants who engaged in most of the intervention
sessions.
WORD leaders completed a log at each intervention session to record
participant attendance and weight. Dr Yeary conducted open-ended interviews with WORD leaders after each intervention session to assess program implementation. Intervention questions asked about inclusion of different components of the intervention (eg,
educational component, self-monitoring, group exercise), ease or difficulty in
implementing intervention components, and how participants received the
intervention. Dr Yeary also observed 6 intervention sessions across the 3 churches and provided
constructive feedback to WORD leaders about their delivery. At 16-week
follow-up, Dr Yeary conducted semistructured interviews with program participants to assess program satisfaction. These interviews asked participants about their satisfaction with certain program components, aspects of the program they did or did not like, and recommendations for improvement. Indicators of program feasibility included meeting of
recruitment goals for WORD leaders and participants, retention of program participants, ease of implementation, significant
improvements in participant variables, and program satisfaction.
Back to top
Outcomes
Intervention development
Focus group participants (n = 36) confirmed the usefulness of linking faith and health through encouraging participants to draw strength from their faith to make positive health changes. Participants liked the inclusion of
Scripture from The WORD in North Carolina and proposed additional Scriptures.
They requested additional graphics in the materials and identified group exercises feasible for community members (eg, walking). The Faith Task Force used the focus group
data to refine the intervention materials.
The collaborative work by the Faith Task Force partners resulted in a 16-week curriculum consisting of adapted materials from the DPP (19) and The WORD in North Carolina (7). Each session included a lesson, a Bible study that connected faith with health, and group exercise. Sessions focused on goal setting and problem solving, with an emphasis on self-monitoring
(Appendix 2). The weight goal was 7% reduction of initial body weight, following the DPP. The program also provided DPP dietary
goals (25% calories from fat, 1.5 cups fruit/d, 2.5 cups vegetables/d, half of all starches as whole grains) and physical activity targets (150 min/wk) to help achieve the weight loss goal; participants
were encouraged to spend time with God at least 15 minutes per day.
Program feasibility testing
Eleven community residents were recruited and trained to serve as WORD leaders. All were African American
women aged 21 or older, and most were current or retired teachers, Sunday school teachers, and Bible study leaders. Seven of 11 recruited people completed the training.
A total of 35 participants were recruited from 12 churches; most (19 of 28 eligible participants) were from the 3 churches that agreed to be a part of the study. Seven recruited participants were ineligible and 2 withdrew before the program began, leaving 26 participants enrolled in the study
(Table 1).
No significant differences were noted in demographic and outcome variables of participants between the 3 churches. Retention rates were high; 22 of
the 26 enrolled participants provided 16-week follow-up data. Dropouts did not significantly differ from nondropouts in demographics or baseline BMI. On average,
13 participants attended each of the group sessions, and
21 of those enrolled attended at least half of all group sessions (Appendix
2).
Significant differences were reported in means for anthropometric, health behavior, and psychosocial variables from baseline to 16-week follow-up
(Table 2). Percentage of initial body weight lost from baseline to follow-up was 2.66% (median, −1.40%; IQR,
−6.57% to 0.69%) weight loss among program participants, translating to a mean weight loss of 2.34 kg (median, −1.36
kg; IQR, −4.99 kg to 0.64 kg). Participants significantly increased their total and moderately
vigorous physical activity during
the intervention period. Although changes in dietary intake were not significant from baseline to 16 weeks, program participants reported increased social support for healthy eating from family and friends and increased social support from family for physical activity.
We examined change over time (from baseline to 16-week follow-up) among participants who attended at least
8 of the 16 group sessions
(Table 3) to examine whether
more engaged participants (defined as attending at least 8 of 16 group sessions) had greater change in outcomes than those
who attended less than 8 of 16 group sessions. Engaged participants lost 4.5% of their initial weight on average and reported significantly
more moderately vigorous physical activity, greater encouragement to eat healthfully from family and friends, and greater encouragement to be physically active from family at follow-up. Weight loss averaged 4.04 kg
in the engaged group (median, −3.1 kg; IQR,
−6.8 kg to 0.05 kg) compared with 0.29 kg in the less engaged group
(median, −0.14 kg; IQR, −1.54 to 0.64 kg).
Participants enjoyed the group exercise sessions and the use of Scripture to promote health. Participants identified the group exercises and format of the program as sources of encouragement through providing opportunities for discussion and mutual learning.
They reported that the connection between faith and health motivated them to make positive behavior changes because it increased their confidence to make healthy choices, and provided an incentive to do well in the program to
show devotion to God.
Many participants said keeping track of their diets entailed too much writing and was overly time-consuming. Some participants did not complete their monitoring books; WORD leaders reported partial or incomplete reporting of foods consumed. Some participants had difficulty reading, writing, and looking up the nutritional content of foods. To encourage self-monitoring, WORD leaders incorporated interactive sessions in which participants brought in food labels and practiced self-monitoring. WORD leaders also
met with participants before intervention meetings and facilitated partnerships between participants and those in the congregation with more advanced reading and writing skills. Self-monitoring improved temporarily with these additional efforts, but WORD leaders reported decreased self-monitoring among participants as the program progressed.
Back to top
Interpretation
The WORD is one of the few faith-based weight loss interventions to use a CBPR approach. A CBPR approach was useful in recruiting
lay health advisors and in culturally adapting the intervention. Community data collectors accurately collected weight and height data but had difficulties collecting survey data, which had some missing data from interviewer error. Hiring data collectors with more experience may be beneficial in a larger trial. Using a CBPR approach also contributed to program
sustainability through building community capacity to conduct research; community partners submitted a community grant to continue the program in additional churches.
Study limitations include the use of self-report measures and participant difficulty in self-monitoring, although these limitations would have decreased the magnitude of the intervention’s effect. The sample was also a convenience sample.
Lay health advisors were successfully recruited through using a CBPR approach to collaborate with pastors; however, the recruitment goal for eligible participants was not met (goal, 30 participants; recruited, 26). Leading participant recruitment may be too burdensome for
lay health advisors, given their other responsibilities. More participants may have been recruited if Faith Task Force community members in addition to
lay health advisors led recruitment efforts. The program was feasible to implement with the exception of the
self-monitoring component, which required extensive writing. Self-monitoring that does not require writing, such as a checklist format, may produce greater adherence.
Positive changes in weight, physical activity, and social support for health behaviors were consistent in magnitude with other faith-based weight loss programs (7,20). Participants who were more engaged in the program demonstrated greater improvements in weight and physical activity, although even those who participated to a lesser extent showed some improvement. Evidence of The WORD’s feasibility in African American adults includes high participant retention, significant changes in
program outcomes, and positive participant evaluations of the program. A full-scale controlled trial will be needed to determine if the program was responsible for producing these health improvements. This study demonstrates the feasibility of delivering this adapted intervention by lay leaders through rural churches.
Back to top
Acknowledgments
We thank the Faith Task Force and the Boys, Girls, Adults Community Development Center. The project described was supported by award no.
P20MD002329 from the National Center on Minority Health and Health Disparities.
Back to top
Author Information
Corresponding Author: Karen Hye-cheon Kim Yeary, PhD, University of Arkansas for Medical Sciences, Department of Health Behavior and Health Education, 4301 West Markham St #820, Little Rock, AR 72205-7199. Telephone: 501-526-6720. E-mail:
khk@uams.edu.
Author Affiliations: Carol E. Cornell, Page Moore, Zoran Bursac, T. Elaine Prewitt, Delia
Smith West, University of Arkansas for Medical Sciences, Fay Boozman College of Public Health, Little Rock, Arkansas; Jerome Turner, Boys, Girls, Adults Community Development Center, Marvell, Arkansas.
Back to top
References
- Mokdad AH, Ford ES, Bowman BA, Dietz WH, Vinicor F, Bales VS, Marks JS.
Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA 2003;289(1):76-9.
- Health, United States, 2001 with urban and rural health chartbook. Hyattsville (MD): National Center for Health Statistics; 2001.
- Baskin ML, Resnicow K, Campbell MK.
Conducting health interventions in black churches: a model for building effective partnerships. Ethn Dis 2001;11(4):823-33.
- DeHaven MJ, Hunter IB, Wilder L, Walton JW, Berry J.
Health programs in faith-based organizations: are they effective? Am J Public Health 2004;94(6):1030-6.
- Kumanyika S. Obesity treatment in minorities. In: Wadden TA, Stunkard AJ, editors. Handbook of obesity treatment. New York (NY): Guilford Press; 2002. p. 416-46.
- Viswanathan M, Ammerman A, Eng E, Garlehner G, Lohr KN, Griffith D, et al.
Community-based participatory research: assessing the evidence. Evid Rep Technol Assess (Summ) 2004;(99):1-8.
- Kim KH, Linnan L, Campbell MK, Brooks C, Koenig HG, Wiesen C.
The WORD (Wholeness, Oneness, Righteousness, Deliverance): a faith-based weight loss program utilizing a participatory approach. Health Educ Behav 2008;35(5):634-50.
- McCloskey AH, Woolwich J, Holahan D. Reforming the health care system: state profiles, 1995. Washington (DC): American Association of Retired Persons; 1995. p. 20-104.
- Lower Mississippi Delta Nutrition Intervention Research Consortium. In: Harrison
G, editor. Nutrition and health status in the Lower Mississippi Delta of Arkansas, Louisiana, Missisippi: a review of existing data. Rockville (MD): Westat Inc; 1997.
- Smith J, Lensing S, Horton JA, Lovejoy J, Zaghloul S, Forrester I, et al.
Prevalence of self-reported nutrition-related health problems in the Lower Mississippi Delta. Am J Public Health 1999;89(9):1418-21.
- Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, Nathan DM.
Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346(6):393-403.
- Baranowski T, Perry CL, Parcel GS. How individuals, environments, and
health behavior interact: social cognitive theory. In: Glanz K, Rimer BK, Lewis
FM, editors. Health behavior and health education: theory, research, and practice. San Francisco (CA): Jossey-Bass; 2003.
- Heaney CA, Israel BA. Social networks and social support. In: Glanz K, Rimer
BK, Lewis FM, editors. Health behavior and health education: theory, research, and practice. San Francisco (CA): Jossey-Bass; 2003.
- Edstrom KM, Devine CM.
Consistency in women’s orientations to food and nutrition in midlife and older age: a 10-year qualitative follow-up. J Nutr Educ 2001;33(4):215-31.
- Campbell MK, James A, Hudson MA, Carr C, Jackson E, Oakes V, et al.
Improving multiple behaviors for colorectal cancer prevention among African American church members. Health Psychol 2004;23(5):492-502.
- Thompson FE, Midthune D, Williams GC, Yaroch AL, Hurley TG, Resnicow K, et al.
Evaluation of a short dietary assessment instrument for percentage energy from fat in an intervention study. J Nutr 2008;138(1):193S-9.
- Sallis JF, Grossman RM, Pinski RB, Patterson TL, Nader PR.
The development of scales to measure social support for diet and exercise behaviors. Prev Med 1987;16(6):825-36.
- Sallis JF, Pinski RB, Grossman RM, Patterson TL, Nader PL. The development of self efficacy scales for health-related diet and exercise behaviors. Health Ed Res 1988;3(3):283-92.
- The DPP Research Group.
The Diabetes Prevention Program (DPP): description of lifestyle intervention. Diabetes Care 2002;25(12):2165-71.
- Fitzgibbon ML, Stolley MR, Ganschow P, Schiffer L, Wells A, Simon N, Dyer A.
Results of a faith-based weight loss intervention for black women. J Natl Med Assoc 2005;97(10):1393-402.
Back to top
