 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Epilepsy Surveillance Among Adults --- 19 States, Behavioral Risk Factor Surveillance System, 2005Rosemarie Kobau, MPH1
Corresponding author: Rosemarie Kobau, MPH, Division of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC, 4770 Buford Hwy, N.E., MS K-51, Atlanta, GA 30347. Telephone: 770-488-6087; Fax: 770-488-5486; E-mail: rkobau@cdc.gov. AbstractProblem/Condition: Epilepsy is a brain disorder characterized by brief, recurrent disturbances in the normal electrical functions of the brain that result in seizures. Few population-based studies of epilepsy have been published for the United States, and the prevalence is expected to increase with the aging of the population. This is the first multistate study examining the prevalence of self-reported epilepsy and active epilepsy and includes an examination of socioedemographic and behavioral characteristics and of health-related quality of life among adults with epilepsy. Reporting Period Covered: Data from the 2005 Behavioral Risk Factor Surveillance System (BRFSS) are presented for 19 states. Description of System: BRFSS is an ongoing, state-based, random-digit--dialed telephone survey of the noninstitutionalized U.S. population aged >18 years. BRFSS collects information on health risk behaviors and preventive health services related to leading causes of death and morbidity. In 2005, 19 states included questions on epilepsy or seizure disorder. Results/Interpretation: During 2005, 1.65% of noninstitutionalized adults from 19 states reported that they had ever been told by a doctor that they had epilepsy or seizure disorder (i.e., a history of epilepsy); 0.84% reported having active epilepsy (i.e., a history of epilepsy and currently taking medication or reporting one or more seizures during the past 3 months), and 0.75% were classified as having inactive epilepsy (i.e., a history of epilepsy or seizure disorder but currently not taking medicine to control epilepsy and no seizures in the 3 months preceding the survey). No substantial differences among states in the prevalence of lifetime epilepsy, active epilepsy, or inactive epilepsy were detected. Prevalence estimates for active and inactive epilepsy revealed no significant differences by sex or race/ethnicity. Adults with a history of epilepsy and with active epilepsy were more likely to report fair or poor health, be unemployed or unable to work, live in households with the lowest annual incomes, and have a history of co-occurring disorders (e.g., stroke or arthritis). Adults with a history of epilepsy and with active epilepsy also reported significantly worse health-related quality of life. Adults with a history of epilepsy were more likely to be obese, physically inactive, and current smokers. Among adults with active epilepsy with recent seizures, 16.1% reported not currently taking their epilepsy medication, and 65.1% reported having had more than one seizure in the past month. Among adults with a history of epilepsy, 23.7% reported cost as a barrier to seeking care from a doctor within the past year. A total of 34.9% of adults with active epilepsy with seizures reported not having seen a neurologist or an epilepsy specialist (i.e., a neurologist who specializes in treating epilepsy) in the previous year. Public Health Action: Additional descriptive and analytic studies of epilepsy occurrence in diverse U.S. communities and populations are needed to better characterize epilepsy incidence rates, risk factors and etiologies, and types and severity, as well as epilepsy-associated conditions and disabilities. Community-based strategies that link health- care providers with social services such as public transportation, mental health services, and employment services might improve quality of life in persons with epilepsy. Implementing educational programs developed by CDC and the Epilepsy Foundation for schools, emergency responders, employers, providers, and the general public can increase awareness about epilepsy and reduce stigma associated with this disorder. IntroductionEpilepsy is one of the most common neurological disorders worldwide, affecting 50 million persons (1), including an estimated 2.1 to 2.7 million persons in the United States (2,3). The condition is a brain disorder characterized by recurrent, transient disturbances in the electrical functions of the brain that result in seizures. Signs and symptoms of seizures include sudden and transitory phenomena such as alterations of consciousness, or involuntary motor, sensory, autonomic, or psychic effects (3--5). Many persons with epilepsy also experience certain signs and symptoms immediately after seizures, such as memory impairment, fatigue, depressive symptoms, or anxiety (i.e., the postictal state) (6). Seizures are broadly classified into generalized, partial, and unclassifiable types, with additional subcategories; persons can experience more than one seizure type (4,5). Seizures and epilepsy result from many causes, including those that are preventable. Causes include traumatic brain injury, stroke, central nervous system (CNS) infections (e.g., meningitis and encephalitis), brain tumor, idiopathic causes presumed to be genetic, and others (5). Not all persons with seizures have epilepsy. Epilepsy is not diagnosed when seizures are provoked by acute and temporary conditions that affect brain function (e.g., fever, acute systemic metabolic disturbance, or alcohol withdrawal). Rather, a person receives a diagnosis of epilepsy only when seizures recur in the absence of such acute conditions and when any underlying pathological conditions, if identifiable, are chronic (4,5). Although persons of all ages can develop epilepsy, incidence rates are higher among young children and older adults because risk factors for epilepsy are more common in these age groups (2,3). Recurrent seizures often result in limitations in activities, depression, anxiety, and impaired quality of life and can increase risk for death (7--9). Misconceptions about epilepsy and its causes and consequences are prevalent, contributing to stigma associated with the condition and increasing challenges for persons living with this disorder (1,8--12). Texas, Georgia, Tennessee, and South Carolina were among the first states to use the state-based BRFSS to assess state-level epilepsy prevalence using five standardized questions developed by the CDC Epilepsy Program (13--17). In 2003 and 2005, CDC, in partnership with the University of California, Los Angeles, used the California Health Interview Survey (CHIS) to assess epilepsy prevalence in California (16). Although case definitions differed among these state studies depending on the questions used, lifetime prevalence estimates ranged from 1.2% to 2.6%, and prevalence estimates for active epilepsy ranged from 0.7% to 1.6% (13--16). With CDC financial and technical support, local foundation affiliates of the national Epilepsy Foundation worked with state departments of public health to incorporate at least one of five standardized epilepsy questions into the 2005 Behavioral Risk Factor Surveillance System (BRFSS). Nineteen states accepted one or more questions. This study is the first to examine the prevalence of self-reported epilepsy in these states and the prevalence of active epilepsy in some states. Sociodemographic and behavioral characteristics, health-related quality of life (HRQOL), and life satisfaction of persons by epilepsy status also were examined. MethodsBRFSS is an ongoing, state-based, random-digit--dialed telephone survey of the civilian, noninstitutionalized population aged >18 years that tracks the prevalence of key health and safety-related behaviors and characteristics (18). The questionnaire consists of three parts: 1) core questions asked in all 50 states, the District of Columbia, and three territories; 2) supplemental modules (i.e., a series of questions on a specific topic such as arthritis, diabetes, or depression); and 3) state-added questions. Each state decides which supplemental modules and state-added questions to include in its BRFSS survey. BRFSS also includes standardized questions on sociodemographic and behavioral characteristics and self-reported chronic diseases. The complete BRFSS survey is available at http://www.cdc.gov/brfss (18). BRFSS data are weighted to reflect the age, sex, and racial/ethnic distribution of the state's estimated population during the survey year. Twelve states included all five epilepsy questions as state-added questions in their 2005 BRFSS questionnaire; one state included three questions; four states included two questions; and two states included one question.* The first question was, "Have you ever been told by a doctor that you have a seizure disorder or epilepsy?" (response options: "yes," "no," "don't know," and "refused"). Participants who answered "yes" to this question were asked some or all of the remaining questions: 2) "Are you currently taking any medicine to control your seizure disorder or epilepsy?" (response options: "yes," "no," "don't know," and "refused"); 3) "How many seizures have you had in the last 3 months?" (response options: "none," "one," "more than one," "no longer have epilepsy or seizure disorder," "don't know," and "refused"); 4) "In the past year, have you seen a neurologist or epilepsy specialist for your epilepsy or seizure disorder?" (response options: "yes," "no," "don't know," and "refused"); and 5) "During the past 30 days, to what extent has epilepsy or its treatment interfered with your normal activities like working, school, or socializing with family or friends?" (response options: "not at all," "slightly," "moderately," "quite a bit," "extremely," "don't know," and "refused"). The lifetime prevalence (i.e., cumulative incidence) of self-reported epilepsy was determined by affirmative responses to the first question. Respondents were classified as having active epilepsy if they responded "yes" to ever having been told by a doctor that they had a seizure disorder or epilepsy and also responded that they either were currently taking medication to control it, had one or more seizures in the past 3 months, or both (Figure). Active epilepsy was further categorized by whether the respondent had experienced a seizure in the past 3 months (i.e., active epilepsy with or without recent seizures). Respondents who responded that they had ever been told by a doctor that they had a seizure disorder or epilepsy (i.e., had a history of epilepsy) but were not taking medication for epilepsy and had not had a seizure in the past 3 months† were classified as those with inactive epilepsy (Figure). HRQOL was measured for all respondents, with and without a history of epilepsy, with the following validated CDC Healthy Days questions (19): 1) "Now thinking about your physical health, which includes physical illness and injury, for how many days during the past 30 days was your physical health not good?" 2) "Now thinking about your mental health, which includes stress, depression, and problems with emotions, for how many days during the past 30 days was your mental health not good?" and 3) "During the past 30 days, for about how many days did poor physical or mental health keep you from doing your usual activities, such as self-care, work, or recreation?" CDC methods for calculating HRQOL were used (19). In addition, all respondents were asked to respond to a question on self-rated health: "Would you say that in general your health is excellent, very good, good, fair, or poor?" Responses for self-rated health were classified into two groups for analysis: 1) excellent, very good, or good and 2) fair or poor. Statistical software was used to account for the complex survey design. Data were weighted to obtain appropriate population estimates, standard errors, and 95% confidence intervals (CIs). Estimates were considered significantly different if CIs did not overlap. The total eligible number of BRFSS respondents among all 50 states was 556,117 adults; the median refusal rate was 14.4% (20). The Council of American Survey Organizations (CASRO) response rates among the 19 states for the 2005 BRFSS survey ranged from 40.0% (New York) to 63.1% (Kansas) (median among 19 states: 51.1%); cooperation rates§ among respondents ranged from 67.6% (New York) to 85.0% (Tennessee) (median among 19 states: 76.9%) (20). ResultsPrevalenceA total of 2,207 adults from 19 states (1.65%, CI = 1.52--1.80) reported ever being told they had epilepsy (i.e., a history of epilepsy) (Table 1). Among 13 states that included three questions sufficient to classify epilepsy status, 919 (0.84%; CI = 0.74--0.96) were classified as having active epilepsy, and 693 (0.75%; CI = 0.65--0.86) were classified as having inactive epilepsy (Table 1). Some significant differences in prevalence were detected between states (e.g., Delaware and Wyoming, New York and Washington). Characteristics of Adults with a History of EpilepsyOf persons ever told they had epilepsy (i.e., persons with a history of epilepsy), 55.9% were women, and half were aged 35--44 (22.0%) to 45--54 years (22.7%); in addition, 74.1% were white, 8.8% were black, 11.2% were Hispanic, and 6.0% were of another race/ethnicity (Table 2). Compared with those without the disorder, a greater percentage of adults with a history of epilepsy had lower levels of education and income. A smaller percentage of persons with a history of epilepsy were married or part of an unmarried couple and a greater percentage were formerly married compared with those without the disorder. A smaller percentage of persons with a history of epilepsy were employed (45.8%) and a greater percentage (23.7%) were unable to work than those without epilepsy (61.6% and 4.8%, respectively) (Table 2). Nearly the same percentages of those with (17.0%) and without (16.3%) a history of epilepsy did not have health-care insurance. However, 23.7% of those with a history of epilepsy reported not being able to see a doctor in the past year because of the cost, compared with 13.4% of those without the disorder. A total of 69.0% of persons with a history of epilepsy reported having a checkup within the past year, a proportion similar to that in the general population. A significantly greater percentage of persons with a history of epilepsy were classified as obese compared with those with no history of epilepsy (30.1% versus 24.0%, respectively). A greater percentage of persons with a history of epilepsy were current smokers compared with those without the disorder (30.1% versus 20.9%, respectively) (Table 2). A total of 33.5% of persons with a history of epilepsy reported no exercise in the past 30 days compared with 24.5% of those without the disorder, and 37.0% of persons with a history of epilepsy reported fair or poor health, compared with 15.8% of those without the disorder (Table 2). In addition, 13.6% of those with a history the disorder reported rarely or never receiving the emotional support they needed, compared with 8.0% of those without the disorder (Table 2). A total of 16.6% of those with a history of epilepsy reported being dissatisfied or very dissatisfied with their life, compared with 5.4% of those without the disorder (Table 2). Classification of Active and Inactive EpilepsyAmong adults with a history of epilepsy, 48.8% reported currently taking medication to control their disorder (Table 3). Of those with a history of epilepsy, 15.0% reported having more than one seizure in the past 3 months; 8.1% had one seizure, and 71.0% had no seizures in the past 3 months (Table 3). A total of 5.9% of those with a history of epilepsy reported no longer having the disorder (self-determined) in response to the question on seizure frequency (Figure, Table 3). Of those classified with active epilepsy, 55.1% reported having had no seizures in the past 3 months, 15.3% reported one seizure, and 28.6% reported more than one seizure; in addition, 6.9% of those classified with active epilepsy reported not taking medication for their seizure disorder but having had recent seizures. Although 1.0% of adults with active epilepsy reported no longer having the disorder, they were classified as having active epilepsy because they also reported currently taking medication (Figure, Table 3). Among adults with active epilepsy and recent seizures, 16.1% reported not taking medication for their disorder, and 34.9% reported having had one seizure in the past 3 months, with 65.1% having had more than one seizure (Table 3). A total of 34.9% of adults with active epilepsy with recent seizures reported not seeing a neurologist or epilepsy specialist in the past year (Table 3). Among adults with active epilepsy and no recent seizures, 40.6% reported not having seen a neurologist or epilepsy specialist in the past year. Among persons with active epilepsy with recent seizures, 32.9% reported that epilepsy or its treatment limited their abilities in the past month "quite a bit or extremely" compared with 7.6% among those with no recent seizures. Characteristics of Adults Classified with Active EpilepsyPrevalence estimates for active and inactive epilepsy reveal no differences by sex or race/ethnicity (Table 4). Differences in prevalence occurred by age (e.g., 35--54 years versus 18--24 years); however, these differences should be interpreted with caution because of the small sample sizes in certain age groups. Among persons with active epilepsy, 56.4% were women, and half were aged 35--54 years (22.1% aged 35--44 years, 26.1% aged 45--54 years) (Table 5). A total of 80.4% of adults with active epilepsy were white, 11.0% were black, and 5.5% were Hispanic. A significantly greater percentage of those with active epilepsy reported not completing high school, compared with adults without the disorder, and a smaller percentage of adults with active epilepsy reported having some college education (Table 5). Similar percentages with respect to educational attainment occurred among those with inactive epilepsy. A total of 47.7% of adults with active epilepsy and 40.7% of those with inactive epilepsy reported an annual household income of <$25,000, compared with 26.5% of adults without the disorder. A significantly smaller percentage of persons with active epilepsy were married or part of an unmarried couple than those without the disorder, and a greater percentage of those with active epilepsy were formerly married compared with those without the disorder (Table 5). Among adults with active epilepsy, 9.8% were unemployed, compared with 5.4% in those without a history of epilepsy. A total of 31.3% of those with active epilepsy and 15.4% of those with inactive epilepsy reported being unable to work, compared with 4.9% of those without the disorder (Table 5). Fair or poor health was reported by 48.5% of adults with active epilepsy and 28.5% of those with inactive epilepsy, both significantly more than the 15.8% of adults without the disorder (Table 6). A significantly greater percentage of adults with inactive epilepsy reported not having health-care insurance (23.9%) compared with those with active epilepsy (10.9%) or those without the disorder (14.1%). From 63.1% to 71.5% of adults in these three groups reported having had a checkup within the past 2 years. However, a significantly greater percentage of adults with active epilepsy reported not being able to see a doctor in the past 12 months because of the cost. A total of 32.2% of adults with active epilepsy and 31.9% of those inactive epilepsy were classified as obese, compared with 23.3% of adults without the disorder (Table 6). A significantly smaller percentage of adults with active epilepsy (60.7%) reported any exercise in the past 30 days compared with adults without the disorder (75.4%). Among those with active epilepsy or inactive epilepsy, 32.4% and 32.0% were current smokers, respectively, compared with 21.6% of those without the disorder. A smaller percentage of adults with active epilepsy (30.4%) reported drinking any alcohol in the past month than those without the disorder (53.4%). A greater percentage of adults with active epilepsy (15.7%) and inactive epilepsy (7.3%) reported having had a stroke than those with no history of the disorder (2.4%). Eight percent of adults with active epilepsy reported having heart disease, compared with 4.8% of those with inactive epilepsy. Twenty percent of adults with active epilepsy reported having asthma, approximately twice the proportion among those with inactive epilepsy or without the disorder. A greater percentage of adults with active epilepsy (13.0%) and inactive epilepsy (14.9%) reported being told they had diabetes compared with those with no history of the disorder (7.7%). A significantly greater percentage of adults with active epilepsy or inactive epilepsy reported being told they had arthritis and reported current joint pain than those without the disorder (Table 6). A total of 21.6% of adults with active epilepsy reported getting the recommended 5 servings of fruits and vegetables a day, similar to those with inactive epilepsy (27.4%) and those without the disorder (26.4%). Approximately the same percentages of adults with and without the disorder reported receiving a flu shot in the past year. A significantly greater percentage of adults with active epilepsy reported rarely or never getting the emotional support they needed (19.1%) than those without the disorder (7.6%). In addition, a greater percentage of those with active epilepsy were dissatisfied or very dissatisfied with their life (18.8%) than those without the disorder (5.7%) (Table 6). Sex and age were not associated with increased or decreased risk for active epilepsy with recent seizures (Table 7). However, a significantly greater percentage of Hispanics (79.2%) reported recent seizures than did whites (40.0%), and a greater percentage of persons with active epilepsy at the lowest annual household income level (57.3%) reported recent seizures than persons with epilepsy at the highest annual household income level (20.9%). Similarly, a greater percentage of adults with active epilepsy who were unemployed or unable to work (59.2%) reported recent seizures than adults with epilepsy who were employed (33.2%) or other groups (33.5%). Health-Related Quality of LifeCompared with adults with no history of the disorder, adults with a history of epilepsy reported significantly more mentally unhealthy days (7.3 versus 3.2), physically unhealthy days (9.1 versus 3.5), overall unhealthy days (13.0 versus 5.9), and activity-limitation days (6.8 versus 2.1) (Table 8). Compared with those with no history of epilepsy, adults with active epilepsy reported significantly more mentally unhealthy days (9.3 versus 3.4), physically unhealthy days (10.7 versus 3.6), overall unhealthy days (15.1 versus 6.1), and activity-limitation days (8.4 versus 2.2) (Table 8). Similarly, adults with inactive epilepsy reported more mentally unhealthy days, physically unhealthy days, overall unhealthy days, and activity-limitation days than those with no history of the disorder (Table 8). Adults with active epilepsy with recent seizures reported significantly more physically unhealthy days than those with no recent seizures (13.1 versus 8.8) and more activity-limitation days (11.1 versus 6.4) than those with no recent seizures. DiscussionPopulation-based epidemiological studies of epilepsy are important for policymakers and health-care providers to plan and provide prevention programs and appropriate care and services for those affected (1,10). Adults with a history of epilepsy and with active epilepsy were more likely to report negative health outcomes, and they face substantial socioeconomic disadvantages such as unemployment and low household income. In addition, these findings highlight the substantial adverse effects of recurring seizures on daily activities and HRQOL in adults with epilepsy. However, because of the cross-sectional nature of BRFSS, no causality among the associations found can be inferred. Although prevalence estimates differed among certain states, these differences might have been a result of random error associated with response rates, response bias, or multiple comparisons. The estimates of persons who were ever told they had epilepsy (i.e., lifetime prevalence) and active epilepsy are comparable to previous estimates from the 1998 Texas BRFSS (lifetime prevalence, 1.8%), 2002 Georgia BRFSS (lifetime prevalence, 1.7%), and 2003 and 2004 South Carolina BRFSS surveys (lifetime prevalence, 2.2%; active epilepsy, 1.1%) and with estimates from the 2003 CHIS (lifetime prevalence, 1.2%; active epilepsy, 0.7%) (13--16). The active epilepsy estimate of 0.8% also is comparable to results from a recent study of a managed care population (0.7%); a 1978 door-to-door survey of all household and institutionalized residents in Copiah County, Mississippi (1%); and a community-based study of diagnostic records for 5 decennial census years in Minnesota (0.7%) (21--23) Despite methodologies that differed from those used in other studies, self-reports of medication use and seizure frequency from this study were comparable to findings from the 2003 CHIS (16), the 2003 and 2004 South Carolina BRFSS surveys (14), the 2004 HealthStyles Survey (17), and Copiah County, Mississippi (22). For example, in California, 10% of adults with active epilepsy reported not taking any medication for their seizure disorder, and 29% reported having had more than one seizure during the past 3 months (16). The finding in this report that epilepsy prevalence was lower among older adults differs from findings in other studies that have shown an increased prevalence with increased age (23); however, this study excluded institutionalized older adults from BRFSS, which might have resulted in the lower estimate. Like this study, other U.S. studies have not found consistent differences in the prevalence of epilepsy by sex or by race (15--17,22--26). Findings from this study regarding educational attainment, employment, marital status, and household income among persons with a history of epilepsy are comparable to those from other U.S. studies based on convenience samples of persons with epilepsy and with longitudinal studies in Canada and Europe (27--29). Researchers who conducted cohort studies of children with epilepsy found a higher prevalence of psychosocial problems, unemployment, and financial dependency and lower levels of education at adulthood compared with controls and suggested that ongoing psychosocial support is needed for children with epilepsy as they transition into adulthood (27). The higher percentages of adults with epilepsy at lower levels of education and income in this study are consistent with findings from the 2002 Georgia BRFSS and 2002 Tennessee BRFSS, which found that 22% of adults with a history of epilepsy did not complete high school and 44% had an annual household income of <$25,000; in addition, in the 2003 CHIS, 45% of Californians with epilepsy reported an annual household income <$25,000 (15,16). However, the results of this study indicate that although nearly half of adults with active epilepsy in 2005 had completed some college or more, many of these adults remained at lower household income levels. For example, 32% (CI = 22.7--42.7) of adults with active epilepsy who either had some college experience or completed college reported an annual household income of <$25,000, although only 15% (CI = 14.5--15.9) of adults with no history of the disorder and comparable education reported an income of <$25,000. Epilepsy and its treatment can impair cognition, limiting academic achievement in some students with epilepsy (30,31), which might contribute to the lower educational attainment among adults with epilepsy. Lower levels of household income might be associated with periods of unemployment, disability status, or other factors unaccounted for in this study. Because these data are cross-sectional, no causal associations between epilepsy and lower levels of education and income can be inferred. The finding of lower rates of marriage and partnership in this analysis among adults with a history epilepsy is similar to findings from the 2003 CHIS, in which only 45% of adults with epilepsy were married, compared with 55% of adults without the disorder (16). This might result from decreased social opportunities among some persons with epilepsy (e.g., from limited access to transportation or to certain educational or occupational opportunities) or from stigma associated with the disorder (11,32). In addition, a higher percentage of adults with a history of epilepsy reported being formerly married compared with those without the disorder, which might be a result of the challenges of living with a chronic condition and the strain it might have on close relationships (33,34). Higher rates of divorce were found among persons with a history of epilepsy who did not disclose their epilepsy before marriage (35,36) and among those whose seizures had remitted (37). Persons with a history of epilepsy and active epilepsy are more likely than those without such histories to be obese, physically inactive, and current smokers (15,16). The stress of living with a chronic disorder such as epilepsy, including its social limitations, might encourage unhealthy coping behaviors (e.g., smoking and poor diet) and discourage healthy behaviors (e.g., physical activity). Persons with a history of epilepsy experience more depression and anxiety than those without the disorder; these common comorbid conditions are associated with unhealthy coping behaviors (38--40). In addition, certain anticonvulsant medications can cause sedation and lethargy, which might impede physical activity, whereas others can stimulate appetite, resulting in weight gain (41,42). Although persons with epilepsy historically have been discouraged from participating in physical activity because of concerns about inducing seizures or sustaining injuries associated with seizures, physical activity can improve seizure control, mood, and quality of life (43,44). Although persons with epilepsy should avoid physical injuries, many can benefit from daily physical activity such as walking (44--46). The higher reported prevalence of obesity, physical inactivity, and current smoking among persons with a history of epilepsy might be a factor in the higher reported prevalence of self-reported heart disease, stroke, diabetes, and arthritis among these persons. In addition, certain underlying brain disorders can lead to decreased mobility and epilepsy. Other studies have found higher prevalence of comorbid illnesses in persons with epilepsy compared with the general population (47,48). Epilepsy and its treatment have been associated with co-occurring disorders and disease risk factors (e.g, cerebrovascular and cardiovascular disorders, obstructive sleep apnea, and depression) (47--58). Because certain comorbid conditions might occur before epilepsy onset, occur simultaneously with epilepsy onset, or result from the condition or its treatment, additional studies are required to identify causal associations and shared disease pathways (47--58). Physicians treating persons with epilepsy should screen for and treat these chronic disease comorbidities and their risk factors (58,59). When recommending treatment options, health-care providers also should consider the effects of antiepileptic drugs on risk factors (e.g., weight gain, mood disorders, and sleep problems) and health status (41,42,57,60,61). In addition, general health-promotion information (e.g., smoking cessation, physical activity and healthy diet, and heart disease prevention) might be useful for providers and Epilepsy Foundation affiliates to distribute to patients with epilepsy. The findings in this study regarding inadequate seizure control by medications might partly be a result of limited knowledge of current diagnostic and treatment standards for the care of epilepsy among certain groups of health care professionals (62,63). Clinical tools and guidelines recommended for epilepsy care are available to improve clinical evaluation and services for patients with epilepsy (59,64,65). Inadequate seizure control might also arise, in part, from the difficulties with maintaining therapy regimens. Epilepsy medication regimens typically require multiple daily doses (and sometimes multiple drugs) that must be taken consistently; patients can have difficulty strictly adhering to these requirements, resulting in seizure recurrence. Lapses in treatment adherence also might arise among patients with discontinuous or inadequate health insurance coverage when such patients are unable to afford medication. Finally, nearly 40% of epilepsy cases with partial seizures are considered refractory (i.e., resistant to medical therapy), resulting in occasional or frequent seizure recurrences despite optimal treatment with antiepileptic drugs (64). Persons with epilepsy might have difficulties finding and navigating through health-care and public services that could be helpful. Collaborative care models such as the chronic care model (66--69) also might improve health outcomes for persons with epilepsy. For example, the Awareness and Access to Care for Children and Youth with Epilepsy (AACYE) initiative focuses on timely clinical follow-up care with medical specialists, including screening and referral for behavioral and mental health needs, and an individualized patient- and family-centered care plan (70). Community-based strategies (e.g., that include public transportation or telemedicine) that provide hard-to-reach persons with epilepsy with access to social services might also be helpful; these strategies have been effective for persons with complex chronic conditions (71--73). Adults with a history of epilepsy reported substantially worse self-rated health and HRQOL, more dissatisfaction with emotional support received, and more overall dissatisfaction with life than adults without the disorder. Depression has been shown to be one of the strongest predictors of quality of life in persons with epilepsy (64). Although this analysis could not control for confounding effects of depression on HRQOL, a recent similar study found that adjusting for covariates such as race/ethnicity and income and chronic disease comorbidity made no difference in HRQOL estimates in persons with self-reported epilepsy or active epilepsy (16). Adults with inactive epilepsy also reported worse HRQOL than those without the disorder, consistent with previous findings (14,16). A diagnosis of epilepsy earlier in life, despite its resolution or remission, can still interfere with later life opportunities and alter perceptions of health status (27,74--76). In addition, some persons with epilepsy who achieve a reduction in number of seizures or complete seizure remission continue to experience psychosocial distress associated with unmet or unrealistic life expectations (76). The results of this study are subject to at least seven limitations. First, the data are self-reported and subject to recall bias and response bias. However, the estimates collected for several years are in general agreement, indicating these types of bias might be minimal (13--17). Second, because the survey is cross-sectional, no causal associations among variables can be inferred. Third, the reported cases of epilepsy are not classified by seizure type, severity, or etiology, and certain acute symptomatic seizures or nonepileptic seizures (NESs) might have been misclassified as epilepsy. However, given the small percentages of adults with NESs, significant skewing of results because of these cases is unlikely (77). In addition, many adults with NESs also have epileptic seizures, making such distinctions less likely to substantially skew results (78,79). Fourth, the higher number of days of impaired HRQOL in persons with inactive epilepsy compared with those without the disorder might also have resulted from the case definition, which was based on a 3-month recall period for seizure frequency and is more conservative than the 5-year recall period recommended by the International League Against Epilepsy (ILAE) (4). Thus, some inactive cases in this study would have been classified as active cases using the ILAE definition. The case definition in this study was used to minimize difficulties in respondent recall of potentially numerous seizures over a lengthy interval, whereas the ILAE approach is designed for epidemiologic studies based on record review. Fifth, the analysis was unable to control for the possible effects of mood disorder on HRQOL in this study. Investigators might be able to do so in future BRFSS studies using data from states that included the Patient Health Questionnaire Survey or the Kessler-6 Psychological Distress scale along with the epilepsy questions (18). Sixth, epilepsy prevalence might be underestimated because of underreporting resulting from the stigma associated with disclosing epilepsy and because BRFSS methodology excludes institutionalized adults. Finally, BRFSS excludes households without landline telephones. However, the National Center for Health Statistics found that the percentage of households without landline phones is still low, and bias for persons who used cellular telephones exclusively was associated with select sociodemographic factors (80). CDC-supported Prevention Research Centers (PRCs) are conducting community-based research on self-management and depression prevention to improve health outcomes in persons with epilepsy (81--83). Pilot testing of WebEase (Web Epilepsy Awareness, Support, and Education), an Internet-based program that is focused on behavioral change theory and tailored communication strategies, found significant improvements in overall self-management and other health outcomes among adults with epilepsy (84,85). Although this study identified effects of epilepsy on persons in several states, additional descriptive and analytic studies of epilepsy occurrence in various U.S. communities and populations are needed. CDC is supporting the development of international standards for studies of epilepsy incidence and prevalence. Such research will better characterize epilepsy incidence rates, risk factors and etiologies, types, severity, associated conditions, and disability (1,10). The Association of State and Territorial Chronic Disease Directors endorsed a role for state public health departments in developing epilepsy surveillance capacity and establishing strong working relationships with other government agencies and with nongovernmental lay and professional groups (86). State and local public health agencies can work with their local Epilepsy Foundation affiliates, other groups such as the Epilepsy Therapy Project (available at http://www.epilepsy.com) that support persons with epilepsy and their families, and social service agencies to promote awareness and reduce social stigma, provide community and professional education about epilepsy, address employment and transportation needs, and provide referral and support for health promotion and disease prevention for persons with epilepsy (86--91). References
Acknowledgments The findings in this report are based, in part, on contributions by the following BRFSS state system coordinators: Brian A. Bender, MBA, Arizona; Fred Breukelman, Delaware; Melissa Murray, MS, Florida; Leah Bryan, MPH, Georgia; Farooq Ghouri, MBBS, MPH, Ghazala Perveen, PhD, Kansas; Tracy Sparks, Kentucky; Ann Rafferty, PhD, Michigan; Janet S. Wilson, MEd, MPA, Missouri; Susan Knight, MPH, New Hampshire; Colleen Baker, New York; Kathryn E. Pickle, Renee K. Boyd, Oregon; Robert F. Dewar, Pennsylvania; Jennifer Chiprich, PhD, South Carolina; David Ridings, Tennessee; Michelle Cook, MPH, Texas; Susan K. Spain, Virginia; Katrina Wynkoop Simmons, PhD, Washington; Anne Ziege, PhD, Wisconsin; and Menlo Futa, Wyoming; and by Laurie Elam-Evans, PhD, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC.
* All five questions: Arizona, Delaware, Georgia, Michigan, Missouri, New York, Oregon, Pennsylvania, South Carolina, Tennessee, Washington, and Wyoming; three questions: Kentucky; two questions: Florida, Texas, Virginia, and Wisconsin; one question: Kansas and New Hampshire. † Including those who responded "no longer have epilepsy" to the seizure frequency question. § The percentage of persons who completed interviews among all eligible persons contacted. Table 1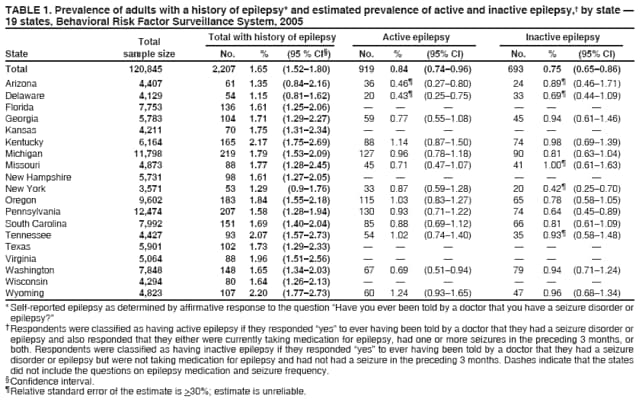 Return to top. Table 2 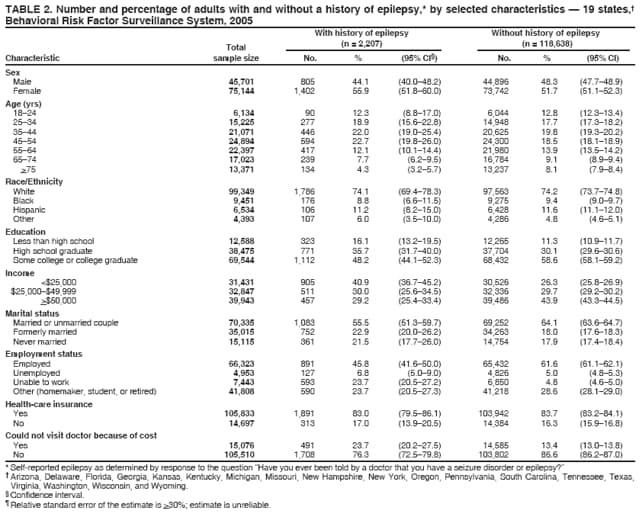 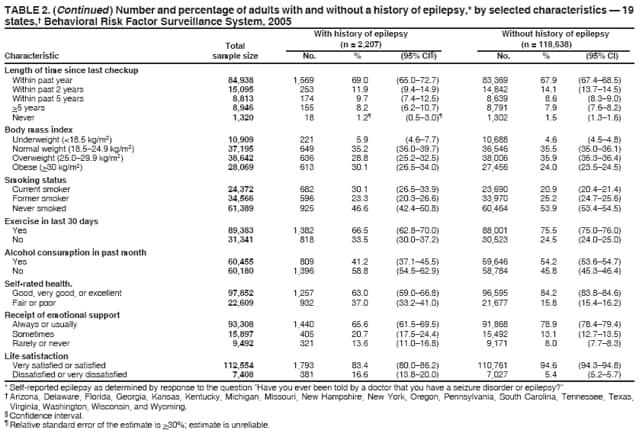 Return to top. Table 3 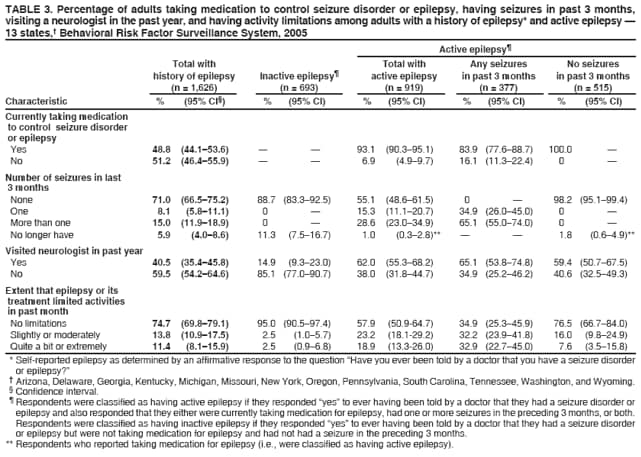 Return to top. Table 4 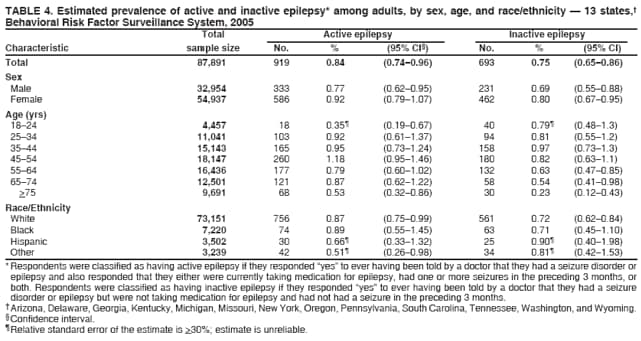 Return to top. Table 5 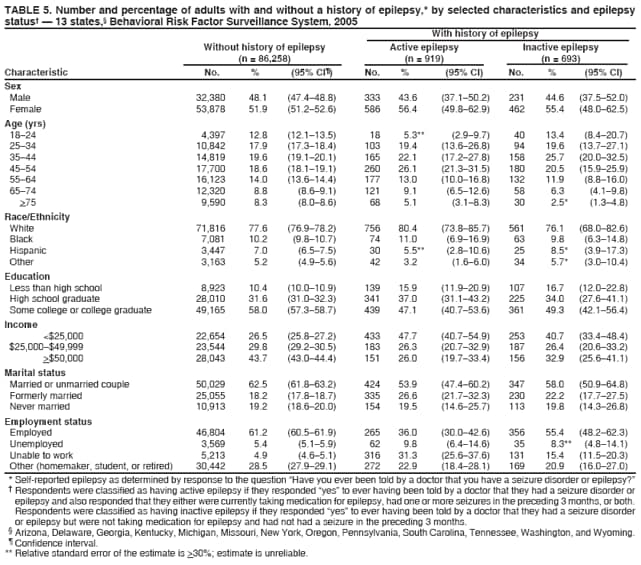 Return to top. Table 6 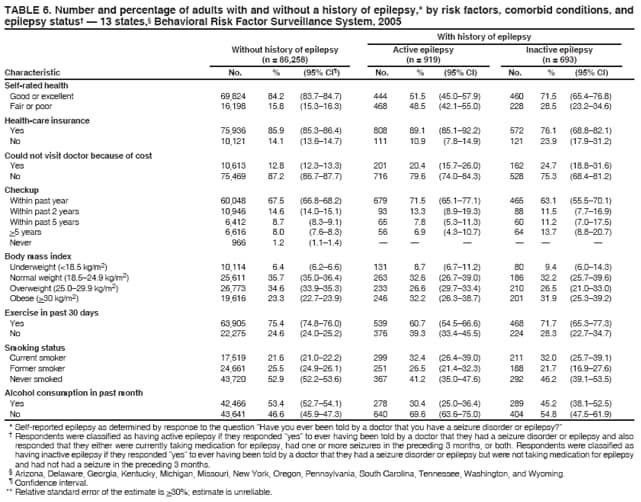 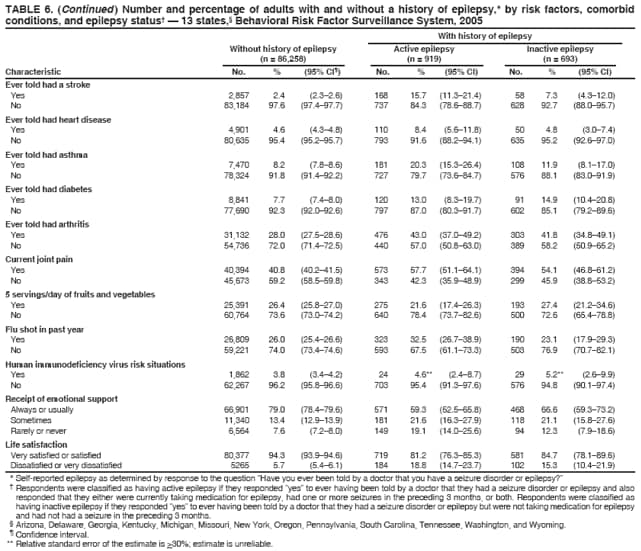 Return to top. Table 7 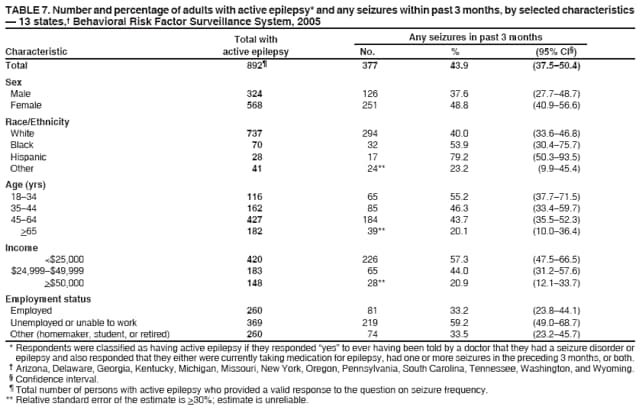 Return to top. Table 8 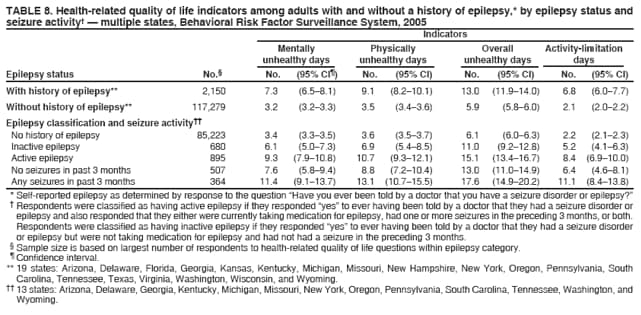 Return to top. Figure 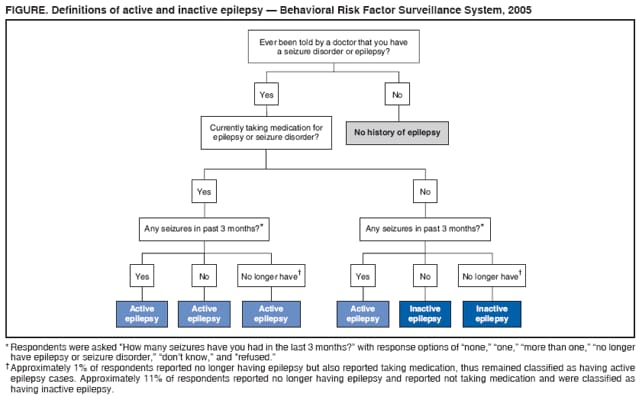 Return to top.
All MMWR HTML versions of articles are electronic conversions from typeset documents. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Date last reviewed: 7/23/2008 |
|||||||||
|