 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Giardiasis Surveillance --- United States, 1998--2002Michele C. Hlavsa, MPH1,2 Corresponding author: Michael J. Beach, PhD, Epidemiologist, CDC/NCID/DPD, 1600 Clifton Rd., NE, MS F-22, Atlanta, GA 30341; Fax: 770-488-7761; E-mail: mjb3@cdc.gov. Abstract Problem/Condition: Giardiasis, a gastrointestinal illness, is caused by the protozoan parasite Giardia intestinalis. Reporting Period: 1998--2002. System Description: State, commonwealth, territorial, and two metropolitan health departments voluntarily reported cases of giardiasis through CDC's National Electronic Telecommunications System for Surveillance. Results: During 1998--2002, the total number of reported cases of giardiasis decreased from 24,226 for 1998 to 19,708 for 2001 and then increased to 21,300 for 2002. The number of states reporting giardiasis cases increased from 42 to 46; however, the number of states reporting more than 15 cases per 100,000 population decreased from 10 to five. A greater number of case reports were received for children aged 1--9 years and for adults aged 30--39 years compared with other age groups. Incidence of giardiasis was highest in northern states. Peak onset of illness occurred annually during early summer through early fall. Interpretation: The increase observed for 2002 might reflect increased reporting after reporting of giardiasis as a nationally notifiable disease began in 2002. Transmission of giardiasis occurs throughout the United States, with increased diagnosis or reporting occurring in northern states. However, state incidence figures should be compared with caution because individual state surveillance systems have varying capabilities to detect cases. The seasonal peak in age-specific case reports coincides with the summer recreational water season and might reflect increased use of communal swimming venues (e.g., lakes, rivers, swimming pools, and water parks) by young children. Public Health Action: Giardiasis surveillance provides data to educate public health practitioners and health-care providers about the epidemiologic characteristics and the disease burden of giardiasis in the United States. These data are used to improve reporting of cases, plan prevention efforts, and establish research priorities. Introduction Giardia intestinalis (also known as G. lamblia and G. duodenalis) is the most common intestinal parasite identified by public health laboratories in the United States (1). This flagellated protozoan causes clinical illness (i.e., giardiasis) characterized by diarrhea, abdominal cramps, bloating, weight loss, and malabsorption; however, asymptomatic infection also frequently occurs (2--4). Case reports indicate that giardiasis also might be associated with the development of reactive arthritis (5). A zoonotic disease, giardiasis also affects domestic and wild mammals (e.g., cats, dogs, cattle, deer, and beavers) (2). Giardia infection is transmitted by the fecal-oral route and results from the ingestion of Giardia cysts through the consumption of fecally contaminated food or water or through person-to-person or animal-to-person transmission. The cysts are infectious immediately upon being excreted in feces. The infectious dose is low; ingestion of 10 cysts has been reported to cause infection (6). Infected persons have been reported to shed <109 cysts in their stool per day and to excrete cysts for months (6--8). Persons at increased risk for infection include 1) travelers to disease-endemic areas; 2) children in child care settings; 3) close contacts of infected persons (e.g., those in the same family or household or in the child care setting); 4) persons who ingest contaminated drinking water; 5) persons who swallow contaminated recreational water (e.g., water in lakes, rivers, and pools); 6) persons taking part in outdoor activities (e.g., backpacking and camping) who consume unfiltered, untreated water or who fail to practice hygienic behaviors (e.g., hand washing); 7) persons who have contact with infected animals; and 8) men who have sex with men (2,9--13). The relative contribution of person-to-person, animal-to-person, foodborne, and waterborne transmission to sporadic human giardiasis in the United States is unknown. Although giardiasis cases can occur sporadically, outbreaks are well documented. During 1991--2000, Giardia was identified as a causal agent of 9.4% (10 of 106) of reported recreational water-associated and 16.2% (21 of 130) of reported drinking water-associated outbreaks of gastroenteritis of known or suspected infectious etiology* (13--17). Additionally, foodborne outbreaks of giardiasis linked to infected foodhandlers and uninfected foodhandlers who diapered infected children have been reported (18). Outbreaks resulting from person-to-person transmission in child care centers also have been reported (19). In 1992, the Council of State and Territorial Epidemiologists (CSTE) assigned giardiasis an event code (code 11570) to facilitate transmission of reported giardiasis data to CDC. Reporting of giardiasis as a nationally notifiable disease began in 2002. This report summarizes national giardiasis surveillance data for 1998--2002. MethodsLaboratory-confirmed and probable cases of giardiasis can be reported voluntarily to CDC. Laboratory-confirmed giardiasis is defined as the detection (in symptomatic or asymptomatic persons) of Giardia intestinalis
A probable case of giardiasis is a clinically compatible case that is linked epidemiologically to a laboratory-confirmed case (20). DFA is the most sensitive and specific detection method for Giardia (21). Because Giardia cysts can be excreted intermittently, and multiple stool collections increase testing sensitivity, a total of three stool specimens should be collected, each on a different day (22). State, District of Columbia (DC), New York City (NYC), commonwealth, and territorial health departments can voluntarily report laboratory-confirmed and probable cases of giardiasis to CDC through the National Electronic Telecommunications System for Surveillance (NETSS). Reports include the patient's geographic information (i.e., state and county), age, sex, race, ethnicity (i.e., Hispanic or non-Hispanic), and date of illness onset and indicate whether the case is related to a known outbreak. An outbreak-related case is a laboratory-confirmed or a probable case that is linked epidemiologically to a laboratory-confirmed case. Analysis of the national giardiasis surveillance data for 1998--2002 was conducted by using SAS® v 8.2 (SAS Institute, Inc.; Cary, North Carolina) and the Food Safety Information Link (FSI Link). FSI Link, an intranet-based tool available to CDC staff, provides access to NETSS data and is used to monitor trends in and investigate outbreaks of reportable foodborne and waterborne diseases. ResultsDuring the 1998--2002 reporting period, the total number of reported cases of giardiasis decreased 18.6% from 24,226 for 1998 to 19,708 for 2001 and then increased 8.1% to 21,300 for 2002 (Table 1). Cases reported to be outbreak related made up 1.6%--11.6% of the total number of cases reported annually for 1999--2002. Although the number of states reporting cases increased from 42 to 46 during the reporting period, the number of states reporting >15 cases per 100,000 population decreased from 10 in 1998 to five in 2002. For 2002, among states reporting cases, incidence of giardiasis ranged from <0.1 cases (Texas) to 23.5 cases (Vermont) per 100,000 population. Vermont reported the greatest number of cases per 100,000 population for each of the 5 years of the reporting period. Northern states reported more cases annually per 100,000 population than southern states (Figure 1) (Table 1). These surveillance data display a bimodal age distribution, with the greatest number of reported cases occurring among children aged 1--9 years and adults aged 30--39 years (Figure 2). When reports for which patients' sex was missing or unknown are excluded, the percentage of cases reported to have occurred among males varied annually from 52.0% (12,125 of 23,310) for 1998 to 55.8% (10,851 of 19,460) for 2001. A twofold increase in reported giardiasis cases by onset of illness occurred during June--October (i.e., weeks 26--42 [early summer through early fall]) compared with January--March (Figure 3). However, the date of onset of illness was indicated for only 43.3% (10,480 of 24,226) of reported cases for 1998, for 43.8% (10,197 of 23,281) for 1999, for 42.6% (9,290 of 21,813) for 2000, for 49.2% (9,692 of 19,708) for 2001, and for 48.1% (10,245 of 21,300) for 2002. Age-specific analysis indicated that the seasonality in onset of illness was exhibited among children aged 1--4 and 5--9 years and adults aged 35--39 years (Figure 4) and among all age groups. The majority of cases for which data on race were available for 1998--2002 occurred among whites, followed by blacks, Asians and Pacific Islanders, and Native Americans (Table 2). However, data on race were not included for 39.2%--46.8% of total annual case reports. Of patients for whom data on ethnicity were reported, 13.6%--16.3% (1,651 of 12,158 for 1998 and 1,526 of 9,361 for 2001, respectively) were reported to be Hispanic. However, data on ethnicity were lacking for 49.5%--54.5% of total annual case reports for 1998--2002. DiscussionNational giardiasis surveillance data are used to assess the epidemiologic characteristics and disease burden of giardiasis in the United States. The total number of cases reported annually decreased during 1998--2001 and then increased in 2002. Reporting of giardiasis as a nationally notifiable disease began in 2002. California, which reported giardiasis cases for the first time in 2002, recorded 2,561 cases, which likely explains the observed increase in case reports for that year. Whether the decrease in reported cases for 1999--2001 reflects changes in reporting patterns and behavior or a real change in infection and disease caused by Giardia is unclear. FoodNet data document a decrease in case reports of other enteric diseases for 1996--2003; this decrease has been attributed to increased government and food industry emphasis on improved food safety (23). Giardiasis is geographically widespread in the United States. These data and data from the previous national giardiasis surveillance summary (1992--1997) indicate that the diagnosis or transmission of giardiasis might be higher in northern states (24). However, because differences in giardiasis surveillance systems among states can affect the capability to detect cases, whether this finding is of true biologic significance or is only the result of differences in case detection or reporting is difficult to determine. Although giardiasis affects persons in all age groups, the number of reported cases was highest among children aged 1--9 years and adults aged 30--39 years. These data are consistent with previously published reports of giardiasis incidence being higher among younger children and of transmission to their caregivers (e.g., child care staff, family members, and other household contacts) (2,24--26). A marked seasonality in the onset of illness occurs in early summer through early fall, and a twofold increase in transmission of giardiasis occurs during the summer. This increase coincides with increased outdoor activities (e.g., swimming during the summer recreational water season and camping) and might reflect heavy use of community swimming (essentially communal bathing) venues by younger children. Transmission through use of surface water (e.g., lakes and rivers) and disinfected venues (e.g., swimming pools and water parks) is facilitated by the substantial number of Giardia cysts that can be shed by a single person; the extended periods of time that cysts can be shed; the low infectious dose; the moderate resistance to chlorine of Giardia; the prevalence of improper pool maintenance (i.e., insufficient disinfection, filtration, and recirculation of water), particularly of children's wading pools; the prevalence of Giardia in fecal material in pools; and documented transmission of Giardia infection among diapered children using swimming venues (6--8,27--29). This seasonal variation also has been noted in state, Canadian provincial, and previous U.S. national surveillance data for giardiasis, as well as for cryptosporidiosis (24--26,30). Among patients for whom data on sex were reported, the proportion reported to be male increased annually during 1998--2001. However, because 12.9% of case reports for 2002 did not include data about sex, whether this increase continued in 2002 is unclear. Because data on race and ethnicity are incomplete, conclusions cannot be made about the differences noted in the epidemiology of giardiasis among members of different racial populations and between Hispanics and non-Hispanics. The data reported likely underestimate the giardiasis burden in the United States. Diarrheal diseases are highly underreported because 1) not all infected persons are symptomatic; 2) those who are symptomatic do not always seek medical care; 3) health-care providers do not always include diagnostics in their workup of diarrheal diseases because they might treat patients without testing stool for the pathogen; and 4) case reports are not always completed for positive laboratory results or forwarded to public health officials (31). An estimated 1%--5% of cases of salmonellosis, another diarrheal illness, are reported to CDC through passive surveillance (32). If these estimates are used to extrapolate from the 21,206 giardiasis cases reported by the 50 states and DC for 2002, the giardiasis disease burden in the United States in 2002 could have been 424,120--2,120,600 cases (147.3--736.4 cases per 100,000 population). The true burden of giardiasis in the United States is likely to fall between these two estimates. Its low infectious dose, protracted communicability, and moderate chlorine resistance make Giardia ideally suited for transmission through drinking and recreational water, food, and both person-to-person and animal-to-person contact. Prevention measures (Box 1) and measures to improve surveillance for giardiasis and increase understanding of its epidemiology and the associated disease burden (Box 2) have been recommended. Information about giardiasis is available from CDC at http://www.cdc.gov/ncidod/dpd/parasites/giardiasis/factsht_giardia.htm. Acknowledgments The authors thank the state, DC, NYC, Puerto Rico, Guam, and the Northern Mariana Islands surveillance coordinators for facilitating the reporting of giardiasis data to CDC, and John Hatmaker and Man-huei Chang of the Division of Public Health Surveillance and Informatics, Epidemiology Program Office, CDC, for facilitating access to the data and for their assistance during the course of its analysis. References1. Kappus KD, Lundgren RG, Juranek DD, Roberts JM, Spencer HC. Intestinal parasitism in the United States: update on a continuing problem. Am J Trop Med Hyg 1994;50:705--13. 2. Thompson RC. Giardiasis as a re-emerging infectious disease and its zoonotic potential. Intl J Parasitol 2000;30:1259--67. 3. Hellard ME, Sinclair MI, Hogg GG, Fairley CK. Prevalence of enteric pathogens among community based asymptomic individuals. Gastroenterol Hepatol 2000;15:290--3. 4. Rodrigquez-Hernandez J, Canut-Blasco A, Martin-Sanchez AM. Seasonal revalences of Cryptosporidium and Giardia infections in children attending day care centres in Salamanca (Spain) studied for a period of 15 months. Eur J Epidemiol 1996;12:291--5. 5. Tupchong M, Simor A, Dewar C. Beaver fever---a rare cause of reactive arthritis. J Rheumatol 1999;26:2701--2. 6. Rendtorff RC. The experimental transmission of human intestinal protozoan parasites. II. Giardia lamblia cysts given in capsules. Am J Hyg 1954;59:209--20. 7. Danciger M, Lopez M. Numbers of Giardia in the feces of infected children. Am J Trop Med Hyg 1975;24:237--42. 8. Pickering LK, Woodward WE, DuPont HL, Sullivan P. Occurrence of Giardia lamblia in children in day care centers. J Pediatr 1984;104:522--6. 9. Hoque ME, Hope VT, Scragg R, Kjellstrom T, Lay-Yee R. Nappy handling and risk of giardiasis. Lancet 2001;357:1017--8. 10. Esfandiari A, Swartz J, Teklehaimanot S. Clustering of giardiasis among AIDS patients in Los Angeles County. Cell Mol Biol 1997;43:1077--83. 11. Welch TP. Risk of giardiasis from consumption of wilderness water in North America: a systematic review of epidemiologic data. Int J Infect Dis 2000;4:100--3. 12. Stuart JM, Orr HJ, Warburton FG, et al. Risk factors for sporadic giardiasis: a case-control study in southwestern England. Emerg Infect Dis 2003;9:229--33. 18. Quick R, Paugh K, Addiss D, Kobayashi J, Baron R. Restaurant-associated outbreak of giardiasis. J Infect Dis 1992;166:673--6. 19. Ang LH. Outbreak of giardiasis in a daycare nursery. Commun Dis Public Health 2003;3:212--3. 20. CDC. Giardiasis (Giardia lambia) case definition. Atlanta, GA: US Department of Health and Human Services, CDC; 1997. Available at http://www.cdc.gov/epo/dphsi/casedef/giardiasis_current.htm. 21. Johnston SP, Ballard MM, Beach MJ, Causer L, Wilkins PP. Evaluation of three commercial assays for detection of Giardia and Cryptosporidium organisms in fecal specimens. J Clin Microbiol 2003;41:623--6. 22. Clinical and Laboratory Standards Institute/NCCLS. Procedures for the recovery and identification of parasites from the intestinal tract; approved guideline [Report no. M28-A]. Wayne, PA: Clinical and Laboratory Standards Institute/NCCLS; 1997. 23. CDC. Preliminary FoodNet data on the incidence of infection with pathogens transmitted commonly through food---selected sites, United States, 2003. MMWR 2004;53:338--43. 25. Naumova, EN, Chen JT, Griffiths JK, Matyas BT, Estes-Smargiassi SA, Morris RD. Use of passive surveillance data to study temporal and spatial variation in the incidence of giardiasis and cryptosporidiosis. Public Health Rep 2000;115:436--47. 26. Greig JD, Michel P, Wilson JB, et al. A descriptive analysis of giardiasis cases reported in Ontario, 1990--1998. Can J Public Health 2001;92:361--5. 29. Harter L, Frost F, Grunenfelder G, Perkins-Jones K, Libby J. Giardiasis in an infant and toddler swim class. Am J Public Health 1984;74:155--6. 31. Mead PS, Slutsker L, Dietz V, et al. Food-related illness and death in the United States. Emerg Infect Dis 1999;5:607--25. 32. Chalker RB, Blaser MJ. A review of human salmonellosis: III. Magnitude of Salmonella infection in the United States. Rev Infect Dis 1988;10:111--24. * The denominator includes outbreaks whose etiology was reported as acute gastrointestinal illness because they were suspected to be caused by an unidentified infectious agent. Table 1 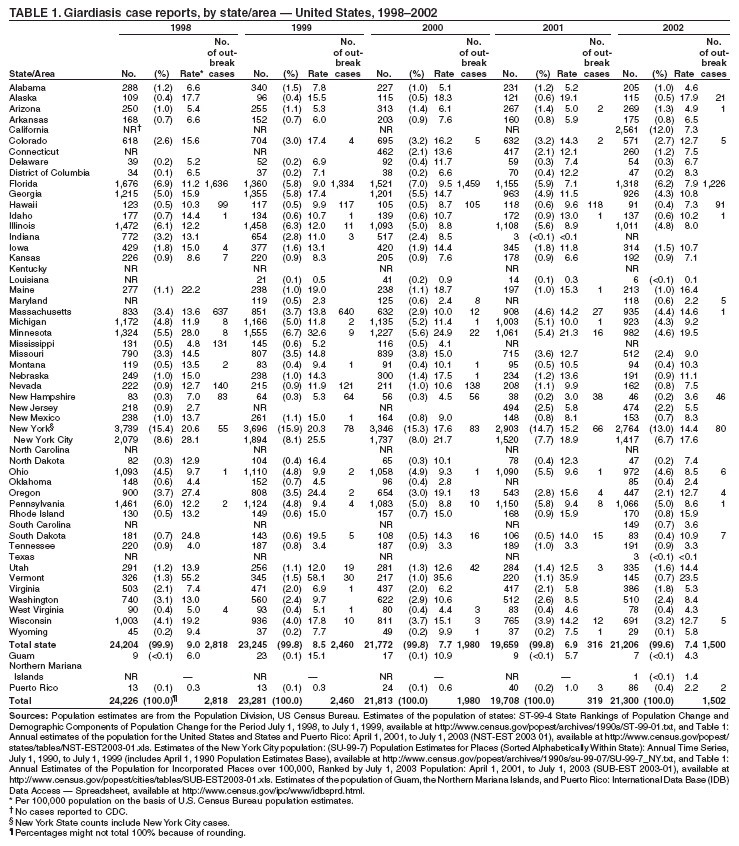 Return to top. Figure 1 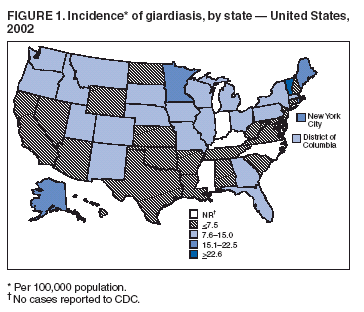 Return to top. Box 1 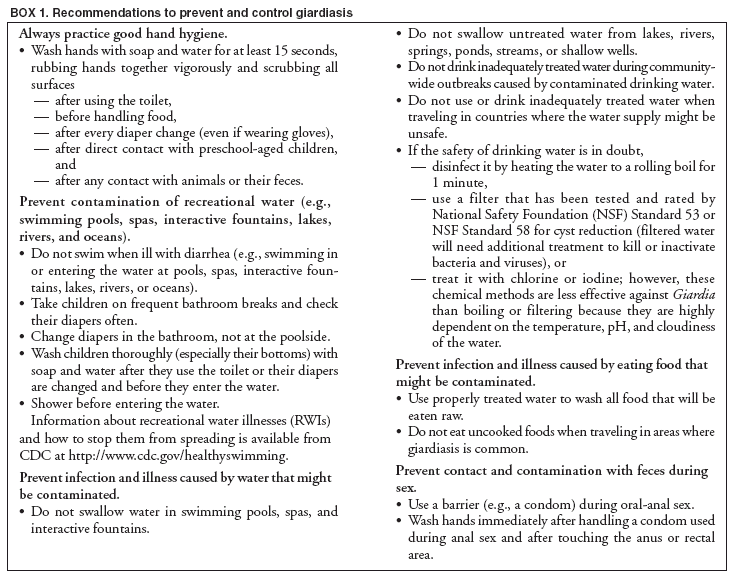 Return to top. Table 2 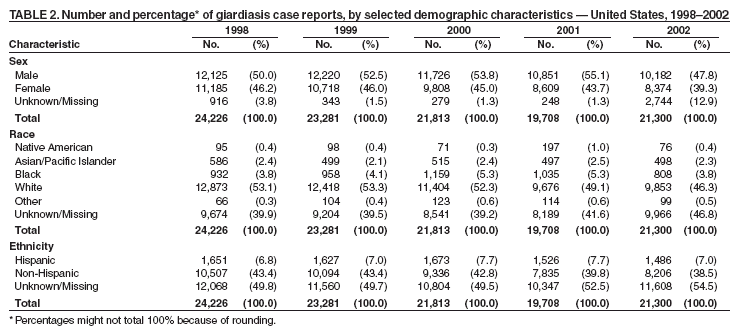 Return to top. Figure 2 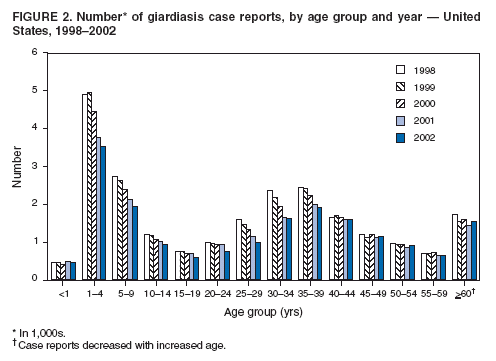 Return to top. Box 2  Return to top. Figure 3 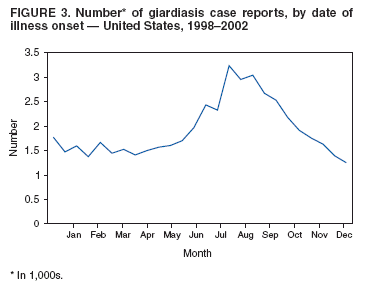 Return to top. Figure 4 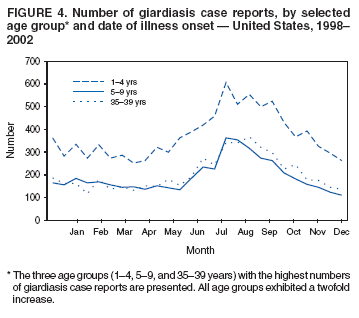 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 1/19/2005 |
|||||||||
This page last reviewed 1/19/2005
|