 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Assisted Reproductive Technology Surveillance --- United States, 2000Please note: An erratum has been published for this article. To view the erratum, please click here. Victoria C. Wright, M.P.H. Abstract Problem/Condition: In 1996, CDC initiated data collection regarding assisted reproductive technology (ART) procedures performed in the United States to determine medical center-specific pregnancy success rates, as mandated by the Fertility Clinic Success Rate and Certification Act (FCSRCA) (Public Law 102-493, October 24, 1992). ART includes fertility treatments in which both eggs and sperm are handled in the laboratory (i.e., in vitro fertilization and related procedures). Patients who undergo ART treatments are more likely to deliver multiple-birth infants than women who conceive naturally. Multiple births are associated with increased risk for mothers and infants (e.g., pregnancy complications, premature delivery, low-birthweight infants, and long-term disability among infants). Reporting Period Covered: 2000. Description of System: CDC contracts with a professional society, the Society for Assisted Reproductive Technology (SART), to obtain data from fertility medical centers located in the United States. Since 1997, CDC has compiled data related to ART procedures. The Assisted Reproductive Technology Surveillance System was initiated by CDC in collaboration with the American Society for Reproductive Medicine, the Society for Assisted Reproductive Technology, and RESOLVE: The National Infertility Association. Results: In 2000, a total of 25,228 live-birth deliveries and 35,025 infants resulting from 99,629 ART procedures were reported to CDC from 383 medical centers that performed ART in the United States and U.S. territories. Nationally, 75,516 (76%) of ART treatments were freshly fertilized embryos using the patient's eggs; 13,312 (13%) were thawed embryos using the patient's eggs; 7,919 (8%) were freshly fertilized embryos from donor eggs; and 2,882 (3%) were thawed embryos from donor eggs. The national live-birth delivery per transfer rate was 30.8%. The five states that reported the highest number of ART procedures were California (13,194), New York (11,239), Massachusetts (8,041), Illinois (7,323), and New Jersey (5,506). These five states also reported the highest number of live-birth deliveries and infants born as a result of ART. Overall, 47% of women undergoing ART-transfer procedures using freshly fertilized embryos from their own eggs were aged <35 years; 23% were aged 35--37 years; 19% were aged 38--40 years; 7% were aged 41--42 years; and 4% were aged >42 years. Among ART treatments in which freshly fertilized embryos from the patient's eggs were used, substantial variation in patient age, infertility diagnoses, history of past infertility treatment, and past births was observed. Nationally, live-birth rates were highest for women aged <35 years (38%). The risk for a multiple-birth delivery was highest for women who underwent ART-transfer procedures using freshly fertilized embryos from either donor eggs (40%) or from their own eggs (35%). Among women who underwent ART-transfer procedures using freshly fertilized embryos from their own eggs, further variation by patient age and number of embryos transferred was observed. Of the 35,025 infants born, 44% were twins, and 9% were triplet and higher order multiples, for a total multiple-infant birth rate of 53%. Patient's residing in states with the highest number of live-birth deliveries also reported the highest number of infants born in multiple-birth deliveries. Interpretation: Whether an ART procedure was successful (defined as resulting in a pregnancy and live-birth delivery) varied according to different patient and treatment factors. Patient factors included the age of the woman undergoing ART, whether she had previously given birth, whether she had previously undergone ART, and the infertility diagnosis of both the female and male partners. Treatment factors included whether eggs were from the patient or a woman serving as an egg donor, whether the embryos were freshly fertilized or previously frozen and thawed, how long the embryos were kept in culture, how many embryos were transferred, and whether various specialized treatment procedures were used in conjunction with ART. ART poses a major risk for multiple births. This risk varied according to the patient's age, the type of ART procedure performed, and the number of embryos transferred. In addition, the increased risk for multiple births has a notable population impact in certain states. Public Health Actions: As use of ART and ART success rates continue to increase, ART-related multiple births are an increasingly important public health problem nationally and in many states. The proportion of infants born through ART in 2000 that were multiple births (53%) was substantially higher than in the general U.S. population during the same period. Data in this report indicate a need to reduce multiple births associated with ART. Efforts should be made to limit the number of embryos transferred for patients undergoing ART. In addition, continued research and surveillance is key to understanding the effect of ART on maternal and child health. IntroductionFor >2 decades, assisted reproductive technologies (ARTs) have been used by couples to overcome infertility. ARTs include those infertility treatments in which both eggs and sperm are handled in the laboratory (i.e., in vitro fertilization and related procedures). Since the birth of the first U.S. infant conceived with ART in 1981, use of these treatments has increased dramatically. Each year, both the number of medical centers providing ART services and the total number of procedures performed have increased notably (1). In 1992, Congress passed the Fertility Clinic Success Rate and Certification Act (FCSRCA),* which requires each medical center in the United States that performs ART to report data to CDC annually and to include every ART procedure initiated. CDC uses the data to report medical center-specific pregnancy success rates. In 1997, CDC published the first surveillance report under this mandate (2). That report was based on ART procedures performed in 1995. Since then, CDC has continued to publish a surveillance report annually that details each medical center's success rates. CDC has also used this surveillance data file to perform more in-depth analyses of infant outcomes (e.g., multiple births) (3,4). Multiple-infant births are associated with greater health problems for both mothers and infants, including higher rates of caesarean deliveries, prematurity, low birthweight, and infant death and disability. This report is based on ART surveillance data provided to CDC's National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP), Division of Reproductive Health, regarding procedures performed in 2000. A report of these data according to the medical center in which the procedure was performed was published separately (1). In this report, emphasis is on presenting state-specific data and presenting more detailed data regarding multiple-birth risk for 2000. MethodsEach year, the Society for Assisted Reproductive Technology (SART), an organization of ART providers affiliated with the American Society for Reproductive Medicine, collects data regarding ART procedures from medical centers performing ART in the United States and its territories and provides these data to CDC by contract. Data collected include patient demographics, medical history and infertility diagnoses, clinical information pertaining to the ART procedure, and information regarding resultant pregnancies and births. The data file is organized with one record per ART procedure performed. Multiple procedures from a single patient are not linked. Despite the federal mandate, certain centers (6%--7%/year) have not reported their data; the majority of these are believed to be smaller than average practices. For this report, data pertaining to ART procedures initiated January 1--December 31, 2000, are presented. ART data and outcomes from ART are presented by state of residence. In cases of missing residency data (10%), the state of residency was assigned as the state in which the ART procedure was performed. Additionally, data regarding number of procedures are presented by treatment type and stage of treatment. ART procedures are usually classified into four groups according to whether a woman used her own eggs or received eggs from a donor and whether or not the embryos transferred were freshly fertilized or previously frozen and thawed. Because both success rates and multiple-birth risk vary substantially among these four treatments groups, data are presented separately for each type. In addition to treatment types, within a given treatment procedure, different stages exist. A typical ART procedure begins when a woman starts taking drugs to stimulate egg production or begins having her ovaries monitored with the intent of having embryos transferred. If eggs are produced, the procedure progresses to the egg retrieval stage. After the eggs are retrieved, they are combined with sperm in the laboratory, and if fertilization is successful, the resulting embryos are selected for transfer. If the embryo implants in the uterus, the cycle progresses to a clinical pregnancy (i.e., the presence of a gestational sac detectable by ultrasound). The resulting pregnancy might progress to a live-birth delivery. A live-birth delivery is defined as the delivery of >1 live-born infant. Only ART procedures involving freshly fertilized eggs include an egg retrieval stage; ART procedures using thawed eggs do not include egg retrieval because eggs were fertilized during a previous procedure and the resulting embryos were frozen until the current procedure. An ART procedure can be discontinued at any step for medical reasons or by the patient's choice. Variations in a typical ART procedure are noteworthy. Although a typical ART procedure includes in vitro fertilization (IVF) of gametes, culture for >2 days and embryo transfer into the uterus (i.e., transcervical embryo transfer), in certain cases, unfertilized gametes (eggs and sperm) or zygotes (early embryos [i.e., a cell that results from fertilization of the egg by a sperm]) are transferred into the fallopian tubes within a day or two of retrieval. These are known as gamete and zygote intrafallopian transfer (GIFT and ZIFT). Another adaptation is intracytoplasmic sperm injection (ICSI) in which fertilization is still in vitro but is accomplished by selection of a single sperm that is injected directly into the egg. This technique was originally developed for couples with male factor infertility but is now commonly used for an array of diagnostic groups. Detailed data are presented in this report for the most common treatment type, those using freshly fertilized embryos from the patient's eggs. These procedures account for >70% of the total number of ART procedures performed each year. For those procedures that progressed to the embryo-transfer stage, percentage distribution of selected patient and treatment factors were calculated. In addition, success rates, defined as live-birth deliveries per ART-transfer procedure, were calculated according to the same patient and treatment characteristics. Patient factors included the age of the woman undergoing ART, whether she had previously given birth, the number of past ART attempts, and the infertility diagnosis of both the female and male partners. The patient's age at the time of the ART procedure were grouped into five categories: aged <35 years, 35--37 years, 38--40 years, 41--42 years, and >42 years. Diagnoses ranged from one factor in one partner to multiple factors in one or both partners and were categorized as
Treatment factors included
The number of embryos transferred in an ART procedure was categorized as 1, 2, 3, 4, or >5. The number of days of embryo culture was calculated by using dates of egg retrieval and embryo transfer and was categorized as 1--6. However, because of limited sample sizes, live-birth rates are presented only for the two most common days, 3 and 5. Likewise, live-birth rates are presented for IVF with and without ICSI only and not for GIFT and ZIFT. Multiple birth was assessed in two ways. First, each multiple-birth delivery was defined as a single event. A multiple-birth delivery was defined as the delivery of >2 infants in which at least one was live-born. The multiple-birth risk was thus calculated as the proportion of multiple-birth deliveries among total live-birth deliveries. Multiple birth was also assessed according to the proportion of infants from multiple deliveries among total infants (i.e., each infant was considered separately in this calculation). The proportion of live-born infants who were multiples (twins and triplets or more) was then calculated. Each of these measures represents a different focus. The multiple-birth risk, based on number of deliveries (or infant sets), provides an estimate of the individual risk posed by ART to the woman for multiple birth. The proportion of infants born in a multiple-birth delivery provides a measure of the effect of ART treatments on children in the population. Both measures are presented by type of ART treatment and by maternal age for births conceived with the patient's eggs. Multiple-birth risk is further presented by number of embryos transferred. Proportion of infants born in a multiple-birth delivery is presented separately by state of residency. All analyses were performed by using SAS software system (5). ResultsA total of 99,629 ART procedures performed in 2000 were reported to CDC (Table 1). The largest number of ART procedures occurred among patients who used their own freshly fertilized embryos (75,516; 76%). Of the 99,629 procedures started, 81,915 (82%) progressed to embryo transfer. Overall, 37% of ART procedures that progressed to the transfer stage resulted in a pregnancy, and 31% resulted in a live-birth delivery. Both pregnancy and live-birth rates varied according to type of ART. The highest rates were observed among ART procedures using donor eggs and freshly fertilized embryos (51% pregnancy rate and 44% live-birth rate). The lowest rates were observed among procedures using the patient's eggs and thawed embryos (26% pregnancy rate and 20% live-birth rate). In all, the 25,228 live-birth deliveries from ART procedures resulted in 35,025 infants (Table 1); the number of infants born was higher than the number of live-birth deliveries because of multiple-infant births. The largest proportion of infants born (76.5%; n = 26,800) were from ART procedures in which patients used freshly fertilized embryos from their own eggs. Of 408 medical centers in the United States and surrounding territories that performed ART in 2000, a total of 383 provided data to CDC (Figure 1). The majority of medical centers that provided ART services were located in the eastern United States, in or near major cities. Within states, the number of medical centers performing ART was variable. Four states had no ART medical centers (Alaska, Maine, Montana, and Wyoming). States with the largest number of ART centers were California (56), Florida (28), New York (28), Illinois (25), and Texas (24). The number of ART procedures performed among residents of each state approximately paralleled the data by medical center location (Table 2). The greatest numbers of ART procedures reported in 2000 were performed among residents of California (13,194), New York (11,239), Massachusetts (8,041), Illinois (7,323), and New Jersey (5,506). The five states with the largest number of ART procedures performed also reported the majority of live-birth deliveries and infants born. ART was used by residents of certain states and territories without an ART medical center (e.g., Alaska, Guam, Maine, Montana, Northern Mariana Islands, Virgin Islands, and Wyoming); however, each accounted for a limited percentage of total ART usage in the United States. Non-U.S. residents accounted for an estimated 1% of ART procedures, live-birth deliveries, and infants born. Forty-seven percent of ART-transfer procedures using freshly fertilized embryos from the patient's eggs were performed on women aged <35 years; 23% on women aged 35--37 years; 19% on women aged 38--40 years; 7% on women aged 41--42; and 4% on women aged >42 years. Patient and treatment characteristics of these women varied by age (Table 3). The most common diagnoses reported for infertility among couples were male factor and tubal factor; however, diagnoses varied overall. Tubal factor, male factor, endometriosis, and ovulatory dysfunction were more commonly reported among younger women than women in older age categories. In contrast, diminished ovarian reserve was reported for only 1% of women aged <35 years; it was reported for 12% of women aged 41--42 years, and 22% of women aged >42 years. Among all women, 10%--12% were reported as having unexplained infertility; 11%--16% were reported as having multiple female factors; and 17%--18% were reported as having both male and female factors. Approximately 60% of women aged <35 years were undergoing their first ART procedure. The percentage of women who had undergone at least one previous ART procedure increased with increasing age: only 40% of women aged >42 years were undergoing their first ART procedure. The percentage of women who had had a previous birth followed similar patterns. Although 19% of women aged <35 years reported at least one previous birth, this increased steadily with age: >35% of women in the oldest age group had had a previous birth.† The majority of ART procedures used IVF with or without ICSI. Only a limited proportion of ART procedures used GIFT or ZIFT. Use of ICSI demonstrated a slight inverse relationship with patient age; these findings are consistent with higher rates of male factor infertility among younger age groups. In all age groups, the majority of procedures included embryo culture for 3 days; the next most common procedure involved embryo culture to day 5. Culture to day 5 coincides with development of the embryo to the blastocyst stage, which was used more frequently among younger women. Although limited variation existed by age, the majority of ART procedures involved transfer of >1 embryo. Among women aged <35 years, 96% of procedures involved transfer of >2 embryos, and 63% involved transfer of >3 embryos. For women aged >42 years, 86% involved transfer of >2 embryos, and 68% involved transfer of >3 embryos. Use of a gestational carrier or surrogate was <1% for all age groups. Live-birth rates for women who underwent ART procedures using freshly fertilized embryos from their own eggs also varied by patient age and selected patient and treatment factors (Table 4). Although the average live-birth rate for ART-transfer procedures performed among women who used their own freshly fertilized eggs was 32%, live-birth rates ranged from 38% among women aged <35 years to 6% among women aged >42 years (Table 4). Women aged <40 years who had an infertility diagnosis of ovulatory dysfunction or endometriosis or had unexplained infertility tended to have higher live-birth rates. Women aged >40 years with a diagnosis of uterine factor had above average live-birth rates (22% for women aged 41--42 years and 15% for women aged >42 years). Across all age groups, a diagnosis of diminished ovarian reserve was related to lower live-birth rates. Also, live-birth rates were lower for couples with a diagnosis of multiple factors, particularly male and female factors. Women aged <42 years who had undergone a previous ART procedure had lower live-birth rates than women undergoing their first ART procedure. However, the number of previous ART procedures cannot be subdivided by whether they were successful or not. Women aged <42 years who had had >1 previous birth had higher live-birth rates than those with no previous births. Women aged >42 years had low live-birth rates overall (6%), regardless of whether they had had a previous ART or a previous birth. ART procedures in which IVF was used with ICSI had lower live-birth rates in all age groups (Table 4). Live-birth rates were higher for women who had had extended embryo culture to day 5 than for women who had embryos cultured to day 3; this pattern was also observed for all age groups. In addition, among all age groups, the highest live-birth rates were observed among women who had transferred > 2 embryos and among women who had used a gestation carrier. However, all of the results for treatment factors need to be considered cautiously because treatment was not randomized but rather based on medical center assessment and patient choice. Of 8,806 multiple-birth deliveries, 6,784 were from pregnancies conceived with freshly fertilized embryos from the patient's eggs; 609 were from thawed embryos from the patient's eggs; 1,236 were from freshly fertilized embryos from a donor's eggs; and 177 were from thawed embryos from a donor's eggs (Table 5). In comparison with ART procedures using the patient's eggs and freshly fertilized embryos, the risks for multiple-birth delivery were increased when eggs from a donor were used and decreased when thawed embryos were used. Among ART procedures in which the patient's own eggs were used, a strong inverse relation existed between multiple-birth risk and patient age. The average multiple-birth risk (i.e., multiple-birth delivery rate) for ART procedure in which freshly fertilized embryos from the patient's eggs were used was 35%. This rate varied from 39% among women aged <35 years to 12% among women aged >42 years. Of 35,025 infants born through ART, 53% (18,603) were born in multiple-birth deliveries (Table 5). The proportion of infants born in a multiple-birth delivery also varied by type of ART procedure and patient age. A more detailed examination of multiple-birth risk for women who underwent ART procedures in which freshly fertilized embryos from their own eggs were used revealed that number of embryos transferred was a risk factor for multiple-birth delivery, but the magnitude of the risk varied according to patient age (Figures 2--6). Among all age groups, transfer of >2 embryos resulted in increased live-birth delivery rates. However, the multiple-birth risk was also substantially increased. Among women aged <35 years (Figure 2) and 35--37 years (Figure 3), the percentage of twin deliveries increased steadily with increasing number of embryos transferred from two to five or more. The percentage of triplet and higher order multiple-birth deliveries demonstrated an even more marked increase as the number of embryos transferred increased. As a result, the percentage of singleton deliveries for both of these two youngest age groups was actually lower when >3 embryos were transferred in comparison with two embryos being transferred. For women aged 38--40 years (Figure 4), transfer of >3 embryos offered a certain advantage in terms of live-birth delivery rates. However, as among younger age groups, the percentage of twin deliveries and triplet or higher order multiple-birth deliveries were substantially increased with >3 embryos having been transferred compared with two. For women aged 41--42 years (Figure 5), both the live-birth delivery rate and the multiple-birth risk increased steadily with an increased number of embryos having been transferred. The percentage of triplet or higher order multiple-birth deliveries did not demonstrate a trend. For women aged >42 years (Figure 6), the percentage of twin deliveries (11%--13%) and triplet or higher order multiple-birth deliveries (0%--2%) did not vary substantially by number of embryos (>2) having been transferred.§ The total number and percentage of infants born in multiple-birth deliveries by maternal state of residency is presented (Table 6). Among states and territories with one or more total infants, conceived through ART, the numbers of infants born in multiple-birth deliveries ranged from 0 for residents of the Virgin Islands to 2,315 for California residents. The states with the highest number of ART-associated live-birth deliveries also had the highest number of infants born in multiple-birth deliveries. These include California (2,315), New York (1,946), Massachusetts (1,268), New Jersey (1,205), and Illinois (1,099). Nationally, the percentage of infants born in multiple-birth deliveries after ART was used was 53%; the percentage of twins and triplets or more were 44% and 9%, respectively. The percentage of infants born in multiple-birth deliveries was >50% in the majority of states. The states with the highest proportion of infants born in multiple-birth deliveries were Wyoming (69%), Nevada (62%), North Carolina (61%), Idaho (61%), and Oregon (60%). DiscussionAccording to the latest estimates of infertility in the United States from the 1995 National Survey of Family Growth, 15% of women of reproductive age reported a past infertility-associated health-care visit, and 2% reported a visit in the past year (6). Among married couples in which the woman was of reproductive age, 7% reported they had not conceived after 12 months of unprotected intercourse. With advances in ART, couples are increasingly turning to these treatments to overcome their infertility. Since the birth of the first infant through ART in the United States in 1981, use of ART has grown substantially. Since 1997, CDC has been monitoring ART procedures performed in the United States. During that time, a notable and consistent increase in the use of ART has occurred. The increased use of ART coupled with increases in ART success rates has resulted in dramatic increases in the number of children conceived through ART each year. From 1996 (i.e., the first full year for which CDC collected data) through 2000, the number of ART procedures performed increased 54%, from 64,724 to 99,629 (1). Additionally, live-birth rates for all types of ART procedures increased from 11% to 22% during 1996--2000. The number of infants conceived through ART increased 67%, from 20,921 infants conceived through ART procedures performed in 1996 to 35,025 infants conceived through ART procedures performed in 2000. This report documents that in 2000, ART use varied according to state of residency. Residents of California, New York, Massachusetts, Illinois, and New Jersey reported the highest number of ART procedures. These states also reported the highest number of infants conceived through ART. In 2000, ART use by state of residency was partly in line with expectations based on the total population size of women of reproductive age (i.e., women aged 15--44 years) within states (7). For example, California, New York, and Illinois were in the top five states for both ART usage and total number of women of reproductive age. However, ART use did not completely parallel population size. Whereas Massachusetts had the third highest number of ART procedures performed, it ranked thirteenth in terms of women of reproductive age. Likewise, New Jersey ranked fifth according to ART use, but ranked tenth according to population size. This divergence is not completely surprising because both Massachusetts and New Jersey had statewide mandates for insurance coverage for ART procedures in 2000. The state variation might also be related to availability of ART services within each state. However, we cannot disentangle the relation between demand for services and availability (i.e., increased availability in certain states might reflect the increased demand for ART among state residents). Patients with an array of characteristics used ART services. Among ART treatments in which freshly fertilized embryos from the patient's eggs were used (i.e., the most frequent type of ART treatment), substantial variation was observed in patient age, infertility diagnoses, history of past infertility treatment, and past births. Success rates from ART use are affected by numerous patient and treatment factors; hence, considering one single measure of success in evaluating ART efficacy is not informative. At a minimum, ART treatments need to be subdivided into general categories on the basis of the source of the egg (patient or donor) and the status of the embryos (freshly fertilized or thawed) because success rates vary substantially across these types. Within the type of ART treatment, further variation exists in success rates by patient and treatment factors, most notably patient age. Other factors to consider when assessing success rates are infertility diagnosis, number of previous ART procedures, number of previous births, type of ART procedure, number of days of embryo culture, number of embryos transferred, and use of a gestational carrier (surrogate). Variation exists in success rates according to each of these factors. CDC's primary focus in collecting ART data has been live-birth deliveries as an indicator of success, because ART surveillance activities were developed in response to a federal mandate to report ART success rate data. Thus, a key role for CDC has been to publish standardized data related to ART success rates, including information regarding factors that affect these rates. With these data, couples can make informed decisions regarding whether to undergo this time-consuming and expensive treatment (8,9).¶ However, success-rate data must also be balanced with consideration of effects on maternal and infant health. Thus, CDC also closely monitors multiple births conceived through ART. Multiple births are associated with an increased health risk for both mothers and infants (10--12). Women with multiple-gestation pregnancies are at increased risk for maternal complications (e.g., hemorrhage and hypertension). Infants born in a multiple-birth delivery are at increased risk for prematurity, low birthweight, infant mortality, and long-term disability. The health risks associated with multiple births have also contributed to rising health-care costs. In 2000, the estimated costs (per family) of delivering multiple-gestation pregnancies resulting from ART procedures ranged from $58,865 for twins to $281,698 for quadruplets (12). Additionally, a study regarding costs per delivery resulting from IVF pregnancies estimated $39,000 for singleton or twin pregnancies and $340,000 for triplet and quadruplet pregnancies (13). In the United States, multiple births have increased dramatically during the last 2 decades (14,15). The rise in multiple births has been attributed to an increased use of ART and delayed childbearing (4,16,17). A recent study concerning trends in multiple births reported that 14% of multiple births in the United States in 2000 were attributed to ART; the proportions of twins and triplets or more attributed to ART were 12% and 43%, respectively (4). Other non-ART infertility treatments were estimated to also have contributed substantially to multiple births in the United States. Thus, even with shifts toward delayed child-bearing and the concomitant increase in multiple births known to be associated with advanced maternal age, by 2000, only 67% of twin births and 18% of triplet or higher order multiple births were estimated to have been naturally conceived. In this report, 53% of infants born through ART in 2000 were multiple births; this compares with 3% in the general U.S. population during the same period (14,18). The twin rate was 44%, 22 times higher than in the general U.S. population (2%); the triplet and higher order multiples rate was 9%, 50 times higher than the general U.S. population (0.18%). Regarding the specific type of ART treatment, the rates are even higher for women who underwent ART procedures using freshly fertilized embryos from their own eggs (54% total multiple births) or from donor eggs (59% total multiple births). In the majority of states, >50% of infants conceived through ART were born in multiple-birth deliveries. North Carolina, Nevada, Idaho, Oregon, and Wyoming reported ART-associated multiple-birth rates >60%. Multiple births resulting from ART are an increasing public health problem, nationally and for the majority of states. The findings in this report confirm the need to reduce the occurrence of multiple births resulting from ART. This analysis was subject to certain limitations. First, ART surveillance data are reported for each ART procedure performed rather than for each patient who used ART. Linking procedures among patients who underwent >1 ART procedure in a given year is not possible. Because patients undergoing >1 procedure in a given year are most likely to be those who failed >1 treatment, the success rates reported here might underestimate the true per-patient success rate. Second, these data represent couples who sought ART services in 2000; therefore, success rates do not represent all couples with infertility who were potential ART users in 2000. Third, 6% of medical centers that performed ART in 2000 did not report their data to CDC as required. Fourth, comparisons among states are based on absolute numbers that are not adjusted for state population size. ART data are reported to CDC by the ART medical center where the procedure was performed rather than by the state where the patient resided. In this report, we present ART data by the female patient's state of residence. In previous reports (16), we were unable to present ART data by state of residence because of incompleteness of residency data. In 2000, residency data were missing for 10% of all live-birth deliveries reported to CDC. The range of missing residency data varied by medical center. Medical centers located in 35 states had <5% missing residency data; medical centers located in six states had 5%--9% missing residency data; medical centers located in one state had 10%--15% missing residency data, and medical centers located in six states had >15% missing residency data. These states were Arizona, Georgia, Massachusetts, Minnesota, New York, and Pennsylvania. In cases of missing residency data, we assigned residency as the state in which the ART procedure was performed. Thus, the number of procedures performed among state residents, number of infants, and number of multiple- birth infants might have been overestimated for these states. Concurrently, the numbers might be underestimated in states bordering states with missing data, particularly states in the Northeast region of the United States. Nonetheless, the effects of missing residency data were not substantial. We separately evaluated statistics according to the state in which the ART medical center was located rather than the patient's state of residency. The rankings of the states in terms of total number of infants and multiple-birth infants were similar to the rankings based on state of residency (data not shown). Despite these limitations, findings from national surveillance of ART procedures performed in the United States provide useful information for patients contemplating ART, ART providers, and health-care policy makers. First, ART surveillance data can be used to monitor trends in ART use and outcomes from ART procedures. Second, data from ART surveillance can be used to assess patient and treatment factors that contribute to higher success rates. Third, ongoing surveillance data can be used to assess the risk of multiple births. Fourth, surveillance data provide information to assess changes in clinical practice related to ART treatment. Multiple births are one of the most important public health concerns associated with using ART. Increased use of ART treatments and the widespread practice of transferring multiple embryos during ART treatments has led to a substantial increase in multiple-birth rates in the United States (4,15). Although balancing the chance of success with ART against the risk of multiple births is difficult in certain cases, efforts should be made to limit the number of embryos transferred for patients undergoing ART. Such efforts will ultimately require ART patients and providers to view treatment success in terms of singleton pregnancies and births. Additionally, continued research is critical to understanding the effect of ART on maternal and child health. CDC will continue to provide updates of ART use in the United States as data become available. Acknowledgments The data used for this study were collected by the Society for Assisted Reproductive Technology (SART). The SART system is jointly supported by CDC, Atlanta, Georgia; SART, Birmingham, Alabama; and the American Society for Reproductive Medicine (ASRM), Birmingham, Alabama. The authors thank SART and ASRM, without whose contributions this work would not have been possible. References
* Fertility Clinic Success Rate and Certification Act of 1992 (FCSRCA), Public Law 102-493, October 24, 1992. † Data were not available to distinguish whether previous births were conceived naturally or conceived with ART or other infertility treatments. § Results are based on total multiple-birth risk and thus do not provide an indication of pregnancies that began as twins, triplets, or more, but reduced (either spontaneously or through medical intervention) to singletons or twins (see Figures 2--6). ¶ Estimated costs for one cycle of IVF range from $7,000 to $11,000 (8,9). Table 1  Return to top. Figure 1 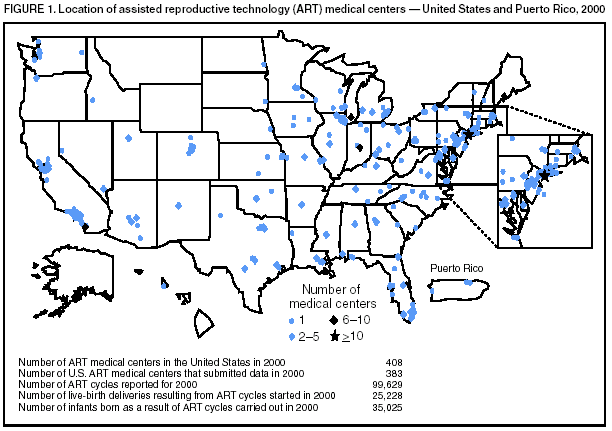 Return to top. Table 2 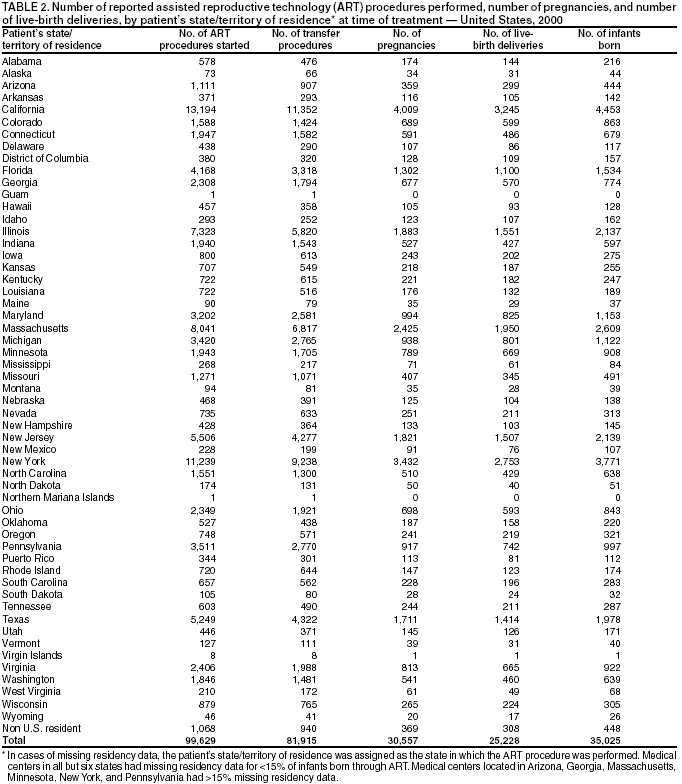 Return to top. Figure 2 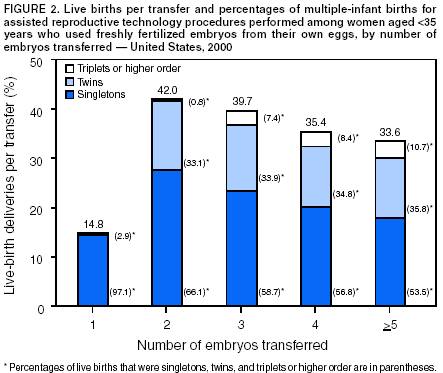 Return to top. Table 3 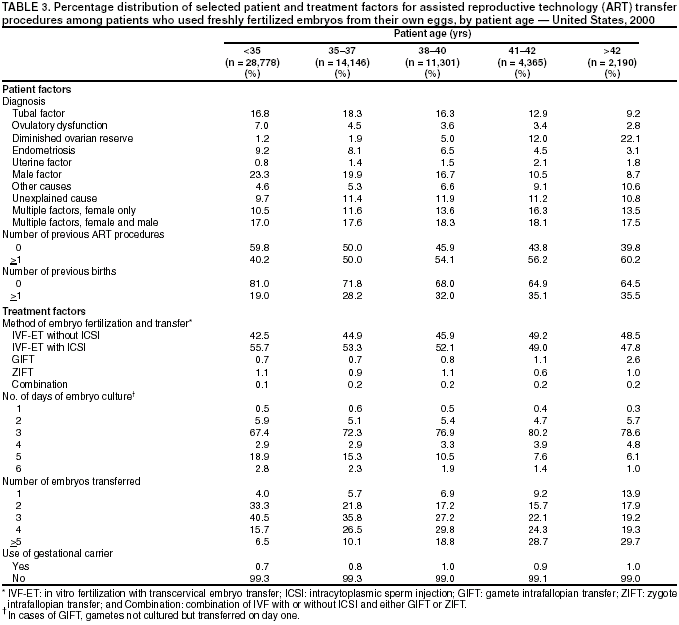 Return to top. Figure 3 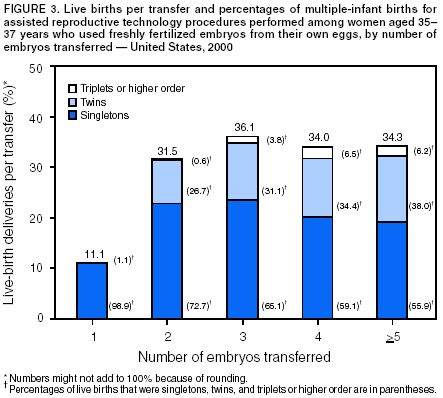 Return to top. Table 4 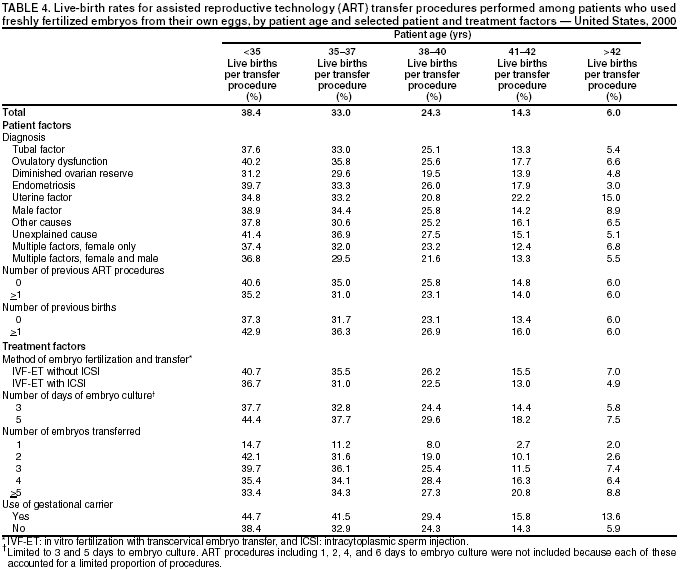 Return to top. Figure 4 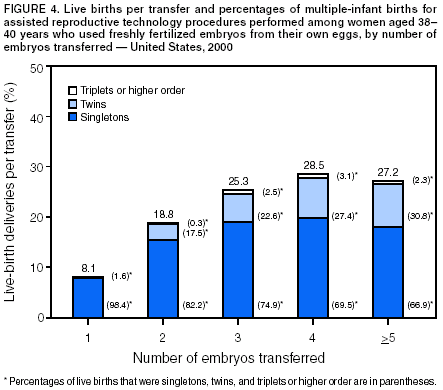 Return to top. Table 5 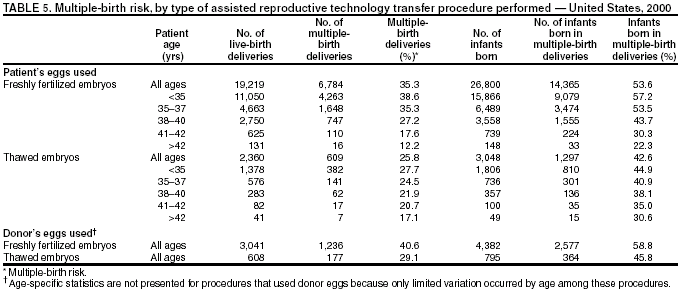 Return to top. Figure 5 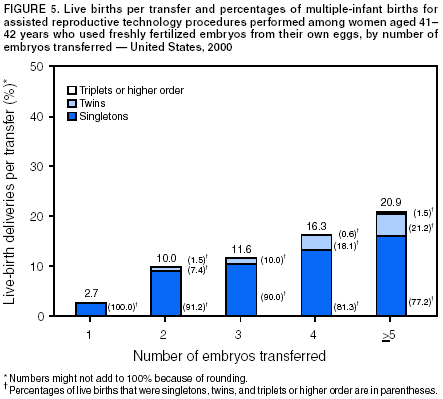 Return to top. Table 6 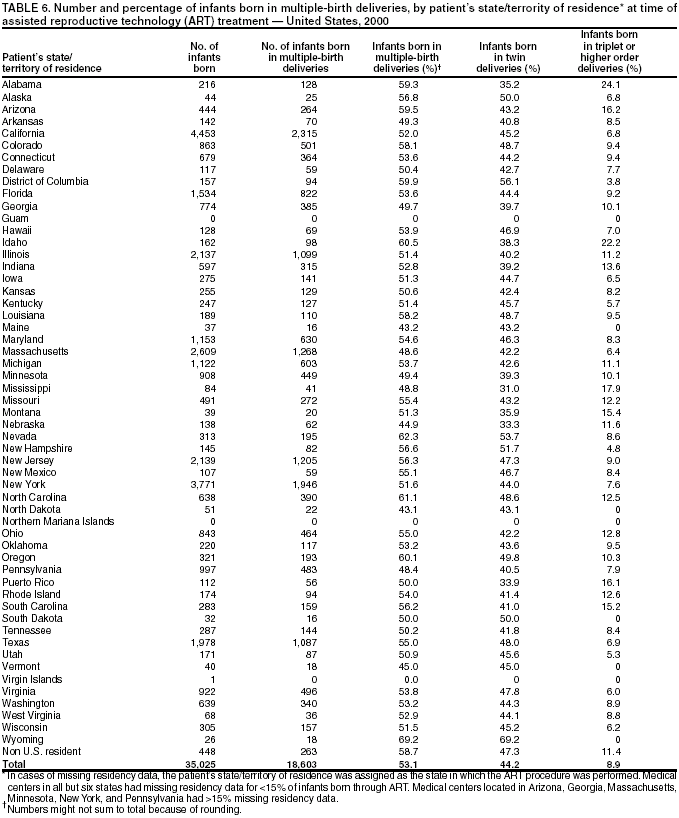 Return to top. Figure 6 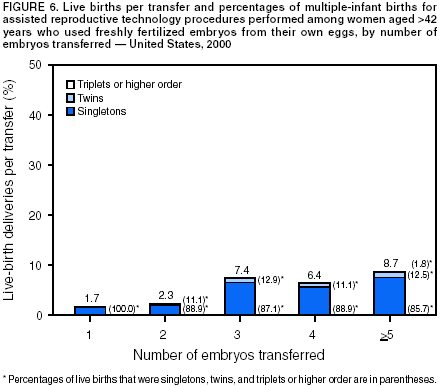 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 8/25/2003 |
|||||||||
This page last reviewed 8/25/2003
|