 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Malaria Surveillance --- United States, 1999Robert D. Newman, M.D.1,2 Abstract Problem/Condition: Malaria is caused by four species of intraerythrocytic protozoa of the genus Plasmodium (i.e., P. falciparum, P. vivax, P. ovale, or P. malariae). Malaria is transmitted by the bite of an infective female Anopheles sp. mosquito. The majority of malaria infections in the United States occur in persons who have traveled to areas with ongoing transmission. In the United States, cases can occur through exposure to infected blood products, by congenital transmission, or locally through mosquitoborne transmission. Malaria surveillance is conducted to identify episodes of local transmission and to guide prevention recommendations for travelers. Period Covered: Cases with onset of illness during 1999. Description of System: Malaria cases confirmed by blood films are reported to local and state health departments by health-care providers or laboratory staff. Case investigations are conducted by local and state health departments, and reports are transmitted to CDC through the National Malaria Surveillance System (NMSS). Data from NMSS serve as the basis for this report. Results: CDC received reports of 1,540 cases of malaria with an onset of symptoms during 1999 among persons in the United States or one of its territories. This number represents an increase of 25.5% from the 1,227 cases reported for 1998. P. falciparum, P. vivax, P. malariae, and P. ovale were identified in 46.0%, 30.7%, 4.6%, and 3.6% of cases, respectively. More than one species was present in 12 patients (0.8% of total). The infecting species was unreported or undetermined in 223 (14.5%) cases. The number of reported malaria cases acquired in Africa increased 27.6% (n = 901), compared with 1998, and an increase of 2.9% (n = 246) occurred in cases acquired in Asia, compared with 1998. Cases from the Americas increased by 19.7% (n = 274) from 1998. Of 831 U.S. civilians who acquired malaria abroad, 159 (19.1%) reported that they had followed a chemoprophylactic drug regimen recommended by CDC for the area to which they had traveled. Three patients became infected in the United States, all through probable local mosquitoborne transmission. Five deaths were attributed to malaria, all caused by P. falciparum. Interpretation: The 25.5% increase in malaria cases in 1999, compared with 1998, resulted primarily from increases in cases acquired in Africa and the Americas. This increase is possibly related to a change in the system by which states report to CDC, but it could also have resulted from local changes in disease transmission, increased travel to these regions, improved reporting to state and local health departments, or a decreased use of effective antimalarial chemoprophylaxis. In the majority of reported cases, U.S. civilians who acquired infection abroad were not on an appropriate chemoprophylaxis regimen for the country where they acquired malaria. Public Health Actions: Additional information was obtained concerning the five fatal cases and the three infections acquired in the United States. The NMSS surveillance form was modified to gather more detailed information regarding compliance with prescribed chemoprophylaxis regimens. Persons traveling to a malarious area should take one of the recommended chemoprophylaxis regimens appropriate to the region of travel, and travelers should use personal protection measures to prevent mosquito bites. Any person who has been to a malarious area and who subsequently develops a fever or influenza-like symptoms should seek medical care immediately; investigation should include a blood-film test for malaria. Malaria infections can be fatal if not diagnosed and treated promptly. Recommendations concerning prevention of malaria can be obtained from CDC. IntroductionMalaria is caused by infection with one or more of four species of Plasmodium (i.e., P. falciparum, P. vivax, P. ovale, and P. malariae) that can infect humans. The infection is transmitted by the bite of an infective female Anopheles sp. mosquito. Malaria infection remains a devastating global problem, with an estimated 300--500 million cases occurring annually. Forty-one percent of the world's population lives in areas where malaria is transmitted (e.g., parts of Africa, Asia, the Middle East, Central and South America, Hispaniola, and Oceania) (1), and 700,000--2.7 million persons die of malaria each year, 75% of them African children (2). In previous years, malaria was endemic throughout much of the continental United States; an estimated 600,000 cases occurred during 1914 (3). During the late 1940s, a combination of improved socioeconomic conditions, water management, vector-control efforts, and case management was successful at interrupting malaria transmission in the United States. Since then, malaria case surveillance has been maintained to detect locally acquired cases that could indicate the reintroduction of transmission and to monitor patterns of antimalarial drug resistance experienced by U.S. travelers. Through 1999, the majority of cases of malaria diagnosed in the United States have been imported from regions of the world where malaria transmission is known to occur, although congenital infections and infections resulting from exposure to blood or blood products are reported in the United States also. In addition, a limited number of cases are reported that might have been acquired through local mosquitoborne transmission (4). State and local health departments and CDC investigate malaria cases acquired in the United States, and CDC analyzes imported cases to detect trends in acquisition. This information has been used to guide malaria prevention recommendations for travelers abroad. For example, an increase in P. falciparum malaria among U.S. travelers to Africa, an area with increasing chloroquine resistance, prompted CDC to change the recommended chemoprophylaxis regimen from chloroquine to mefloquine in 1990 (5). The signs and symptoms of malaria illness are varied, but the majority of patients experience fever. Other common symptoms include headache, back pain, chills, increased sweating, myalgia, nausea, vomiting, diarrhea, and cough. A diagnosis of malaria should be considered for persons who experience these symptoms and who have traveled to an area with known malaria transmission. Malaria should also be considered in the differential diagnoses of persons who experience fevers of unknown origin, regardless of their travel history. Untreated P. falciparum infections can rapidly progress to coma, renal failure, pulmonary edema, and death. Asymptomatic parasitemia can occur among persons who have been long-term residents of malarious areas. This report summarizes malaria cases reported to CDC with onset of symptoms in 1999. MethodsData SourcesMalaria case data are reported to the National Malaria Surveillance System (NMSS) and the National Notifiable Diseases Surveillance System (NNDSS) (6). Although both systems rely on passive reporting, the numbers of reported cases might differ because of differences in collection and transmission of data. A major difference in the data collected in these two systems is that NMSS receives more detailed clinical and epidemiologic data regarding each case (e.g., information concerning the area to which the infected person has traveled). This report presents only data regarding cases reported to NMSS. Cases of blood-film--confirmed malaria among civilians and military personnel are identified by health-care providers or laboratories. Each slide-confirmed case is reported to local or state health departments and to CDC on a uniform case report form that contains clinical, laboratory, and epidemiologic information. CDC staff review all report forms when received and request additional information, if necessary (e.g., when no recent travel to a malarious country is reported). Reports of other cases are telephoned directly by health-care providers to CDC, usually when assistance with diagnosis or treatment is requested. All cases that have been acquired in the United States are investigated, including all induced and congenital cases and possible introduced or cryptic cases. Information derived from uniform case report forms is entered into a database and analyzed annually. DefinitionsThe following definitions are used in this report:
This report also uses terminology derived from the recommendations of the World Health Organization (7). Definitions of the following terms are included for reference.
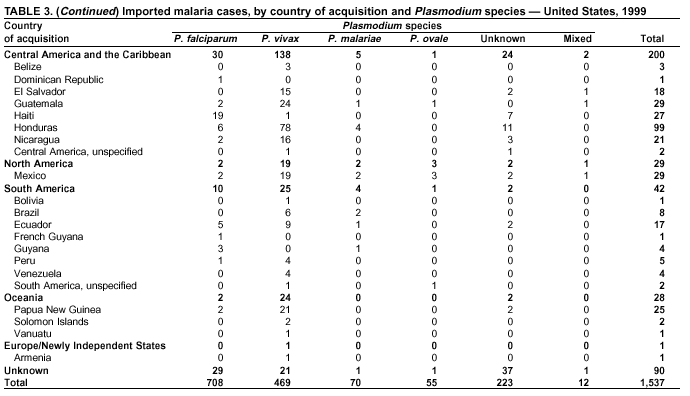
Microscopic Diagnosis of MalariaThe early diagnosis of malaria requires that physicians consider malaria in the differential diagnosis of every patient who is experiencing fever; the evaluation of such a patient should include taking a comprehensive travel history. If malaria is suspected, a Giemsa-stained film of the patient's peripheral blood should be examined for parasites. Thick and thin blood films must be prepared properly because diagnostic accuracy depends on blood-film quality and experienced laboratory personnel* (see Appendix for procedures for accurately diagnosing malaria). ResultsGeneral SurveillanceDuring 1999, CDC received 1,540 malaria case reports occurring among persons in the United States and its territories, representing a 25.5% increase from the 1,227 cases reported for 1998 (8). This incidence is the second highest number of reported cases since 1980 and represents the highest number of U.S. civilian cases reported in the past 30 years (Table 1). In 1999, a total of 833 cases occurred among U.S. civilians, compared with 636 cases reported for 1998, whereas the number of cases among foreign civilians also increased from 361 cases to 381 (Figure 1). In 1999, cases among U.S. military personnel also increased from 22 to 55. In 271 cases, information was insufficient to determine civilian or military status. Plasmodium SpeciesThe infecting species of Plasmodium was identified in 1,317 (85.5%) of the cases reported in 1999. P. falciparum and P. vivax were identified in blood films from 46.0% and 30.7% of infected persons, respectively (Table 2). The 708 P. falciparum cases reported for 1999 represented a 34.9% increase from the 525 cases in 1998, whereas the number of P. vivax infections increased by 1.7% (from 464 in 1998 to 472 in 1999). Among 1,261 cases in which both the region of acquisition and the infecting species were known, 78.5% of infections acquired in Africa were attributed to P. falciparum; 9.3% were attributed to P. vivax. The converse was true of infections acquired in the Americas and Asia: 74.9% and 78.2% were attributed to P. vivax, and only 17.3% and 12.5% were attributed to P. falciparum, respectively. Region of Acquisition and DiagnosisApproximately 99% (n = 1,537) of reported cases were imported. Of 1,447 imported cases in which the region of acquisition was known, the majority, 62.3% (n = 901), were acquired in Africa; 18.7% (n = 271) and 17.0% (n = 246) were acquired in the Americas and Asia, respectively (Table 3). The highest concentration of cases acquired in Africa came from countries in western Africa (68.6%; n = 618), whereas the majority of cases acquired in Asia came from the Indian subcontinent (69.1%; n = 170). The other regions where imported cases of malaria were acquired were Central America and the Caribbean (13.8%; n = 200), South America (2.9%; n = 42) and Oceania (1.9%; n = 28). Information regarding region of acquisition was missing for 90 (5.9%) of the imported cases. The number of reported malaria cases acquired in Africa increased 27.6% (n = 901), compared with 1998, and a 19.7% (n = 271) increase in the Americas occurred, compared with 1998. Cases from Asia increased by a lesser margin (2.9%; n = 246), compared with 1998. In the United States, the six health departments reporting the highest number of malaria cases were New York City (n = 246), California (n = 239), Texas (n = 119), Minnesota (n = 82), Virginia (n = 80), and Illinois (n = 80) (Figure 2). Of these, only Minnesota reported a decrease in cases in 1999, compared with 1998. This overall increase in reported number of cases might be a result of efforts to increase reporting from states or reflect an increased rate of international travel, a greater risk for malaria among travelers, improved access to health care, or more sensitive surveillance by state and local health departments. Interval Between Arrival and IllnessThe interval between date of arrival in the United States and onset of illness and the infecting Plasmodium species were known for 650 (42.3%) of the imported cases of malaria (Table 4). Symptoms began after arrival in the United States for 590 (90.8%) of these patients. Clinical malaria developed within 1 month after arrival in 370 (83.1%) of the 445 P. falciparum cases and in 65 (41.7%) of the 156 P. vivax cases (Table 4). Only 7 (1.2%) of the 590 persons became ill >1 year after return to the United States. An additional 60 (9.2%) persons reported becoming ill before arriving in the United States. Imported Malaria CasesImported Malaria Among U.S. Military Personnel In 1999, a total of 55 cases of imported malaria were reported among U.S. military personnel. Of the 51 cases for whom information regarding chemoprophylaxis use was available, 14 patients were not using any prophylaxis. Imported Malaria Among Civilians A total of 1,212 imported malaria cases were reported among civilians. Of these, 831 (68.6%) cases occurred among U.S. residents, and 381 (31.4%) cases occurred among residents of other countries (Table 5). Of the 831 imported malaria cases among U.S. civilians, 550 (66.2%) had been acquired in Africa, an increase of 39.6% from cases reported in 1998. Asia accounted for 118 (14.2%) cases of imported malaria among U.S. civilians, whereas travel to the Central American and Caribbean regions accounted for an additional 91 (10.6%) cases. Of the 381 imported cases among foreign civilians, the majority of cases were acquired in either Africa (n = 207; 54.3%) or Asia (n = 85; 22.3%). Antimalarial Chemoprophylaxis UseChemoprophylaxis Use Among U.S. Civilians Information concerning chemoprophylaxis use and travel area was known for 768 (92.4%) of the 831 U.S. civilians who had imported malaria. Of these 768 persons, 498 (64.8%) had not taken any chemoprophylaxis, and 77 (10.0%) had not taken a CDC-recommended drug for the area visited (9). Only 159 (20.7%) U.S. civilians had taken a CDC-recommended medication (9). Data for the specific drug taken were missing for the remaining 36 (4.7%) travelers. A total of 125 (78.6%) patients on CDC-recommended prophylaxis had taken mefloquine weekly; eight (5.0%) had taken doxycycline daily; and 14 (8.8%) who had traveled only in areas where chloroquine-resistant malaria has not been documented, had taken chloroquine weekly. Twelve patients (7.5%) had taken combinations of drugs that included >1 CDC-recommended drugs for the travel region. Of the 77 patients taking a nonrecommended drug, 59 (76.6%) reported taking chloroquine either alone or in combination with another ineffective drug during travel to an area where chloroquine resistance had been documented. Malaria Infection After Recommended Prophylaxis Use A total of 214 patients (i.e., 159 U.S. civilians, 34 persons in the U.S. military, 10 foreign civilians, and 11 persons whose information regarding their status was missing) experienced malaria after taking a recommended antimalarial drug for chemoprophylaxis. Information regarding infecting species was available for 190 (88.8%) patients taking a recommended antimalarial drug; the infecting species was undetermined for the remaining 24. Cases of P. vivax or P. ovale After Recommended Prophylaxis Use. Of the 214 patients who experienced malaria after recommended chemoprophylaxis use, 103 cases (48.1%) were caused by P. vivax and 15 (7.0%) by P. ovale. Notes on the malaria case surveillance reports indicated that 26 (22.0%) of these 118 patients were noncompliant with antimalarial prophylaxis. A total of 33 (28.0%) cases of P. vivax or P. ovale occurred >45 days after arrival in the United States. These cases were consistent with relapsing infections and, thus, do not indicate prophylaxis failures. Information was insufficient (because of missing data regarding symptom onset or return date) to assess whether 78 cases were relapsing infections. Seven cases, all caused by P. vivax, occurred <45 days after the patient returned to the United States. Of these patients, three were known to be noncompliant with their antimalarial chemoprophylaxis. Region of acquisition varied for the four patients who were not known to be noncompliant (two from Central America, one from South America, and one from Papua New Guinea). Blood samples were not available; therefore, serum drug levels were not measured for any of these patients. The probable explanations for these cases are either inappropriate dosing or noncompliance that was not reported. Evidence is lacking that would indicate any new area of chloroquine-resistant P. vivax. Cases of P. falciparum and P. malariae After Recommended Prophylaxis Use. The remaining 96 cases of malaria reported among persons who had taken a recommended antimalarial drug for chemoprophylaxis include 65 cases of P. falciparum, 7 cases of P. malariae, and 24 cases in which the infecting species was unidentified. A total of 59 of the 65 P. falciparum cases among those who reported taking a recommended antimalarial drug were acquired in Africa, two in the Caribbean, and one in Asia. In 30 (46.2%) of these 65 cases, noncompliance with antimalarials was reported. Of the remaining 35 cases of P. falciparum for which the patient either specifically reported compliance with the regimen (n = 4) or compliance was unknown (n = 31), the majority were acquired in Africa (n = 32): 21 in western Africa, seven in eastern Africa, one in central Africa, one in southern Africa, and one in an unspecified African region. Three cases were acquired outside Africa: two in the Caribbean (Haiti) and one in Asia (Laos/Thailand). Serum drug levels were available for two of these 35 patients. In both cases, the patients took mefloquine for prophylaxis for travel to Africa, and serum drug levels were below the therapeutic threshold <1 month after return, indicating either noncompliance with the recommended regimen or malabsorption of the drug. The probable explanations for the cases without serum drug levels are either inappropriate dosing or noncompliance. Five of the seven P. malariae cases among those who reported taking a recommended antimalarial drug were acquired in Africa. In four (57.1%) of these seven cases, noncompliance with antimalarials was reported. In three cases, it was unknown whether the patient complied with prophylaxis; two had traveled in the Americas, and one in Africa. Purpose of TravelPurpose of travel to malaria-endemic areas was reported for 666 (80.1%) of the 831 U.S. civilians with imported malaria (Table 6). Of the U.S. civilians with malaria, the largest percentage (39.1%) were persons who had visited friends or relatives in malarious areas; the second and third largest percentages, 10.7% and 9.2%, had traveled for tourism and to do missionary work, respectively. Malaria During PregnancyA total of 37 cases of malaria were reported among pregnant women in 1999, representing 7.0% of cases among women. Fourteen (37.8%) were among U.S. civilians. Eleven of these 14 women (78.6%) had traveled to visit friends and relatives, of whom 92.9% traveled in Africa. Only two pregnant women (14.3%) reported taking prophylaxis, compared with 33.2% of nonpregnant women. Twelve women (85.7%) were hospitalized, compared with 56.3% of nonpregnant women. Malaria Acquired in the United StatesCongenital Malaria No cases of congenital malaria were reported in 1999. Cryptic Malaria Three cases of cryptic malaria were reported in 1999 (10,11) and are described in the following case reports:
Induced Malaria No cases of induced malaria were reported in 1999. Deaths Attributed to MalariaFive deaths attributable to malaria were reported in 1999 and are described in the following case reports:
DiscussionA total of 1,540 cases of malaria were reported to CDC for 1999, representing a 25.5% increase from the 1,227 cases reported for 1998. This change primarily resulted from an increase in cases acquired in Africa and the Americas. Beginning in 2000, CDC began to routinely contact state health departments to ask for outstanding reports from the previous reporting year, or for a statement that reporting was complete. That system change might account for the increase in cases in 1999, compared with 1998, although other possibilities include improved reporting to state health departments, increased international travel, changing patterns of travel (e.g., immigration from malarious areas or adventure tourism), or a decreased use of effective antimalarial chemoprophylaxis. One reason for conducting malaria surveillance is to monitor emergence of drug resistance and the consequent failure of chemoprophylaxis; however, >60% of imported malaria among U.S. civilians occurred among persons who were either not taking prophylaxis or taking nonrecommended prophylaxis for the region to which they were traveling. Of the 89 persons who reported taking appropriate prophylaxis and for whom adequate information was available regarding species and onset of symptoms to indicate that the infection was a primary infection rather than a relapse, for 42 cases (i.e., 35 P. falciparum, four P. vivax, and three P. malariae), insufficient information was available to determine whether they represented problems with compliance while using proper antimalarial chemoprophylaxis, reporting errors, or emerging drug resistance. However, no conclusive evidence existed to indicate a single national or regional source of infection among this group of patients or the failure of a particular chemoprophylactic regimen. Health-care providers are encouraged to contact CDC rapidly if they suspect chemoprophylaxis failure, thus enabling measurement of serum drug levels of the antimalarial drug in question. CDC has received an increased number of reports of U.S. civilians who fail to take chemoprophylaxis, take an inappropriate regimen, or are not optimally compliant with the prescribed regimen. Therefore, CDC revised the NMSS case report form in 2001 to facilitate collection of more thorough data regarding chemoprophylaxis. The current form solicits more detailed information regarding the prescribed regimen (including the use of atovaquone-proguanil [Malarone™; manufactured by GlaxoSmithKline], a drug approved in the United States in July 2000 for treatment and chemoprophylaxis of malaria), the degree of compliance with the regimen, and the reasons for noncompliance, if any. Data gathered from the responses to these questions will be useful in generating public health messages to improve use of antimalarial chemoprophyalxis, and therefore, decrease malaria-associated morbidity and mortality among U.S. civilians. The importance of taking correct precautions and chemoprophylaxis is underscored by the five fatal cases of malaria that occurred in the United States in 1999. An earlier review of deaths attributed to malaria in the United States identified key risk factors for fatal malaria, including failure to take recommended antimalarial chemoprophylaxis, refusal of or delay in seeking medical care, and misdiagnosis (12). The occurrence of 14 cases of malaria among pregnant U.S. civilians is cause for concern. Malaria during pregnancy among nonimmune women is more likely to result in severe disease or contribute to an adverse outcome than malaria in a nonpregnant woman, and might also adversely affect the fetus (13,14). Pregnant travelers should be counseled to avoid travel to malarious areas, if possible. If deferral of travel is impossible, pregnant women should be informed that the risks for malaria outweigh those associated with prophylaxis, and that safe chemoprophylaxis regimens are available. Specific guidance for pregnant travelers is available from CDC's website at http://www.cdc.gov/travel/mal_preg_pub.htm (accessed November 30, 2001). Signs and symptoms of malaria are often vague, but fever is usually present. Other symptoms include headache, chills, increased sweating, back pain, myalgia, diarrhea, nausea, vomiting, and cough. Prompt diagnosis requires that malaria be included in the differential diagnosis of illness in a febrile person with a history of travel to a malarious area. Clinicians should ask all febrile patients for a travel history, including when evaluating febrile illnesses in international visitors, immigrants, refugees, migrant laborers, and international travelers. Treatment for malaria should be initiated immediately after the diagnosis has been confirmed by a positive blood film. Treatment should be determined on the basis of the infecting Plasmodium species, the probable geographic origin of the parasite, the parasite density, and the patient's clinical status (15). Although nonfalciparum malaria rarely causes complications, persons who experience diagnosed P. falciparum infection are at risk for developing severe, life-threatening complications. Health-care workers should be familiar with prevention, recognition, and treatment of malaria and are encouraged to consult appropriate sources for malaria treatment recommendations or call CDC's National Center for Infectious Diseases, Division of Parasitic Diseases at 770-488-7788. Detailed recommendations for preventing malaria are available 24 hours a day from CDC by telephone at 877-394-8747 (voice information system) or 888-232-3299 (facsimile request line), or on the Internet at http://www.cdc.gov/travel/diseases.htm#malaria (accessed November 30, 2001). In addition, CDC biannually publishes recommendations in the Health Information for International Travel (9), which is available for purchase from the Public Health Foundation at 877-252-1200 or 301-645-7773; it is also available and updated more frequently on CDC's Internet site at http://www.cdc.gov/travel (accessed November 30, 2001). CDC provides support for the diagnosis of malaria through DPDx, a program that enhances diagnosis of parasitic diseases in the United States and the world. It includes an Internet site (http://www.dpd.cdc.gov/dpdx [accessed November 30, 2001]) that contains information regarding laboratory diagnosis, geographic distribution, clinical features, treatment, and life cycles of >100 species of parasites. The DPDx Internet site is also a portal for diagnostic assistance through telediagnosis. Digital images captured from diagnostic specimens are submitted for diagnostic consultation through electronic mail. Because laboratories can transmit images to CDC and rapidly obtain answers to their inquiries, this system allows more efficient diagnosis of difficult cases and more rapid dissemination of information. Approximately 36 laboratories in 34 states have or are in the process of acquiring the hardware to perform telediagnosis. AcknowledgmentsThe authors acknowledge the state, territorial, and local health departments, health-care providers, and laboratories for reporting this information to CDC. References
* To obtain confirmation diagnosis of blood films from questionable cases and to obtain appropriate treatment recommendations, contact either your state or local health department or CDC's National Center for Infectious Diseases, Division of Parasitic Diseases, Malaria Epidemiology Branch at 770-488-7788. Table 1 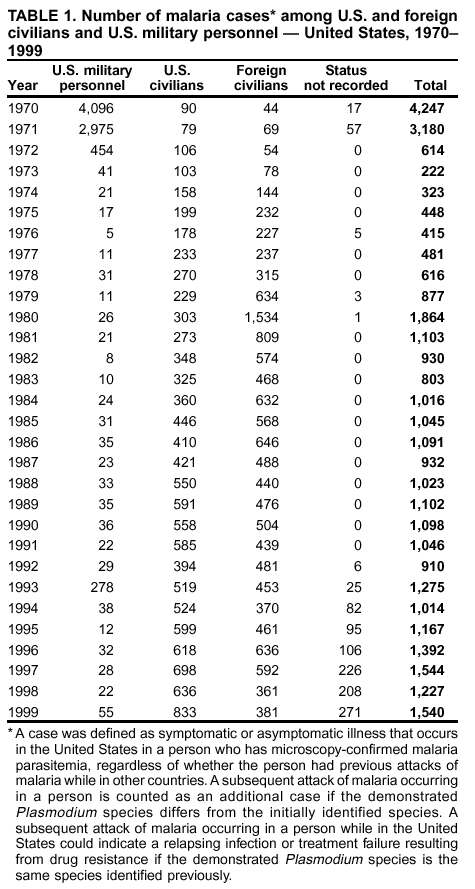 Return to top. Figure 1 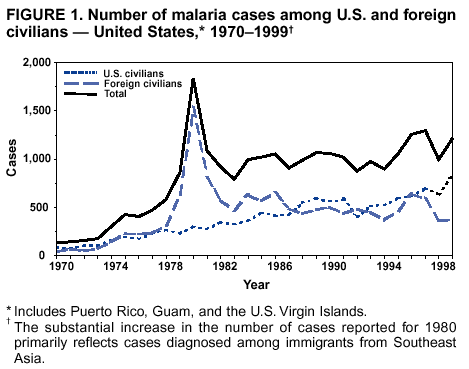 Return to top. Table 2 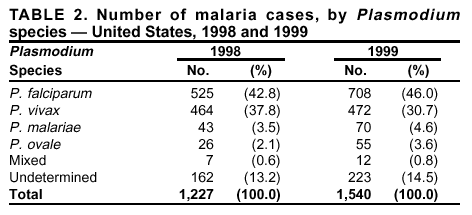 Return to top. Figure 2 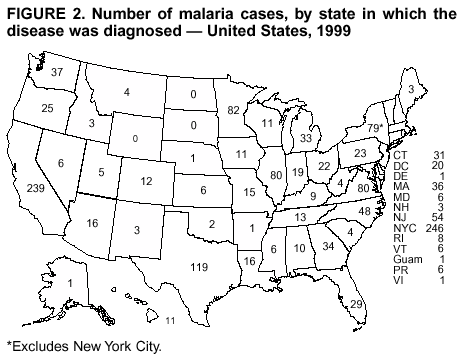 Return to top. Table 3 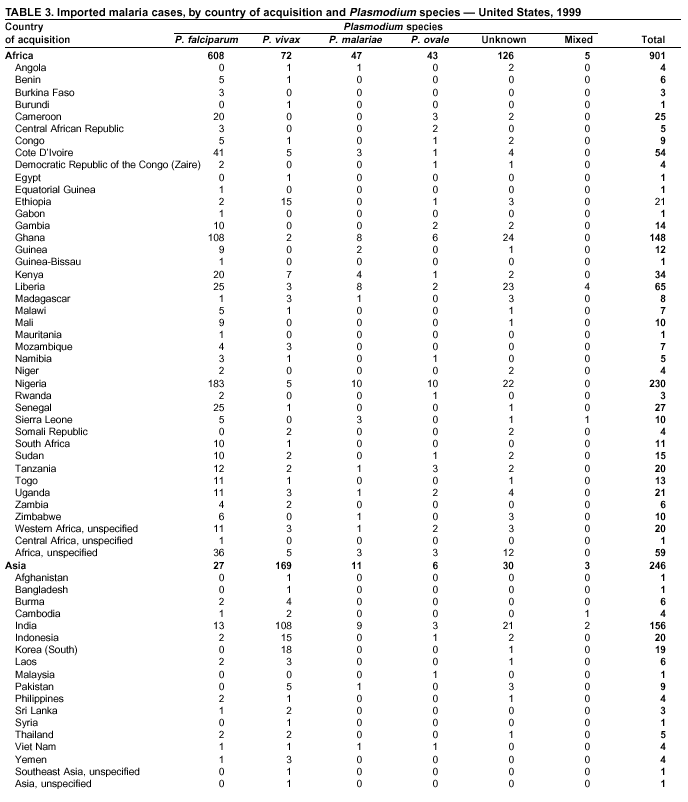
 Return to top. Table 4 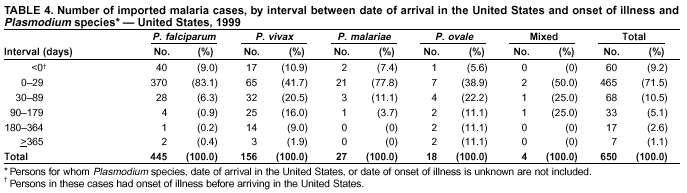 Return to top. Table 5 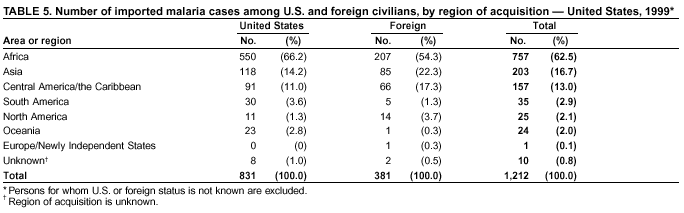 Return to top. Table 6 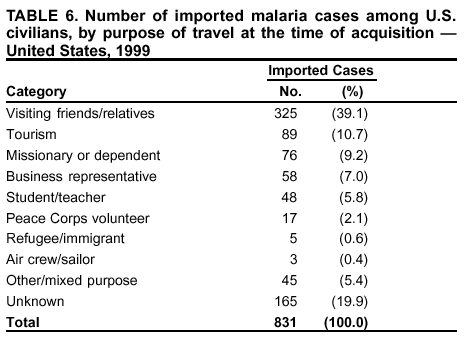 Return to top. AppendixMicroscopic Procedures for Diagnosing MalariaTo establish the diagnosis of malaria, a blood film must be prepared from fresh blood obtained by pricking the patient's finger (Figures A-1 and A-2).* The thin film is fixed in methanol before staining; the thick film is stained unfixed. Certain hospitals have a Wright-Giemsa stain available, which is acceptable; however, Wright stain alone will not reliably indicate Plasmodium parasites. For best results, the film should be stained with a 3% Giemsa solution (pH of 7.2) for 30--45 minutes. In P. falciparum infections, the parasite density should be estimated by counting the percentage of red blood cells infected --- not the number of parasites --- under an oil immersion lens on a thin film. Thick blood films are more sensitive in detecting malaria parasites because the blood is concentrated, allowing a greater volume of blood to be examined. However, thick films are more difficult to read, and thin films might be preferred by laboratories that have limited experience. Plasmodium parasites are always intracellular, and they demonstrate, if stained correctly, blue cytoplasm with a red chromatin dot. Common errors in reading malaria films are caused by platelets overlying a red blood cell, concern regarding missing a positive slide, and misreading artifacts as parasites. Persons suspected of having malaria, but whose blood films do not indicate the presence of parasites, should have blood films repeated approximately every 12--24 hours for 3 consecutive days. If films remain negative, then the diagnosis of malaria is unlikely. For rapid diagnosis, the thick and thin films should be made on separate slides. The thin film should be air-dried, fixed with methyl alcohol, and immediately stained. If no parasites are visible on the thin film, the laboratorian should wait until the thick film is dry, then examine it for organisms that might not have been detected on the thin preparation.
* In Figures A-1 and A-2, the hands are illustrated ungloved to better indicate their placement during the procedures. However, wearing gloves while processing blood specimens is recommended to prevent transmission of bloodborne pathogens (MMWR 1988;37:377--82, 387--8 and MMWR 1987;36[No. S2]). Figure A-1 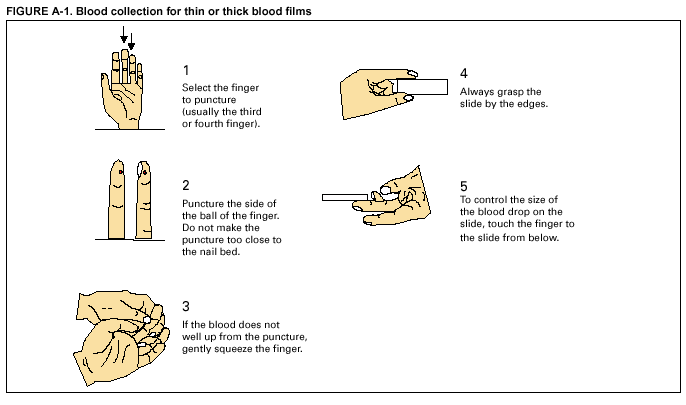 Return to top. Figure A-2 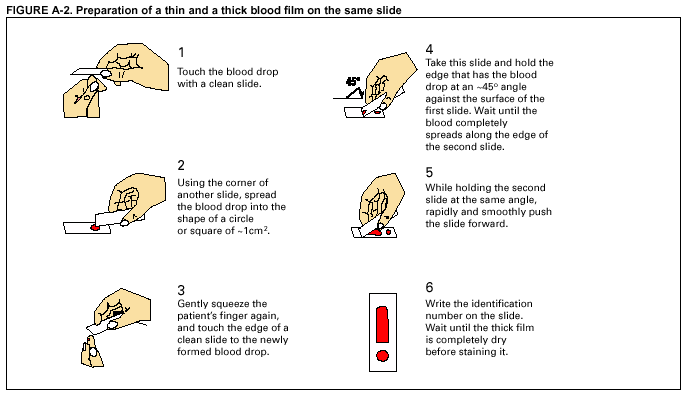 Return to top.
All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 3/13/2002 |
|||||||||
This page last reviewed 3/13/2002
|