 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Smoking Prevalence Among Women of Reproductive Age --- United States, 2006Cigarette smoking continues to be the leading cause of preventable morbidity and mortality in the United States. Women of reproductive age (18--44 years) who smoke risk adverse pregnancy outcomes and adverse health consequences for themselves. They also are exposing their children to secondhand smoke and modeling behavior that will increase the likelihood that their children will become smokers. CDC analyzed state-specific prevalence of smoking and attempts to quit among women of reproductive age, using 2006 data from the Behavioral Risk Factor Surveillance System (BRFSS). The data indicated a six-fold difference between the state and territory with the highest and lowest prevalence (range: 5.8% [U.S. Virgin Islands (USVI)]--34.7% [Kentucky]). Among women of reproductive age, those aged 18--24 years were most likely to have attempted to quit (68.4%), but least likely to have quit smoking (26.3%). Successful prevention and cessation interventions for this group of women can protect their own and their children's health. BRFSS is a state-based, random-digit--dialed telephone survey of the noninstitutionalized, U.S. civilian population aged >18 years. Estimates were weighted by age and sex distribution for each state and area population, data were adjusted for nonresponse, and 95% confidence intervals were calculated. Statistical software was used to account for the complex sampling design. Aggregated data were examined to determine the prevalence of current smokers, percentage of ever smokers who had quit, and quit attempts by age, race/ethnicity, education, and marital status among women of reproductive age. Puerto Rico and USVI were excluded in the calculation of median prevalence rates for current smoking, percentage ever smokers who had quit, and quit attempts. Median response rate across 50 states and the District of Columbia was 51.4% (range: 35.1% [New Jersey] to 66.0% [Nebraska]). Respondents were asked, "Have you smoked at least 100 cigarettes in your entire life?" and "Do you now smoke cigarettes every day, some days, or not at all?" Current smokers were defined as those who reported having smoked >100 cigarettes during their lifetime and who currently smoke every day or some days. Former smokers were defined as those who reported having smoked >100 cigarettes during their lifetime and currently do not smoke. Never smokers were defined as those who reported not smoking >100 cigarettes during their lifetime. Quit attempt was defined as the percentage of daily smokers (a subset of current smokers) who had quit for at least 1 day in the past year because they were trying to quit smoking. The percentage of ever smokers who had quit is the number of former smokers divided by the number of ever smokers. The analysis only included women aged 18--44 years. Median state prevalence of current smoking was 22.4% (Table 1). Smoking prevalence was highest among non-Hispanic whites (24.5%), those with a high school diploma (29.4%), those with less than a high school diploma (28.3%), and divorced, widowed, or separated women (34.7%), but did not differ by age group (Table 2). The percentage of ever smokers who had quit varied among states and territories. USVI (51.0%) and California (50.4%) had the highest rates, whereas Louisiana (26.8%) and Mississippi (27.3%) had the lowest rates. Among ever smokers who had quit, college graduates (59.7%) and married women (49.6%) had the highest percentages, and women aged 18--24 years (26.3%), non-Hispanic blacks (24.5%), and those with less than a high school diploma (24.7%) had the lowest percentages. For daily smokers who made a quit attempt, the highest percentages occurred among women aged 18--24 years (68.4%) and non-Hispanic blacks (68.1%). The highest proportion of those who made a quit attempt in the previous year lived in Delaware (67.7%), followed by Puerto Rico (66.6%); the lowest proportions were in Arizona (33.6%) and Kentucky (43.4%). Reported by: E Maurice, MS, J Kahende, PhD, A Trosclair, MS, S Dube, PhD, MPH, C Husten, MD, Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The prevalence of smoking among women of reproductive age (aged 18--44 years) in 2006 is similar to results obtained from the Pregnancy Risk Assessment and Monitoring System (PRAMS), which measures the range of maternal tobacco use from 26 reporting areas (2004: 12.3% [Utah] to 39.5% [West Virginia]) (1). A gradual decline in the median state smoking prevalence among women of reproductive age occurred from 1996 (25.9%) to 2006 (22.4%). The 22.4% median smoking prevalence for women of reproductive age reported here is higher than the 18.5% median smoking prevalence reported for women aged >18 years in a separate study of the general population (2). However, prevalence of current smoking, percentage of ever smokers who had quit smoking, and percentage of quit attempts by selected demographics were similar to the prevalences reported in that study. These comparisons are not exact because of a difference in the age range examined in these two studies. In this analysis, large variations among states were observed in smoking prevalence, the percentage of ever smokers who had quit, and quit attempts. The variations are likely the result of differences in socioeconomic determinants (e.g. race/ethnicity, education, marital status) of smoking, differing social norms regarding tobacco use, and variation in implementation of tobacco control programs and policies in states. Women of reproductive age who smoke are at increased risk for multiple adverse pregnancy-related health outcomes, including difficulty conceiving, infertility, spontaneous abortion, premature rupture of membranes, low birth weight, neonatal mortality, stillbirth, preterm delivery, and sudden infant death syndrome (SIDS) (3). These smoking-related adverse reproductive health outcomes are associated with substantial economic and societal costs. Estimated neonatal health care costs attributable to maternal smoking are approximately $366 million per year in the United States (4). In addition, women who smoke are at increased risk for adverse health outcomes, including lung and other cancers, chronic obstructive pulmonary disease, and heart disease (3). Smoking cessation is beneficial at any age, but the relative benefits of cessation are greater if women can stop smoking at younger ages, before they develop smoking-related diseases (3). In addition, parents who smoke often expose their children to secondhand smoke, with associated adverse health consequences and economic costs, and model smoking behavior to their children, potentially increasing the likelihood that their children will become smokers (5). The findings in this report are subject to at least three limitations. First, BRFSS does not survey persons in households without landline telephones or those in wireless-only telephone households, populations that might be more likely to include smokers (6,7). Preliminary findings from the National Health Interview Survey (NHIS) indicate that 10.5% of women lived in households with only wireless telephones in 2006 (8). Those findings also indicate that 25.2% of adults aged 18--24 years, 29.1% of adults aged 25--29 years, and 12.4% of adults aged 30--44 years lived in households with only wireless telephones in 2006 (7). The exclusion of persons with wireless-only telephone service might have led to underestimation of smoking prevalence. Second, the median response rate was 51.4% (range: 35.1%--66.0%). Low response rates indicate a potential for response bias; however, BRFSS estimates for current cigarette smoking are generally comparable with smoking estimates from surveys with higher response rates (6). Finally, estimates for cigarette smoking and smoking cessation attempts are based on self-report and are not validated by biochemical tests. However, self-reported data on current smoking status have high validity (6). The 2006--2007 Annual Report of the President's Cancer Panel described tobacco use as the number one cause of preventable death in the United States and the second leading cause of death in the world. Worldwide, approximately 10 million tobacco-related deaths will occur each year by 2020 if current tobacco use trends continue, with more than 1 billion tobacco-related deaths in the 21st century (8). The Institute of Medicine (IOM) has called for increasing the federal excise tax on cigarette substantially and dedicating a portion of the higher taxes or other resources to fund tobacco control efforts in each state (9). The IOM also recommends that states maintain a comprehensive integrated tobacco control strategy and fund tobacco control activities at the level recommended by CDC (9). Evidence-based comprehensive tobacco control programs that can prevent initiation, increase cessation, and eliminate exposure to secondhand smoke should be used to reduce smoking among women of reproductive age (10). The prevention and reduction of tobacco use among women of reproductive age are essential to reduce the burden of reproductive health complications from smoking and adverse health effects of children's exposure to secondhand smoke, and to improve the life expectancy of the women themselves. References
Table 1 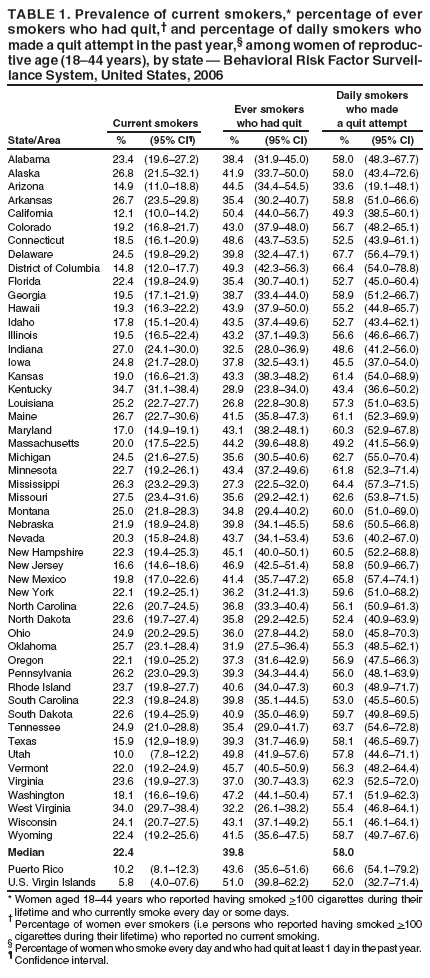 Return to top. Table 2 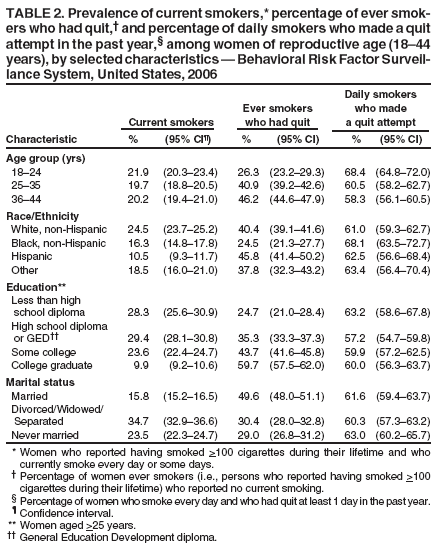 Return to top.
All MMWR HTML versions of articles are electronic conversions from typeset documents. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Date last reviewed: 8/6/2008 |
|||||||||
|