 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Fatal Rat-Bite Fever --- Florida and Washington, 2003Rat-bite fever (RBF) is a rare, systemic illness caused by infection with Streptobacillus moniliformis. RBF has a case-fatality rate of 7%--10% among untreated patients (1). S. moniliformis is commonly found in the nasal and oropharyngeal flora of rats. Human infection can result from a bite or scratch from an infected or colonized rat, handling of an infected rat, or ingestion of food or water contaminated with infected rat excreta (1). An abrupt onset of fever, myalgias, arthralgias, vomiting, and headache typically occurs within 2--10 days of exposure and is usually followed by a maculopapular rash on the extremities (1). This report summarizes the clinical course and exposure history of two rapidly fatal cases of RBF identified by the CDC Unexplained Deaths and Critical Illnesses (UNEX) Project in 2003. These cases underscore the importance of 1) including RBF in the differential diagnoses of acutely ill patients with reported rat exposures and 2) preventing zoonotic infections among persons with occupational or recreational exposure to rats. Case ReportsFlorida. In early September 2003, a previously healthy woman aged 52 years visited an emergency department (ED) with a 2-day history of headache, abdominal pain, diarrhea, lethargy, right axillary lymphadenopathy, progressive myalgias, and pain in her distal extremities. On physical examination, she was afebrile and hypotensive (blood pressure: 82/40 mmHg) with left-sided abdominal tenderness and scleral icterus; no rash was noted. Laboratory tests indicated a mildly elevated white blood cell count of 13,800 cells/µL (normal: 5,000--10,000 cells/µL), thrombocytopenia (71,000 platelets/µL [normal: 130,000--500,000 platelets/µL]), elevated alanine aminotransferase of 112 U/L (normal: 20--52 U/L), elevated aspartate aminotransferase of 154 U/L (normal: <40 U/L), elevated total bilirubin of 5.8 mg/dL (normal: 0.2--1.2 mg/dL), elevated blood urea nitrogen of 55 mg/dL (normal: 7--23 mg/dL), and elevated creatinine of 2.9 mg/dL (normal: 0.7--1.5 mg/dL). The patient was admitted to the intensive care unit, where she became increasingly hypoxic with marked anemia (hemoglobin: 8.6 g/dL [normal: 12--16 g/dL]) and increasingly severe thrombocytopenia (32,000 platelets/µL). She was treated with ciprofloxacin, metronidazole, and vancomycin for possible gram-negative sepsis and received two blood transfusions; however, she died approximately 12 hours after admission. A maculopapular rash was noted postmortem. No autopsy was performed. Peripheral blood smears obtained before death revealed abundant neutrophils and intracellular collections of filamentous bacteria (Figure). Premortem blood from a tube containing no additives or separators was inoculated onto a blood agar plate and incubated in CO2 at 95ºF (35ºC). After 72 hours, the culture demonstrated slight growth of gram-negative filamentous bacteria. UNEX was contacted for assistance, and diagnostic specimens were submitted to CDC for further laboratory evaluation. At CDC, the isolate was subcultured onto media enriched with 20% solution of sterile normal rabbit serum and incubated in a candle jar for 48 hours. Biochemical analyses identified the bacterial isolate as S. moniliformis. The 16S rRNA gene sequences amplified from DNA extracted from the patient's blood and the bacterial isolate were consistent with S. moniliformis. The patient had been employed at a pet store. She was bitten on her right index finger by a rat in the store 2 days before symptom onset and 4 days before arriving at the ED. She self-treated the wound by using antiseptic ointment immediately after being bitten. In addition, she had regular contact with several pet rats, cats, a dog, and an iguana at her home; however, no bites from these animals were reported. None of the animals were tested for S. moniliformis. Washington. In late November 2003, a previously healthy woman aged 19 years was pronounced dead on arrival at a hospital ED. No laboratory studies were performed in the ED. An acquaintance reported that the patient had experienced a 3-day history of fever, headache, myalgias, nausea, and profound weakness without cough, vomiting, diarrhea, or rash. Before her transport to the ED, she exhibited anxiety, confusion, and labored breathing. ED staff noted that she appeared jaundiced. The body was transported to the coroner's office, where an autopsy was performed. Cultures of blood and tissue from autopsy were negative for pathogenic organisms. A toxicology screen was negative. Serologic assays for leptospirosis, Epstein-Barr virus, cytomegalovirus, and viral hepatitis were negative for recent infection. Histopathology revealed findings suggestive of a systemic infectious process that included disseminated intravascular coagulopathy and inflammatory cell infiltrates in the liver, heart, and lungs. UNEX was contacted for assistance, and project staff facilitated the submission of diagnostic specimens to CDC for further laboratory evaluation. Immunohistochemical assays performed at CDC for Leptospira spp., Bartonella quintana, spotted fever and typhus group rickettsiae, flaviviruses, hantaviruses, and influenza viruses were negative. Clusters of filamentous bacteria were identified in sections of the liver and kidney by using a silver stain. The 16S rRNA gene sequence amplified from DNA extracted from paraffin-embedded, formalin-fixed samples of liver and kidney was consistent with S. moniliformis. The patient worked as a dog groomer and lived in an apartment with nine pet rats. One pet rat with respiratory symptoms had recently been prescribed oral doxycycline after having been evaluated at a veterinary clinic. Doxycycline was subsequently used to treat a second ill rat. None of the rats were tested for S. moniliformis. The patient had no known animal bites during the 2 weeks preceding her death. Reported by: WJ Pollock, MD, R Cunningham, Baptist Hospital; J Lanza, MD, S Buck, MD, PA Williams, Escambia County Health Dept, Pensacola; JJ Hamilton, MPH, R Sanderson, MA, Bur of Epidemiology, Florida Dept of Health. D Selove, MD, T Harper, Thurston County Coroner's Office; DT Yu, MD, Thurston County Dept of Health, Olympia; M Leslie, DVM, J Hofmann, MD, Washington Dept of Health. S Reagan, MPH, M Fischer, MD, A Whitney, MS, C Sacchi, PhD, P Levett, PhD, M Daneshvar, PhD, L Helsel, R Morey, Div of Bacterial and Mycotic Diseases; S Zaki, MD, C Paddock, MD, W Shieh, MD, J Sumner, J Guarner, MD, Div of Viral and Rickettsial Diseases, National Center for Infectious Diseases; D Gross, DVM, EIS Officer, CDC. Editorial Note:Although rapidly fatal pediatric cases of RBF have been described previously (2,3), similar mortality among adults has not been reported. Mortality attributed to severe systemic complications (e.g., endocarditis, myocarditis, meningitis, pneumonia, or multiple organ failure) has been documented in certain adult patients (1,4). Both patients described in this report died within 12 hours of presentation, allowing little opportunity for assessment and treatment. These case reports demonstrate that infection with S. moniliformis can cause fulminant sepsis and death in previously healthy adults. As a result, prevention of severe disease might depend on increasing the awareness of appropriate risk-reduction activities and possible symptoms of RBF among persons who have exposure to rats. Intravenous penicillin is the treatment of choice, and prompt therapy can prevent severe complications (1). Because rapid laboratory confirmation of infection with S. moniliformis might not be possible, clinicians should consider initiating empiric therapy for patients with a compatible clinical presentation and exposure history. Clinicians should consider RBF in the differential diagnosis for unexplained febrile illness or sepsis in patients reporting rat exposure. Initial symptoms might be nonspecific (Box), but a maculopapular rash and septic arthritis commonly develop (1,5). However, as demonstrated by the cases in this report, patients can have severe disease before the onset of typical symptoms. Despite its name, approximately 30% of patients with RBF do not report having been bitten or scratched by a rat (1,5). Risk factors for RBF include handling rats at home and in the workplace (e.g., laboratories or pet stores). RBF is rare in the United States, with only a few cases documented each year (1,6,7). However, because RBF is not a nationally notifiable disease, its actual incidence has not been well described. In the cases described here, diagnosis of RBF was delayed in part because of the inability to rapidly isolate or identify S. moniliformis. If infection with S. moniliformis is suspected, specific media and incubation conditions should be used (8) (Box). In the absence of a positive culture, identification of pleomorphic gram-negative bacilli in appropriate specimens might support a preliminary diagnosis (1). In the event of an unexplained death in a person with rat exposure, performing an autopsy might also be critical to identifying an etiology. Because of the high prevalence of colonization and asymptomatic infection with S. moniliformis among rodents (Box), testing and treatment of rats is not practical. Disease prevention should center on risk reduction among persons with frequent rat exposure. Adherence to simple precautions while handling rats can reduce the risk for RBF and other potential rodent-borne zoonotic infections, wound infections, and injuries. Persons should wear gloves, practice regular hand washing, and avoid hand-to-mouth contact when handling rats or cleaning rat cages (1,9). If bitten by a rat, persons should promptly clean and disinfect the wound, seek medical attention, and report their exposure history. A tetanus toxoid booster should be administered if >10 years have lapsed since the last dose (9,10). Clinicians should contact their state health departments for assistance with diagnosis of unexplained deaths or critical illnesses and cases or clusters of suspected RBF or other zoonotic infections. UNEX coordinates surveillance for unexplained deaths possibly attributed to infection throughout the United States. Cases are reported by a network of health departments, medical examiners/coroners, pathologists, and clinicians. Epidemiologic and clinical data are collected, and available clinical and pathologic specimens are obtained for reference and diagnostic testing at state, CDC, and other laboratories. State and local health departments may contact UNEX for assistance with the evaluation of unexplained deaths that occur in their jurisdictions. References
Figure 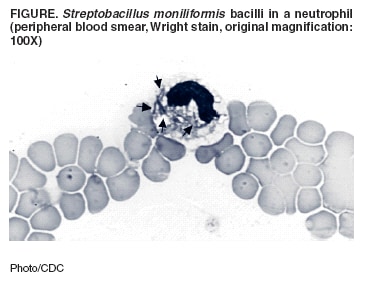 Return to top. Box  Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 1/6/2005 |
|||||||||
This page last reviewed 1/6/2005
|