 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Prevalence of Visual Impairment and Selected Eye Diseases Among Persons Aged >50 Years With and Without Diabetes --- United States, 2002Visual impairment and blindness* affect an estimated 3.4 million U.S. adults aged >40 years (1). The leading causes of visual impairment and blindness are diabetic retinopathy and age-related eye diseases (e.g., cataracts, macular degeneration, and glaucoma) (2). Diabetes affects approximately 18 million U.S. adults, of whom an estimated 30% have undiagnosed diabetes, and imposes an increased risk for eye disease (3). To characterize the prevalence of visual impairment and selected eye diseases (i.e., diabetic retinopathy, cataracts, macular degeneration, and glaucoma) among persons aged >50 years with and without diabetes, CDC analyzed data from the 2002 National Health Interview Survey (NHIS). This report summarizes the findings of that analysis, which identified a substantially higher prevalence of visual impairment and eye disease among those with diabetes compared with those without diabetes. Measures are needed to increase comprehensive eye examinations, especially among adults at high risk for blindness and visual impairment (e.g., persons aged >65 years and those with diabetes). NHIS is a stratified, multistage probability sample survey representing the U.S. civilian, noninstitutionalized population. For this analysis, respondents were classified as having diabetes if they answered "yes" to the question, "Have you ever been told by a doctor or health professional that you have diabetes or sugar diabetes?" Women who had diabetes only during pregnancy and persons who reported having borderline diabetes were classified as not having diabetes. Respondents were classified as having visual impairment (including blindness) if they answered "yes" to the question, "Do you have any trouble seeing even when wearing glasses or contact lenses?" Respondents were classified as having diabetic retinopathy, cataracts, glaucoma, or macular degeneration if they answered "yes" to the question, "Have you ever been told by a doctor or other health-care professional that you had diabetic retinopathy, cataracts, glaucoma, or macular degeneration?" The prevalence of visual impairment and selected eye diseases was determined for adults with and without diabetes and for specific characteristics (i.e., age, sex, race/ethnicity, education, and health insurance status). Logistic regression analysis was used to assess the association between diabetes status and prevalence of visual impairment or selected eye diseases while adjusting for demographic characteristics. Chi-square analysis was used to test for statistical significance. All data were weighted to reflect the age, sex, and racial/ethnic distribution of the adult population, and analyses were conducted by using statistical software. Data were age-adjusted to the 2000 U.S. standard population. All results are statistically significant (p<0.05) unless otherwise noted. In 2002, among persons aged >50 years with and without diabetes, the age-adjusted prevalence of visual impairment was 23.5% and 12.4%, respectively. The age-adjusted prevalence of diabetic retinopathy among persons aged >50 years with diabetes was 10.2%. The age-adjusted prevalence for cataracts among those with and without diabetes was 31.8% and 21.2%, respectively; for glaucoma, 8.0% and 4.3%; and for macular degeneration, 2.8% and 2.9% (Table). The prevalence of visual impairment, cataracts, and glaucoma was higher among persons aged >50 years with diabetes than among those without diabetes, overall, and for most groups examined (Table). Among persons with diabetes, the age-adjusted prevalence of visual impairment was higher among women than men (28.5% versus 19.2%) and higher among those with less than high school education than among those with high school or more education (30.5% versus 20.9%). Among persons without diabetes, the prevalence of visual impairment was higher among persons aged >65 years than persons aged 50--64 years (16.1% versus 9.2%), higher among women than men (13.6% versus 10.9%), higher among other racial/ethnic populations than non-Hispanic whites (14.1% versus 12.0%), and higher among those with less than a high school education than among those with at least a high school education (18.0% versus 11.0%). Among persons with diabetes, the prevalence of cataracts was higher among persons aged >65 years than persons aged 50--64 years (50.3% versus 16.1%), higher among women than men (37.3% versus 26.7%), and higher among non-Hispanic whites than those of other racial/ethnic populations (34.8% versus 24.1%). The prevalence of glaucoma was higher among persons aged >65 years than persons aged 50--64 years (11.7% versus 4.9%) and higher among other racial/ethnic populations than non-Hispanic whites (11.4% versus 6.8%). The prevalence of macular degeneration was higher among persons aged >65 years than persons aged 50--64 years (4.7% versus 1.1%), higher among non-Hispanic whites than other racial/ethnic populations (3.2% versus 1.4%), and higher among those with at least a high school education than those with less than a high school education (3.3% versus 1.7%). No statistically significant differences in the prevalence of diabetic retinopathy between age, sex, race/ethnicity, education, and health insurance status were observed. After data were adjusted for all demographic characteristics, persons with diabetes reported having more visual impairment (odds ratio [OR] = 2.1; 95% confidence interval [CI] = 1.8--2.5), cataracts (OR = 2.1; 95% CI = 1.8--2.4), and glaucoma (OR = 1.9; 95% CI = 1.5--2.4), compared with persons without diabetes; however, differences in prevalence of age-related macular degeneration were not statistically significant (OR = 1.0; 95% CI = 0.8--1.5). Reported by: J Saaddine, MD, S Benjamin, PhD, L Pan, MD, KM Venkat Narayan, MD, E Tierney, MPH, S Kanjilal, MPH, L Geiss, MA, Div of Diabetes Translation, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The findings in this report suggest a higher prevalence of visual impairment and eye disease among persons aged >50 years with diagnosed diabetes than among those without diabetes. Although diabetic retinopathy is a major cause of visual impairment among persons with diabetes, other causes (e.g., cataracts, glaucoma, and macular degeneration) are frequently responsible for visual impairment in persons with diabetes (4,5). The prevalence of diabetes mellitus is increasing in the United States (6). With the aging of the U.S. population, the number of older persons with diabetes is likely to increase, which suggests that a smaller proportion of visual impairment among persons with diabetes will be attributed to diabetic retinopathy. Health-care professionals should check for eye diseases and diabetic retinopathy when evaluating persons with diabetes. Yearly dilated eye examinations should be part of diabetes management in addition to managing hyperglycemia, hypertension, and lipid abnormalities. The findings in this report are subject to at least four limitations. First, self-reported visual impairment might not represent measured vision impairment; however, it does represent the perceived vision quality of a population (7). Second, the prevalence of visual impairment and eye disease documented in this report is limited to persons with diagnosed diabetes; approximately 30% of persons have undiagnosed diabetes, and a substantial proportion of persons with undiagnosed diabetes might have diabetes-related vision disorders. Third, self-reported eye diseases could be misclassified; persons might mistake their disease for other conditions, and self-reported diabetic retinopathy might not include the early stages of the disease because patients might not count it as retinopathy. Finally, the increased prevalence of visual impairment and eye disease among older persons (i.e., aged >65 years) might also be attributed to detection bias associated with higher rates of insurance coverage among persons aged >65 years versus persons aged 50--64 years (98.5% versus 88.7%; p<0.05) and, thus, higher rates of health-care use. Moreover, the high prevalence of visual impairment and eye disease among persons with diabetes in these findings might be related to more frequent use of their health-care system. Reducing visual impairment, increasing preventive eye care, and increasing use of vision rehabilitation services are public health priorities. CDC has made progress in vision health for persons with diabetes. For example, increasing comprehensive eye examination is a national objective for diabetes prevention and control programs. Although the percentage of annual comprehensive eye examinations has increased (e.g., from 58.9% in 1995 to 65.9% in 2001), the percentage is still below the 2010 national health objective of 75% (8). CDC also collaborates with the National Eye Institute through the National Eye Health Education Program (NEHEP) to increase public and professional awareness activities related to diabetic eye disease. NEHEP materials designed to educate the public and health-care providers are available at http://www.nei.nih.gov/publications/publications.htm. References
* Visual impairment is defined as best-corrected visual acuity of <20/40 in the better-seeing eye. Blindness is defined as best-corrected visual acuity of <20/200 in the better-seeing eye. Table 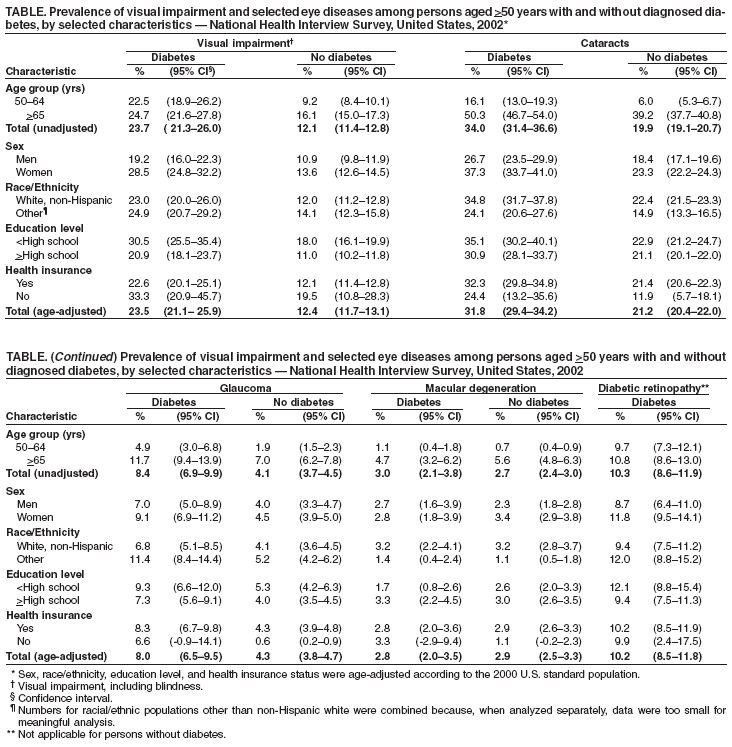 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/18/2004 |
|||||||||
This page last reviewed 11/18/2004
|