 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Outbreak of Histoplasmosis Among Industrial Plant Workers --- Nebraska, 2004In February 2004, the Nebraska Health and Human Services System (NHHSS) notified CDC about an outbreak of histoplasmosis among workers at a local agricultural processing plant (plant A). Three workers at the plant had acute, febrile, respiratory illness; two had serologic evidence of histoplasmosis. NHHSS and CDC conducted an investigation to determine the source of transmission and the extent of the outbreak. This report summarizes the findings of that investigation, which confirmed occupationally acquired histoplasmosis. Additional measures might be necessary to minimize risk for histoplasmosis among persons who work in the agricultural industry in areas where it is endemic. Plant A is located in an area with historically low endemicity for histoplasmosis. However, in September 2003, NHHSS had investigated an outbreak of histoplasmosis at plant A related to excavation of soil and repair of an underground outdoor pipe. Approximately 3 months later, on January 2, 2004, the excavated soil (i.e., spoil pile) was moved, under standard protocol and appropriate precautions, to an off-site landfill. None of the plant workers with suspected histoplasmosis in the 2004 outbreak had participated in removal of the spoil pile, nor had they been implicated in the 2003 outbreak. To identify workers with symptomatic acute pulmonary histoplasmosis acquired during the 2004 outbreak, a cohort study was conducted among plant workers. To better identify risk factors for disease, a nested case-control study was performed among workers who had laboratory testing for histoplasmosis. For the cohort study, all workers were instructed by plant safety managers to complete a self-administered, web-based questionnaire in late February 2004. A clinical case of histoplasmosis was defined as fever plus at least one of the following four symptoms in a plant A worker reported since January 1, 2004: headache, cough, chest pain, or shortness of breath. Workers whose symptoms were consistent with the clinical case definition had histoplasmosis serology testing performed. A laboratory-confirmed case was defined as the presence of a complement fixation (CF) titer >1:32 and/or the presence of an H or M band by immunodiffusion test from a single serum sample obtained from a plant A worker, drawn at least 6 weeks after onset of illness. Controls for the case-control study were randomly selected from workers without any symptoms of histoplasmosis identified during the cohort study. These workers were asked to have a serum sample drawn for histoplasmosis testing and were found to have no serologic evidence of recent Histoplasma capsulatum infection. Of 979 plant workers, 724 (74%) completed the cohort questionnaire; 108 (16%) had symptoms consistent with the clinical case definition. The most commonly reported symptoms were headache (93%), cough (77%), and shortness of breath (44%). No workers were hospitalized. Symptomatic workers (clinical cases) were as likely as asymptomatic workers (nonclinical cases) to report working outside, seeing bird droppings, and performing grounds work. Symptomatic workers were more likely to have worked in building complex X (the complex in closest proximity to the spoil pile) than asymptomatic workers (44 [41%] versus 141 [23%]; risk ratio = 2.0; p<0.001). Building complex X was not located in an area known to be heavily contaminated with bird droppings. Of the 108 symptomatic workers, 90 (83%) had sera available for testing; 25 (28%) had laboratory-confirmed histoplasmosis. Analysis of 22 workers with laboratory-confirmed histoplasmosis with specified dates of symptom onset indicated a cluster of cases during mid-January (Figure). Workers with laboratory-confirmed histoplasmosis were further categorized as clustered cases (n = 18) (symptom onset during January 7--25) and outlying cases (all others, n = four). For the case-control study, the 22 workers with laboratory-confirmed histoplasmosis were compared with 31 unmatched controls. Workers categorized as clustered cases were more likely to have worked in building complex X than controls (12 [67%] versus eight [26%]; odds ratio [OR] = 5.8; 95% confidence interval [CI] = 1.6--20.4); no specific activities, dates reporting to work, or relative amount of outside activity during days of any reported soil disruptions (i.e., December 30, January 2, and January 15) were associated with increased risk for acquiring histoplasmosis. In contrast, workers categorized as outlying cases were as likely to work in building complex X as controls (one [25%] versus eight [26%]; OR = 1.0; p = 1.0); no specific occupation was associated with workers with outlying case status. Reported by: T Safranek, MD, B Beecham, MPH, Nebraska Health and Human Svcs System. B King, MPH, G Burr, National Institute for Occupational Safety and Health; M Lamias, Office of the Director/Office of Informatics; S Fridkin, MD, J Morgan, MD, M Lindsley, ScD, DW Warnock, PhD, Div of Bacterial and Mycotic Diseases, National Center for Infectious Diseases; A Macedo de Oliveira, MD, S Shetty, MD, EIS officers, CDC. Editorial Note:The findings in this report confirm that an outbreak of occupationally acquired histoplasmosis occurred among at least 25 workers from plant A in January 2004. Histoplasmosis usually is an acute, self-limited respiratory illness with an incubation period of 1--2 weeks after inhalation of H. capsulatum spores (1). Previous occupation-related outbreaks of histoplasmosis occurred among workers in a paper factory and courthouse and among bridge workers (2--4), in which disruption of bird or bat droppings, known sources of transmission for H. capsulatum spores, had occurred. As in previous outbreaks, this investigation identified cases clustered in time and location. The majority of patients reported illness onset in mid-January, suggesting a point-source exposure in early January. In addition, workers with laboratory-confirmed infection and onset of illness in mid-January were more likely to work at building complex X than controls, supporting the hypothesis of a common source of exposure. The likely source of this outbreak was the disruption of the spoil pile from the 2003 outbreak. The spoil pile was known to be contaminated with H. capsulatum; the workers closest in proximity to it worked at building complex X, and the timing until symptom onset for workers categorized as clustered cases was consistent with histoplasmosis. However, implication of the spoil pile as the source of the outbreak was surprising for several reasons. First, building complex X was approximately 950 feet from the spoil pile. Second, appropriate precautions were taken during removal of the spoil pile (e.g., limiting the number of workers in the area, using appropriate personal protective equipment [PPE], soaking the spoil pile with water before manipulation, and using both a plastic liner and a tarp to cover the soil once it was transferred to a dumpster). Onset of illness after the mid-January period indicates that some illness might not be associated with the point-source exposure at the plant, but rather might reflect ongoing low-level exposure to H. capsulatum either through other work-related or nonwork-related activities. Further investigation will be necessary to identify all activities placing workers at increased risk for disease. This outbreak underscores the highly infectious nature of H. capsulatum spores and the need to protect workers when engaging in work-related activities involving exposure to H. capsulatum. In particular, these data suggest that manipulation of soil known to be contaminated with H. capsulatum can pose a risk to persons who are not engaged in the activity directly but who might be hundreds of feet away. In addition to following CDC guidelines for the prevention of histoplasmosis among workers (5), the recommendations given to prevent further outbreaks of histoplasmosis at this site included assigning job activities according to three levels of risk: higher, lower, and minimal/no risk. Activities identified as higher risk include those involved in disturbing soil obviously contaminated with bird droppings or in disturbing accumulations of bird droppings. The level of PPE required for these activities includes the use of disposable coveralls such as Tyvek®, rubber boots over normal work shoes, and a respirator providing a higher level of protection, such as a powered air-purifying respirator with high-efficiency particulate air (HEPA) filters or a full-facepiece respirator with HEPA filter. For lower-risk activities (e.g., those disturbing soil that has not been contaminated by bird droppings or during the changing of air filters from buildings or equipment), the level of PPE might be decreased to a NIOSH-certified N-95 filtering facepiece respirator. For activities designated as minimal risk (e.g., those in which no soil or bird droppings are disturbed), no respiratory protection is required, but N-95 filtering facepiece respirators should be available on a voluntary-use basis. References
Figure 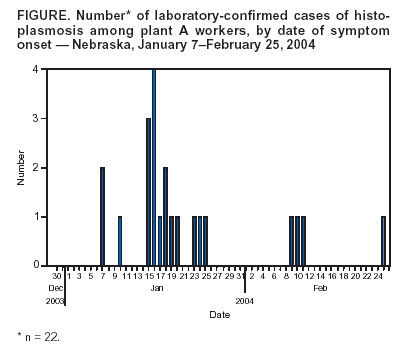 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/4/2004 |
|||||||||
This page last reviewed 11/4/2004
|