 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Racial/Ethnic Trends in Fetal Mortality --- United States, 1990--2000Fetal deaths at >20 weeks' gestation account for 49% of all deaths that occur between the 20th week of pregnancy and the first year of life. Although the risk for fetal death has declined substantially since the 1950s, disparities in the risk for fetal death by race/ethnicity exist (1,2). One of the national health objectives for 2010 is to reduce deaths among fetuses of >20 weeks' gestation to 4.1 deaths per 1,000 live births plus fetal deaths for all racial/ethnic populations (objective no. 16-1a) (3). To assess progress toward meeting this objective, CDC analyzed 1990--2000 data from the National Vital Statistics System (NVSS). The findings indicate substantial reductions in fetal deaths, primarily because of reductions in late fetal deaths (>28 weeks' gestation) compared with early fetal deaths (20--27 weeks' gestation). Despite these reductions, racial/ethnic disparities in fetal deaths persist, particularly among non-Hispanic blacks. Prevention strategies should recognize fetal deaths as a public health problem, improve fetal death surveillance and reporting, target etiologic research, and educate practitioners in identifying women at risk. During 1990--2000, NVSS data included all U.S. fetal deaths that were reported at >20 weeks' gestation. A fetal death was defined as an involuntary loss in which the fetus showed no evidence of life (i.e., no heartbeat or respiration) on delivery. Infant death was defined as the delivery of a live-born infant who subsequently died by age 1 year (4). Perinatal deaths included fetal and infant deaths (i.e., >20 weeks' gestation to age 1 year). The fetal mortality rate (FMR) was calculated as the number of fetal deaths in a specified group per 1,000 live births plus fetal deaths. Fetal deaths with presumed gestation of >20 weeks but with unknown specific gestational ages (2% of all fetal deaths at >20 weeks) were redistributed proportionately to calculate rates for early and late fetal deaths. Race/ethnicity was based on the self-reported race of the mother. Plurality (i.e., the number of fetuses delivered in a pregnancy) was categorized into deaths in singleton and multiple deliveries. All differences in mortality rates (based on Z scores) are statistically significant (p<0.05) unless otherwise noted. In 1990, of 69,737 perinatal deaths reported, 29,345 (42%) were fetal deaths; of these, 12,554 were early fetal deaths, and 16,791 were late fetal deaths. In 2000, of 54,964 perinatal deaths reported, 27,003 (49%) were fetal deaths, including 13,497 early fetal deaths and 13,506 late fetal deaths. A comparison of fetal deaths in 1990 and 2000 by more detailed gestational age groups indicated a shift in the distribution toward deaths at earlier gestational ages (Figure). During 1990--2000, late fetal deaths decreased; however, early fetal deaths at 20--23 weeks increased from 27% to 34%. During 1990--2000, FMR for all pluralities decreased 12%, from 7.5 per 1,000 live births plus fetal deaths to 6.6 (Table 1). However, contrasting trends were observed for early and late FMRs. Early FMRs increased slightly, from 3.2 to 3.3, whereas late FMRs declined 23%, from 4.3 to 3.3. Among singleton deliveries (91% of all fetal deaths in 2000), FMRs decreased 13% overall (early FMR increased slightly, and late FMR decreased 22%). Among multiple deliveries, larger declines were observed; overall FMRs decreased 22% (early and late FMRs decreased 11% and 35%, respectively). Despite improvements in FMRs for multiple deliveries, in 2000, the risk for fetal mortality for multiples was approximately three times that for singletons (FMR =18.5 versus 6.2). Declines in overall fetal mortality were observed for all groups except Asians/Pacific Islanders (A/PIs) (Table 2). FMRs declined 27% for American Indians/Alaska Natives (AI/ANs), 16% for Hispanics, 10% for non-Hispanic whites, and 5% for non-Hispanic blacks. Increases in early fetal mortality were observed for all groups except AI/ANs and A/PIs, whereas decreases in late fetal mortality were observed for all racial/ethnic populations. Total, early, and late FMRs were substantially higher among non-Hispanic blacks in 1990 and 2000 than among other racial/ethnic populations. In 2000, FMR for non-Hispanic blacks was 12.1, compared with a total U.S. FMR of 6.6. The gap between FMRs for non-Hispanic blacks and other racial/ethnic populations remained wide during during 1990--2000; the FMR ratio between non-Hispanic blacks and the U.S. total was 1.7 for 1990 and 1.8 for 2000. Reported by: W Barfield, MD, Div of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion; J Martin, MPH, D Hoyert, PhD, Div of Vital Statistics, National Center for Health Statistics, CDC. Editorial Note:The findings in this report indicate substantial declines in late fetal mortality for all populations (i.e., singleton and multiple deliveries in all racial/ethnic populations) during 1990--2000. The 23% decline observed in late fetal mortality is similar to that reported for neonatal mortality during the same period (2). The findings also indicate that mortality among fetuses delivered at 20--27 weeks' gestation increased slightly during 1990--2000. This finding was consistent for all populations except multiples and AI/ANs. To determine whether the lack of improvement in early fetal mortality was restricted to earlier and less viable gestations, FMRs were calculated separately for fetal deaths at 20--23 and 24--27 weeks. No improvement in FMRs was reported for either group. In contrast, outcomes among live-born infants delivered at 24--27 weeks have improved (5). Trends in the risk for early and late fetal death suggest that changes in perinatal technologies (e.g., fetal imaging, prevention of perinatal infections, effective treatment of maternal medical conditions such as diabetes and chronic hypertension, and more aggressive management of labor and delivery) (6) might have had more of an impact on fetal survival at later rather than earlier gestational ages. In addition, rates of prenatal-care use increased substantially during the 1990s (7), and the subsequent improved access to care also might have had more impact on late rather than early fetal mortality (e.g., through the detection of maternal, fetal, or placental abnormalities that might lead to a live-born delivery). The lack of progress in reducing fetal mortality at earlier gestational ages might be related to 1) poor understanding of the factors associated with premature delivery and 2) limited understanding of the causes of fetal death and the role of maternal, fetal, and placental pathology (8). Racial/ethnic disparities in fetal mortality persist. The risk for early fetal mortality among non-Hispanic blacks was more than double that for other racial/ethnic populations; the risk for late fetal mortality for non-Hispanic blacks was approximately two thirds higher. Despite substantial reductions in late fetal mortality among non-Hispanic blacks during 1990--2000, greater reductions must occur during the next decade if the 2010 national health objective is to be achieved. CDC, in conjunction with state partners, has revised the U.S. Standard Report of Fetal Death and is collaborating with the National Association for Public Health Statistics and Information Systems and the Social Security Administration to improve the quality of fetal death surveillance (4,9). Several states are linking additional data sources (e.g., maternal delivery and hospital records) to fetal death records to enhance understanding of the relationship between maternal disease and fetal death (9). The National Institutes of Child Health and Human Development recently established a national research agenda on stillbirths (fetal deaths at >20 weeks' gestation) (8) and granted awards to five sites to conduct population-based studies of stillbirths. The March of Dimes also has launched a 5-year national prematurity campaign focusing on education and research that includes fetal deaths (10). The findings in this report are subject to at least two limitations. First, fetal deaths might be underreported, particularly at earlier gestational ages. Considerable variability was observed among reporting areas in the quality and completeness of data elements such as Hispanic ethnicity (4). The completeness of reporting of gestational age improved from 93.6% to 96.4% for all records during 1990--2000. Because reporting tends to be less complete at earlier gestational ages (4), the likely impact of this change, if any, would be to increase the number of early fetal deaths. Thus, the increase in early fetal mortality (but not overall mortality) might be less than reported here. Second, live-born infants who died shortly after birth, particularly infants born at early gestational ages or low birthweights, might have been misclassified as fetal deaths. In the United States, the number of fetal deaths nearly equals that of infant deaths during the perinatal period. Mechanisms that contribute to fetal and infant deaths might be related in certain circumstances, but targeting infant deaths is insufficient to appropriately address adverse pregnancy outcomes. Prevention efforts must first acknowledge fetal deaths as a public health problem. Prevention strategies should begin with accurate surveillance and reporting of fetal death to provide researchers with population-based information that provides a better understanding of the factors associated with fetal death. Racial/ethnic disparities also must be addressed in research on fetal deaths, including preconceptional and maternal medical conditions, fetal and placental pathology, and social and environmental factors. These findings can be used by health-care professionals to 1) improve the identification of women at risk for fetal death and 2) educate practitioners on improving the health of women and their infants. References
Table 1  Return to top. Table 2 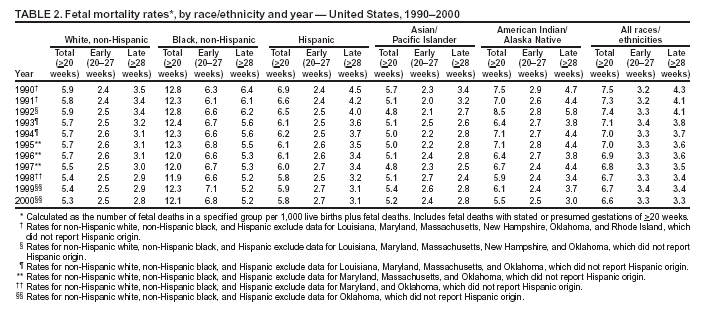 Return to top. Figure 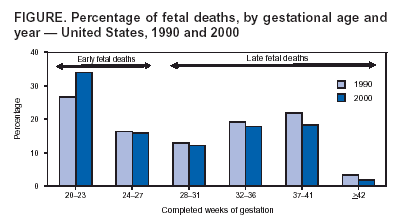 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 6/23/2004 |
|||||||||
This page last reviewed 6/23/2004
|