 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Hepatitis A Outbreak Associated with Green Onions at a Restaurant --- Monaca, Pennsylvania, 2003Please note: The text of this report has been corrected and does not correspond to the official electronic PDF version. An erratum will be published in a subsequent issue. The Pennsylvania Department of Health and CDC are investigating an outbreak of hepatitis A outbreak among patrons of a restaurant (Restaurant A) in Monaca, Pennsylvania. As of November 20, approximately 555 persons with hepatitis A have been identified, including at least 13 Restaurant A food service workers and 75 residents of six other states who dined at Restaurant A. Three persons have died. Preliminary sequence analysis of a 340 nucleotide region of viral RNA obtained from three patrons who had hepatitis A indicated that all three virus sequences were identical. Preliminary analysis of a case-control study implicated green onions as the source of the outbreak. Among 207 persons with hepatitis A who were interviewed and who ate at Restaurant A only once during the 2--6 weeks (i.e., the typical incubation period for hepatitis A) before illness, dates of illness onset were between October 14 and November 12. These 207 patrons reported eating food prepared in Restaurant A during September 14--October 17; a total of 181 (87%) persons reported eating at Restaurant A during October 3--6 (Figure). All infected Restaurant A food service workers became ill after October 26, suggesting that a food service worker could not have been the source of the outbreak. However, during late October--early November, these ill food service workers were working in Restaurant A when they could have been infectious. For this reason, immune globulin has been provided to approximately 9,000 persons who ate food from Restaurant A during this time or had exposures to ill persons involved in the outbreak. The restaurant has been closed. A case-control study was conducted to identify menu item(s) or ingredient(s) associated with illness. A case-patient was defined as a person who had illness onset during October 14--November 12, had laboratory confirmation of acute hepatitis A virus (HAV) infection (i.e., positive IgM anti-HAV), reported eating food prepared at Restaurant A during October 3--6, and had eaten only once at Restaurant A during the 2--6 weeks before illness onset. Controls included persons without hepatitis A who either had dined with case-patients at Restaurant A or were identified through credit card receipts as having dined at Restaurant A during October 3--6. Controls with a previous history of hepatitis A, hepatitis A vaccination, or receipt of immune globulin within 2 weeks after eating Restaurant A food were excluded. Enrolled case-patients and controls were asked about Restaurant A food that they had eaten. The median age of the 181 case-patients in the study was 34 years (range: 4--73 years), and that of the 83 controls was 28 years (range: 2--81, p>0.05). Of 133 menu items, only chili con queso and mild salsa were associated significantly with illness. Mild salsa was eaten by 94% of case-patients, compared with 39% of controls (odds ratio [OR] = 24.2; 95% confidence interval [CI] = 11.4--51.4). Chili con queso was eaten by 15% of case-patients, compared with 3% of controls (OR = 5.2, 95% CI = 1.5--17.8). Both menu items associated with illness contained uncooked or minimally heated fresh green onions. Among 11 case-patients who reported not eating mild salsa, seven ate at least one of the other 52 menu items that contained green onions. Of 103 ingredients used at the restaurant, 12 were associated with illness in a univariate analysis. Of these, 10 had been consumed by <50% of case-patients. Eating a menu item containing green onions was reported by 98% of case-patients, compared with 69% of controls (OR = 20.2, 95%CI = 6.8--59.9). Eating a menu item containing white onions also was associated with illness. However, among the 176 case-patients who reported eating white onions, 174 (99%) also ate green onions. Among the four case-patients and 28 controls who reported not eating green onions, white onions were not associated with illness (OR = 2.5, 95% 0.3--20.9). During interviews conducted at Restaurant A, food service workers described green onion storage, washing, and preparation practices. Green onions were shipped in 8.5-lb. boxes containing multiple small bundles (6--8 green onions per bundle). Each box was unpacked, and bundles were stored upright (root side down) and refrigerated in a bucket with ice included in the shipment. Green onions were stored ≤5 days before processing, which consisted of rinsing intact onion bundles, cutting the roots off, and removing the rubber bands. Green onions from each box were chopped by machine to yield approximately 8 qts. Chopped green onions were refrigerated for approximately 2 days. Periodically (i.e., every 1--3 days), salsas were prepared in batches of 40--80 qts. Mild salsa included chopped fresh green onions; hot salsa did not. Salsas were refrigerated in 8-quart containers with a shelf life of 3 days. Mild and hot salsa were ladled into bowls and provided free with tortilla chips upon seating at Restaurant A. The Food and Drug Administration (FDA), CDC, and the state health departments are investigating the source of the green onions associated with this outbreak and how they became contaminated with HAV. Preliminary traceback information indicates that green onions supplied to Restaurant A were grown in Mexico. Reported by: V Dato, MD, A Weltman, MD, K Waller, MD, Bur of Epidemiology, Pennsylvania Dept of Health. MA Ruta, Ohio Dept of Health. U.S. Food and Drug Administration. Div of Viral Hepatitis, National Center for Infectious Diseases; A Highbaugh-Battle, C Hembree, S Evenson, Epidemiology Program Office; C Wheeler, MD, T Vogt, PhD, EIS officers, CDC. Editorial Note:This report describes a large hepatitis A outbreak associated with eating a food item containing green onions at a single restaurant. The majority of ill patrons interviewed as of November 21 were exposed during a 3-day period in early October. No ill food service worker identified could have been the source of the outbreak. The green onions likely were contaminated with HAV in the distribution system or during growing, harvest, packing, or cooling. Traceback investigations completed to date have determined that the green onion source is one or more farms in Mexico. Both green onions and white onions were associated with illness in the univariate analysis. However, white onions were not associated with illness among those who did not eat green onions. This association with white onions observed in the univariate analysis might not remain when multivariate modeling is completed. Restaurant A purchases previously chopped white onions and adds them to several menu items, including hot and mild salsa. Mild salsa, which contains both green onions and white onions, was associated with illness; however, hot salsa, which contains only white onions, was not associated with illness. The genetic sequence of the outbreak strain is very similar to viral sequences obtained from persons involved in hepatitis A outbreaks in Tennessee, Georgia, and North Carolina during September 2003 that were linked epidemiologically to green onions. These sequences also were identical or very similar to sequences observed among persons with hepatitis A living along the United States-Mexico border and travelers returning from Mexico, consistent with a source in Mexico (CDC, unpublished data, 2003). Raw green onions from three firms in Mexico have been implicated in the Tennessee and Georgia outbreaks. FDA is still reviewing records to determine if additional firms are involved. The Mexican government is assisting with the traceback investigation in Mexico and the investigation to determine the source of the contamination. Previous hepatitis A outbreaks linked to green onions have been reported and have involved patrons of a single restaurant (1). However, the outbreak at Restaurant A was unusually large. Several characteristics of the way food was prepared and served in Restaurant A could have contributed to the outbreak's size, including 1) multiple opportunities for intermingling of uncontaminated and contaminated green onions in a common bucket for 5 days with the ice in which they were shipped and 2) serving contaminated items with a relatively long shelf life (e.g., mild salsa) to a large proportion of patrons over several days. HAV is transmitted by the fecal-oral route. Green onions require extensive handling during harvesting and preparation for packing. Contamination of green onions could occur 1) by contact with HAV-infected workers, especially children, working in the field during harvesting and preparation and 2) by contact with HAV-contaminated water during irrigation, rinsing, processing, cooling, and icing of the product. Green onions and other selected produce items (e.g., strawberries [2]) might be more vulnerable to contamination because plant surfaces are particularly complex or adherent to viral or fecal particles. Outbreaks of other enteric pathogens linked to green onions have been reported (3). On November 15, FDA issued an alert to consumers about the recent hepatitis A outbreaks associated with green onions (available at http://www.fda.gov/bbs/topics/ANSWERS/2003/ANS01262.html). FDA advised consumers concerned about the possibility of getting hepatitis A from green onions to cook green onions thoroughly before eating and to ask about use of green onions in prepared foods. Unless directed otherwise by public health officials, persons who have recently eaten green onions do not need postexposure prophylaxis (i.e., immune globulin). CDC is working with state health departments to identify other hepatitis A outbreaks associated with green onions. As of November 21, no other hepatitis A outbreaks have been identified. To identify other cases related to these outbreaks, state and local health officials should interview persons with hepatitis A with onset after October 1. Persons without typical risk factors for hepatitis A (4) should be asked about food and restaurant exposures during their incubation period. Because molecular epidemiologic techniques have been useful for identifying related cases of foodborne hepatitis A in previous outbreaks (2), health departments might consider obtaining serum specimens for cases of interest. An increasing proportion of reported foodborne outbreaks have been linked to fresh produce (3). This increase might be attributed to increased consumption of fresh produce or better surveillance techniques. HAV contamination of fresh produce can be reduced by using approaches such as the application of Good Agricultural Practices/Good Manufacturing Practices recommended by FDA (5) Recommended control measures include providing sanitary facilities for field workers, ensuring appropriate water quality, use of properly treated manure or biosolids, and ensuring worker health. Reducing HAV transmission in areas where produce is grown and discouraging the presence of children in areas where food is harvested also will reduce opportunities for HAV contamination. Further investigation of this and other hepatitis A outbreaks linked to green onions, including observation of cultivation and harvesting practices, can guide additional specific critical control measures. References
Figure 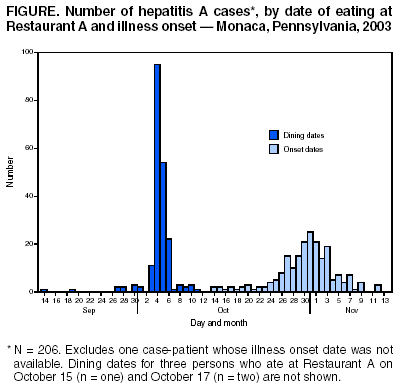 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/21/2003 |
|||||||||
This page last reviewed 11/21/2003
|