 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Invasive Streptococcus pyogenes After Allograft Implantation --- Colorado, 2003Allograft tissues are used for various orthopedic procedures (e.g., ligament reconstruction, meniscal transplantation, and spinal surgery). In 2002, approximately one million allografts were distributed for transplantation (American Association of Tissue Banks [AATB], unpublished data, 2002). Recent reports of allograft-associated infections have prompted evaluation of the processing and quality-control methods employed by tissue processors (1,2). This report describes a case of invasive disease with Streptococcus pyogenes (i.e., group A streptococcus [GAS]), after reconstructive knee surgery using contaminated allograft tissue and provides recommendations to reduce the risk for allograft-associated infections. Although allograft infections are rare, they highlight the need for improved tissue evaluation and processing standards. In September 2003, a previously healthy male aged 17 years underwent elective anterior cruciate ligament repair with a hemi-patellar tendon allograft at an ambulatory surgical center in Colorado. Six days after the procedure, he was admitted to a local hospital with pain and erythema at the incision site, fever of 102° F (39° C), and chills. The allograft tissue was removed, and the patient underwent surgical exploration and fasciotomy of the affected thigh. Cultures of his blood, wound aspirate, and explanted tissue grew GAS. His hospital course required a stay in the intensive care unit and was complicated by persistent fever and fluid collection in the affected leg, which was managed with computerized tomography--guided needle aspiration. After 7 days of treatment with clindamycin and cefazolin, the wound aspirate again yielded GAS. The patient was discharged after 17 days and completed a course of intravenous antibiotics at home; he was later readmitted to the hospital for related complications and discharged subsequently. The allograft received by the patient came from a cadaveric donor (Figure) and was supplied by tissue processor A (TP-A). After the patient's surgeon alerted TP-A to this case of presumptive allograft infection, TP-A contacted the Food and Drug Administration (FDA). Tendon allografts from the donor had been implanted in five other patients; as of December 1, no adverse outcomes had been detected by their surgeons. All remaining allografts recovered from the donor and processed by TP-A were placed on hold or recalled. According to medical examiner's records, the donor had undergone cervical spinal fusion 3 weeks before his death; autopsy findings included a generalized rash and potentially toxic levels of a muscle relaxant and an analgesic medication. On autopsy, the cause of death was attributed to the toxic effects of these drugs. Cultures of the donor's tissues, obtained by the tissue recovery organization before distribution to two tissue processors, yielded GAS. Preprocessing cultures obtained by TP-A also yielded GAS. TP-A processed the allografts using aseptic technique and an antimicrobial solution, but no sterilization procedure (e.g., gamma irradiation) was used. After the recovered tissues were processed, all postprocessing cultures were reported as negative to TP-A, and these allografts were distributed. Other tissues recovered from the donor were distributed to a second tissue processor (TP-B) and were held for further review. CDC, FDA, and the Colorado Department of Public Health and Environment conducted an investigation to determine whether the allograft had been the source of GAS infection in the recipient. TP-B provided CDC with donor tissues that had not undergone antimicrobial processing; GAS was identified in a specimen of fascia lata. GAS also was isolated from a specimen of the donor's blood, which had been stored by TP-A. Emm typing of the isolates was performed at CDC to sequence the variable region of the emm gene of GAS (3). Sequence analysis confirmed that blood and tissue isolates from both donor and recipient were a newly discovered subtype emm3.17 that had not been identified among 108 invasive emm3 isolates characterized recently (4) or among 155 emm3 isolates recovered from children with pharyngitis (CDC, unpublished data, 2003). During the investigation, TP-A suspended distribution of all orthopedic allografts containing bone, such as the tissue implanted in the recipient. Reported by: J Bos, MPH, JM Crutcher, MD, Oklahoma State Dept of Health. K Gershman MD, Colorado Dept of Public Health and Environment. T Coté, MD, MA Greenwald, MD, J Polder, MPH, Center for Biologics Evaluation and Research, U.S. Food and Drug Administration. A Srinivasan, MD, M Arduino, DrPH, DB Jernigan, MD, Div of Healthcare Quality Promotion; B Beall, PhD, JA Elliott PhD, RR Facklam, PhD, A Schuchat, MD, C Van Beneden, Div of Bacterial and Mycotic Diseases; Div of Viral and Rickettsial Diseases, National Center for Infectious Diseases; E Lee, MD, D Ferguson, MD, EIS officers, CDC. Editorial Note:This report describes a case of invasive GAS infection associated with a contaminated musculoskeletal allograft. The uncommon strain of GAS detected in the donor's blood and tissues before processing was indistinguishable from the strain isolated from the recipient after implantation. The implicated allograft tissue had been subjected to antimicrobial treatment and postprocessing cultures before release by TP-A. GAS has not been reported previously in association with allograft infections. Although invasive disease caused by GAS is associated most commonly with skin and other soft tissue infections (5), GAS accounted for <0.4% of all surgical-site infections annually during 1998--2002 (CDC, unpublished data, 2003). During 2000--2002, approximately 350--400 annual cases of invasive GAS were classified as postsurgical (i.e., occurring during the first 7 days after surgery), representing approximately 4.0% of invasive GAS infections reported for those years (CDC, unpublished data, 2003). Among tissue donors, data suggest the prevalence of GAS in preprocessing cultures of blood and musculoskeletal tissues is low, with a range of 0.2%--0.4% (O. Martinez, Ph.D., University of Miami Tissue Bank, and S. Brubaker, LifeNet, personal communications, 2003). GAS was detected in preprocessing cultures of all tissues recovered from the donor. These results did not prompt TP-A to reject the tissues, because all postprocessing cultures were negative. Previous reports of allograft-associated infections have highlighted several problems with aseptic tissue processing and culturing methods used to detect bacterial contamination after processing (1,2). In one case, antimicrobial treatment did not eradicate Clostridium sordellii, and postprocessing cultures failed to detect the contamination with C. sordellii, resulting in the death of a recipient of a bone-cartilage allograft (2). Although sterilization methods can further reduce the risk for contaminated allografts, tissues processed with the most common method (e.g., irradiation) have been associated with altered biomechanics. As a result, sterilization methods are not used routinely by soft-tissue processors (6). This investigation implicated contaminated allograft tissue in the transmission of GAS. Given the apparent ability of the organism to endure tissue processing with antimicrobial treatment, the presence of GAS in donor tissue should prompt rejection of the tissue unless a sterilizing procedure can be used. Because GAS prevalence among donor cultures is low, this recommendation should not limit the supply of tissue available for transplantation substantially. AATB, a voluntary accreditation organization, has proposed sterilizing or discarding certain tissues if specified organisms, including GAS, are detected (S. Brubaker, AATB, personal communication, 2003). Tissue processors should adopt processes to ensure tissue safety. If tissue is contaminated with GAS or other pathogenic, highly virulent organisms, standard protocols for sterilization should be employed by tissue processors when possible, or the tissue should be discarded. When applicable, tissue processors should validate methods used to obtain culture specimens after antimicrobial treatment or sterilization. AATB standards require rejection of donor tissues with evidence of active infection at the time of donation, including septicemia (7). Assessment of infection also should occur during tissue processing. Typically, evidence of systemic infection in prospective donors is detected before tissue recovery (8). However, when systemic infection is not detected before tissue recovery, donor eligibility should be reconsidered if cultures of multiple allograft tissues from the same donor yield the same organism. Multiple positive cultures for the same organism, even those not specified as highly virulent by AATB, might indicate systemic disease and should be considered in the comprehensive evaluation of the donor. CDC guidelines for prevention of GAS disease identify the occurrence of postsurgical infection with GAS as a sentinel event that should prompt an epidemiologic investigation and enhanced surveillance within the hospital (9). Certain postsurgical GAS infections reflect transmission from asymptomatic, colonized health-care workers who should be identified to prevent additional postsurgical infections. Contaminated allografts should be considered as potential sources of GAS when postsurgical infections are recognized. Early signs of infection with GAS are nonspecific and might include localized pain, swelling, or erythema. Pain associated with invasive GAS infections often is disproportionate to clinical findings. Diagnostic evaluation should include anaerobic and aerobic cultures of blood and other specimens (2). Clinicians should be aware of the possibility of allograft-associated infections in the postoperative setting and should report these infections to the tissue processor and local health department. State health departments, CDC, and FDA should be notified to assist with investigations. Data about invasive GAS are available through CDC's Active Bacterial Surveillance system http://www.cdc.gov/ncidod/dbmd/abcs/survreports.htm. Additional information about surveillance for surgical-site infections is available through CDC's National Nosocomial Infections Surveillance System at http://www.cdc.gov/ncidod/hip/surveill/nnis.htm. Acknowledgments This report is based on contributions by MA Kainer, MD, Tennessee Dept of Health. PR Rigney, American Association of Tissue Banks (AATB), McLean; S Brubaker, AATB and LifeNet, Virginia Beach, Virginia. M Elledge, American Red Cross Transplantation Svcs, Washington, DC. OV Martinez, PhD, Univ of Miami Tissue Bank, Miami, Florida. References
Figure 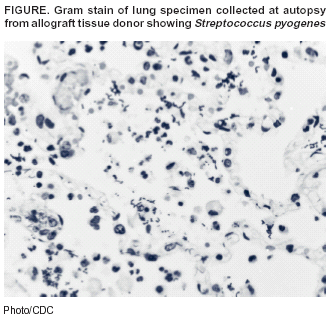 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 12/4/2003 |
|||||||||
This page last reviewed 12/4/2003
|