 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Receipt of Cardiac Rehabilitation Services Among Heart Attack Survivors --- 19 States and the District of Columbia, 2001Each year, approximately 650,000 persons have a first heart attack in the United States. Heart attack survivors are at increased risk for recurrent heart attacks, cardiovascular complications, and sudden cardiac death (1). A major component of risk-reduction strategies for these patients is cardiac rehabilitation consisting of nutritional counseling; management of lipid levels, hypertension, weight, and diabetes; smoking cessation; psychosocial interventions; and physical activity counseling and exercise training (2). Although cardiac rehabilitation has been associated with substantially improved survival rates (3), the majority of eligible patients do not participate in cardiac rehabilitation (4). This report summarizes data from the Behavioral Risk Factor Surveillance System (BRFSS) on the prevalence of self-reported participation in cardiac rehabilitation services among persons in 19 states* and the District of Columbia (DC) who have had a heart attack. The findings indicate that less than one third of these respondents have participated in cardiac rehabilitation. Including cardiac rehabilitation in all intervention plans for eligible patients with coronary heart disease remains a key strategy for reducing further disability. BRFSS is a state-based, random-digit--dialed telephone survey of the noninstitutionalized U.S. civilian population aged >18 years. In 2001, a total of 65,253 persons in 19 states and DC responded to questions about history of heart attack and receipt of cardiac rehabilitation services after a heart attack (median response rate: 52%). Surveyed participants were asked, "Were you ever told by a doctor that you had a heart attack or myocardial infarction?" Those who answered "yes" also were asked, "After you left the hospital following your heart attack, did you go to any kind of outpatient rehabilitation? This is sometimes called `cardiac rehab.'" Other data collected by BRFSS included sex, age, race/ethnicity, education, cardiovascular disease risk factors, and state of residence. Data were weighted according to state population estimates. Estimates and standard errors were calculated by using SUDAAN to account for the complex sampling design. To ensure stability, estimates were not calculated if cell sizes were <50. Chi square analyses were used to test overall differences in unadjusted estimates by sex, race/ethnicity, age, and education level. Logistic regression analysis was used to examine the odds of risk factors and preventive actions by receipt of rehabilitation, adjusted for sex, age, and education level. Approximately 4% of surveyed respondents reported having ever had a heart attack (Table 1). This percentage increased with age, was higher among men than women, varied among racial/ethnic groups, and was highest among those with less education. The percentage of respondents who reported having had a heart attack ranged from 2.9% in Utah to 6.4% in West Virginia. Overall, 29.5% of persons having had a heart attack reported having received cardiac rehabilitation services (Table 1). Men were more likely than women to report having received cardiac rehabilitation, as were persons aged 50--64 years compared with other age groups and those with more education compared with those with less. Numbers were too small for reliable estimates by race/ethnicity and state. Persons who received cardiac rehabilitation were more likely than those who did not receive cardiac rehabilitation to report having high blood cholesterol levels (p<0.01); other reported risk factors (e.g., self-reported high blood pressure, diabetes, overweight, and smoking) and perceived health status did not differ significantly between the two groups (Table 2). Persons who received cardiac rehabilitation were more likely than those who did not receive such services to report engaging in physical activity during the 30 days preceding the survey (p<0.05) and to report having been counseled to reduce dietary fat and cholesterol intake (p<0.05), increase fruit and vegetable intake (p<0.01), and increase exercise (p<0.01). Persons who received cardiac rehabilitation were significantly more likely than those who did not receive cardiac rehabilitation to report exercising more (p<0.05). The majority of persons with a heart attack reported taking aspirin regularly; however, the prevalence of aspirin use was greater among those receiving cardiac rehabilitation services. After adjustments for sex, age, and education, persons receiving cardiac rehabilitation were more likely than persons not receiving these services to report 1) having been diagnosed with high blood cholesterol (odds ratio [OR] = 1.4; 95% confidence interval [CI] = 1.1--1.9; p = 0.02); 2) having been told to eat fewer high-fat/high-cholesterol foods (OR = 1.4; 95% CI = 1.1--1.9; p = 0.02), to eat more fruits and vegetables (OR = 1.74; 95% CI = 1.3--2.3; p = 0.0002), and to exercise more (OR = 1.6; 95% CI = 1.2--2.2; p = 0.001); and 3) taking aspirin regularly (OR = 2.2; 95% CI = 1.3--3.2; p = 0.004). Reported by: C Ayala, PhD, D Orenstein, PhD, KJ Greenlund, PhD, JB Croft, LJ Neff, PhD, GA Mensah, MD, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:Cardiac rehabilitation is safe and beneficial when patients are evaluated and screened properly for these services (2,3) and has been shown to reduce recurrence of subsequent heart attacks and co-morbidities (2). However, consistent with previous studies (3,4), the findings in this report indicate that less than one third of respondents who have had a heart attack participated in cardiac rehabilitation. Contraindications for cardiac rehabilitation include unstable angina, serious arrhythmias, congestive heart failure, previous cardiac arrest during exercise, extremely low activity level, and very high risk (5). Increased adherence to guidelines for assessment of patient eligibility is needed for appropriate referral. In addition, sufficient time and personnel are needed for counseling of post--heart attack patients about lifestyle modifications that might reduce risk factors (5--7). Persons who cannot participate in cardiac rehabilitation because of physical limitations need periodic evaluation with continued counseling to help reduce recurrent heart problems and improve quality of life (5). The findings in this report are subject to at least three limitations. First, because the study was limited to residents of 19 states and DC who had a heart attack and did not reside in long-term--care facilities, the findings might not be representative of the U.S. population. Second, because the severity of a respondent's disability after a heart attack was not ascertained, observed differences might be attributed to differences in disease severity. Finally, because self-reported health data are dependent on factors such as respondents' awareness of their conditions, recall bias, and the social desirability of certain responses, the findings might be biased. The benefits of cardiac rehabilitation include greater exercise tolerance, fewer cardiac symptoms, lower blood fat levels, cessation of smoking, improved psychosocial well-being, and reduced risk for illness and death. To help patients obtain these benefits, public health efforts should encourage policies that result in increased insurance coverage for cardiac rehabilitation services. In addition, adherence to assessment and treatment guidelines might be enhanced by 1) updated guidelines for physicians, 2) updated assessment of patients to help in tracking participation, 3) a reminder system to improve compliance, and 4) appropriate education and counseling for patients in cardiac rehabilitation. Further research is needed to identify factors that improve participation and adherence to lifestyle modifications prescribed in cardiac rehabilitation. References
* Alabama, Arkansas, Colorado, Iowa, Minnesota, Mississippi, Missouri, Montana, New York, North Dakota, Ohio, Oklahoma, South Carolina, Tennessee, Utah, Virginia, Washington, West Virginia, and Wyoming.
Table 1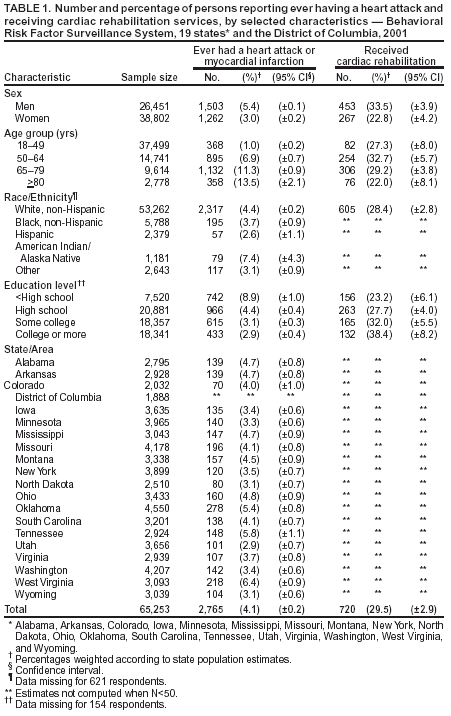 Return to top. Table 2 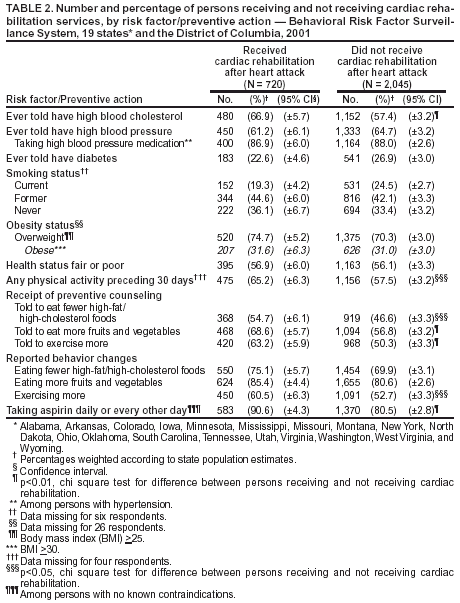 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/6/2003 |
|||||||||
This page last reviewed 11/6/2003
|