 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Foodborne Transmission of Hepatitis A --- Massachusetts, 2001Hepatitis A virus (HAV) is transmitted typically from person to person by the fecal-oral route. Foodborne
transmission occurs when an HAV-infected food handler contaminates food during preparation
(1--3) or when food is contaminated during harvesting or processing before reaching the food service establishment or home
(4,5). Postexposure prophylaxis (PEP) with immune globulin (IG) can prevent hepatitis A among exposed persons if administered within 14 days of exposure. On October 26, 2001, the Massachusetts Department of Public Health (MDPH) was notified that a worker at restaurant A in county X had hepatitis A with symptom onset on October 17. On the basis of the date of symptom onset, the worker was considered to have been potentially infectious during October 3--24. The worker's primary responsibility was managerial, but the worker also prepared menu items (primarily sandwiches that were not cooked after preparation) as needed and had worked most recently on October 18. During an interview, the worker reported frequent hand washing and diligent glove use while handling food; supervisors validated the worker's hygiene practices. On the basis of the worker's reported hygiene practices, work duties, and lack of gastrointestinal symptoms, health officials considered HAV contamination of food prepared by this food handler unlikely and did not issue a public notification or recommend PEP for restaurant patrons. The worker denied any change in bowel habits; however, assessment was difficult because the worker had a colostomy and normally produced unformed stool that collected in an ostomy appliance. The worker reported that the appliance was secured under several layers of clothing and was never changed at work. On October 26, the restaurant's owners closed and cleaned the restaurant voluntarily. On October 27, an inspection by MDPH found no sanitary code violations. None of the 20 food handlers at the restaurant had symptoms of hepatitis A, although none was tested serologically for evidence of recent HAV infection. The restaurant reopened after 19 food handlers received IG and one was excluded from work. On November 20, MDPH was notified of six cases of hepatitis A among residents of county X, all with illness onsets during November 8--15. By December 3, a total of 46 persons had been reported in county X, with illness onsets during October 29--November 26 (Figure), compared with no cases during the same period in 2000. The median age of patients was 38 years (range: 5--76 years); 31 (67%) were males. Of the patients who could recall where they had eaten during their hepatitis A incubation period (2--6 weeks before illness onset), 35 (76%) of 46 reported eating at restaurant A, 15 (35%) of 43 at restaurant B, 16 (35%) of 46 at restaurant C, and nine (20%) of 45 at restaurant D. Eating at other restaurants was reported less frequently. A matched case-control study was conducted to determine whether persons with hepatitis A were more likely than neighborhood controls to have eaten at one of the four restaurants. A case-patient was defined as a resident of county X who had illness onset during October 18--November 29 and had laboratory confirmation of HAV infection (positive IgM anti-HAV). Potential controls were identified by using a web-based neighbor search, matched by age group (2--13 years, 14--22 years, 23--40 years, 41--54 years, and >55 years) and interviewed by telephone. Potential controls who reported previous hepatitis A vaccination, possible hepatitis A illness during October 18--November 29, or a history of physician-diagnosed hepatitis A were excluded from participation. One neighborhood control was recruited for each of 43 (93%) case-patients; no neighborhood control was found for the remaining three case-patients. Controls were asked about eating food from restaurants from October 1 (4 weeks before the earliest illness onset of any case-patient) to November 12 (2 weeks before the latest illness onset of any case-patient). An exact conditional logistic regression model was used to determine the relation between restaurant patronage and illness; illness was associated with eating food from restaurant A (odds ratio = 29.4; 95% confidence interval = 5.1--infinity) but not food from restaurants B, C, or D. A total of 32 (74%) of the 43 case-patients and seven (16%) of neighborhood controls reported having eaten food from restaurant A. An epidemiologic study to determine whether any specific foods served at restaurant A were associated with illness was not performed. Sequence analysis of a segment of HAV RNA isolated from 28 case-patients was performed by using a reverse transcriptase-polymerase chain reaction method (6). A total of 25 sequences were identical, including all 21 from case-patients who reported eating food prepared at restaurant A. The remaining four patients reported not eating food from restaurant A during their incubation period. Three additional persons who did not eat at restaurant A had nonidentical viral RNA sequences. Two case-patients were food handlers at restaurant Z, also in Massachusetts. Each had worked at restaurant Z when they were potentially infectious and prepared foods that were not cooked after handling. On November 27, after interviewing food handlers and inspecting restaurant Z, local health officials issued a public notice offering IG to customers who ate uncooked or cold food prepared at restaurant Z during November 14--23. Approximately 1,600 persons responded to the public notice and were administered IG at a clinic held at a local hospital. Reported by: T LaPorte, MS, D Heisey-Grove, MPH, P Kludt, MPH, BT Matyas, MD, A DeMaria, Jr, MD, Bur of Communicable Disease Control, Massachusetts Dept of Public Health. R Dicker, MD, A De, PhD, Div of Applied Public Health Training, Epidemiology Program Office; A Fiore, MD, O Nainan, PhD, Div of Viral Hepatitis, National Center for Infectious Diseases; DS Friedman, PhD, EIS Officer, CDC. Editorial Note:The probable source of the hepatitis A outbreak described in this report was a food handler in restaurant A who worked while infectious and contaminated food that was not cooked subsequently. Although the food handler with hepatitis A was the probable source, transmission from another food handler in restaurant A with unidentified or unreported HAV infection cannot be excluded. This outbreak investigation highlights difficulties faced by public health officials when making hepatitis A PEP decisions. In this investigation, determining the risk for transmission to patrons from the implicated food handler, who handled uncooked foods while potentially infectious, was based on an assessment of self-reported activities such as gastrointestinal symptoms, personal hygiene, and glove use. The factors that led to transmission despite reportedly good hygiene cannot be determined. During 1992--2001, approximately 230,000 cases of hepatitis A were reported in the United States (7). Although food handlers are not at higher risk for HAV infection because of their occupation, approximately 8% of adults reported with hepatitis A are identified annually as food handlers (CDC, unpublished data, 2003), indicating that thousands of food handlers have hepatitis A each year. Unlike the majority of persons with hepatitis A who transmit HAV only to close contacts, an HAV-infected food handler potentially can transmit HAV to many others and cause a substantial economic burden to public health. The estimated societal cost of a single foodborne outbreak of hepatitis A involving 43 cases was approximately $800,000; >90% of these costs were incurred by the public health department (8). Considerable effort is involved in determining the risk for transmission from an HAV-infected food handler to customers. An interview that includes detailed questions about job duties, work dates, clinical symptoms, and hygiene is the basis for determining the need for PEP. CDC guidelines recommend that PEP can be considered if 1) during the time when the food handler was probably infectious, the food handler both directly handled uncooked foods or foods after cooking and had diarrhea or poor hygiene practices; and 2) patrons can be identified and treated within 2 weeks after the exposure (9). However, because good personal hygiene is subjective and difficult to corroborate or might not prevent disease transmission completely, a food handler's report of good hygiene should not be the only criterion for determining whether patron notification and PEP are needed. Other factors that might affect personal hygiene and the potential for HAV transmission should be examined, including the presence of underlying medical conditions. For the outbreak described in this report, the worker's ostomy might have compromised hygiene. HAV transmission from a food handler with a colostomy has been identified previously (D. Perrotta, Ph.D., Texas Department of Health, personal communication, 2003). A better understanding is needed regarding hygiene practices, clinical symptoms, and viral characteristics that contribute to HAV transmission by contaminated food. However, prevention measures that can reduce the risk for transmission of HAV and other enteric pathogens also should be emphasized, including regular and thorough hand washing, reducing bare-hand contact with foods that are not cooked subsequently, restricting ill food handlers from working directly with food or food equipment, and providing a sick leave policy so workers can discontinue working while ill (10). Hepatitis A vaccination should be encouraged for persons who are both recommended for routine vaccination (i.e., men who have sex with men, illicit-drug users, and persons who plan travel to countries in which hepatitis A is endemic) and are employed as food handlers. The factors that led to HAV transmission in this outbreak cannot be determined. Until the determinants of HAV transmission through contaminated food are understood better, decisions about providing PEP to customers of food service establishments will continue to be based on data obtained during case interviews and on the judgment and experience of public health officials. Food handlers acquire HAV infection from others within their communities, and reducing food handler transmission of HAV will be achieved ultimately through routine vaccination of persons at risk for HAV infection within these communities. References
Figure 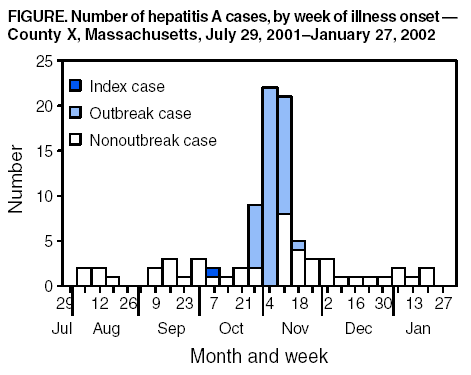 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 6/19/2003 |
|||||||||
This page last reviewed 6/19/2003
|