 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Populations Receiving Optimally Fluoridated Public Drinking Water --- United States, 2000Dental caries (i.e., tooth decay) is a transmissible, multi-factor disease that affects 50% of children aged 5--9 years, 67% of adolescents aged 12--17 years (1), and 94% of adults aged >18 years (2) in the United States. During the second half of the 20th century (3), a major decline in the prevalence and severity of dental caries resulted from the identification of fluoride as an effective method of preventing caries. Fluoridation of the public water supply is the most equitable, cost-effective, and cost-saving method of delivering fluoride to the community (4,5). In the United States during 2000, approximately 162 million persons (65.8% of the population served by public water systems) received optimally fluoridated water compared with 144 million (62.1%) in 1992 (6). This report presents state-specific data on the status of water fluoridation in the United States and describes a new surveillance system designed to routinely produce state and national data to monitor fluoridation in the public water supply. The results of this report indicate slow progress toward increasing access to optimally fluoridated water for persons using public water systems. Data from the new surveillance system can heighten public awareness of this effective caries prevention measure and can be used to identify areas where additional health promotion efforts are needed. The 2000 and 2010 national health goals include objectives (13.9 and 21.9, respectively) (7,8) to increase the 1989 and 1992 national baseline fluoridation levels (61% and 62%, respectively) (6,9) to 75% of the U.S. population served by community water systems that receive water with optimal levels of fluoride (0.7--1.2 ppm depending on the average maximum daily air temperature of the area). The U.S. Environmental Protection Agency (EPA) does not regulate the addition of fluoride to water, and EPA's Safe Drinking Water Information System (SDWIS) actively tracks fluoride concentrations only in water systems with naturally occurring fluoride levels above the established regulatory limits (>2.0 ppm). During 1998--2000, CDC developed the Water Fluoridation Reporting System (WFRS), a surveillance database that included CDC's 1992 water fluoridation census (6) and EPA's SDWIS. To ensure that initial data were accurate and complete, in 2000, CDC sent state-specific reports generated from WFRS to the oral health contact at each state health agency for review; updated information was returned, and nonrespondents were contacted through telephone calls and electronic messages. In July 2001, each state received its preliminary public water system data and was asked to submit corrections. Alabama, California, Kansas, Louisiana, Montana, Rhode Island, Texas, and Wyoming had not updated their data by September 1, 2001; therefore, existing WFRS data were used in this report. Fluoridation percentages were determined by dividing the number of persons using public water systems with fluoride levels considered optimal (naturally occurring and adjusted) for the state by the total population of the state served by public water systems. When the population served by public water systems exceeded the 2000 population census for that state, the state census was used as the population using the public water supplies. This might occur as a result of the methods used by water systems to estimate the population served. These states were Alabama, Hawaii, Louisiana, Massachusetts, Missouri, Utah, and Wyoming. In the United States during 2000, approximately 162 million persons (65.8% of the population served by public water systems) received optimally fluoridated water compared with 144 million (62.1%) in 1992 (6); state-specific percentages (Table 1) ranged from 2% (Utah) to 100% (District of Columbia) (median: 76.7%). In 27 states during 1992--2000, the proportion increased (range: 0.8%--63.8% [Georgia and Nevada, respectively]; median: 4.9%), and in 23 states, the proportion decreased (range: from --0.1% to --6.0% [Iowa and Alaska, respectively]; median: 2.9%); the District of Columbia remained 100% fluoridated. Delaware, Maine, Missouri, Nebraska, and Virginia reached 75% in 2000 and Oklahoma reached 74.6%. The national objective has been met by 26 states, and the small increase from 1992 to 2000 of 3.7 percentage points has left a gap of 9.2 percentage points from the overall target. Reported by: D Apanian, MS, D Malvitz, DrPH, S Presson, DDS, Div of Oral Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:WFRS data indicate that during the 1990s, the estimated proportion of the U.S. population using public water supplies that maintained optimally fluoridated water increased from 62.1% to 65.8%. This modest progress occurred as the result of substantial increases in coverage in a few states and, in some instances, because several large metropolitan areas commenced fluoridation (e.g., Clark County [Las Vegas], Nevada; Los Angeles and Sacramento, California; and Manchester, New Hampshire). The findings in this report are subject to at least three limitations. First, nonresponses might have affected the accuracy of some states' final water fluoridation percentages by not accounting for changes in status. Second, use of the 2000 U.S. census data as the denominator for calculating water fluoridation percentages in seven states might have resulted in the percentages being underestimated because, in most states, the number of persons using public water systems was probably less than the 2000 U.S. census population. Finally, three states (Kentucky, Rhode Island, and South Dakota) reported their 1992 fluoridation rates as 100%; in these states, the apparent decrease from 1992 to 2000 in the percentage of persons using public water supplies receiving optimally fluoridated water represents an error correction in reporting methods rather than a true decrease. WFRS will become an increasingly valuable tool for monitoring state and annually updating national water fluoridation data as more users register and routinely participate in entering data and receiving reports. WFRS updates and reports will assist states in monitoring the extent and consistency of water fluoridation. During 2002, CDC will provide online information on water fluoridation for states that update their data electronically. Although the new WFRS online site might facilitate public knowledge about optimally fluoridated water, efforts to convince jurisdictions to provide such water must address 1) the perception by some scientists, policymakers, and members of the public that dental caries is no longer a public health problem or that fluoridation is no longer necessary or effective; 2) the often complex political process involved in adopting water fluoridation; and 3) unsubstantiated claims by opponents of water fluoridation about its alleged adverse health effects (10). To reach the goal of 75% of the public water drinking population supplied with optimally fluoridated water, policymakers and public health officials at the federal, state, and local levels will need to devise new promotion and funding approaches to gain support for this prevention measure. Acknowledgements This report is based on data contributed by state health, natural resources, and environmental departments. S Randlett, Alaska Dept of Environmental Conservation. K Hayward, Arizona Dept of Health Svcs. L Mouden, DDS, Arkansas Dept of Health. D Brunson, MPH, Colorado Dept of Public Health and Environment. H Link, Connecticut Dept of Public Health. H Davis, DDS, Florida Dept of Health. E Alderman, DDS, Georgia Dept of Human Resources. M Greer, DMD, Hawaii Dept of Health. L Penny, Idaho Dept of Health and Welfare. L Lampiris, DDS, Illinois Dept of Public Health. D Cain, Indiana State Dept of Health. M Magnant, Iowa Dept of Public Health. R Murphy, Kentucky Dept for Public Health. S Russ, Maine Dept of Human Svcs. N Reilman, Maryland Dept of the Environment. F Barker, Massachusetts Dept of Public Health. J Shekter, Michigan Dept of Environmental Quality. D Rindall, Minnesota Dept of Health. J Young, DMD, Mississippi State Dept of Health. M Logston, Missouri Dept of Natural Resources. K McFarland, DDS, Nebraska Health and Human Svcs System. C Lawson, Nevada State Health Div. A Pelletier, MD, New Hampshire Dept of Health and Human Svcs. F Dickert, New Jersey Dept of Environmental Protection. R Romero, DDS, New Mexico Dept of Health. E Green, DDS, New York State Dept of Health. R King, DDS, North Carolina Dept of Health and Human Svcs. G Stewart, MPA, North Dakota Dept of Health. J Pierson, Ohio Dept of Health. M Morgan, DDS, Oklahoma State Dept of Health. K Salis, Oregon Health Div. N Gardner, DDS, Pennsylvania Dept of Health. R Lala, DDS, South Carolina Dept of Health and Environmental Control. M Baker, South Dakota Dept of Health. W Wells, Tennessee Dept of Environment and Conservation. K Zinner, MPH, Utah Dept of Health. A Lund, Vermont Dept of Health. K Day, DDS, Virginia Dept of Health. T Wilson, Washington Dept of Health. G Black, DDS, West Virginia Bur of Public Health. W LeMay, DDS, Wisconsin Div of Public Health. References
Table 1 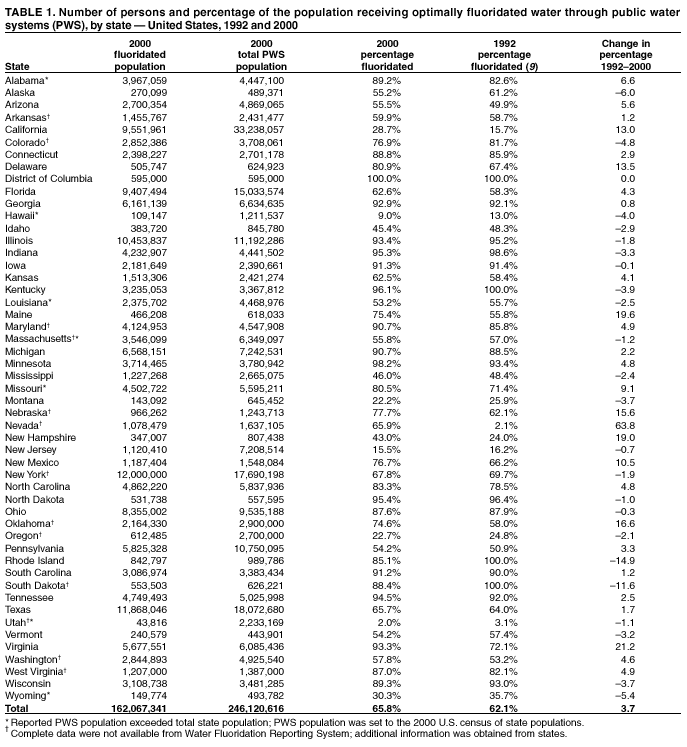 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 2/21/2002 |
|||||||||
This page last reviewed 2/21/2002
|