 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Pregnancy-Related Deaths Among Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native Women --- United States, 1991--1997In the United States in 1997, the Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native population represented 16% of all reproductive-age women (aged 15--49 years) but accounted for 23.5% of all live births (1,2). Although statistics by race/ethnicity are available for maternal deaths (3), pregnancy-related mortality ratios (PRMRs) have been reported regularly only for black and white women. Pregnancy-related deaths in Hispanic women have been studied (4); however, combining pregnancy-related mortality risk among Asians/Pacific Islanders and American Indians/Alaska Natives into an "other" category masks differences in their health status. This report presents PRMRs among Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native women in the United States during 1991--1997. The findings indicate that these groups have higher PRMRs than non-Hispanic white (white) women and lower ratios than non-Hispanic black (black) women and underscore the need for targeted interventions that address the maternal health needs of racial/ethnic minority women. For this report, pregnancy-related death was defined as a death that occurred during pregnancy or within 1 year after the end of pregnancy and resulted from 1) complications of pregnancy itself, 2) a chain of events initiated by pregnancy, or 3) aggravation of an unrelated condition by the physiologic effects of pregnancy. PRMRs were defined as the number of pregnancy-related deaths per 100,000 live births. PRMRs were calculated using data from the National Pregnancy Mortality Surveillance System (NPMSS) for the numerator and the public use natality files from CDC's National Center for Health Statistics for the denominator (2). NPMSS data are derived from death certificates sent to CDC by the 50 states, the District of Columbia (DC), and New York City. The death certificates are those on which pregnancy was indicated and for women who had given birth during the year preceding their death; matching live birth and fetal death certificates also are forwarded when available. In this analysis, racial/ethnic categories used were Hispanic, defined as a woman of any race who was of Hispanic origin, Asian/Pacific Islander, and American Indian/Alaska Native. Findings for white and black women were included for comparison. Place of birth (i.e., the 50 states, DC, and outside the United States) was analyzed for 1993 through 1997. During 1991--1997, 3193 pregnancy-related deaths occurred. The overall PRMR was 11.5. PRMR among American Indians/Alaska Natives was 12.2, among Asians/Pacific Islanders was 11.3, and among Hispanics was 10.3. PRMR was 29.6 and 7.3 among blacks and whites, respectively (Table 1). The risk among Hispanics, Asians/Pacific Islanders, and American Indians/Alaska Natives was lower than for blacks but higher than for whites; relative ratios ranged from 1.4 to 1.7. Among racial/ethnic groups for which rates have been estimated, the risk for death was lowest among women aged <30 years and increased after age 35 years. In all age groups, the risk for death was highest among black women, with a risk three to four times greater than white women. During 1993--1997, approximately 19% of all live births were to women born outside the 50 states and DC: among white, black, and American Indian/Alaska Native women, the percentage of live births to foreign-born women was <10%; among Hispanic women, approximately 62%; and among Asian/Pacific Islander women, approximately 86%. Hispanic women born outside the United States had a PRMR approximately 50% higher than U.S.-born Hispanic women (Table 2). Asian/Pacific Islander women born outside the United States also had a higher PRMR than their U.S.-born counterparts. However, the estimate should be interpreted with caution because of the small number of events. Black and white women had no significant differences in PRMRs by place of birth. PRMR for American Indians/Alaska Natives could not be analyzed by place of birth because of small numbers. Reported by: Div of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion; and an EIS Officer, CDC. Editorial Note:By 2025, Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native women are expected to represent approximately 25% of the females of reproductive age in the United States (1). The findings in this report indicate that these women have a significantly higher risk for pregnancy-related death than white women. The report also found that being born outside the 50 states and DC may be a more important risk factor than racial/ethnic heritage for some groups; increased risk for pregnancy-related death was found among foreign-born Hispanic women and possibly among Asians/Pacific Islanders. Examination of health outcomes only by racial and ethnic classification is insufficient to understand and reduce health disparities. Race and ethnicity may be indicators of differences in socioeconomic status, access to and quality of care, and psychosocial and environmental stress. Nativity also may be associated with factors (e.g., low income, low levels of education, lack of health insurance, and legal, language, and cultural barriers) that can adversely affect health outcomes, including inadequate health care (5). In addition, heterogeneity within racial/ethnic minority groups should be considered. Among Hispanics, reproductive health outcomes may differ among Mexican, Puerto Rican, and Cuban women (3,6). Asians/Pacific Islanders have many differences in language, culture, history, demographic characteristics, and circumstances of migration, and have a pattern of socioeconomic extremes, with a large proportion at high income levels and a large proportion in poverty (7). American Indians/Alaska Natives are from more than 500 different tribes, with differences in health status among tribes and between urban and reservation communities. This heterogeneity means that the PRMRs in this report could mask higher levels of risk among groups that have been combined with other groups at lower risk. The findings in this report are subject to at least four limitations. First, race/ethnicity information on death certificates, which is reported by a funeral director, may be less accurate than on birth certificates, which is usually reported by the mother. Death rates are estimated to be understated for Native Americans by 21%, for Asians/Pacific Islanders by 11%, and for Hispanics by 2% (8). Second, pregnancy-related deaths in general are underestimated because the death certificate frequently does not reflect the relation between a woman's pregnancy and her death (9). Third, in some groups the number of cases is small, which can lead to unstable PRMR estimates. Fourth, this report is limited to women who lived in the 50 states, DC, and New York City. Inclusion of data from Puerto Rico would be useful for investigating reproductive health outcomes among Hispanic women from that commonwealth. An important national health objective for 2010 is to eliminate racial disparities, including those in pregnancy-related death. Additional information on maternal health of minority women is needed to plan effective interventions. Studies could address the unique concerns of immigrant women in pregnancy and the prevalence and case- fatality rates for specific conditions in each group. Although rare, pregnancy-related deaths can be viewed as sentinel events in women's health; pregnancy-related illness is more common, with 18 pregnancy-associated hospitalizations per 100 live births (10). Developing systems to monitor pregnancy-related illness would contribute to a comprehensive understanding of factors that affect maternal health. Existing systems to monitor maternal health, such as the Pregnancy Risk Assessment Monitoring System, may be adapted to assist in this process. Reducing the maternal health disparities will require ongoing surveillance of morbidity and mortality, prevention research to identify the impact of key cultural and health issues, and prevention programs to address them. References
Table 1 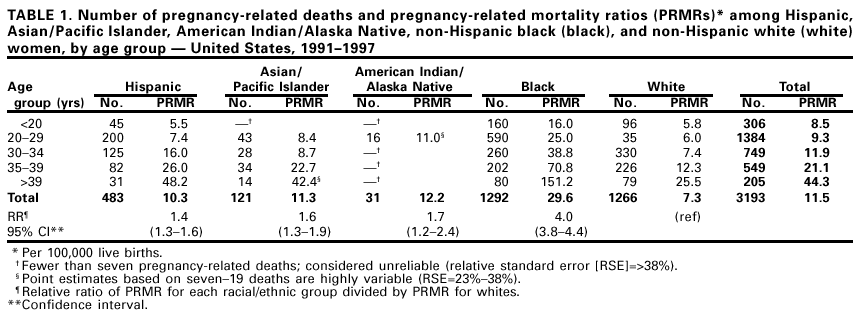 Return to top. Table 2 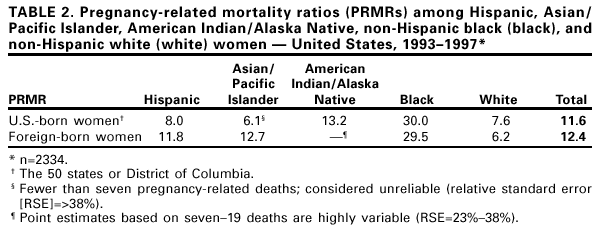 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 5/10/2001 |
|||||||||
This page last reviewed 5/10/2001
|