 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Public Health Consequences Among First Responders to Emergency Events Associated With Illicit Methamphetamine Laboratories --- Selected States, 1996--1999Methamphetamine, a central nervous system stimulant, is manufactured in illicit laboratories using over-the-counter ingredients (1). Many of these ingredients are hazardous substances* that when released from active or abandoned methamphetamine laboratories can place first responders† at risk for serious injuries and death. In 16 states§, the Agency for Toxic Substances and Disease Registry maintains the Hazardous Substances Emergency Events Surveillance (HSEES) system to collect and analyze data about the morbidity and mortality associated with hazardous substance-release events¶. Based on events reported to HSEES during 1996--1999, this report describes examples of events associated with illicit methamphetamine laboratories that resulted in injuries** to first responders in three states, summarizes methamphetamine-laboratory events involving injured first responders, and suggests injury prevention methods to protect first responders. WashingtonIn April 1996, an oven exploded as two persons were using acetone, hydrochloric acid, and sodium hydroxide to manufacture methamphetamine in an illicit apartment laboratory; one person sustained chemical burns and was taken to a hospital emergency department. The source of the burns was not revealed and, as a result, three hospital employees had nausea and vomited while treating the person. Three emergency medical technicians (EMTs) and two police officers exposed to emissions from the fire had eye and respiratory irritation. None of the injured first responders was wearing personal protective equipment (PPE) at the time of injury. OregonIn February 1999, a firefighter sustained chemical burns after exposure to hydrochloric acid and ephedrine during a fire at an illicit methamphetamine laboratory in a house in a residential neighborhood. Chemicals and other drug-manufacturing paraphernalia used to make methamphetamine were found after the fire was extinguished. The firefighter, who had worn turn-out gear†† as PPE at the time of injury, was decontaminated at the site, treated at a local hospital, and released. IowaIn March 1999, three police officers had respiratory irritation after exposure to anhydrous ammonia and ether emissions during a raid of an illicit residential methamphetamine laboratory. The officers were decontaminated at the site, treated at a local hospital, and released. They had not worn PPE at the time of injury. SummaryOf the 23,327 events reported to the HSEES system during 1996--1999, 1673 (7.2%) resulted in injuries: 112 (0.5%) events were associated with methamphetamine; 59 (52.7%) methamphetamine-associated events resulted in injuries. Methamphetamine-associated events were reported by five state health departments (Iowa, Minnesota, Missouri, Oregon, and Washington) participating in the HSEES system. Of the 112 events, 155 persons were injured; 79 (51.0%) injured persons were first responders: 55 (69.6%) police officers, nine (11.4%) EMTs, eight (10.1%) firefighters, and seven (8.9%) hospital employees (Table 1). The 79 injured first responders had 111 injuries (Table 1); 60 (54.1%) were respiratory irritation (e.g., cough, difficulty breathing, and throat irritation), and 12 (10.8%) were eye irritation; 61 (77.2%) injured first responders were treated at a hospital and did not require admission. PPE status at the time of injury was known for 67 (84.8%) of the 79 injured first responders; 57 (85.1%) had not worn PPE at the time of injury (45 [78.9%] were police officers). Of the 36 events causing injuries to first responders, 12 (33.3%) involved anhydrous ammonia and 11 (30.6%) involved hydrochloric acid. In 33 (91.7%) of the 36 events for which the type of release was known, 19 (57.6%) involved air emissions, 10 (30.3%) involved fires, and seven (21.2%) involved explosions. Reported by: D Cooper, Iowa Dept of Public Health. L Souther, Minnesota Dept of Health. D Hanlon, P Fischer, Missouri Dept of Health. R Leiker, MS, T Tsongas, PhD, Oregon Health Div. L Harter, C Comeau, Washington Dept of Health. Epidemiology and Surveillance Br, Div of Health Studies, Agency for Toxic Substances and Disease Registry. Editorial Note:This report illustrates how first responders were at risk for injuries during emergency events associated with illicit methamphetamine laboratories. Of all HSEES events, methamphetamine-associated events accounted for a small number; however, they were more likely to result in injuries. Substances used in methamphetamine laboratories often are corrosive, explosive, flammable, and toxic and can cause fires, explosions, and other uncontrolled reactions (3,4). These laboratories may be found in various environments, including motel rooms, private residences, campgrounds, and motor vehicles (3,5); an estimated 20%--30% of known methamphetamine laboratories were discovered because of fires and explosions (6). Hazardous substances released during and after an event usually enter the body by inhalation and skin absorption (3); acute exposures may result in cough, headache, chest pain, burns, pulmonary edema, respiratory failure, coma, and death (3,4,6). Of the types of responders usually on site first, police officers had the greatest number of injuries because they were present during and immediately after a release. EMTs sustained most injuries through on-site exposure or direct contact with the clothing or skin of contaminated persons. Firefighters, the least often injured on-site first responders, were likely to be wearing PPE during events. Hospital personnel injuries may have been caused by injured persons not being decontaminated before being brought to the hospital. Standard uniforms worn by police officers, EMTs, and hospital personnel provided little or no chemical/respiratory protection. During some events, turn-out gear worn by firefighters offered only limited protection. The findings in this report are subject to at least two limitations. Reporting of any event to HSEES is not mandatory; therefore, participating state health departments may not be informed about every event. Because methamphetamine laboratories are illicit, sources (primarily law enforcement officials) might hesitate to report events that may jeopardize investigations. Second, HSEES is not conducted in all states, and HSEES data may not represent populations in other areas. Interventions that can reduce risk for injuries among first responders to methamphetamine-laboratory events include 1) increasing awareness of the risks associated with illicit drug laboratories, 2) encouraging training in situations involving hazardous material, 3) identifying the nature of the event before entering the contaminated area, 4) wearing appropriate PPE, and 5) following a proper decontamination process after exposure to hazard ous substances. Information about the hazards likely to be encountered and protective measures that can be taken by first responders at methamphetamine-associated events can be found at http://www.cdc.gov/niosh/npg/pgdstart.html and http://hazmat.dot.gov/erg2000/psnsort.htm§§ . References
* Any substance that can cause an adverse health effect (2). † Includes firefighters (e.g., professional and volunteer), police officers, emergency medical technicians, and hospital personnel (e.g., physicians and nurses). § During 1996--1999, state health departments in Alabama, Colorado, Iowa, Minnesota, Mississippi, Missouri, New Hampshire (in 1996), New York, North Carolina, Oregon, Rhode Island, Texas, Washington, and Wisconsin participated in HSEES. Three states were added in 2000. ¶ An uncontrolled or illegal release (e.g., spill, fire, and explosion) or threatened release of hazardous substances or hazardous by-products. To be considered a methamphetamine event, it must meet the HSEES definition and be associated with the illicit production of methamphetamine. The existence of these laboratories does not qualify them as an event. Information on substances released, number of persons injured, types of injuries, and evacuations is collected by state health departments from sources such as state environmental protection agencies, local police and fire departments, local media, and hospitals, and is reported to HSEES. ** Includes illnesses and other adverse health effects. §§ References to sites of nonCDC organizations on the WorldWide Web are provided as a service to MMWR readers and do not constitute or imply endorsement of these organizations or their programs by CDC or the U.S. Department of Health and Human Services. CDC is not responsible for the content of pages found at these sites. †† Coat, pants, boots, and gloves worn during structural firefighting operations that offer limited harmful vapor or liquid protection with self-contained breathing apparatus. Table 1 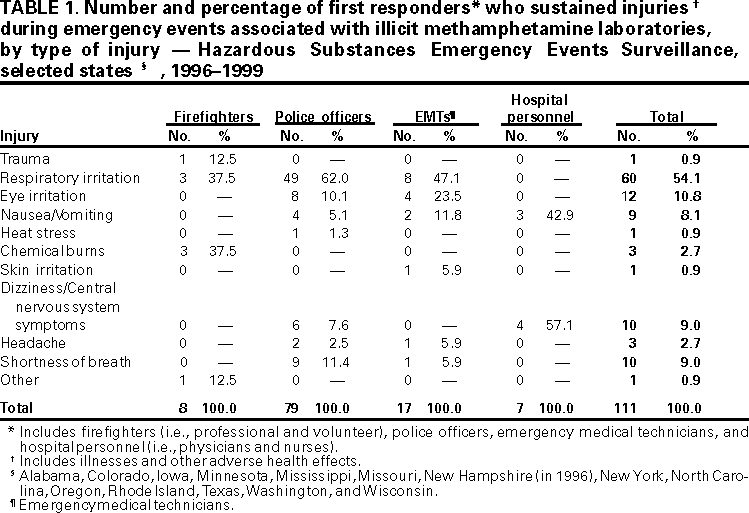 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 11/16/2000 |
|||||||||
This page last reviewed 5/2/01
|