 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Receipt of Advice to Quit Smoking in Medicare Managed Care --- United States, 1998In the United States, cigarette smoking is the leading cause of preventable morbidity and mortality, and smokers who stop at any age reduce their risk for premature death (1). Because older smokers are more likely to report having seen a physician during the preceding year (84% in 1992) compared with younger smokers (69%) (2), health-care providers have many opportunities to advise older smokers to quit. To characterize smoking and advice to quit among Medicare managed-care recipients, the Health Care Financing Administration and CDC analyzed data from the 1998 Health Outcomes Survey (HOS). This report summarizes the results of that analysis, which indicates that approximately 13% of enrollees in Medicare managed care reported they were current smokers, and among those who visited a physician or health-care provider, approximately 71% reported receiving advice to quit. HOS is an ongoing, 2-year, longitudinal cohort survey administered to Medicare beneficiaries enrolled in managed-care plans nationwide. The survey measures health status and health outcomes to provide risk-adjusted measures of managed-care plan performance and to track population-based care outcomes. Medicare enrollees were initially contacted by mailed questionnaire, and nonrespondents were followed up by mail and telephone. Respondents were asked about current smoking status, quitting behavior during the preceding 12 months or longer, receipt of advice to quit from a doctor or other health-care provider, and the number of health-care visits during the preceding year. A random sample of approximately 1000 Medicare managed-care enrollees was selected from each of 287 separate strata, representing 268 different health plans. Thirteen of these plans had two to four geographically distinct subplan market areas for 19 additional strata. A total of 279,135 Medicare beneficiaries were in the sample. The sample included both Medicare beneficiaries aged >65 years (91.5%) and persons aged <65 years and in Medicare because of disabilities (8.5%) who were enrolled in their plan for at least 6 months. It also included institutionalized beneficiaries but excluded persons eligible for Medicare because of end-stage renal disease alone. Baseline data were collected during May--July 1998. The overall response rate to the baseline survey was 59.9% (167,201); 152,259 reported their smoking status, and 19,604 (95.6%) of those who reported smoking during the previous year responded to the question about whether they received advice to quit. Data were weighted to the total population of each stratum and adjusted to the overall population age, race, and sex distribution. In 1998, 10.4% of Medicare managed-care enrollees reported smoking every day and 2.9% reported smoking some days (Table 1). Daily smoking prevalence was highest among enrollees aged <65 years and lowest among enrollees aged >85 years. Daily smoking prevalence was higher for men than for women, and smoking prevalence was greater among those with less education and less income. Among all enrollees, 1.6% reported having quit during the preceding 12 months, and 39.3% reported having quit smoking >1 year before the survey. Smoking prevalence was lowest and quit rates highest among enrollees from the western region. Of persons who reported any smoking during the preceding 12 months and who visited a physician or other health-care provider at least once during that time, 70.7% reported they had been advised to quit smoking (Table 2). Advice to quit increased with increasing numbers of visits: 61.5% of smokers with one visit during the year reported receiving advice to quit compared with 76.2% of those with five or more visits. Across all visit categories, women who made one to four visits reported receiving advice to quit at slightly higher rates than did men, and smokers aged >75 years reported receiving less advice to quit than did younger smokers. Blacks and Hispanics reported receiving less advice than did whites. Overall, those with more education reported receiving less advice. Differences were reported in receipt of advice to quit between the types of managed-care plans, with providers in independent practice associations giving less advice than those in staff or group model practices, especially when a single visit was reported. Reported by: D Arday, MD, Office of Clinical Standards and Quality, Health Care Financing Administration. Epidemiology Br, Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The findings in this report indicate that receipt of advice to quit smoking probably has improved since the early 1990s, when 38.8% of smokers aged >65 years reported receiving advice (3). Self-reported receipt of advice is higher in this survey than the national average (62.5%) reported by the National Committee for Quality Assurance (NCQA) (4). The NCQA report is based on 1998 Health Plan Employer Data and Information Set (HEDIS) data from plan-administered surveys. However, the HEDIS data used a different sampling frame that applied to all adult beneficiaries in managed-care plans, not just those in Medicare. On the basis of these results, of 5.8 million Medicare enrollees in the sampling frame, approximately 92,000 had quit during the preceding year. Increasing the delivery of smoking cessation advice to 90% of those who still smoke would reach approximately 150,000 additional smokers and might encourage 25,000 more smokers to initiate quitting each year. Based on these survey findings, public health programs should target health-care providers in independent practice associations (IPAs) to deliver cessation advice. IPAs represent most physicians in private or small group practices who have contracted with HMO plans, and counseling rates for IPAs are lower than for group or staff model plans. The difference in receipt of advice to quit among racial/ethnic groups may be influenced by social or cultural factors. For example, among elderly Hispanics and Asian Americans, language barriers may affect the lower rates of receiving advice to quit or in understanding the advice. Health-care providers should offer culturally appropriate or tailored interventions for racial/ethnic populations (5). The findings in this report are subject to at least four limitations. First, the overall response rate for the 1998 HOS survey was 59.9%. Response rates varied widely by plan and somewhat by age and race. Although the HOS data were weighted to account for the stratified design and the overall population distribution by age, race, and sex, some differences could be the result of response biases. Second, because the HOS design does not include any oversampling of racial/ethnic minority groups or the oldest Medicare recipients, sample sizes within some substrata were inadequate to allow complete comparisons by all smoking or visit categories. Third, not all persons who reported quitting during the previous 12 months may have been candidates for advice. Because smoking status at the time of each doctor visit was not known, some may have quit before their first visit. Finally, because the reason for each visit was not included in the survey, some visits may have been for emergencies and other conditions during which counseling would not have been appropriate. Smoking prevalence among Medicare managed-care enrollees is similar to that among older adults (6). Despite the lower prevalence of current smoking among older adults compared with middle aged and young adults, older smokers are at greater risk from smoking because they have smoked longer, tend to be heavier smokers, and are more likely to suffer already from smoking-related illnesses (7). Overall, 1.6% of the Medicare managed-care population reported quitting during the preceding 12 months, representing approximately 10% of the smokers who reported any smoking within that period. However, it is likely that some of those who quit during the preceding year will begin smoking again. Health-care providers should be aware that smoking cessation counseling, even brief advice to quit smoking, can be effective in encouraging older smokers to quit. All health-care providers should deliver tobacco-use treatment interventions to their patients (5). Basic components of a counseling session include asking each patient whether he or she uses tobacco, urging all tobacco users to stop, identifying tobacco users willing to quit, providing assistance to these patients (e.g., establishing a quit date, providing support and practical advice on the quitting process, and encouraging the use of approved pharmocotherapies such as nicotine replacement therapy and buproprion when appropriate), and arranging follow-up visits for support (5). Use of office reminders, such as chart stickers or vital sign, can increase the provision of cessation advice by providers (5). Reimbursement of treatment services and products has been shown to increase use of cessation services and overall quit rates (8). References
Table 1 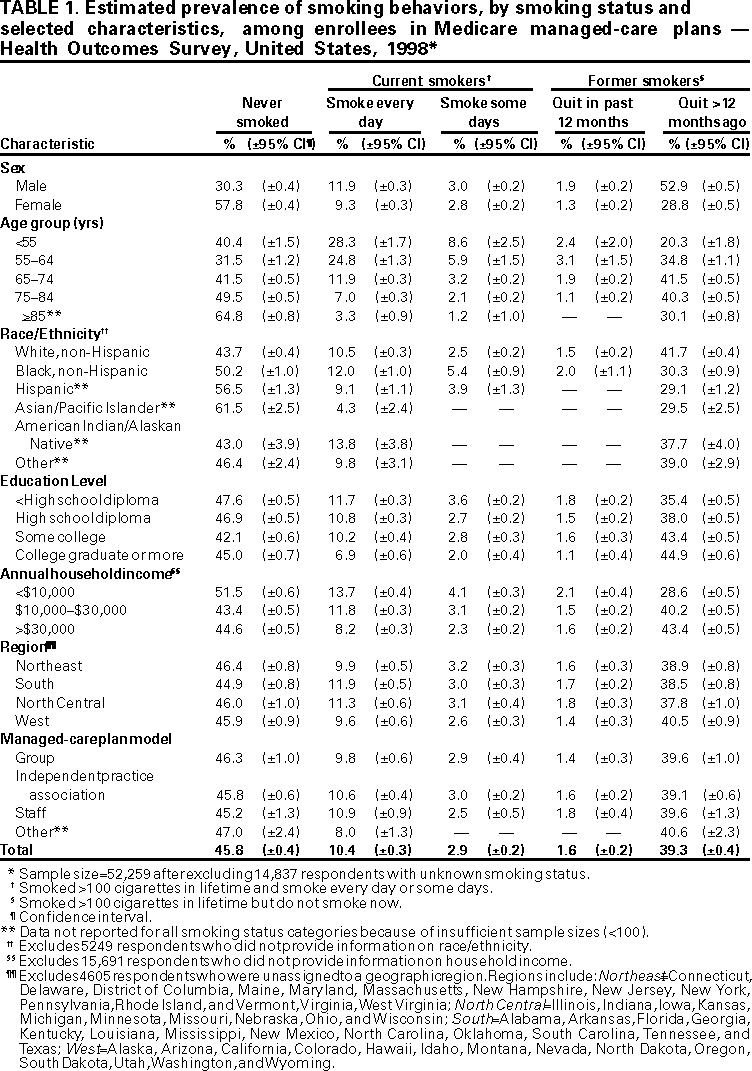 Return to top. Table 2 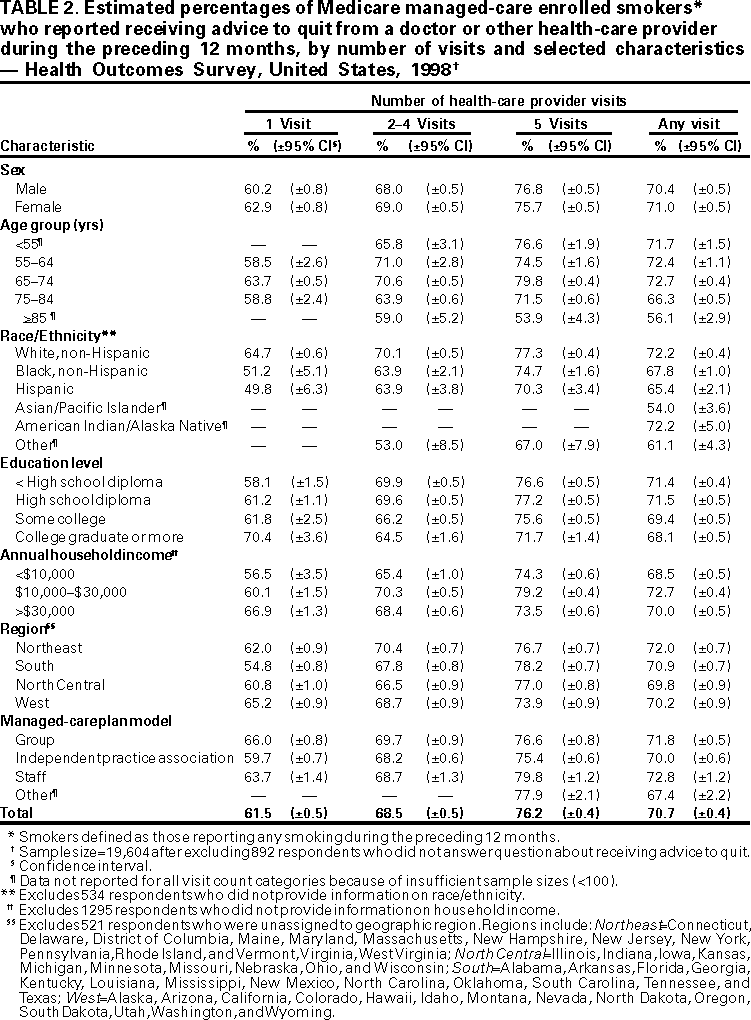 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 9/7/2000 |
|||||||||
This page last reviewed 5/2/01
|