 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Prevalence of Selected Cardiovascular Disease Risk Factors Among American Indians and Alaska Natives --- United States, 1997Heart disease and stroke, the principal causes of cardiovascular disease (CVD), are the first and fifth leading causes of death among American Indians and Alaska Natives (AI/AN) (1,2). Risk factors for CVD frequently cluster, which may increase CVD risk multiplicatively (3). To characterize the prevalence of risk factors for CVD (i.e., hypertension, current cigarette smoking, high cholesterol, obesity, and diabetes) among AI/AN, CDC analyzed data from the 1997 Behavioral Risk Factor Surveillance System (BRFSS). This report summarizes the results of that analysis, which indicated that 63.7% of AI/AN men and 61.4% of AI/AN women who participated in the survey had one or more CVD risk factors. BRFSS is an ongoing state-based, random-digit--dialed telephone survey of the U.S., noninstitutionalized civilian population. Self-reported data were analyzed for the 1820 AI/AN aged >18 years who participated in the 1997 BRFSS in 50 states and the District of Columbia (DC). Identification of race as AI/AN was based on response to the question, "What is your race?" Awareness of hypertension, high cholesterol, and diabetes was determined by the response to, "Have you even been told by a doctor or other health professional that you have (hypertension, high cholesterol, diabetes)." Current smoking status was defined as having smoked at least 100 cigarettes during one's lifetime and still smoking at the time of the survey. Self-reported data on height and weight were used to calculate body mass index (BMI). Obesity was defined as a BMI >30 kg/m2. Persons defined as employed were either employed for wages or self-employed, regardless of the number of hours spent on the job. The 50 states and DC were grouped into the four geographic regions defined by the U.S. Bureau of the Census (1). Sample estimates were weighted by sex, age, and race to reflect the state's noninstitutionalized civilian population. To account for the complex sampling design, SUDAAN was used for data analysis (4). Of the 1820 AI/AN BRFSS participants, 46.3% were women; 63.3% were aged 18--44 years, 25.6% were 45--64 years, and 11.1% were >65 years (mean: 42.4 years; standard deviation=16.2); 15.9% were college graduates; 60.2% were employed; and 49.8% ranked their health status as excellent or very good. The largest percentage of AI/AN participants in the BRFSS lived in the West (47.4%), followed by the South (25.9%), the Midwest (17.4%) and the Northeast (9.3%).* Approximately 22% of participants reported being told by a health professional that they had hypertension (women=23.0%, men=21.0%). Thirty-one percent reported they were current smokers (men=32.8%; women=28.8%). Approximately 16% were told by a health professional that they had high cholesterol, and 7% were told they had diabetes. Awareness of high cholesterol and diabetes was higher among women (17.6% and 9.1%, respectively) than men (13.8% and 5.5%, respectively). Nearly one fourth (23.6%) of men and nearly one fifth (19.1%) of women were categorized as obese (21.5% of all AI/AN). Among AI/AN men, 36.3% reported having none of the selected CVD risk factors, 41.4% reported having one risk factor, and 22.3% reported having >2 risk factors (Table 1). Among AI/AN women, 38.6% reported having no CVD risk factors, 37.7% reported having one risk factor, and 23.7% reported having >2 risk factors. The prevalence of having one or more CVD risk factors increased with increasing age (Table 1). The prevalence of having >2 risk factors was highest among respondents aged >65 years. The prevalence of having >2 CVD risk factors varied inversely with level of education (Table 1). Approximately 25% of AI/AN men with less than a high school education reported having >2 CVD risk factors, compared with approximately 15% of AI/AN men who were college graduates. AI/AN women with less than a high school education were almost three times more likely to report having >2 risk factors than were AI/AN women who had graduated from college. The percentage of having >2 risk factors was almost three times higher among unemployed women than employed women. Half of the respondents who reported their health status as fair or poor reported having >2 CVD risk factors (women=51.8%; men=50.0%) compared with approximately one eighth of respondents who reported their health status as excellent or very good (women=13.3%; men=13.2%) (Table 1). The number of reported CVD risk factors varied by geographic region (Table 1). For men, the prevalence of having >2 risk factors was highest in the Midwest (26.1%) and lowest in the Northeast (13.8%). Less geographic variation was observed among women. The prevalence of having >2 risk factors was highest in the Northeast (28.0%) and lowest in the West (20.0%). Reported by the following BRFSS coordinators: S Reese, MPH, Alabama; P Owen, Alaska; B Bender, MBA, Arizona; G Potts, MBA, Arkansas; B Davis, PhD, California; M Leff, MSPH, Colorado; M Adams, MPH, Connecticut; F Breukelman, Delaware; I Bullo, District of Columbia; S Hoecherl, Florida; L Martin, MS, Georgia; F Reyes-Salvail, MS, Hawaii; J Aydelotte, MA, Idaho; B Steiner, MS, Illinois; L Stemnock, Indiana; K MacIntyre, Iowa; C Hunt, Kansas; T Sparks, Kentucky; B Bates, MSPH, Louisiana; D Maines, Maine; A Weinstein, MA, Maryland; D Brooks, MPH, Massachusetts; H McGee, MPH, Michigan; N Salem, PhD, Minnesota; D Johnson, MS, Mississippi; J Jackson-Thompson, PhD, Missouri; P Feigley, PhD, Montana; L Andelt, PhD, Nebraska; E DeJan, MPH, Nevada; L Powers, MA, New Hampshire; G Boeselager, MS, New Jersey; W Honey, MPH, New Mexico; C Baker, New York; P Buescher, PhD, North Carolina; L Shireley, MPH, North Dakota; P Pullen, Ohio; K Baker, MPH, Oklahoma; J Grant-Worley, MS, Oregon; L Mann, Pennsylvania; J Hesser, PhD, Rhode Island; M Wu, MD, South Carolina; M Gildemaster, South Dakota; D Ridings, Tennessee; K Condon, Texas; K Marti, Utah; C Roe, MS, Vermont; K Carswell, MPH, Virginia; K Wynkoop Simmons, PhD, Washington; F King, West Virginia; P Imm, MS, Wisconsin; M Futa, MA, Wyoming. Div of Applied Public Health Training, Epidemiology Program Office; Cardiovascular Health Br, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion; and an EIS Officer, CDC. Editorial Note:The findings in this report document the prevalence of selected CVD risk factors among AI/AN by sociodemographic characteristics and are consistent with previous findings that CVD risk factors and death rates are not uniformly distributed across regions among AI/AN (2,5). Higher CVD death rates have been reported among AI/AN residing in the Midwest (2); data from this study indicate that AI/AN men residing in the Midwest were most likely to report having >2 CVD risk factors. Geographic variation in risk factors and death rates may reflect differences in cultural backgrounds, historical circumstances, and socioeconomic conditions. Prevalence estimates probably are influenced by sociodemographic factors (i.e., age distribution, educational attainment, employment status, and poverty), lifestyle (i.e., physical inactivity), aspects of the social environment (i.e., educational and economic opportunities), and factors affecting the health-care system (i.e., access to health care, cost, and availability of screening for diseases and risk factors). Higher prevalences of multiple CVD risk factors among AI/AN participants who were either unemployed or had completed less than a high school education corroborate the well-documented influence of low socioeconomic status on CVD risk factors. The findings in this report are subject to at least five limitations. First, estimates of CVD risk factors are based on self-reported data and are subject to the biases associated with self-reported data. Second, these results probably underestimate the prevalence of CVD risk factors because the data are dependent on the respondent being aware of his risk factor profile. Third, data on physical inactivity, a risk factor for CVD, was not collected in the 1997 BRFSS survey. If data on physical activity levels had been included, the prevalence of CVD risk factors among AI/AN probably would have been higher. Fourth, approximately 23% of AI/AN households do not have a telephone (6); these findings could underestimate the prevalence of CVD risk factors among AI/AN because persons without telephones are more likely to be of lower socioeconomic status and to have higher risk for disease (7). Finally, BRFSS does not collect information on reservation residency or tribal affiliation. Aggregating the AI/AN participants into relatively large geographic regions may mask important differences among the tribes. The percentages of AI/AN with multiple CVD risk factors highlight the importance of enhancing primary prevention activities among communities of AI/AN. Through CDC's Racial and Ethnic Approaches to Community Health (REACH 2010) Project (8), two AI/AN communities are developing effective and sustainable programs designed to eliminate racial/ethnic disparities in CVD and diabetes. Another activity is the Inter-Tribal Heart Project, a collaboration between CDC, the Indian Health Service, and three tribal communities to determine the prevalence of risk factors for heart disease and to implement community-based heart disease prevention programs (9). Reducing the prevalence of CVD risk factors among AI/AN requires an understanding of the diversity of cultural values and practices among AI/AN, and historical circumstances that contributed to the current socioeconomic conditions. Therefore, tribal-specific assessments of CVD risk factor profiles and CVD morbidity and mortality profiles are needed to develop culturally relevant CVD prevention programs and policies that support heart-healthy living and working conditions for AI/AN. References
*Northeast=Connecticut, Maine, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Vermont; Midwest=Illinois, Indiana, Iowa, Kansas, Michigan, Minnesota, Missouri, Nebraska, North Dakota, Ohio, South Dakota, and Wisconsin; South=Alabama, Arkansas, Delaware, District of Columbia, Florida, Georgia, Kentucky, Louisiana, Maryland, Mississippi, North Carolina, Oklahoma, South Carolina, Tennessee, Texas, Virginia, and West Virginia; and West=Alaska, Arizona, California, Colorado, Hawaii, Idaho, Montana, Nevada, New Mexico, Oregon, Utah, Washington, and Wyoming. Table 1 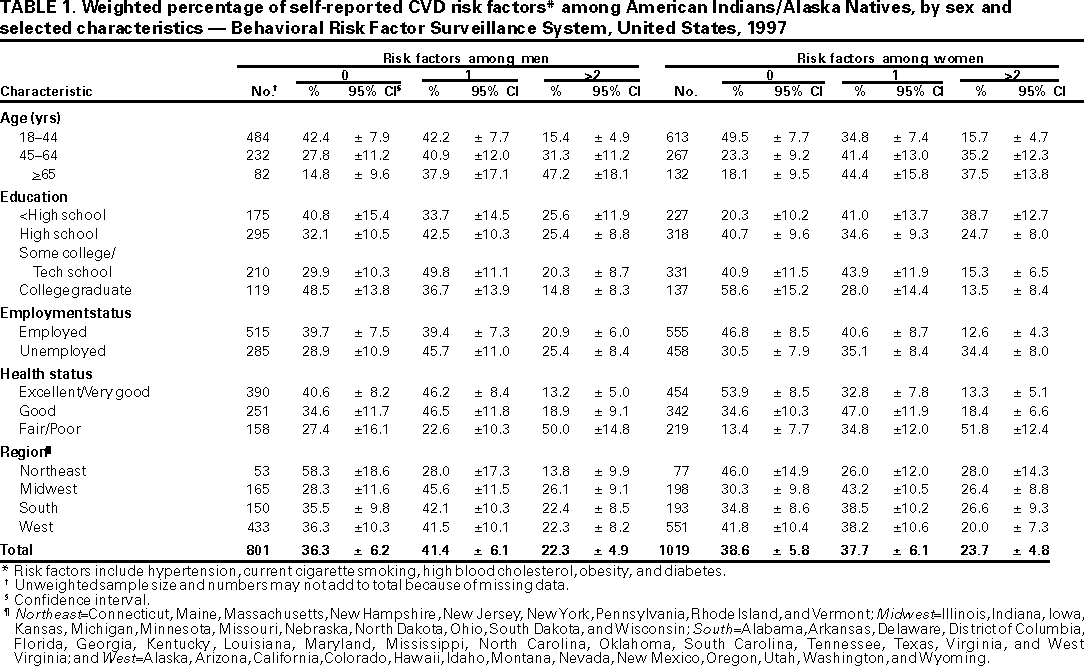 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 6/5/2000 |
|||||||||
This page last reviewed 5/2/01
|