 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Surveillance for Possible Estuary-Associated Syndrome --- Six States, 1998--1999Pfiesteria piscicida (Pp) is an alga that has been associated with fish kills in estuaries (where fresh water mixes with salty seawater) along the eastern seaboard and possibly with human health effects (1,2). Since June 1, 1998, surveillance for possible estuary-associated syndrome (PEAS), including possible Pp-related human illness, has been conducted in Delaware, Florida, Maryland, North Carolina, South Carolina, and Virginia. This report summarizes passive surveillance for PEAS during June 1, 1998--December 31, 1999, which indicated no persons had illnesses that met PEAS criteria. The PEAS surveillance system collects information about possible human health problems that may occur after exposure to estuarine water (such as sounds or coastal river mouths or in laboratories or aquaculture facilities). For surveillance purposes, persons are considered to have PEAS if 1) they report developing symptoms within 2 weeks after confirmed exposure to estuarine water; 2) they report memory loss or confusion of any duration and/or three or more selected symptoms (i.e., headache, skin rash at the site of water contact, sensation of burning skin, eye irritation, upper respiratory irritation, muscle cramps, and gastrointestinal symptoms) that, except for skin rash at the site of water contact and sensation of burning skin, persist for >2 weeks; and 3) a health-care provider cannot identify another cause for the symptoms. The six state health agencies were available throughout the year to respond to inquiries from the public and health-care providers. Calls from persons requesting information or reporting symptoms that may be related to Pp or Pfiesteria-like organisms (PLOs) were recorded; environmental exposure and symptom information were recorded in the surveillance database. Surveillance information was periodically transferred to CDC for data aggregation and dissemination to the public. From June 1, 1998, through December 31, 1999, the six state health departments received 1984 calls about Pp, PLOs, and PEAS (Table 1). Most (96%) calls involved requests for information about Pp, PLOs, or PEAS. Seventy-eight calls concerned a symptomatic person; 54 (69%) of these persons had possible exposure to estuarine water. Of the 54 persons, 44 were seen by or referred to a health-care provider. Of the 44, 24 did not meet PEAS symptom or exposure criteria, 15 had another cause for symptoms identified, and five have environmental and medical results pending. To date, no illnesses have met the PEAS criteria. Reported by: AL Hathcock, PhD, C Nace, MS, Delaware Dept of Health and Social Svcs. D Johnson, MD, R Quimbo, MS, Florida Dept of Health. R Venezia, DrPH, A Chapin, MPH, Maryland Dept of Health and Mental Hygiene. JS Cline, DDS, K Buckheit, MPH, P Webb, MPH, North Carolina Dept of Health and Human Svcs. R Ball, MD, N Scruggs, MSPH, South Carolina Dept of Health and Environmental Control. S Jenkins, VMD, LA Peipins, PhD, M Monti, MS, M Brooks, Virginia Dept of Health. Health Studies Br, Div of Environmental Hazards and Health Effects, National Center for Environmental Health, CDC. Editorial Note:The greatest benefit of the PEAS surveillance system has been to provide information quickly to educate the public. Without specific tests, definitive diagnosis of illnesses associated with Pp or PLOs is not possible. However, health-care providers should continue to report suspected PEAS cases to their local health department. The PEAS criteria may change as new information becomes available from epidemiologic studies and laboratory tests are developed to identify Pp and its putative toxin in water and in human blood. The lack of PEAS cases may be explained by few "fish events" that have possible links to Pp since June 1, 1998. Fish events include fish kills, large numbers of fish with ulcerative lesions, or fish displaying abnormal behavior. One possible reason for the low number of Pp blooms is the massive hurricane-related flooding during the previous 2 years. Floods can dilute estuaries or deposit contaminants into coastal waters that may affect the life cycle and behavior of Pp. The findings in this report are subject to at least four limitations. First, because surveillance was passive, some cases may have been missed. Second, the number of information-only calls are underreported because several states do not track all information requests because of state differences in hotline system design. Third, data provided may have been incomplete because all states did not use the same data collection methods; however, a standardized core data collection method has been developed. Finally, the surveillance system tracks PEAS rather than Pp-related illness because a Pp toxin(s) has not been identified; therefore, a biomarker of exposure has not been developed. For this reason, association between PEAS and Pp remains to be established. Detection of Pp or lesioned fish in water has been used as evidence of suspected Pp toxin(s) (3). However, Pp has been found in waters without reports of harm to fish or persons, and fish lesions can result from a variety of biologic, physical, and environmental factors that may be unrelated to Pp. Consequently, detecting Pp or observing lesioned fish may not indicate the presence of a putative Pp toxin(s). It is unclear whether persons exposed to Pp while swimming, boating, or engaging in other recreational activities in coastal waters are at risk for developing PEAS. PEAS is not infectious and has not been associated with eating fish or shellfish caught in waters where Pp has been found. However, persons should avoid areas with large numbers of diseased, dying, or dead fish and should promptly report those areas to the state's environmental or natural resource agency. In addition, persons should not go in or near the water in areas that are closed officially by the state and should not harvest or eat fish or shellfish from these areas. Persons who experience health problems after exposure to estuarine water, a fish-disease event, or a fish-kill site should contact their health-care provider and state or local public health agency. Several states have established toll-free PEAS information lines: Delaware, (800) 523-3336; Florida, (888) 232-8635; Maryland, (888) 584-3110; North Carolina, (888) 823-6915; South Carolina, (888) 481-0125; and Virginia, (888) 238-6154. References
Table 1 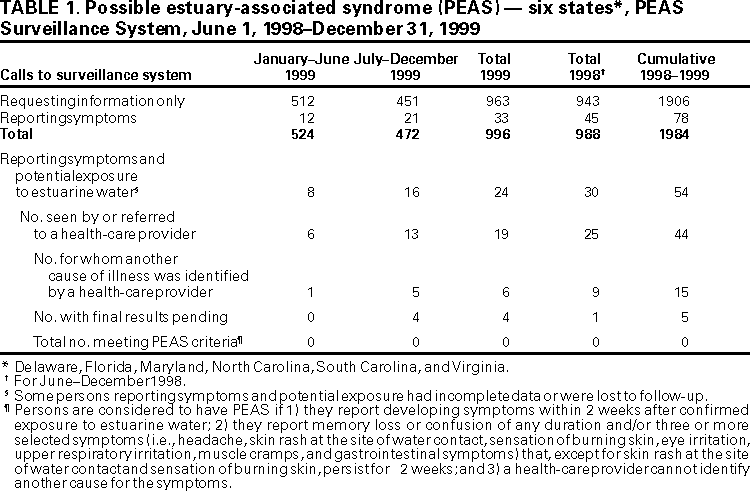 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 5/4/2000 |
|||||||||
This page last reviewed 5/2/01
|