 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Epidemic Typhoid Fever -- Dushanbe, Tajikistan, 1997Typhoid fever, a severe systemic illness transmitted through food or water, is caused by the bacterium Salmonella serotype Typhi (1). This report describes a major epidemic of typhoid fever in Dushanbe, Tajikistan (Figure_1), that resulted from contamination of the municipal water system. In Tajikistan, the Sanitary Epidemiologic Service (SES) maintains records for reportable diseases (2). Dushanbe (1997 population: 600,000) residents receive health care through assigned polyclinics; surveillance for reportable diseases is based on polyclinic records. A case of typhoid fever is defined as physician diagnosis or isolation of S. Typhi from stool, blood, or urine cultures. In February 1997, a sudden increase in the number of typhoid fever cases was identified by SES in Dushanbe, with approximately 2000 cases registered during a 2-week period. In March, the Ministry of Health of Tajikistan requested assistance from CDC. In collaboration with local authorities and nongovernmental partners, CDC reviewed epidemiologic and laboratory surveillance; conducted a case-control study to identify risk factors for infection; and evaluated municipal drinking water quality, water wastage, and health-education campaigns. Of 10,766 cases of typhoid fever reported to SES during January 1996-July 1997, 8901 cases (2659 {30%} confirmed) and 95 deaths (case-fatality rate: 1.1%) occurred during January-June 1997 (Figure_2). The monthly typhoid fever incidence peaked at 570 per 100,000 population during February and decreased to 93 in June. Median patient age was 16 years (range less than 1-80 years); 50% were female. The microbiology laboratory of City Hospital Number 2 monitored antimicrobial resistance during the epidemic. Of 56 isolates at that hospital from January through March 1997, 52 (93%) were resistant to chloramphenicol, ampicillin, and trimethoprim-sulfamethoxazole, antimicrobial agents used traditionally as first-line therapy for treatment of typhoid fever. On additional testing at CDC, 79% of the isolates also were resistant to nalidixic acid; none were resistant to ciporfloxacin. CDC and SES conducted a case-control study to determine risk factors for developing typhoid fever. Using a written questionnaire, SES interviewed 43 culture-positive patients or their parents and 123 age-matched, neighborhood controls. Illness was associated with drinking unboiled water in the 30 days before onset (matched odds ratio {MOR}=6.5; 95% confidence interval {CI}=3.0-24.0), obtaining drinking water from a tap outside the home (MOR=9.1; 95% CI=1.6-82.0), and eating food from a street vendor (MOR=2.9; 95% CI=1.4-7.2). On multivariate conditional logistic regression analysis, drinking unboiled water (MOR=9.6; 95% CI=2.7-34.0) and obtaining water from an outside tap (MOR=16.7; 95% CI=2.0-138.0) were significantly associated with illness. Routinely boiling water in one's home for drinking was protective (MOR=0.2; 95% CI=0.05-0.5). Municipal drinking water in Dushanbe is supplied by two surface water (Varzob River) and two ground water treatment plants. On inspection of the surface water treatment plants in March 1997, sedimentation basins and filters were full of silt, rendering them ineffective at removing solids and biological contaminants from river water. Finished water samples obtained before distribution from both surface treatment plants during March 22-April 7 revealed concentrations of 100-200 colony forming units (CFU) of fecal (thermotolerant) coliform bacteria per 100 mL. Water leaving the treatment plants entered an interconnected distribution system where surface and ground water blended. In the distribution system, the average concentration of fecal coliform bacteria in water, adjusted for the proportion of water supplied by each plant, was approximately 60 CFU per 100 mL. World Health Organization guidelines for potable water require less than 1 CFU per 100 mL (3). To evaluate further municipal water quality, water samples were collected from taps in randomly selected 1 hectare areas in Dushanbe. Fecal coliform bacteria were detected in 26 of 27 household tap water samples tested (mean=175 CFU per 100 mL; range: 4-greater than 400 CFU per 100 mL). Although water leaving the surface water treatment plants was fecally contaminated, higher colony counts at taps suggested that further contamination occurred within the distribution system. Water distribution pipes were frequently located in open storm channels that also contained wastewater runoff. Low water pressure in the distribution system contributed to cross-contamination of drinking water with wastewater. To determine how pressure in the municipal water system could be increased, investigators measured water wastage from open and broken taps and pipes in randomly selected Dushanbe neighborhoods. Average water wastage was estimated to be 1040 liters per person per day. Chlorination of the municipal water supply ceased in December 1996, when chlorine supplies were exhausted, and resumed in April 1997, after international relief organizations provided chlorine to the water utility. After chlorination resumed, free chlorine residuals were monitored at the treatment plants and in tap water samples at 14 randomly selected sites during June 24-August 15, 1997. Free chlorine residuals in 30% of tap water samples tested remained below the targeted goal of 0.2 mg/L set by the water utility and international relief organizations. Follow-up testing in March 1998 revealed adequate chlorine residuals in tap water throughout the city. To control the epidemic, local authorities and nongovernmental organizations initiated public information campaigns for water conservation and typhoid fever prevention in June 1997. In August, 200 randomly selected households in Dushanbe were surveyed to assess knowledge, attitudes, and practices regarding these issues. Ninety-one percent of respondents reported having heard or read the campaign messages and having altered some of their behaviors. However, 51% of those surveyed reported they still drank unboiled water because they perceived municipal water to be safe. Repeated surveys indicate that after water conservation campaigns were initiated, water wastage in Dushanbe decreased by approximately half. These savings have enabled Dushanbe's water utility to plan closure of its largest surface water treatment plant, thus providing a larger proportion of the population with water from cleaner and safer groundwater sources. Reported by: A Samaridin, M Akhmedov, M Karimova, A Pirova, K Pirmamadov, M Rakhmonova, Dushanbe Sanitary Epidemiologic Svc; B Shoismatuloyev, Republican Sanitary Epidemiology Svc; I Dmitrievna Tkachuk, L Gasanova, S Lomakina, City Hospital Number 2; N Kravchenko, Dushanbe City Health Dept; K Faramusova, D Inomzoda, Red Crescent Society of Tajikistan; I Usmanov, A Akhmedov, Tajikistan Ministry of Health; K Metzler, Association for Technical Collaboration (GTZ), Wels, Germany. Refugee Health Unit, National Center for Environmental Health; Div of International Health, Epidemiology Program Office; Hospital Environment Laboratory, Hospital Infections Program, and Foodborne and Diarrheal Diseases Br, Div of Bacterial and Mycotic Diseases, National Center for Infectious Diseases; and EIS officers, CDC. Editorial NoteEditorial Note: Epidemic typhoid fever emerged in Dushanbe because of contamination of the city's water treatment and distribution systems following the dissolution of the Soviet Union and an ensuing civil war. Through support from the U.S. Agency for International Development (USAID), the International Federation of Red Cross and Red Crescent Societies, and other partners, measures to improve chlorination, repair infrastructure, conserve water, and educate the public have contributed to controlling the epidemic. During January-March 1998, the incidence of typhoid fever in Dushanbe decreased approximately 90% compared with January-March 1997; however, continued epidemiologic and laboratory surveillance are needed to guide resource allocation, monitor the effectiveness of prevention efforts, and determine appropriate antimicrobial therapy. The judicious use of fluoroquinolones is recommended to treat typhoid fever in Dushanbe. However, patients infected with nalidixic acid-resistant S. Typhi who receive short-course therapy with fluoroquinolones may not demonstrate clinical recovery and require repeated or alternative retreatment (4). In addition, the potential emergence of ciprofloxacin-resistant strains warrants close vigilance. The control and prevention of typhoid fever and other waterborne epidemic diseases in Dushanbe depends on repairing the water treatment and distribution systems and achieving adequate chlorination of drinking water. Major infrastructure repairs may require years of investment and should be complemented by water conservation efforts and the eventual introduction of a fee-for-use schedule. Reducing water wastage will improve water pressure in the distribution system and decrease the volume of water that needs to be provided and the amount of resources required to treat water. Until the municipal water supply reliably provides safe drinking water, public education campaigns stressing the importance of boiling all drinking water, conserving municipal water, and promoting basic hygiene measures to prevent the spread of typhoid fever will need to be strengthened. Other central Asian cities have similar economic and infrastructure problems and may be at risk for similar waterborne epidemics. To reduce the risk for similar epidemics in the region, CDC is working with USAID and the governments of the other central Asian republics to evaluate water treatment and distribution systems and enhance surveillance for diseases caused by waterborne pathogens. References
Figure_1  Return to top. Figure_2 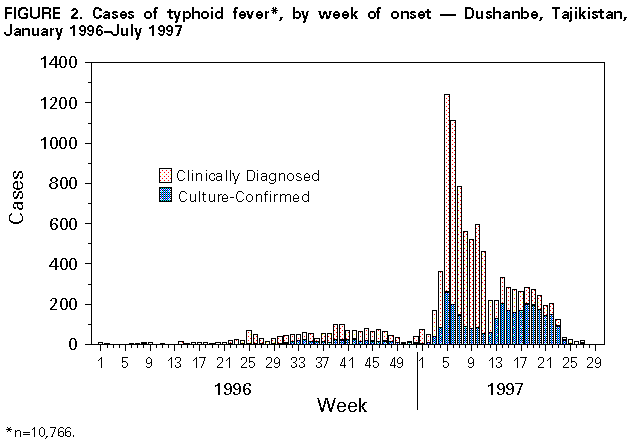 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/05/98 |
|||||||||
This page last reviewed 5/2/01
|