 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Rift Valley Fever -- East Africa, 1997-1998In December 1997, the Kenya Ministry of Health and the World Health Organization (WHO) in Nairobi received reports of 478 unexplained deaths in the North Eastern province of Kenya and southern Somalia. Clinical features included acute onset of fever and headache associated with hemorrhage (hematochezia, hematemesis, and bleeding from other mucosal sites). Local health officials also reported high rates of illness and death resulting from hemorrhage among domestic animals in the area. This report describes the preliminary results of the outbreak investigation and the results of a serologic survey. From late October 1997 through January 1998, torrential rains occurred in most of East Africa, resulting in the worst flooding in the region since 1961 and rainfall that was 60-100 times the seasonal average (National Climatic Data Center, unpublished data, 1998). Diagnostic testing of the initial 36 specimens received at the National Institute of Virology, South Africa, and at CDC confirmed acute infection with Rift Valley fever (RVF) virus in 17 (47%) persons from whom specimens were obtained; confirmation was made by detection of IgM antibodies, virus isolation, reverse-transcriptase-polymerase chain reaction for viral nucleic acid, or immunohistochemistry. Active surveillance conducted by WHO, the Kenya Ministry of Health, and international relief organizations during December 22-28 in 18 villages (population: 200,000) in Garissa district, North Eastern province, Kenya, identified 170 deaths resulting from a "bleeding disease." Severe flooding and large distances between settlements complicated case ascertainment and subsequent evaluation. Despite these constraints, the surveillance system received reports and blood specimens for 231 cases of unexplained severe febrile illness with onset from November 25, 1997, through February 14, 1998. Of the 231 reported cases, 115 met the case definition for hemorrhagic fever (i.e., fever and mucosal or gastrointestinal bleeding). Of the 115 patients with hemorrhagic fever, 58% were male (median age: 30 years {range: 3-85 years}); diagnostic testing demonstrated acute RVF viral infection in 27 (23%) (Figure_1). Of the 116 persons whose illnesses did not meet the case-definition for hemorrhagic fever, 26 (22%) had acute infection with RVF virus. Of these 26 persons, 14 had symptoms compatible with complications of RVF viral infection, including nine with neurologic disease and five with visual disturbances. In addition to the confirmed RVF cases in the North Eastern province and the Gedo, Hiran, and Lower Shabeelle provinces of Somalia, acute confirmed RVF cases were identified in the Central (one case), Eastern (nine cases), and Rift Valley (12 cases) provinces of Kenya (Figure_2). Studies conducted during this outbreak included human, livestock, and entomologic sampling. Using a multistage cluster sampling strategy based on the population distribution in Garissa district, an international task force led by the Kenya Ministry of Health conducted a cross-sectional study to examine risk factors and determine the prevalence of recent infection with RVF virus. Anti-RVF virus IgM was detected by enzyme-linked immunosorbent assay in 18 (9%) of the 202 persons in the sample; all 18 had recently been ill, compared with 80% of the seronegative persons (p=0.05). The study did not identify statistically significant differences in the frequency of IgM antibody by sex or age. However, contact with livestock (e.g., herding, milking, slaughtering, and sheltering animals in the home) was statistically associated with serologic evidence of acute infection with RVF virus (p less than 0.01). In this cross-sectional survey, livestock owners reported losses of approximately 70% of their sheep and goats and 20%-30% of cattle and camels. Other infections contributing to the high mortality in the epizootic included nonspecific pneumonia, pasteurellosis, contagious caprine pleuropneumonia, contagious pustular dermatitis, bluetongue, and complications of mange and foot rot (Field Mission of the Food and Agriculture Organization of the United Nations, unpublished data, 1998). RVF serologic results from animal samples collected by veterinary staff in this and other regions of Kenya are pending. In February 1998 in Garissa district, 3180 mosquitoes from three trapping sites were collected. Three of the nine captured species have been previously implicated in RVF transmission (Anopheles coustani, Mansonia africana, and M. uniformis). Viral isolation studies are under way. Reported by: Kenya Ministries of Health and Agriculture; Virus Research Center, Kenyan Medical Research Institute; African Medical Relief Foundation; International Federation of Red Cross and Red Crescent; Somalia Aid Coordinating Board, Nairobi, Kenya. Ministries of Health and Agriculture, Dar es Salaam, Tanzania. Univ of Pretoria, Onderstepoort; National Institute of Virology, Sandringham, South Africa. Med�cins Sans Fronti�res International; European Programme for Intervention Epidemiology (EPIET), European Union. EPICENTRE; Med�cins du Monde, Paris, France. Emergency Prevention System, Food and Agriculture Organization, Rome, Italy. World Health Organization Country Offices for Kenya, Somalia, and Tanzania; African Regional Office, Harare, Zimbabwe. Div of Emerging and other Communicable Disease Surveillance and Control; World Health Organization, Geneva, Switzerland. US Army Medical Research Unit-Kenya. US Naval Medical Research Unit No. 3, Cairo, Egypt. Health Studies Br, Div of Environmental Hazards and Health Effects, National Center for Environmental Health; Meningitis and Special Pathogens Br, Div of Bacterial and Mycotic Diseases, Div of Vector-Borne Infectious Diseases, Infectious Diseases Pathology Activity and Special Pathogens Br, Div of Viral and Rickettsial Diseases, National Center for Infectious Diseases; and EIS Officers, CDC. Editorial NoteEditorial Note: In Kenya in 1930, RVF virus was first isolated and recognized as the etiologic agent for a zoonotic disease associated with substantial perinatal mortality and abortions in livestock (1). RVF outbreaks historically occurred in sub-Saharan Africa until 1977-1978, when an estimated 18,000 human infections and 598 deaths were officially reported in Egypt. In addition, during this outbreak, most pregnant ewes aborted and most lambs died (2). Epizootics occur periodically after heavy rains that flood natural depressions, which enables hatching of the primary vector and reservoir (Aedes sp. mosquitoes). High levels of viremia in animals lead to infection of secondary arthropod vector species and virus amplification in livestock with collateral infection of humans. As noted in this outbreak, transmission of RVF virus to humans also can occur by contact with blood or body fluids from viremic animals. Disease in humans usually is a mild, febrile illness; however, 1%-2% of infections may result in fatal hemorrhagic fever or encephalitis. Vascular retinitis with permanent partial loss of vision develops in a higher percentage of patients. The magnitude of infection and economic loss from the outbreak described in this report is difficult to gauge. Preliminary estimates of deaths among animals and humans suggest this may be the largest reported outbreak of RVF in East Africa and the first recorded in Somalia (3). On the basis of an estimated antibody prevalence of 9% and the assumption that all persons residing in the North Eastern province and southern Somalia were at risk for infection, an estimated 89,000 humans in this region could have been infected. This does not include infected persons in the rest of Kenya and neighboring countries. Preliminary laboratory results have confirmed other viral agents, malaria, Shigella dysentery, and leptospirosis as explanations for some of the reported illnesses that met the case definition for hemorrhagic fever but were seronegative for RVF virus. Other possible explanations for the cases of fever with hemorrhage that were negative for RVF virus include an extremely sensitive case definition, inadequate samples, and other pathogens, toxins, and complications of malnutrition. Ongoing investigations may help define the magnitude and identify additional etiologic agents associated with this outbreak. Satellite and precipitation data document widespread high levels of rainfall with increases in vegetation during the same period in previous years; these conditions support transmission of RVF virus throughout Kenya and the surrounding countries. This is consistent with reports of confirmed cases from at least four provinces in Kenya (North Eastern, Eastern, Central, and Rift Valley), southern Somalia, and northern Tanzania. Deaths resulting from acute hemorrhagic fever among humans and abortions among livestock also have been reported from bordering countries, although no specimens have been available for diagnostic testing. The extent of RVF virus transmission and the probability of recurring outbreaks in East Africa emphasize the necessity of developing and validating methods to predict, prevent, and treat RVF (4). Longitudinal studies are required to validate remote sensing satellite data and to target areas for animal vaccination and vector control, enhance surveillance activities for RVF in animals and humans, and enable prospective entomologic studies. References
Figure_1 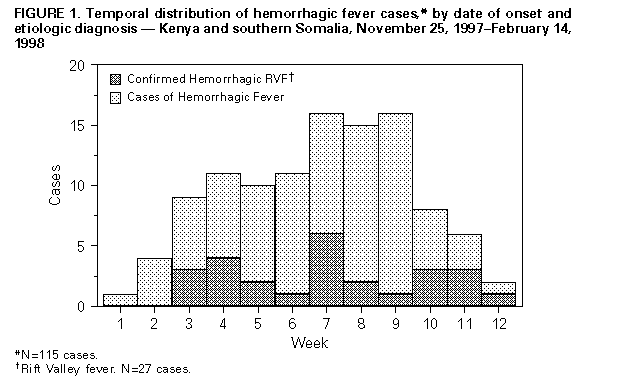 Return to top. Figure_2 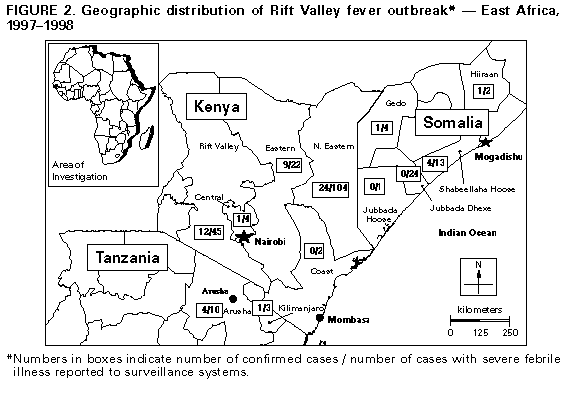 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/05/98 |
|||||||||
This page last reviewed 5/2/01
|