 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Serious Hearing Impairment Among Children Aged 3-10 Years -- Atlanta, Georgia, 1991-1993Hearing impairment without appropriate intervention among young children can delay the acquisition of speech and language skills that, in turn, can result in learning and other problems at school age (1). Interventions to reduce the occurrence of communication disabilities associated with hearing impairment are most successful if affected children are identified early, ideally during the first few months of life (1). Technologies are now available to accurately and routinely screen all newborns for hearing impairment before hospital discharge (2,3). One of the national health objectives for the year 2000 is to reduce the average age at which children with serious hearing impairment are identified to no more than 12 months (objective 17.16) (4). Since 1991, CDC's Metropolitan Atlanta Developmental Disabilities Surveillance Program (MADDSP) has monitored the prevalence of serious hearing impairment among children aged 3-10 years in the metropolitan Atlanta area. This report presents findings from MADDSP for 1991-1993 (the most recent years for which data were available) about the age of diagnosis of serious bilateral hearing impairment among children born from 1981 through 1990 and highlights the public health intervention opportunity of universal newborn hearing screening programs for the earlier identification of and intervention for children with hearing impairment. For surveillance purposes, MADDSP defines hearing impairment as a bilateral, pure-tone hearing loss at frequencies of 500, 1000, and 2000 Hertz averaging 40 decibels (dBs) or more, unaided, in the better ear as indicated by the results of an audiologic test. Children for whom test results are not available but for whom records include a description, by a licensed or certified audiologist or qualified physician, of a hearing loss of greater than or equal to 40 dBs in their better ear also are considered to be hearing impaired. The MADDSP identifies children with serious hearing impairment by reviewing existing records at multiple sources, including the special education programs in the nine public school systems serving the surveillance area; state schools for the hearing impaired; the three pediatric specialty care hospitals and associated clinics in the area; and facilities operated by the Georgia Department of Human Resources that provide services for children with sensory, motor, or mental impairments. For all children with hearing impairments, MADDSP seeks information on type of hearing impairment (sensorineural, conductive, or mixed), level of impairment (moderate, 40-64 dBs; severe, 65-84 dBs; or profound, greater than or equal to 85 dBs), and the earliest age when the children's hearing loss first met the MADDSP criteria. During 1991-1993, an estimated 263,000 children aged 3-10 years resided in the metro-Atlanta area during each of those years. For this period, MADDSP identified 413 children (283 in 1991, 288 in 1992, and 293 in 1993) who met the surveillance case definition for hearing impairment. The average annual prevalence rate was 1.1 per 1000 children aged 3-10 years. Approximately two thirds (283 {69%}) of the children had a sensorineural hearing loss that did not result from a postnatal cause and was presumed to be present at birth. To ensure more complete information about age at first diagnosis, additional analysis was restricted to the subgroup of these children who were born to a resident of the study area (n=173). Of these, 13 (8%) children had had their hearing impairment diagnosed during their first year of life, and 81 (47%) did not have their impairment diagnosed until they were aged greater than or equal to 3 years (Figure_1). The mean age at earliest known diagnosis was 2.9 years. In general, the severity of the hearing impairment varied inversely with the child's age at diagnosis: among children with severe to profound hearing loss, the mean age at diagnosis was 2.4 years, compared with 3.6 years for children with a moderate loss. In addition, 50 (29%) of the 173 children had at least one other developmental disability (i.e., mental retardation, cerebral palsy, or vision impairment) and 17 (10%) had been very low birthweight (less than 3 lbs, 5 oz {less than 1500 g}) infants. However, very low birthweight was not statistically associated with an earlier age at diagnosis (2.6 years compared with 2.9 years for children with hearing impairment born weighing greater than or equal to 3 lbs, 5 oz {greater than or equal to 1500 g}; p=0.7). Reported by: Developmental Disabilities Br, Div of Birth Defects and Developmental Disabilities, National Center for Environmental Health, CDC. Editorial NoteEditorial Note: Based on the analysis in this report, a substantial proportion of children born with serious bilateral hearing impairment in Atlanta during 1981-1990 were not diagnosed at a sufficiently early age to benefit fully from intervention services to minimize delays in the acquisition of speech and language skills and, possibly, reduce the occurrence of other disabilities associated with hearing impairments. Because MADDSP focuses primarily on children with serious bilateral hearing impairment, these findings probably underestimate the actual magnitude of delayed diagnosis. Specifically, while the prevalence of hearing impairment in MADDSP is comparable to other population-based studies using similar definitions of hearing loss (5), studies of less severe loss (e.g., greater than 20 dBs, including unilateral losses) have documented higher prevalence rates (3.0-5.0 per 1000 children) (6,7). Losses of 25-30 dB and greater are considered to interfere with the development of communication skills, even if the loss is unilateral (1). The findings in this report are subject to at least two limitations. First, data were obtained from existing records that were accessible to the surveillance staff. As a result, some information relevant to a child's disability may not have been found in the records available for review. Second, the age at earliest diagnosis used by MADDSP refers to the age when the child's hearing loss first met the MADDSP case definition; this age may not be the earliest time when a less serious loss was noticed. As a result, information about the age at earliest diagnosis in the MADDSP may be inaccurate for some children. In 1982, the Joint Committee on Infant Hearing recommended audiologic screening for infants with one or more specified risk factors (e.g., a birthweight less than 3 lbs 5 oz {less than 1500 g}), bacterial meningitis, and anatomic malformations of the ear) for hearing loss (8). However, one or more of these risk factors are present in only 50% of all children among whom substantial hearing impairment is eventually diagnosed (1). In Atlanta, the mean age at diagnosis for children with sensorineural hearing impairment who were born weighing less than 3 lbs, 5 oz (less than 1500 g) was similar to that for children of greater birthweight, indicating that even in some high-risk children, hearing impairment is not diagnosed until substantially after the first year of life. The more recent recommendations, including those from the 1994 Joint Committee on Infant Hearing, specify universal newborn screening by age 3 months and the initiation of appropriate intervention by age 6 months (9,10). Children reported in MADDSP were born during 1981-1990, before the issuance of recommendations for universal newborn hearing screening. Some states have recently implemented universal newborn hearing screening programs while others, including Georgia, have begun planning for such services. For example, beginning in 1997, 20 hospitals in Georgia (which account for 24% of all births) are either offering or preparing to offer universal newborn hearing screening programs. The findings in this report emphasize the public health opportunity for the early identification of and appropriate intervention for children with hearing impairment and the need for the development and evaluation of universal newborn hearing screening programs. References
Figure_1 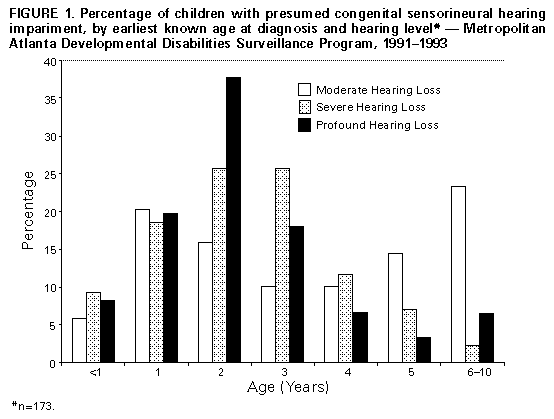 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|