 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Outbreaks of Salmonella Serotype Enteritidis Infection Associated with Consumption of Raw Shell Eggs -- United States, 1994-1995Salmonella serotype Enteritidis (SE) accounts for an increasing proportion of all Salmonella serotypes reported to CDC's National Salmonella Surveillance System. During 1976-1994, the proportion of reported Salmonella isolates that were SE increased from 5% to 26% (Figure_1). During 1985-1995, state and territorial health departments reported 582 SE outbreaks, which accounted for 24,058 cases of illness, 2290 hospitalizations, and 70 deaths. This report describes four SE outbreaks during 1994-1995 associated with consumption of raw shell eggs (i.e., unpasteurized eggs) and underscores that outbreaks of egg-associated SE infections remain a public health problem. Washington, D.C. In August 1994, a total of 56 persons who ate at a Washington, D.C., hotel had onset of diarrhea; 20 persons were hospitalized. Salmonella group D was isolated from stools of the 29 patrons who submitted specimens; 27 of the 29 isolates further typed were identified as SE. An investigation by the District of Columbia Commission of Public Health (DCCPH) involved 41 ill patrons and 23 well patrons who had eaten brunch at the hotel on August 28. A case was defined as onset of diarrheal illness in a person who ate brunch at the hotel on August 28. All 39 patrons who had eaten hollandaise sauce became ill, compared with two (8%) of 25 persons who had not eaten the sauce (odds ratio {OR}=undefined; lower 95% confidence limit=52; p= less than 0.01). Cultures of the sauce served on August 28 yielded SE. Of the 11 isolates tested (10 obtained from ill persons and one from the sauce), all were phage type 8. Cultures of pooled whole raw shell eggs, egg whites, and raw shell eggs from the same shipment as the implicated eggs did not yield Salmonella. The hollandaise sauce was prepared on August 28 by hand-cracking and pooling the egg yolks from 36 extra-large grade A raw shell eggs. Lemon juice, melted butter, salt, and pepper were added to the egg yolk mixture while heating over a hot water bath. After preparation, the sauce was held in a hot water bath at an estimated temperature of 100 F-120 F (38 C-49 C) for 9 hours while being served. Traceback of the implicated eggs by DCCPH, the Maryland Veterinary Service, and the U.S. Department of Agriculture's (USDA's) Animal and Plant Health Inspection Service (APHIS) identified two flocks in Pennsylvania as possible sources for the eggs. Indiana In June 1995, approximately 70 residents and staff of a nursing home in Indiana had onset of diarrhea and abdominal cramps. Stool cultures from symptomatic residents and staff yielded 39 confirmed cases of SE. The one isolate tested was phage type 13A. Three residents died from complications of SE infection. An investigation by the Indiana State Department of Health and the Vanderburgh County Health Department involved seven of the initial 18 case-patients and 13 well residents. A case was defined as diarrheal illness in a nursing home resident with onset on June 9. Six (86%) of the seven patients had eaten baked eggs for breakfast on June 7, compared with three (23%) of 13 well persons (OR=16.5; 95% CI=1.3-1009; p=0.02). The baked eggs were prepared by hand-cracking and pooling 180 medium grade A raw shell eggs, mixing the eggs with a hand whisk, and baking them in a single 8-inch deep pan at 400 F (204 C) for 45 minutes-1 hour. The eggs were then placed on a steam table where an internal temperature was obtained and reported in a chart log. Although recorded internal temperatures of eggs prepared during June ranged from 180 F-200 F (82 C-93 C), inadequate cooking may have contributed to the outbreak because the eggs were not stirred while being baked, and the internal temperature was obtained from only one place in the pan. The eggs were served within 30 minutes after cooking. At the time of the investigation, none of the prepared eggs or raw shell eggs from the same shipment were available for testing. APHIS traced the implicated eggs to a distributor who received eggs from at least 35 different flocks. Greenport, New York On June 24, 1995, a total of 76 persons attended a catered wedding reception. Following the reception, attendees contacted the local health department to report onset of a gastrointestinal illness. Salmonella group D was isolated from stools of the 13 persons who submitted specimens; 11 of the 13 isolates further typed were identified as SE. An investigation by the Suffolk County Health Department involved the 28 ill attendees and the 12 well attendees that were contacted. A case was defined as onset of diarrheal illness in an attendee of the reception. Twenty-six (93%) of 28 persons who had eaten Caesar salad became ill, compared with two (17%) of 12 persons who had not eaten the salad, (OR=52; 95% CI=6.2-849; p= less than 0.01). The Caesar salad dressing was prepared with 18 raw shell eggs, olive oil, lemon juice, anchovies, Romano cheese, and Worcestershire sauce at 11:30 a.m. on June 24. The mixture was held unrefrigerated at the catering establishment for 2 hours, then placed in an unrefrigerated van until delivered and served at the reception at 6 p.m. A traceback by the New York State Department of Agriculture and Markets (NYSDAM) identified the source of the eggs as a producer/distributor in Pennsylvania who received and commingled eggs from at least five flocks. New York City On July 23, 1995, three persons who lived in the same household drank a homemade beverage known as "Jamaican malt" and had onset of diarrhea, vomiting, and abdominal cramps; two were hospitalized. The mean period from consumption to onset of illness was 7.6 hours (range: 5.5-10.5 hours). Stool cultures from all three persons yielded SE. The beverage was prepared at home the evening of July 22 by mixing beer, refrigerated raw shell eggs, sweetened condensed milk, oatmeal, and ice. Two patients drank the beverage immediately after preparation, and the third drank it 5 hours later. The beverage had been refrigerated after preparation. Cultures of the leftover beverage, raw eggs from the same carton used to prepare the drink, and leftover egg shells from the eggs used to prepare the drink all yielded SE. Isolates from the one patient tested and all three food samples were phage type 13A. Traceback of the implicated eggs by NYSDAM identified a single flock in Pennsyl-vania. At the recommendation of the Pennsylvania Department of Health, eggs from the implicated flock were diverted to a pasteurization plant. Reported by: M Levy, MD, M Fletcher, PhD, M Moody, MS, Bur of Epidemiology and Disease Control, District of Columbia Commission of Public Health. D Cory, W Corbitt, MS, C Borowiecki, D Gries, J Heidingsfelder, MD, Vanderburgh County Health Dept, Evansville; A Oglesby, MPH, J Butwin, MSN, D Ewert, MPH, D Bixler, MD, B Barrett, K Laurie, E Muniz, MD, G Steele, DrPH, State Epidemiologist, Indiana State Dept of Health. A Baldonti, MD, Albert Einstein College of Medicine, New York City; B Williamson, Suffolk County Health Dept, Hauppauge; M Layton, MD, Bur of Communicable Disease Control, L Kornstein, PhD, Bur of Laboratories, E Griffin, Bur of Environmental Investigation, New York City Health Dept; M Cambridge, N Fogg, J Guzewich, Bur of Community Sanitation and Food Protection, T Root, Wadsworth Center for Laboratories and Research, D Morse, MD, State Epidemiologist, New York State Dept of Health; J Wagoner, New York State Dept of Agriculture and Markets. M Deasey, Div of Epidemiology, Pennsylvania Dept of Health; K Miller, Pennsylvania Dept of Agriculture. Animal and Plant Health Inspection Service, Food Safety and Inspection Service, US Dept of Agriculture. Food and Drug Administration. Foodborne and Diarrheal Diseases Br, Div of Bacterial and Mycotic Diseases, National Center for Infectious Diseases, CDC. Editorial NoteEditorial Note: During 1976-1994, rates of isolation of SE increased in the United States from 0.5 to 3.9 per 100,000 population (Figure_2). Two important factors probably contributed to the increase in 1994: 1) the effect of an outbreak of SE infections associated with a nationally distributed ice cream product (1) and 2) the expansion of the SE epidemic into California. During 1990-1994, the SE isolation rate for the Northeast region decreased from 8.9 to 7.0 per 100,000 population; the rate increased approximately threefold for the Pacific region (Figure_2). This increase was primarily associated with reports from California, where the percentage of Salmonella isolates that were SE increased from 11% in 1990 to 38% in 1994. In 1994, 24% of all SE isolates in the United States were from California. In the United States, both sporadic and outbreak-associated cases of SE infection frequently have been associated with consumption of raw or undercooked shell eggs (2-4). The findings in this report illustrate that outbreaks of egg-associated SE infections remain a public health problem in commercial food-service establishments, institutional facilities, and private homes throughout the United States. However, the risk for SE infection in humans can be reduced through public health prevention efforts (see box) (Table_B)(5). In 1994, no reported deaths resulted from SE outbreaks in the United States; however, in 1995, five deaths were associated with SE outbreaks, including the three in Indiana described in this report. One possible explanation for the lack of deaths in 1994 is that no nursing home outbreaks were reported that year; four of the five reported deaths in 1995 occurred among nursing home residents. During 1985-1991, a total of 59 SE outbreaks occurred in hospitals or nursing homes, accounting for only 12% of all outbreak-associated cases but 90% of all deaths. The case-fatality rate in these institutions was 70 times higher than in outbreaks in other settings (4). This underscores the importance of using pasteurized egg products for all recipes requiring pooled, raw, or undercooked shell eggs for the institutionalized elderly and other high-risk populations. In 1990, USDA initiated a mandatory program to test for SE in breeder flocks that produce egg-laying chickens. In addition, USDA traced the eggs implicated in human foodborne SE outbreaks back to the farm of origin and, when feasible, conducted serologic and microbiologic assessments of the farm. If SE was detected at the source farm, the eggs were diverted to pasteurization. Funding for this program was discontinued effective October 1, 1995. As a result, these efforts are conducted by the Food and Drug Administration, which has regulatory authority for shell eggs in interstate commerce. Further control of SE will require limiting the spread of SE on farms. In 1992, USDA, in collaboration with the industry, academia, and the Pennsylvania Department of Agriculture (PDA), initiated a flock-based intervention program, the Pennsylvania Pilot Project (6), which evolved in 1994 into the current Pennsylvania Egg Quality Assurance Program (PEQAP). USDA provided oversight for PEQAP until June 30, 1996, when the program was transferred to PDA and the industry. This prevention program uses many of the on-farm microbiologic testing and control procedures developed in the pilot project to reduce SE contamination of eggs. The decrease in SE infections in the Northeast may reflect the collaborative prevention efforts in that region; similar efforts may be necessary to control the problem elsewhere in the country. References
Figure_1 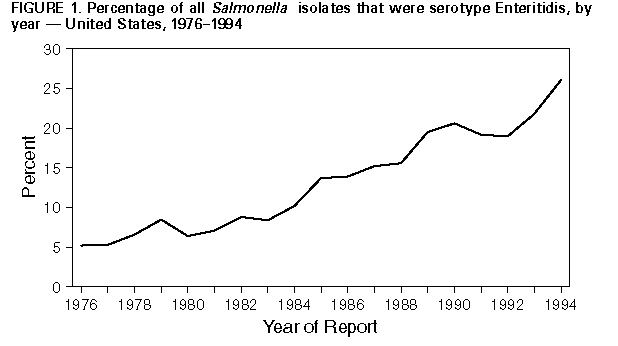 Return to top. Figure_2 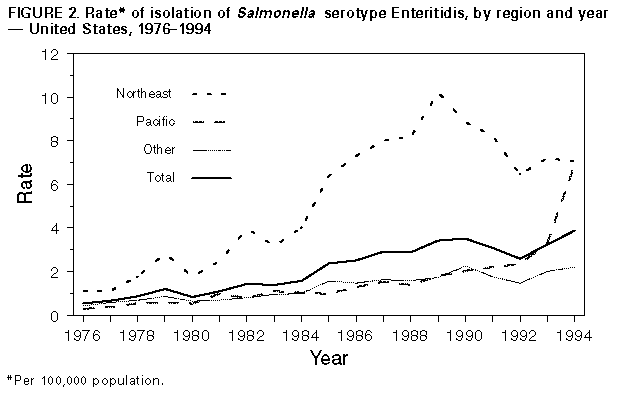 Return to top. Table_B Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size.
Recommendations for Preventing
Salmonella Serotype Enteritidis Infections Associated with Eggs
========================================================================================
- Consumption of raw or undercooked eggs should be avoided, especially by
immunocompromised or other debilitated persons.
- In hospitals, nursing homes, and commercial kitchens, pooled eggs or raw or
undercooked eggs should be substituted with pasteurized egg products.
- Eggs should be cooked at >=145 F (>=63 C) for >=15 seconds (until the white is
completely set and the yolk begins to thicken) and eaten promptly after cook-
ing.
- Hands, cooking utensils, and food-preparation surfaces should be washed with
soap and water after contact with raw eggs.
- Eggs should be purchased refrigerated and stored refrigerated at <=41 F (<=5 C) at
all times.
- Flock-based egg-quality-assurance programs that meet national standards and
include microbiologic testing should be adopted by industry nationwide.
========================================================================================
Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|