 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Outbreak of Salmonellosis Associated With Beef Jerky -- New Mexico, 1995In February 1995, the New Mexico Department of Health (NMDOH) was notified of cases of salmonellosis in two persons who had eaten beef jerky. An investigation by the New Mexico Environment Department determined that these cases were associated with beef jerky processed at a local plant. An investigation by NMDOH identified 91 additional cases. This report summarizes the investigation of this outbreak. On January 26, 1995, two men presented to the emergency department of a local hospital after onset of diarrhea and abdominal cramps. On January 24, the men had purchased and consumed carne seca, a locally produced beef jerky. Cultures of leftover beef jerky and stool obtained from one patient grew Salmonella. On February 7, NMDOH identified both isolates as Salmonella serotype Montevideo. NMDOH initiated efforts to determine whether other cases of salmonellosis associated with beef jerky had occurred. On February 8, NMDOH issued a news release advising the public not to eat the implicated brand of beef jerky and to contact the local health department if illness had occurred after eating the product. Cases also were identified through a review of NMDOH records for isolates matching those identified in jerky samples. A confirmed case of beef jerky-related salmonellosis was defined as isolation of Salmonella from a stool sample obtained from a person who had consumed the implicated jerky. A probable case was defined as onset of diarrhea, abdominal cramps, vomiting, and/or nausea in a person who had consumed the implicated jerky. Illness in 93 persons met the probable or confirmed case definitions. Ill persons reported purchasing the jerky at the local processing plant and eating the jerky during January 21-February 7; onset of symptoms occurred during January 22-February 11 Figure_1 Incubation periods for most (89%) persons were less than or equal to 3 days. The median age of ill persons was 22 years (range: 2-65 years); 56 (60%) were male. Symptoms of the 93 persons included diarrhea (93%), bloody diarrhea (13%), abdominal cramps (87%), headache (74%), fever (61%), vomiting (43%), and chills (40%). The median duration of illness was 7 days (range: 1-40 days). Five persons (5.4%) were hospitalized. Of the 93 cases, 40 were culture-confirmed. From the stool samples of these 40 ill persons, three Salmonella serotypes were isolated: Salmonella Typhimurium (31 persons), Salmonella Montevideo (12), and Salmonella Kentucky (11). Stool samples from 12 persons yielded two serotypes, and the sample from one patient contained all three serotypes. Samples of leftover beef jerky were obtained from five ill persons and from the manufacturer; 11 of the 12 samples tested contained one or more of the three Salmonella serotypes isolated from the patients. Each of the Salmonella Typhimurium isolates obtained from 31 persons with culture-confirmed cases and from the beef jerky were the same uncommon phenotypic variant. The processing plant that manufactured the contaminated beef jerky was inspected by state authorities on January 31. However, because the plant was not in production, processing-stage temperatures could not be obtained. The owner of the plant described the processing to include placement of slices of partially frozen beef on racks in a drying room at 140 F (60 C) for 3 hours, then holding the meat at 115 F (46 C) for approximately 19 hours; however, temperatures of the meat were never measured. After processing, the jerky was placed in uncovered plastic tubs for sale to the public. The plant owner, who performed all the work in the plant, denied a history of recent gastrointestinal illness but declined to provide a stool specimen. The plant voluntarily closed permanently on February 10. Salmonella was not isolated from environmental swabs taken from 20 surfaces within the plant on February 20. Reported by: FH Crespin, MD, B Eason, K Gorbitz, T Grass, C Chavala, Public Health Div, PA Gutierrez, MS, J Miller, LJ Nims, MS, Scientific Laboratory Div, M Tanuz, M Eidson, DVM, E Umland, MD, P Ettestad, DVM, Div of Epidemiology, Evaluation and Planning, CM Sewell, DrPH, State Epidemiologist, New Mexico Dept of Health; T Madrid, K Smith, C Hennessee, Div of Field Svcs, New Mexico Environment Dept. Foodborne and Diarrheal Diseases Br, Div of Bacterial and Mycotic Diseases, National Center for Infectious Diseases; Div of Field Epidemiology, Epidemiology Program Office, CDC. Editorial NoteEditorial Note: Although beef jerky and other processed meat products are considered to be ready-to-eat and, therefore, are expected to be pathogen-free, some recent foodborne disease outbreaks have been associated with ready-to-eat meat products, including salami and sausage (1,2). In the outbreak described in this report, the isolation of the same Salmonella serotype from leftover beef jerky and the stool specimen of an ill person who reported eating the jerky warranted the rapid intervention initiated by NMDOH. Isolation of the combination of uncommon Salmonella serotypes from leftover jerky and the stool specimen of one patient confirmed beef jerky as the source of the outbreak. In addition to this outbreak, NMDOH investigated five outbreaks of salmonellosis associated with locally produced beef jerky during 1966-1988 (3,4) and one outbreak of staphylococcal food poisoning in 1982; none of the beef jerky implicated in these outbreaks had been shipped to other states. To determine whether consumption of jerky had been associated with foodborne outbreaks in other states during 1976-1995, NMDOH and CDC during May-August 1995 conducted an electronic mail survey with telephone follow-up of all other state health departments. Of the 47 state health departments that responded, 24 (51%) reported that processors of beef jerky were located within their state; however, only four states reported foodborne disease outbreaks associated with locally produced or homemade jerky during 1976-1995, and these outbreaks were caused by Trichinella spiralis and nitrite poisoning. In addition to beef, jerky implicated in these outbreaks had been produced from meat obtained from cougar and bear. Potential explanations for the larger number of jerky-related cases in New Mexico include higher prevalences of consumption of beef jerky, enhanced surveillance for outbreaks, and differences in production methods. This outbreak underscores the risk for foodborne disease associated with consumption of locally produced beef jerky and the need for preventive measures. Conditions recommended for the prevention of bacterial growth during jerky production include rapid drying at high temperatures (i.e., initial drying temperature greater than 155 F {68.3 C} for 4 hours, then greater than 140 F {60 C} for an additional 4 hours) and decreased water activity (i.e., aw=0.86) (5,6). In 1989, because of several beef jerky-related foodborne outbreaks, the New Mexico Environment Department promulgated regulations regarding the commercial production of jerky made from meat or poultry. The outbreak described in this report is the first jerky-related outbreak to be recognized in New Mexico since the regulations were implemented. As a result of this outbreak, the New Mexico Environment Department plans to evaluate the production processes, including temperatures of meat during drying, of all jerky processors in New Mexico and to assist processors in implementing changes necessary to comply with the regulations. References
Figure_1 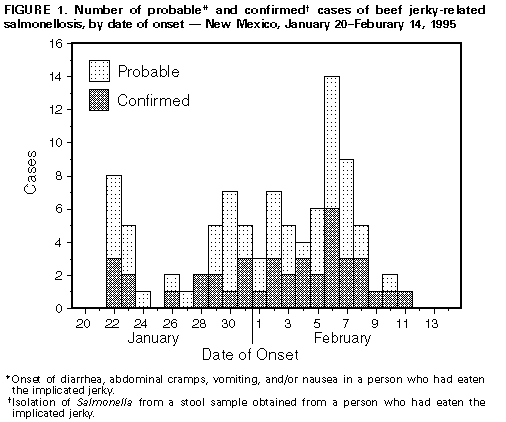 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|