 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Heat-Related Mortality -- Chicago, July 1995During July 12-16, 1995, Chicago experienced unusually high maximum daily temperatures, ranging from 93 F to 104 F (33.9 C to 40.0 C). On July 13, the heat index* peaked at 119 F (48.3 C) -- a record high for the city. This report describes the heat- related deaths reported by the Cook County Medical Examiner's Office (CCMEO) during this heat wave. Deaths classified as heat-related by the CCMEO met one of the following three criteria: 1) core body temperature of the decedent greater than or equal to 105 F ( greater than or equal to 40.6 C) at the time of or immediately after death, 2) substantial environmental or circumstantial evidence of heat as a contributor to death (e.g., decedent found in a room without air conditioning, all windows closed, and a high ambient temperature), or 3) decedent in a decomposed condition without evidence of other cause of death and with evidence that the decedent was last seen alive during the heat wave period. During July 11-27, a total of 465 deaths were certified as heat-related by the CCMEO Figure_1; during July 4-10, no deaths were certified as heat-related. The highest number of heat-related deaths previously certified by the CCMEO -- associated with a heat wave in 1988 -- was 77. The number of heat-related deaths peaked 2 days after the heat index peaked. Deaths increased from 49 (July 14) to a maximum of 162 (July 15) Figure_1. Of the 465 decedents, 257 (55%) were male. Based on race-specific data, 229 (49%) decedents were black; 215 (46%), white; and 21 (5%), other racial/ethnic groups.** Within racial categories, 128 (56%) blacks were male, and 114 (53%) whites were male. Of the 437 decedents for whom age could be determined, age ranged from 3 years to 103 years (median: 75 years, mean: 72 years); 222 (51%) were aged greater than or equal to 75 years. During July 13-21 (when most heat-related deaths were certified by the CCMEO), a total of 1177 deaths occurred in Chicago -- an 85% increase over the same period in 1994 (637 deaths). Reported by: ER Donoghue, MD, MB Kalelkar, MD, MA Boehmer, Office of the Medical Examiner County of Cook, Chicago; J Wilhelm, MD, S Whitman, PhD, G Good, MS, S Lyne, RSM, Commissioner, City of Chicago Dept of Health; J Lumpkin, MD, L Landrum, MUPP, BJ Francis, MD, State Epidemiologist, Illinois Dept of Public Health. Div of Environmental Hazards and Health Effects, National Center for Environmental Health, CDC. Editorial NoteEditorial Note: Excess mortality from hyperthermia and cardiovascular disease during heat waves has been well documented (2,3). The findings in Chicago by the CCMEO that blacks, males, and the elderly appear to be particularly susceptible to heat-related death are similar to previous studies of heat waves. During public health crises such as heat waves, state-specific mortality data are often incomplete or unavailable; therefore, data from medical examiners' (MEs') offices may be used to assess mortality during such crises. Although ME-based surveillance for heat-related deaths can prompt timely public health responses during heat waves, use of ME data is limited because of selection bias. Individual MEs and other persons who certify deaths (e.g., coroners and attending physicians) use varying criteria to determine which deaths are heat-related, largely because no standardized definition exists. In the United States, lack of a uniform definition for heat-related death results in substantial variation in the criteria used to certify such deaths. The most stringent definition of heat-related death is a core body temperature of greater than or equal to 105 F (greater than or equal to 40.6 C) taken at the time of death, with no other reasonable explanation of death. This definition precludes certifying any death as heat-related if core body temperature is not measured before or near the time of death and may underestimate excess heat-related mortality. A nonspecific definition of heat-related death (which could include all deaths that occur during a heat wave) would overestimate this mortality. The definition used by the CCMEO to classify deaths as heat-related has remained unchanged since 1978 and is based on a reasonable approach (i.e., evidence of exposure to high levels of environmental heat). These two factors (as well as the finding that the data about heat-related deaths are consistent with preliminary data about total mortality in Chicago during July 1995) suggest that the CCMEO data did not overestimate heat-related mortality during that period. The differential impact of a heat wave on specific population subgroups cannot be determined based on ME data alone because of incompleteness and potential bias (3,4). For example, based on CCMEO data, a disproportionately high number of heat-related deaths occurred among blacks in Chicago on July 15 Figure_1. Because CCMEO data do not include all deaths nor equally represent all socioeconomic status (SES) categories, it is not yet possible to completely describe mortality, calculate death rates, or determine whether the race- and sex-specific distribution of the heat-related deaths is disproportionate to overall mortality in Chicago. A case-control study is under way in Chicago to examine the influences of SES and specific environmental factors on heat-related mortality. Despite their limitations, the data in this report confirm that 1) public health information should be directed toward susceptible populations (e.g., the elderly), 2) as in other heat waves (2,3), the time between the beginning of a heat wave and the resulting heat-related deaths (e.g., 2 days in Chicago) should be sufficient to disseminate prevention messages to the public, and 3) a standardized definition of heat-related death is needed. Heat-related mortality is preventable. The most effective measures for preventing heat-related illness and death include reducing physical activity, drinking additional nonalcoholic liquids, and increasing the amount of time spent in air-conditioned environments. In addition, because increased air movement (e.g., fans) has been associated with heat stress when the ambient temperature exceeds approximately 100 F (37.8 C) and because fans are not protective at temperatures greater than 90 F (greater than 32.3 C) with humidity greater than 35% (the exact temperature varies with the humidity), fans should not be used for preventing heat-related illness in areas with high humidity (3,5). To further define information that can be used to identify persons at greatest risk during hot weather, CDC is collaborating with Chicago and Illinois health officials to determine risk factors to better target persons at increased risk for heat-related illness or death. A standard definition for heat-related death will be addressed at the February 1996 meeting of the American Academy of Forensic Sciences. References
* The heat index (i.e., the apparent temperature) is an estimation of the influence of temperature and humidity on the evaporative and radiative transfer of heat between a typical human and the atmosphere. The values can be derived from a chart available through the National Weather Service (1). ** The CCMEO categorizes race of decedents as black, white, or other. Figure_1 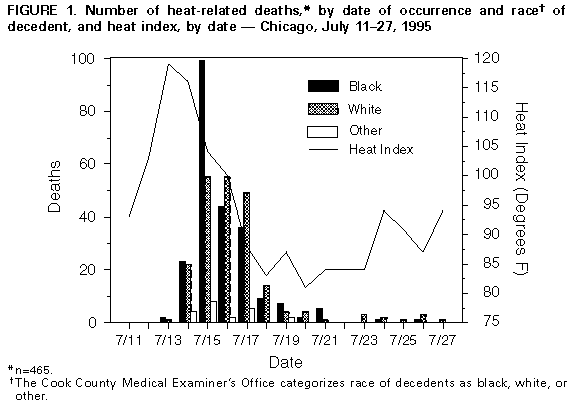 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|